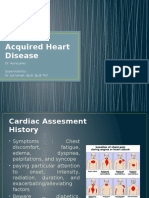
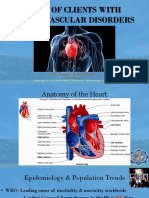
Contraindications: Indications For Surgery
Diunggah oleh
profJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Contraindications: Indications For Surgery
Diunggah oleh
profHak Cipta:
Format Tersedia
CARDIAC TRANSPLANTATION
Well-accepted therapeutic modality for the patient with end-stage heart disease
Majority of patients have ischemic (60%) or idiopathic (20%) cardiomyopathy, with the minority having
valvular or congenital problems
World-wide overall 1 year survival is 79%, with an annual mortality rate of 4%, and a 5 year survival
approximately 60%
Indications for surgery
• End-stage heart disease (e.g. EF< 20%, nonbypassable CAD) refractory to other surgical or medical
management
• NYHA III-IV symptoms with maximal medical therapy and prognosis for 1 year survival < 75%
• No other major organ or systemic disease
• Emotionally stable with social support
• Medically compliant and motivated
Contraindications
• Incurable malignancy
• Major systemic illness
• Irreversible major organ disease (e.g. renal, hepatic)
• Active systemic infection (e.g. Hep C, HIV)
• Emotional instability or acute psychiatric illness
• Age > 70 years
• Obesity
• Irreversible pulmonary hypertension (PVR > 6 Wood units)
• Severe COPD (FEV 1 < 1 L)
• Active drug addiction or alcoholism
Precardiac transplant assessment
• Consultations;
cardiology,
cardiovascular surgery,
respirology,
transplant immunology,
psychiatry,
psychology,
dental surgery,
social work,
chaplaincy,
transplant coordinator
• labs:
group and screen,
CBC,
ESR,
INR,
PTT,
lytes,
BUN,
creatinine,
uric acid,
glucose,
cholesterol,
triglycerides,
LFTs,
protein electrophoresis,
thyroid tests,
stool analysis,
urinalysis (24 hour)
• Investigations:
right and left heart catheterization,
2D Echo,
ECG,
PFTs,
ABG,
CXR,
Abdo U/S,
antibody screen (HBV, HCV, HIV),
HLA typing,
anti-HLA antibodies,
digoxin levels,
antibody titres (CMV, herpes simplex, EBV, toxoplasmosis)
• patients are optimized medically with diuretics, vasodilators (ACE inhibitors, hydralazine, B-
blockers), IABP, inotropes (digoxin), +/– LV assist device
• Donor hearts are considered from patients up to age 50-55
Contraindications to heart donation
major chest trauma
known cardiac disease
acute or chronic infection
prolonged cardiac arrest
HIV or Hep B/C positive
systemic malignancy
Matching is according to;
blood type (ABO match is mandatory to avoid hyper acute rejection),
body size and weight (should be within 25%) and
HLA tissue matching (if time allows)
Donor harvest
• The heart is inspected for evidence of coronary disease
• The SVC and IVC are clamped, the aorta is crossclamped, and cold crystalloid cardioplegia is
administered
• The heart is excised: as much SVC and IVC are preserved as possible, the pulmonary veins are divided,
the aorta is divided proximal to the crossclamp, and the distal main PA is divided
• The heart is bagged in cold saline and transported at 4-6ºC
Recipient operation
• The recipient is placed on CPB
• the diseased heart is excised leaving: a long cuff of SVC, a segment of low right atrium near the IVC,
the posterior wall of the left atrium, and the great vessels are incised just above the semilunar valves
• The donor heart is prepared by removing excess tissue
• The first suture line is started at the left atrial appendage of the donor heart and the free wall of the
left atrium is sewn and then the atrial septum
• The SVC and IVC are connected, followed by the pulmonary artery and then the aorta
Immediate postoperative management
• Keep heart rate 75-90 (may need pacing)
• keep CVP low with diuretics to improve RV function
• treat high PA pressures with NO, nitroglycerin, milrinone, etc.
