Eklabu
Diunggah oleh
Ruth GaleraJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Eklabu
Diunggah oleh
Ruth GaleraHak Cipta:
Format Tersedia
Module No.
5
OBSTETRIC & GYNECOLOGY II
GYNE ONCOLOGY : FALLOPIAN TUBE & PERITONEAL CANCER 2.2
BOOK BASED
19 February 2018
• Mostly involve: fimbriated end of the fallopian tube
Outline
• Fallopian tube: primary source of ovarian and primary peritoneal serous
I. Overview carcinomas in women w/ BRCA mutations.
II. Causes
• Recommended following rrBSO to undergo examination for neoplasm.
III. Clinical Findings
• Consists of serial sectioning and extensively examining the fimbrial end of
IV. Diagnosis
the fallopian tube using the sectioning and extensively examining the
V. Pathological Findings
fimbriated end (SEE-FIM) protocol
VI. Treatment
VII. Surveillance • Ovarian and peritoneal cancer coexist w/ a STIC
VIII. Prognosis • Kindelberger study: 47% of 43 tumors classified as primary ovarian
cancers, a STIC was present
LEGEND • Carlson: 47% of 19 women w/ serous peritoneal cancers have a STIC in
Note! Purely textbook since this was not discussed during the lecture. the fallopian tube
• p53 mutational analyses showed the same mutations in the STIC and
distant tumors, providing a genetic link between the two.
I. OVERVIEW
• Fallopian tube and primary peritoneal cancers - similar but pathologically
distinct entities from epithelial ovarian cancer. III. CLINICAL FINDINGS
• Similarity in (compared to ovarian cancer): Fallopian Tube (FT) Cancer
✓ Clinical characteristics • Mean age: 58 years, range of 26 to 85 years
✓ Patterns of spread • Women w/ BRCA-associated FT carcinoma, the age at diagnosis is
✓ Response to treatment younger
✓ Survival rates. • Cass study: median age is 57 years in BRCA mutation carriers compared
• High grade papillary serous adenocarcinoma - most common histologic w/ 65 years in sporadic cases
type for all three malignancies • More common among white women (age-adjusted incidence rate, 0.41),
• Fallopian tube and primary peritoneal cancers – have distinct pathologic compared w/ black women (0.27), Hispanic women (0.27), and Asians and
findings. Pacific Islanders (0.25)
• Presenting symptoms related to the degree of obstruction of the distal tube
II. CAUSES • Many women are asymptomatic
Fallopian Tube (FT) Cancer • Most commonly reported s/sx:
- Abnormal vaginal bleeding/serosanguineous vaginal discharge (35-
• Rare, 0.2% of gynecologic malignancies 60%)
• Incidence in US: 0.41/ 100,000 women - Palpable adnexal mass (10% to 60%)
• May actually arise from the epithelial lining of the fallopian tube fimbria - Crampy lower abdominal pain caused by tubal distention and forced
• Primary risk factor: inherited mutation in the BRCA1 and BRCA2 tumor peristalsis (20% to 50%)
suppressor genes • Hydrops tubae profluens: term used to describe intermittent expulsion of
• Chen and Mavaddat study: Women with BRCA1 and BRCA2 mutations clear or serosanguineous fluid from the vagina caused by contraction of a
have a 40% to 60% and 20% to 30% lifetime risk, respectively. distended, distally occluded fallopian tube.
