Pedoman Ibu Hamil
Diunggah oleh
Monyet...Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Pedoman Ibu Hamil
Diunggah oleh
Monyet...Hak Cipta:
Format Tersedia
[Downloaded free from http://www.nigerianjsurg.com on Wednesday, August 8, 2018, IP: 36.84.69.
67]
Review Article
Surgical Scales: Primary Closure versus Gastric Resection for
Perforated Gastric Ulcer ‑ A Surgical Debate
Mahir Gachabayov, Valentin Babyshin, Oleg Durymanov, Dmitriy Neronov1
Departments of Abdominal Perforated gastric ulcer is one of the most life‑threatening complications of peptic
Abstract
Surgery and 1ICU and
Anaesthesiology, Vladimir
ulcer disease with high morbidity and mortality rates. The surgical strategy for
City Clinical Hospital gastric perforation in contrast with duodenal perforations often requires consilium
of Emergency Medicine, and intraoperative debates. The subject of the debate is a 59‑year‑old male patient
Vladimir, Russia who presented with perforated giant gastric ulcer complicated by generalized
peritonitis and severe sepsis. The debate is based on a systematized table dividing
all factors into three groups and putting them on surgical scales. Pathology‑related
factors influencing the decision‑making are size and site of perforation, local tissue
inflammation, signs of malignancy, simultaneous complications of peptic ulcer,
peritonitis, and sepsis. Besides these factors, patient‑ and healthcare‑related factors
should also be considered.
Keywords: Gastrectomy, gastric resection, gastric ulcer, giant ulcer, perforated
ulcer, primary ulcer repair
Introduction before admission, L1–L2 intervertebral disc hernia
for which he had used nonsteroidal anti‑inflammatory
P erforated peptic ulcers are encountered in 2–14%
of patients with complicated peptic ulcer disease.[1]
Perforated peptic ulcers, especially gastric ulcers, are
drugs (NSAIDs). On admission, he had tachypnea (28–
30 breaths/min), tachycardia (108 beats/min),
associated with high mortality reaching to 41%.[2] hypotension (blood pressure [BP] =80/50 mmHg),
Surgical strategy with perforated duodenal ulcers having and hyperthermia (t = 38.2°C). There were board‑like
minimal risk of malignancy is clear, minor surgery being rigidity and positive peritoneal signs. His white blood
the goal. In case of perforated gastric ulcers (PGUs), cells (WBCs) count was 12.5 with 14% band forms.
almost every operation bears the question: “Which is the Abdominal X‑ray showed free gas under the diaphragm.
best choice? Minor or major surgery? Primary closure A clinical diagnosis of perforated peptic ulcer complicated
or gastric resection?” and requires multidimensional with peritonitis and sepsis was made. He was resuscitated
approach. This surgical debate took place in the in the Intensive Care Unit until physiological parameters
operation theater. were stable and transferred to the operating room when
his systolic BP was 140 mmHg.
Discussion
Operation
The subject of the debate
Laparotomy was performed which revealed generalized
Preoperatively
peritonitis. Upon revision, a large necrotic defect in the
A 59‑year‑old male patient from a rural place mesocolon was found [Figure 1]. The lesser sac was
was admitted to Vladimir City Clinical Hospital
of Emergency Medicine with 4 days history of
abdominal pain, fatigue, and hyperthermia up to Address for correspondence: Dr. Mahir Gachabayov,
39°C. The onset of pain was sudden and knife‑like. Department of Abdominal Surgery, Vladimir City Clinical
His medical history was significant for duodenal Hospital of Emergency Medicine, 600022,
Stavrovskaya Street, 6-73, Vladimir, Russia.
ulcer bleeding treated conservatively about 13 years E‑mail: ggachabayovmahir@gmail.com
Access this article online This is an open access article distributed under the terms of the Creative Commons
Attribution‑NonCommercial‑ShareAlike 3.0 License, which allows others to remix, tweak,
Quick Response Code: and build upon the work non‑commercially, as long as the author is credited and the new
Website: www.nigerianjsurg.com creations are licensed under the identical terms.
For reprints contact: reprints@medknow.com
How to cite this article: Gachabayov M, Babyshin V, Durymanov O, Neronov D.
DOI: 10.4103/1117-6806.199959 Surgical scales: Primary closure versus gastric resection for perforated gastric
ulcer - A surgical debate. Niger J Surg 2017;23:1-4.