• Levine and Cass study: 15% to 45% of women w/ FT cancers have a - Followed by shrinkage or resolution of the adnexal mass
BRCA mutation - Triad (Latzko’s triad): intermittent serosanguineous discharge,
• Risk- reducing bilateral salpingo-oophorectomy (rrBSO) is there- fore colicky pain, and a mass pathognomonic of FT cancer (15% of
recommended for women with a BRCA mutation once they have patients)
completed childbearing • 10% to 40%: abnormal cervical cytology results, including
• In women w/o a BRCA mutation, the cause of FT carcinoma remains adenocarcinoma or atypical glandular cells (AGUSs)
unclear • CA-125 level evaluation and transvaginal ultrasound: rule out ovarian and
• Associated risk factors: infertility, low parity, early menarche, and late FT cancer
menopause - Considered in women w/ AGUs who have a negative workup for
• Protective factors: OCP use, multiparity, breastfeeding, and tubal ligation endocervical and endometrial carcinoma
Peritoneal Cancer Peritoneal Cancer
• Previously known as primary peritoneal carcinoma • Older women, median age range from 63 to 66 years
• First described in 1959 by Swerdlow • Typically present w/ pain, abdominal distention, pressure, and/or
• Diffusely involves the peritoneal surfaces while sparing or minimally gastrointestinal symptoms
involving the ovaries • Small proportion are asymptomatic
• Incidence in US: 0.46 per 100,000 women with 1:10 ratio of peritoneal • Occasionally detected during exploratory surgery
cancer to ovarian cancer cases.
• Histologically indistinguishable from epithelial ovarian cancer
IV. DIAGNOSIS
- Similar clinical characteristics, patterns of spread, response to
treatment, and survival rates • A definitive diagnosis is usually made at the time of surgery.
• Risk factors: similar w/ ovarian and FT cancer, and low parity
• Also associated w/ older age at diagnosis and increased rate of obesity Ultrasound
• Pathogenesis is not well characterized • Classic ultrasound findings for FT cancer: fluid-filled, tubular or ovoid
- Germinal epithelium of the ovary and mesothelium of the peritoneum mass w/ internal papillations, mural nodules, and/or septations that is
arise from the same embryonic origin separate from the uterus and ovaries
- Suggests that primary peritoneal cancer may develop from a • Primary peritoneal and FT cancers: ascites and/or peritoneal implants may
malignant transformation of these cells be present
- Other proposed theory: coelomic epithelium lining the abdominal • Both malignancies often have normal appearing ovaries
cavity (peritoneum) and ovaries (germinal epithelium) manifesting a
common response to an oncogenic stimulus
Other Imaging Modalities
- Molecular studies have been inconclusive
• A diagnosis of exclusion when primary ovarian or FT carcinoma cannot • CT, MRI, PET scans: provide additional information regarding the extent
be identified of disease and sites of metastatic spread
Serous Tubal Intraepithelial Carcinoma (STIC) CA-125 Level
• 5% and 15% of women undergoing risk-reducing salpingo-oophorectomy • Elevated in more than 80% of women
(RRSO) are found to have occult serous cancers • Useful for monitoring response to treatment or evaluating a woman in
• A precursor lesion known whom the disease is suspected but is not recommended as a screening test
Transcribed by: PELISCO | VIRADOR Checked by: ABU Page 1 of 3
OBSTETRICS AND GYNECOLOGY Gynecologic Oncology: Fallopian Tube and Peritoneal Cancer Module 5, Lecture 2.2
• Other rare histologic subtypes: sarcomas, carcinosarcomas, germ cell
Staging tumors, and gestational trophoblastic tumors
• Most patients have grade 2 or 3 tumors, <5% being grade 1 tumors.
• Serous adenocarcinomas: diagnosed at advanced stages
• Endometrioid adenocarcinomas: diagnosed at earlier stages
• Distinguishing characteristic of primary FT carcinoma from metastatic
ovarian/primary peritoneal carcinoma (modified by Sedlis 1978):
1. Main tumor lies in the tube and arises from the endosalpinx.
2. Histologic pattern reproduces the papillary epithelium of tubal
mucosa.
3. A transition can be demonstrated between the malignant and
nonmalignant tubal epithelium.
4. Ovaries and uterus are normal or contain fewer tumors than the
fallopian tube.
• Data also suggest that:
- (+) STIC and minimal involvement of ovary: primary fallopian tube
- (-) STIC and majority of the tumor is in the ovary: ovarian origin
• Patterns of spread related to the degree of obstruction of the distal tube.
- Tumors, previous injury, infection, by-products of tumor growth
(blood and increased serous fluid) distend the tube discharged
intermittently through the vagina.
- Patent distal portion of the fallopian tube malignancy spreads more
easily, resulting in tumor seeding of the peritoneal cavity, ascites, and
omental caking
- Intraperitoneal spread occur as the tumor grows through the muscular
wall of the tube
• Peritoneum: most frequent site of metastatic spread
• Lymphatic spread also occurs to the pelvic and paraaortic lymph nodes
• Occult lymph node metastases may be present in patients w/ tumor that
grossly appeared to be confined to the fallopian tube.
Peritoneal Cancer
• Tends to involve the abdominal and pelvic surfaces diffusely
• Most common histologic type: high grade serous carcinoma
• Cases of endometrioid, clear cell, mucinous, and carcinosarcoma have also
been reported
• The Gynecologic Oncology Group (GOG) pathologic criteria for the
diagnosis of primary peritoneal carcinoma:
1. Both ovaries must be physiologically normal in size or enlarged by a
benign process.
2. Involvement: extra ovarian sites > surface of either ovary.
3. Microscopically, the ovarian component must be one of the following:
✓
Nonexistent
✓ Confined to the ovarian surface epithelium w/ no evidence of
cortical invasion
✓ Involving ovarian surface epithelium and underlying cortical
stroma but w/ any given tumor size smaller than 5x5 mm
✓ Tumor smaller than 5x5 mm w/in the ovarian substance, w/ or
w/o surface disease
2014 FIGO Staging of Ovarian, Fallopian Tube and Peritoneal Cancer 4. Histologic and cytologic characteristics of the tumor must be
predominantly of serous type similar or identical to ovarian serous
V. PATHOLOGICAL FINDINGS papillary adenocarcinoma, any grade.
Fallopian Tube (FT) Cancer
VI. TREATMENT
Surgery
• Primary surgery: collection of peritoneal washings or ascites (if present)
• Followed by hysterectomy and bilateral salpingo-oophorectomy
• Staging operation should be performed in early-stage disease
• Includes omentectomy, pelvic and paraaortic lymph node dissection, and
peritoneal biopsies
A. B. • Advanced disease: cytoreductive surgery w/ removal of as much visible
tumor as possible
• Improved survival rates are associated w/ optimal cytoreduction
- May be difficult to achieve w/ primary peritoneal cancer caused by
widespread peritoneal disease w/o a predominant pelvic or ovarian
mass.
Chemotherapy
• Advanced-stage: combination of carboplatin and paclitaxel.
C. D.
• Unresectable disease w/ large tumor burden or medical comorbidity
• Arise in either tube w/ similar frequency precluding surgery: neoadjuvant chemotherapy
• Bilateral in 3% to 8% of cases • Diagnostic laparoscopy: used to determine resectability and decide
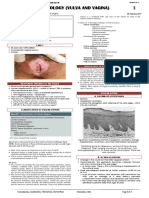
• Fimbriated end of the fallopian tube is grossly occluded in 50% of whether primary surgery or neoadjuvant chemotherapy is more
patients, resulting in a dilated lumen filled w/ tumor and/or fluid (Image A appropriate
& B)
• 80 to 90% of FT carcinomas are adenocarcinomas (Image C & D) Radiation Therapy
• Most of these are serous carcinomas, followed by endometrioid and clear
cell adenocarcinomas • Not recommended due to its tendency to spread throughout the abdominal
cavity and may cause excessive side effects even after administration of
Transcribed by: PELISCO | VIRADOR Checked by: ABU Page 2 of 3
OBSTETRICS AND GYNECOLOGY Gynecologic Oncology: Fallopian Tube and Peritoneal Cancer Module 5, Lecture 2.2
therapeutic doses.