© 2017 Nigerian Journal of Surgery | Published by Wolters Kluwer - Medknow 1
[Downloaded free from http://www.nigerianjsurg.com on Wednesday, August 8, 2018, IP: 36.84.69.67]
Gachabayov, et al.: Perforated gastric ulcers
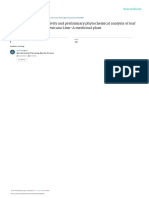
Figure 1: Destructive defect in the mesocolon Figure 2: Giant perforated gastric ulcer of the posterior wall of the antrum
opened, and a giant perforating gastric ulcer (with the Table 1: Factors influencing the choice of surgery for
diameter of 7 cm, Johnson Type V) on the posterior perforated gastric ulcer
wall of the antrum was found [Figure 2]. The strategic Pathology‑related factors
question emerged at this stage: What to do primary repair Pathomorphological factors
or gastric resection? To act in the most correct way, a Size of perforation
consilium was called to the operation theater, and the Location of perforated ulcer
strategy was debated. The oral debate in the operation Local tissue inflammation
theater took 3 to 5 min. Excision of the ulcer edges with Suspicion of malignancy
primary repair was the option chosen. A nasogastric Other complications and risk factors of peptic ulcer
tube (for decompression) and nasojejunal tube (for Complications
feeding) were placed. Peritoneal contamination
Presence of sepsis, severe sepsis, or septic shock
Postoperatively, he received intravenous fluids for Patient‑related factors
3 days with proton‑pump inhibitors and wide‑spectrum Age, gender
antibiotics. The patient was fed through the nasojejunal Comorbidities
tube for 4 days, and on the 5th postoperative day, the Healthcare‑related factors
tubes were removed and oral nutrition resumed. The Presence of a qualified surgeon
patient recovered uneventfully and was discharged on the Presence of facilities
10th postoperative day. The pathologist found no atypical
cells in the specimen. On the follow‑up after 4 months, large perforations.[3] Sarath Chandra et al. showed large
the patient was well. gastric perforations (with the diameter of >3 cm) in most
The debate cases to be an indication for resectional surgery while
not influencing the outcome.[4] The size of perforation
In the past, gastric resection was the procedure of choice
determines the outcome in elderly patients.[5] In our case,
for gastric ulcers. Nowadays, the success in the medical
the size of perforation required gastric resection.
treatment of gastric ulcers changed the vector of choice
toward omental patch closure, primary closure, and The location of perforated gastric ulcer
ulcer excision. Against this background, several factors Turner et al. recommended gastric resection for
influence the choice of any of these strategies thus prepyloric ulcers.[6] However, resectional surgery in
making PGU surgery, a challenge requiring consideration current practice is reserved mostly for Johnson Type I
of all these factors promptly. These factors could be and IV ulcers considering higher risk of malignancy.[7]
classified as it is shown in Table 1. In our case, the PGU is Johnson Type V located on the
Pathology‑related factors: Pathomorphological factors posterior wall of the antrum. Hence, the location does
The size of perforation not require resectional surgery.
Excision of the ulcer followed by omental patch Local tissue inflammation
or primary closure is practiced with small gastric Not having specific surgical treatment recommendations,
perforations. PGUs larger than 2 cm are considered to be the site of PGU and the secondary effects on the
2 Nigerian Journal of Surgery ¦ Volume 23 ¦ Issue 1 ¦ January-June 2017
[Downloaded free from http://www.nigerianjsurg.com on Wednesday, August 8, 2018, IP: 36.84.69.67]
Gachabayov, et al.: Perforated gastric ulcers
surrounding anatomical structures will determine the
necessary intervention.[8] This pathomorphologic aspect
includes two conditions: Local tissue changes during
the index procedure due to ulcer penetration and friable
tissues at the index procedure or re‑operation due to
long‑standing diffuse peritoneal contamination. Both
conditions are the parts of the other rubric complications.
However, this aspect is another viewpoint to them, so
that in both conditions, the emerging problem is technical
difficulty limiting primary closure. In our case, the ulcer
although penetrating the mesocolon did not significantly Figure 3: Surgical scales weighing factors influencing surgical strategy
alter the elasticity of the gastric wall. Hence, the extent for perforated gastric ulcer
of local tissue inflammation allows to perform primary
closure. increase in mortality while delays of 24 h and more are
associated with a 9‑fold increase in mortality.[16] In all
Suspicion of malignancy existing scoring systems such as Boey score,[17] Mannheim
Historically, surgeons were used to consider malignancy peritonitis index,[18] and peptic ulcer perforation score,[19]
in any case of PGU, and nonradical surgery was the extent of peritoneal contamination and septic signs
a concern that a malignant ulcer could be missed. such as hypotonia and organ failure is included. In our
However, several studies showed the frequency of case, generalized suppurative peritonitis and severe sepsis
malignant ulcers among all PGUs to be from 3% to are present, so primary closure is more appropriate.
14%.[9,10] In an emergency setting, frozen pathology is
Patient‑related factors: Age, gender, and comorbidity
mostly unavailable, so a clinicopathological pathway
of predicting malignancy including age, ulcer diameter, Boldly, advanced age is a risk factor increasing morbidity
perforation diameter, symptom duration, and WBC was and mortality what was shown in several studies. So et al.
reported by Ergul and Gozetlik.[11] Such pathologic showed that the age more than 65 was associated with
features as Johnson Type I and IV ulcers,[7] scalloped poor outcomes after emergency gastrectomy not depending
margins, and loss of rugal folds around ulcer,[12] regional on underlying disease.[20] Bulut et al. showed that the age
lymph node enlargement are thought to bear a high index more than seventy dramatically increases morbidity up to
of suspicion of malignancy. On the other hand, even if 30%.[21] In the study by Thorsen et al., females comprised
the PGU is a malignant ulcer, noncurative and palliative more than half of the cases, they were older, had more
gastric resections due to diffuse peritonitis should be comorbidities and higher Boey risk score.[22] Comorbidities
avoided; instead, two‑stage gastric resection (curative are also an important factor determining the outcome. That
R0 resection) following peritonitis recovery and detailed is why several scoring systems include comorbidities such
examinations should be performed as it was shown by as malignancy, AIDS, liver cirrhosis, chronic obstructive
Hata et al.[13] Hence, in cases of PGU treated by primary pulmonary disease, and chronic steroid use. Patient‑related
closure, an important point is ulcer excision.[10] According factors in our patient allow to perform gastric resection.
to the low index of suspicion of malignancy, in our case, Healthcare-related factors
primary closure with ulcer excision is better choice. Healthcare‑related factors are also essential so that even
Other complications and risk factors of peptic ulcer if gastrectomy is indicated and even if the patient is fit
The combination of PGU with other complications for major intervention, the absence of an experienced
of peptic ulcer is a positive indication of advanced, surgeon or facilities to perform a major surgery can
intractable ulcer disease requiring definitive surgical emerge to be a serious disturbance. In our case, there
treatment.[14] In patients with NSAID usage and were no such disturbances, so gastric resection could be
Helicobacter pylori infection, acid‑reducing surgery is performed.
recommended.[15] In our case, the absence of simultaneous The surgical scale emerging as a result of the debate is
peptic ulcer complication and the presence of NSAID shown in Figure 3.
usage do not require resectional surgery.
Pathology‑related factors: Complications Conclusion
Peritoneal contamination and sepsis are also the factors The decision‑making for the choice of surgery for
influencing the choice of surgery for PGU significantly. PGU is a multifaceted task requiring consideration
Delays in the treatment of PGU of >12 h result in a 3‑fold of several factors including pathology‑related,
Nigerian Journal of Surgery ¦ Volume 23 ¦ Issue 1 ¦ January-June 2017 3
[Downloaded free from http://www.nigerianjsurg.com on Wednesday, August 8, 2018, IP: 36.84.69.67]
Gachabayov, et al.: Perforated gastric ulcers
patient‑related, and healthcare‑related factors. Fabbri C, et al. Diagnosis and treatment of perforated or bleeding
Pathology‑related factors include pathomorphological peptic ulcers: 2013 WSES position paper. World J Emerg Surg
2014;9:45.
factors such as size and location of perforation, local 9. Madiba TE, Nair R, Mulaudzi TV, Thomson SR. Perforated gastric
tissue inflammation, suspicion of malignancy, other ulcer – Reappraisal of surgical options. S Afr J Surg 2005;43:58‑60.
simultaneous complications and risk factors of peptic 10. Hodnett RM, Gonzalez F, Lee WC, Nance FC, Deboisblanc R.
ulcer disease, and such complications as peritonitis and The need for definitive therapy in the management of perforated
sepsis. Patient‑related factors include age, gender, and gastric ulcers. Review of 202 cases. Ann Surg 1989;209:36‑9.