VII. SURVEILLANCE
• Follow-up visits
- Every 2 to 4 months for the first 2 years
- Every 3 to 6 months for the following 3 years
- Annually after 5 years
• Includes physical examination w/ pelvic examination, and CA-125 level
measurement if initially elevated
• Imaging studies not routinely performed unless clinically indicated
• Pap tests are generally not indicated
VIII. PROGNOSIS
• Prognosis for patients w/ FT cancer is strongly related to the stage of
disease
• 5-year survival rates:
- 81% for stage I disease
- 67% for stage II disease
- 41% for stage III disease
- 33% for stage IV disease
• Other prognostic factors for early-stage disease include:
- Degree of invasion of the fallopian tube wall
- Location of the tumor w/in the tube (fimbrial vs nonfimbrial)
• Improved survival: tumor can be completely removed at the time of
surgery
• Patients w/ a BRCA mutation showed higher survival rates.
• Cass study: median survival time of 68 months for patients w/ BRCA-
associated FT cancer compared w/ 37 months for sporadic cases.
• Most studies have reported a better survival for patients w/ advanced-stage
FT cancer compared w/ primary ovarian cancer
• Retrospective case-control: no difference in survival rates between
patients w/ primary peritoneal cancer and w/ ovarian cancer.
• Favorable prognosis may be the result of a higher rate of BRCA mutation
carriers among women w/ FT cancer versus ovarian and primary
peritoneal cancers.
• If a subset of ovarian and primary peritoneal carcinomas actually arises
from the fallopian tube, the prognosis for women w/ fallopian tube,
primary peritoneal, and ovarian cancer may actually be similar.
SUMMARY
➢ There is increasing evidence that many cases of ovarian and peritoneal
carcinoma may actually arise from the fallopian tube, thereby
underestimating the incidence of fallopian tube carcinoma.
➢ Fallopian tube and peritoneal cancers are similar entities to epithelial
ovarian cancer.
➢ Fallopian tube and peritoneal cancers have similar clinical
characteristics, patterns of spread, and response to treatment compared
with ovarian cancer.
➢ The primary risk factor for fallopian tube and peritoneal cancer is an
inherited mutation in the BRCA1 or BRCA2 tumor suppressor gene.
➢ The most common histologic subtype of fallopian tube and peritoneal
carcinoma is high-grade serous carcinoma.
➢ The treatment of fallopian tube and peritoneal cancer is identical to that
for ovarian cancer and typically includes a combination of surgery and
chemotherapy.
➢ Prognosis for ovarian and peritoneal cancer is most strongly related to
the stage of disease and amount of residual tumor following the initial
tumor reduction surgery.
➢ Fallopian tube cancer has been shown to have a better prognosis
compared with ovarian and peritoneal cancer, but this may be because
of a higher rate of BRCA mutation carriers in women with fallopian tube
cancer.