11. Ergul E, Gozetlik EO. Emergency spontaneous gastric
comorbidities, and healthcare‑related factors include the
perforations: Ulcus versus cancer. Langenbecks Arch Surg
presence of facilities and qualified surgeon. Each factor 2009;394:643‑6.
per se and their association depicting surgical scales is 12. Kumar P, Khan HM, Hasanrabba S. Treatment of perforated
important in decision‑making about the choice of surgical giant gastric ulcer in an emergency setting. World J Gastrointest
strategy. Surg 2014;6:5‑8.
13. Hata T, Sakata N, Kudoh K, Shibata C, Unno M. The best
Financial support and sponsorship surgical approach for perforated gastric cancer: One‑stage vs.
Nil. two‑stage gastrectomy. Gastric Cancer 2014;17:578‑87.
14. Moore SW, Fuller FW. Multiple simultaneous complications of
Conflicts of interest peptic ulcer. Am J Surg 1959;97:184‑90.
There are no conflicts of interest. 15. Nivatvongs S. Is there any role of acid reducing gastric
surgery in peptic ulcer perforation? J Med Assoc Thai
2005;88 Suppl 4:S373‑5.
References
16. Hermansson M, Staël von Holstein C, Zilling T. Surgical
1. Bertleff MJ, Lange JF. Perforated peptic ulcer disease: A review approach and prognostic factors after peptic ulcer perforation.
of history and treatment. Dig Surg 2010;27:161‑9. Eur J Surg 1999;165:566‑72.
2. Tsugawa K, Koyanagi N, Hashizume M, Tomikawa M, 17. Boey J, Choi SK, Poon A, Alagaratnam TT. Risk stratification in
Akahoshi K, Ayukawa K, et al. The therapeutic strategies perforated duodenal ulcers. A prospective validation of predictive
in performing emergency surgery for gastroduodenal factors. Ann Surg 1987;205:22‑6.
ulcer perforation in 130 patients over 70 years of age.
18. Linder MM, Wacha H, Feldmann U, Wesch G, Streifensand RA,
Hepatogastroenterology 2001;48:156‑62.
Gundlach E. The Mannheim peritonitis index. An instrument
3. Lulu DJ. Benign giant gastric ulcer. Am Surg 1971;37:357‑62. for the intraoperative prognosis of peritonitis. Chirurg
4. Sarath Chandra S, Kumar SS. Definitive or conservative surgery 1987;58:84‑92.
for perforated gastric ulcer? – An unresolved problem. Int J Surg 19. Møller MH, Engebjerg MC, Adamsen S, Bendix J, Thomsen RW.
2009;7:136‑9. The peptic ulcer perforation (PULP) score: A predictor of
5. Uccheddu A, Floris G, Altana ML, Pisanu A, Cois A, Farci SL. mortality following peptic ulcer perforation. A cohort study. Acta
Surgery for perforated peptic ulcer in the elderly. Evaluation Anaesthesiol Scand 2012;56:655‑62.
of factors influencing prognosis. Hepatogastroenterology 20. So JB, Yam A, Cheah WK, Kum CK, Goh PM. Risk factors
2003;50:1956‑8. related to operative mortality and morbidity in patients
6. Turner WW Jr., Thompson WM Jr., Thal ER. Perforated gastric undergoing emergency gastrectomy. Br J Surg 2000;87:1702‑7.
ulcers. A plea for management by simple closures. Arch Surg 21. Bulut OB, Rasmussen C, Fischer A. Acute surgical treatment of
1988;123:960‑4. complicated peptic ulcers with special reference to the elderly.
7. Rigopoulos A, Ramboiu S, Georgescu I. A critical evaluation World J Surg 1996;20:574‑7.
of surgical treatment of perforated ulcer. Curr Health Sci J 22. Thorsen K, Glomsaker TB, von Meer A, Søreide K, Søreide JA.
2011;37:75‑8. Trends in diagnosis and surgical management of patients with
8. Di Saverio S, Bassi M, Smerieri N, Masetti M, Ferrara F, perforated peptic ulcer. J Gastrointest Surg 2011;15:1329‑35.