REFERENCES
Comprehensive Gynecology 7th Edition
Transcribed by: PELISCO | VIRADOR Checked by: ABU Page 3 of 3
Anda mungkin juga menyukai
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (890)
- 500 Important Spoken Tamil Situations Into Spoken English Sentences SampleDokumen7 halaman500 Important Spoken Tamil Situations Into Spoken English Sentences SamplerameshdurairajBelum ada peringkat
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Stavanger Tourist SpotDokumen96 halamanStavanger Tourist Spotregupathi6413Belum ada peringkat
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- Allen Bradley Power Monitor 3000 Manual PDFDokumen356 halamanAllen Bradley Power Monitor 3000 Manual PDFAndrewcaesar100% (1)
- Revised fire drill performance standardsDokumen47 halamanRevised fire drill performance standardsKartikeya GuptaBelum ada peringkat
- Power Tube Biasing Operation Manual 15-01-08Dokumen2 halamanPower Tube Biasing Operation Manual 15-01-08MitchBelum ada peringkat
- Exercise Stress TestingDokumen54 halamanExercise Stress TestingSaranya R S100% (2)
- YOKOGAWADokumen16 halamanYOKOGAWADavide ContiBelum ada peringkat
- Mortgage Foreclosure Case Annulled Due to Lack of NoticeDokumen3 halamanMortgage Foreclosure Case Annulled Due to Lack of NoticeRuth Galera100% (1)
- Halaguen A Vs Pal Case DigestDokumen4 halamanHalaguen A Vs Pal Case DigestOnireblabas Yor Osicran100% (2)
- BS en 12201 5 2011Dokumen20 halamanBS en 12201 5 2011fatjon31100% (4)
- LIST Real Estate Contacts ListDokumen4 halamanLIST Real Estate Contacts ListChauhan Harshit100% (1)
- The Dedication of the Broken Hearted SailorDokumen492 halamanThe Dedication of the Broken Hearted SailorGabriele TorresBelum ada peringkat
- Mcqs in Labor Relations Law 4 Uc, No AnswersDokumen35 halamanMcqs in Labor Relations Law 4 Uc, No AnswersRuth GaleraBelum ada peringkat
- Rule 6: Kinds of PleadingsDokumen8 halamanRule 6: Kinds of PleadingsRuth GaleraBelum ada peringkat
- Rule 6: Kinds of PleadingsDokumen8 halamanRule 6: Kinds of PleadingsRuth GaleraBelum ada peringkat
- (Rule 6, Section 1) : Affirmative NegativeDokumen5 halaman(Rule 6, Section 1) : Affirmative NegativeRuth GaleraBelum ada peringkat
- Mighty Corporation and La Campana Fabrica de TobacoDokumen4 halamanMighty Corporation and La Campana Fabrica de TobacoRuth GaleraBelum ada peringkat
- Rules 1-3Dokumen34 halamanRules 1-3Ruth GaleraBelum ada peringkat
- Shinryo Phils. vs. RRN Inc.Dokumen12 halamanShinryo Phils. vs. RRN Inc.Ruth GaleraBelum ada peringkat
- 18 - 19 Draft of Step 8 EmailDokumen2 halaman18 - 19 Draft of Step 8 EmailRuth GaleraBelum ada peringkat
- Rules 1-3Dokumen34 halamanRules 1-3Ruth GaleraBelum ada peringkat
- Custom Search: Today Is Saturday, April 14, 2018Dokumen4 halamanCustom Search: Today Is Saturday, April 14, 2018Ruth GaleraBelum ada peringkat
- DocumentDokumen1 halamanDocumentKarl Rigo AndrinoBelum ada peringkat
- Corporation LawDokumen181 halamanCorporation LawRodil FlanciaBelum ada peringkat
- And or ButDokumen1 halamanAnd or ButRuth GaleraBelum ada peringkat
- 276 276 1 PBDokumen5 halaman276 276 1 PBRuth GaleraBelum ada peringkat
- GKJ KNLKDokumen1 halamanGKJ KNLKRuth GaleraBelum ada peringkat
- DBP Vs CaDokumen8 halamanDBP Vs CaRuth GaleraBelum ada peringkat
- Internal Medicine Patient with Abdominal PainDokumen28 halamanInternal Medicine Patient with Abdominal PainRuth GaleraBelum ada peringkat
- Vva AdvaDokumen1 halamanVva AdvaRuth GaleraBelum ada peringkat