4 Nigerian Journal of Surgery ¦ Volume 23 ¦ Issue 1 ¦ January-June 2017
Anda mungkin juga menyukai
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- Kha Thir 2021Dokumen8 halamanKha Thir 2021Monyet...Belum ada peringkat
- Chemical Properties and Probiotics Survivability of Symbiotic CocDokumen79 halamanChemical Properties and Probiotics Survivability of Symbiotic CocMonyet...Belum ada peringkat
- Rohaya 2019Dokumen7 halamanRohaya 2019Monyet...Belum ada peringkat
- 10 1088@1757-899X@523@1@012011Dokumen7 halaman10 1088@1757-899X@523@1@012011Monyet...Belum ada peringkat
- MoleculesDokumen13 halamanMoleculesMonyet...Belum ada peringkat
- JCDR 7 243Dokumen4 halamanJCDR 7 243Monyet...Belum ada peringkat
- Characterization Antimicrobes of Pliek U, A Traditional Spice of AcehDokumen6 halamanCharacterization Antimicrobes of Pliek U, A Traditional Spice of AcehMonyet...Belum ada peringkat
- Taskova ADokumen37 halamanTaskova AMonyet...Belum ada peringkat
- Lima-Filho 2013Dokumen17 halamanLima-Filho 2013Monyet...Belum ada peringkat
- Activity of Virgin Coconut Oil, Lauric Acid or Monolaurin in Combination With Lactic Acid Against Staphylococcus AureusDokumen17 halamanActivity of Virgin Coconut Oil, Lauric Acid or Monolaurin in Combination With Lactic Acid Against Staphylococcus AureusMonyet...Belum ada peringkat
- Cefepime Shows Good Efficacy and No Antibiotic Resistance in Pneumonia Caused by Serratia Marcescens and Proteus Mirabilis - An Observational StudyDokumen9 halamanCefepime Shows Good Efficacy and No Antibiotic Resistance in Pneumonia Caused by Serratia Marcescens and Proteus Mirabilis - An Observational StudyMonyet...Belum ada peringkat
- Gyawali 2014Dokumen90 halamanGyawali 2014Monyet...Belum ada peringkat
- Antimicrobial Natural ProductsDokumen17 halamanAntimicrobial Natural ProductsMonyet...Belum ada peringkat
- Art 20632Dokumen3 halamanArt 20632Monyet...Belum ada peringkat
- Stan 2021Dokumen25 halamanStan 2021Monyet...Belum ada peringkat
- Tekwu 2012Dokumen9 halamanTekwu 2012Monyet...Belum ada peringkat
- Sridhar 2021Dokumen20 halamanSridhar 2021Monyet...Belum ada peringkat
- Miethke M 2021Dokumen24 halamanMiethke M 2021Monyet...Belum ada peringkat
- Shekar 2022Dokumen7 halamanShekar 2022Monyet...Belum ada peringkat
- Khameneh 2019Dokumen28 halamanKhameneh 2019Monyet...Belum ada peringkat
- ArgemoneDokumen4 halamanArgemoneMonyet...Belum ada peringkat
- Appr MS Id 000539Dokumen5 halamanAppr MS Id 000539Monyet...Belum ada peringkat
- Antimicrobial Susceptibility and Minimum Inhibitory Concentration of Salmonella Enterica Isolates From Chickens in SomeDokumen11 halamanAntimicrobial Susceptibility and Minimum Inhibitory Concentration of Salmonella Enterica Isolates From Chickens in SomeMonyet...Belum ada peringkat
- Kusuma - WJPR - 1580448147Dokumen9 halamanKusuma - WJPR - 1580448147Monyet...Belum ada peringkat
- Antimicrobial Activity of Some Ethno-Medicinal Plants Used by Baiga Tribes From Amarkantak, India-With-Cover-Page-V2Dokumen9 halamanAntimicrobial Activity of Some Ethno-Medicinal Plants Used by Baiga Tribes From Amarkantak, India-With-Cover-Page-V2Monyet...Belum ada peringkat
- 210Dokumen3 halaman210Monyet...Belum ada peringkat
- 186 PDFDokumen4 halaman186 PDFMonyet...Belum ada peringkat
- 32 Vol. 7 Issue 9 September 2016 IJPSR RA 6515Dokumen5 halaman32 Vol. 7 Issue 9 September 2016 IJPSR RA 6515Monyet...Belum ada peringkat
- Antibacterial Activity of Mentha Longifolia Against SalmonellaDokumen6 halamanAntibacterial Activity of Mentha Longifolia Against SalmonellaMonyet...Belum ada peringkat
- 69 279 1 PBDokumen8 halaman69 279 1 PBMonyet...Belum ada peringkat
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- CriticalCare - ICU Skills ChecklistDokumen8 halamanCriticalCare - ICU Skills Checklistyash Inficare100% (2)
- Organic BrainDokumen48 halamanOrganic BrainAalia RanaBelum ada peringkat
- All Uworld Notes 2019 Nclex Nursing ResourcesDokumen152 halamanAll Uworld Notes 2019 Nclex Nursing Resourcesnene lewis100% (1)
- AntipyreticsDokumen20 halamanAntipyreticsJoshua VillarbaBelum ada peringkat
- Defect de Sept AtrialDokumen4 halamanDefect de Sept Atrial22194Belum ada peringkat
- MCQ EXAMS ENT 3rd edition الهيئة السعوديةDokumen162 halamanMCQ EXAMS ENT 3rd edition الهيئة السعوديةmirumirmisha92% (13)
- Resident PacketDokumen54 halamanResident PacketJorge Alberto100% (1)
- UVA Family Medicine QbankDokumen32 halamanUVA Family Medicine QbankjamesmgangBelum ada peringkat
- Family Names of DrugsDokumen1 halamanFamily Names of DrugsangelBelum ada peringkat
- 61st Annual Conference of Indian Society of Gastroenterology, Num 04 Virtual Diamond Jubilee ISGCON 2020, 19-20th December 2020Dokumen127 halaman61st Annual Conference of Indian Society of Gastroenterology, Num 04 Virtual Diamond Jubilee ISGCON 2020, 19-20th December 2020Chawki MokademBelum ada peringkat
- 26 Patofisiologi Edema FK Unhas TGL 5 Mei 2015Dokumen65 halaman26 Patofisiologi Edema FK Unhas TGL 5 Mei 2015sri ayu lestari wulandariBelum ada peringkat
- Jurnal Coomb Test PDFDokumen6 halamanJurnal Coomb Test PDFElang SudewaBelum ada peringkat
- Iron Deficiency Aneamia in Adults Gutjnl 2021 325210Dokumen22 halamanIron Deficiency Aneamia in Adults Gutjnl 2021 325210Bookgeek23Belum ada peringkat
- Specific Indications in Clinical PracticeDokumen58 halamanSpecific Indications in Clinical PracticeOccult Librarian100% (5)
- Case Presentation: Normal Spontaneous Deliver Cil Rmle IiDokumen31 halamanCase Presentation: Normal Spontaneous Deliver Cil Rmle IiJose Bryan NacillaBelum ada peringkat
- Multiple SclerosisDokumen21 halamanMultiple Sclerosisjhodane100% (1)
- Lower Limb Neurological ExamDokumen2 halamanLower Limb Neurological ExamRochelle BaileyBelum ada peringkat
- 初級婦產科超音波 陳郁菁醫師2Dokumen23 halaman初級婦產科超音波 陳郁菁醫師2陳威遠Belum ada peringkat
- Placental Insufficiency and Fetal Growth RestrictionDokumen7 halamanPlacental Insufficiency and Fetal Growth RestrictionAmalina Izati Nur IbrahimBelum ada peringkat
- ENT Deferential Diagnosis MEDADDokumen22 halamanENT Deferential Diagnosis MEDADReham AshourBelum ada peringkat
- Medicine Revision E6.5 (Medicalstudyzone - Com)Dokumen209 halamanMedicine Revision E6.5 (Medicalstudyzone - Com)Diya B johnBelum ada peringkat
- Pharmacotherapy Handbook - ALLERGIC RHINITISDokumen8 halamanPharmacotherapy Handbook - ALLERGIC RHINITISstella.gillesania.chenBelum ada peringkat
- Augmentin DdsDokumen12 halamanAugmentin DdsQureshi imtiyazBelum ada peringkat
- Pathology: Fluid & Hemodynamic Derangement - MCQDokumen5 halamanPathology: Fluid & Hemodynamic Derangement - MCQahmed jaradBelum ada peringkat
- DS & LTsDokumen11 halamanDS & LTsLemuel Glenn BautistaBelum ada peringkat
- SS DM MCH 2020 - 2021 Schedule Nov 6th Update PDFDokumen32 halamanSS DM MCH 2020 - 2021 Schedule Nov 6th Update PDFlakshminivas PingaliBelum ada peringkat
- A Productive and Friendly Epididymitis TreatmentDokumen10 halamanA Productive and Friendly Epididymitis TreatmentwozhiainiBelum ada peringkat
- Niferex Gastro-Resistant Capsule, Hard ENG SMPCDokumen7 halamanNiferex Gastro-Resistant Capsule, Hard ENG SMPCRabiatul 'raney' AdawiyahBelum ada peringkat
- TCM 09 2020 TCM ResourceDokumen103 halamanTCM 09 2020 TCM ResourceBrian LiBelum ada peringkat