- Conclusions Are Esent Barangays Covered by San Sebastian Health CenterDokumen2 halamanConclusions Are Esent Barangays Covered by San Sebastian Health CenterRuth GaleraBelum ada peringkat
- Court Case Document SummaryDokumen7 halamanCourt Case Document SummaryRuth GaleraBelum ada peringkat
- ADR - Ruth Part 2Dokumen2 halamanADR - Ruth Part 2Ruth GaleraBelum ada peringkat
- DigesrDokumen8 halamanDigesrRuth GaleraBelum ada peringkat
- Ek ParDokumen7 halamanEk ParRuth GaleraBelum ada peringkat
- Internal Medicine Patient with Abdominal PainDokumen28 halamanInternal Medicine Patient with Abdominal PainRuth GaleraBelum ada peringkat
- LaborDokumen14 halamanLaborRuth GaleraBelum ada peringkat
- Account ID Account Name Billing State/Province 2015-2016 ACT 2016 - 2017 ACTDokumen7 halamanAccount ID Account Name Billing State/Province 2015-2016 ACT 2016 - 2017 ACTRuth GaleraBelum ada peringkat
- NAPOCOR vs. Alonzo-LegastoDokumen37 halamanNAPOCOR vs. Alonzo-LegastoRuth GaleraBelum ada peringkat
- 2 - Alaska - WorksheetsDokumen7 halaman2 - Alaska - WorksheetsTamni MajmuniBelum ada peringkat
- Ericsson Microwave Outlook 2021Dokumen16 halamanEricsson Microwave Outlook 2021Ahmed HussainBelum ada peringkat
- Print Date:: Container No NO Size Seal No Seal Party Supplier Status Movement TypeDokumen3 halamanPrint Date:: Container No NO Size Seal No Seal Party Supplier Status Movement TypeYudha PermanaBelum ada peringkat
- UPSC IFS Botany Syllabus: Paper - IDokumen3 halamanUPSC IFS Botany Syllabus: Paper - IVikram Singh ChauhanBelum ada peringkat
- Whatever Happens, Happens For Something Good by MR SmileyDokumen133 halamanWhatever Happens, Happens For Something Good by MR SmileyPrateek100% (3)
- Workload Assessment in Railway ControlDokumen8 halamanWorkload Assessment in Railway ControlbbeeBelum ada peringkat
- Template EbcrDokumen7 halamanTemplate EbcrNoraBelum ada peringkat
- Deforestation Management System Using Force and SoundDokumen4 halamanDeforestation Management System Using Force and SoundManeesh SvsBelum ada peringkat
- Dahua Pfa130 e Korisnicko Uputstvo EngleskiDokumen5 halamanDahua Pfa130 e Korisnicko Uputstvo EngleskiSaša CucakBelum ada peringkat
- How Does Marijuana Affect The BrainDokumen3 halamanHow Does Marijuana Affect The BrainWanNurAtikahBelum ada peringkat
- Project Data Collection & Risk ReportingDokumen2 halamanProject Data Collection & Risk Reportinggambler yeagerBelum ada peringkat
- GMsetDokumen8 halamanGMsetdilo001Belum ada peringkat
- Desiderata: by Max EhrmannDokumen6 halamanDesiderata: by Max EhrmannTanay AshwathBelum ada peringkat
- Gerovital anti-aging skin care product guideDokumen10 halamanGerovital anti-aging skin care product guideכרמן גאורגיהBelum ada peringkat
- Specifications Sheet ReddyDokumen4 halamanSpecifications Sheet ReddyHenry CruzBelum ada peringkat
- Sundar KandvalmikiDokumen98 halamanSundar Kandvalmikifactree09Belum ada peringkat
- The Relevance of Vivekananda S Thought IDokumen16 halamanThe Relevance of Vivekananda S Thought IJaiyansh VatsBelum ada peringkat
- Bajaj Auto Company NewDokumen94 halamanBajaj Auto Company Newbhas_786Belum ada peringkat
- BMW Mini COoper Installation InstructionsDokumen1 halamanBMW Mini COoper Installation InstructionsEdiJonBelum ada peringkat
- CSC-1321 Gateway User Guide: Downloaded From Manuals Search EngineDokumen48 halamanCSC-1321 Gateway User Guide: Downloaded From Manuals Search EngineKislan MislaBelum ada peringkat