• support the RV with inotropes and afterload reducers for high PA pressures • support LV if necessary
(IABP, inotropes)
• treat coagulopathy aggressively
• monitor for, prevent and treat other organ system failure (renal, respiratory, hepatic, and
neurological)
Immunosuppression
• The goal of immunosuppression is selective modulation of the recipient's immune response to prevent
rejection while maintaining defenses against infection and neoplasia, and minimizing toxicity
• Immunosuppression protocols include rabbit anti-thymocyte serum (RATS), OKT3, azathioprine, solu-
medrol, cyclosporine, FK506 (tacrolimus) and mycophenolate mofetil (Cellcept)
Complications
• Rejection
• The majority of transplant patients experience some form of rejection, though less than 5%
have hemodynamic compromise
• No noninvasive tests to detect rejection, and the gold standard remains endomyocardial
biopsies
• Risk of acute rejection is greatest during the first 3 months after transplant
• Infection
• Bacterial and viral infections predominate, although fungal ( Candida) and protozoan (PCP,
toxoplasmosis) are noted in 10% of patients
• Fevers, rising WBC counts and abnormal CXR's must be aggressively evaluated
• Allograft coronary artery disease
• Approximately 50% develop graft CAD within 5 years of transplantation
• Graft vasculopathy is the most common cause of late death following transplantation
• may reduce rate of graft CAD with diltiazem and statins
• Malignancy
• develop in 15% of cardiac transplant recipients
• Second most common cause of late death following transplantation
• Cutaneous neoplams most common, followed by non-Hodgkin's lymphoma and lung cancer
• Immunosuppressive medication side effects
include hypertension (cyclosporine),
hyperlipidemia (cyclosporine, steroids),
nephrotoxicity (cyclosporine),
GI problems (steroids),
osteopenic bone disease (steroids)
Anda mungkin juga menyukai
- Nursing: Lab Values: a QuickStudy Laminated 6-Page Reference GuideDari EverandNursing: Lab Values: a QuickStudy Laminated 6-Page Reference GuideBelum ada peringkat
- HESI Study Guide Psychiatric NursingDokumen26 halamanHESI Study Guide Psychiatric NursingDean Winchester100% (4)
- Cardiac Surgery MCQDokumen43 halamanCardiac Surgery MCQprofarmah100% (7)
- Heart Failure: Abdul Hafiz AliasDokumen19 halamanHeart Failure: Abdul Hafiz AliasAbdul Hafiz Alias100% (5)
- Cerebrovascular AccidentDokumen26 halamanCerebrovascular AccidentMustafa Aadan100% (1)
- 3.preoperative Patient Assessment and ManagementDokumen76 halaman3.preoperative Patient Assessment and Managementoliyad alemayehuBelum ada peringkat
- Hepato-Biliary System 26.4.2016Dokumen59 halamanHepato-Biliary System 26.4.2016S B SayedBelum ada peringkat
- Basic Priciples of Heart SurgeryDokumen6 halamanBasic Priciples of Heart SurgeryprofarmahBelum ada peringkat
- Blood TransfusionDokumen58 halamanBlood Transfusionmsat72100% (12)
- Eight Hallmarks of Cancer ExplainedDokumen40 halamanEight Hallmarks of Cancer ExplainedArnab KalitaBelum ada peringkat
- Annex A. ChecklistDokumen2 halamanAnnex A. ChecklistroseannurakBelum ada peringkat
- Coronary Arterial Disease: S Chapter 60 1657Dokumen26 halamanCoronary Arterial Disease: S Chapter 60 1657Staen KisBelum ada peringkat
- Infective EndocarditisDokumen18 halamanInfective EndocarditisSam100% (1)
- CABGDokumen3 halamanCABGprofarmahBelum ada peringkat
- Septic Shock: Rashmika Magan Roll No. 15Dokumen29 halamanSeptic Shock: Rashmika Magan Roll No. 15Rashmika MaganBelum ada peringkat
- Treatment of Endometriosis in Women Desiring FertilityDokumen23 halamanTreatment of Endometriosis in Women Desiring FertilityVaisnavi Muthoovaloo67% (3)
- 2014 Fundamentals of Skeletal Radiology, 4eDokumen239 halaman2014 Fundamentals of Skeletal Radiology, 4eLuís RobertoBelum ada peringkat
- Acquired Heart Disease EditedDokumen63 halamanAcquired Heart Disease Editedapalah_niBelum ada peringkat
- Acquired Heart Disease Edited2Dokumen50 halamanAcquired Heart Disease Edited2apalah_niBelum ada peringkat
- Course 3 Liver and Heart Transplantation PDFDokumen22 halamanCourse 3 Liver and Heart Transplantation PDFVladimir PetreBelum ada peringkat
- Anaesthetic Management of Congenital Heart DiseasesDokumen56 halamanAnaesthetic Management of Congenital Heart DiseasesShehan WijayasiriwardanaBelum ada peringkat
- 4.massive HemorrhageDokumen44 halaman4.massive HemorrhageyeabsraBelum ada peringkat
- DR AGUS SETIYANA Adult Congenital Heart Disease APDokumen25 halamanDR AGUS SETIYANA Adult Congenital Heart Disease APryandikaBelum ada peringkat
- HPB Adverse Transfusion ReactionDokumen26 halamanHPB Adverse Transfusion ReactionFransiscus RivaldyBelum ada peringkat
- DR - Sfeir Principles+of+Cardiac+SurgeryDokumen91 halamanDR - Sfeir Principles+of+Cardiac+SurgeryFrida AtallahBelum ada peringkat
- Pre OpDokumen14 halamanPre OpReem IssaBelum ada peringkat
- Cardiogenic Shock Management UpdateDokumen49 halamanCardiogenic Shock Management UpdateelsarahmiBelum ada peringkat
- Sepsis 3 HossamDokumen76 halamanSepsis 3 HossamHossam atefBelum ada peringkat
- Hypertension GuideDokumen25 halamanHypertension GuideBulborea MihaelaBelum ada peringkat
- Blood Transfusion Blood Grouping and Cross MatchingDokumen46 halamanBlood Transfusion Blood Grouping and Cross MatchingHa LeemBelum ada peringkat
- 5in - Cardiac TransplantDokumen18 halaman5in - Cardiac TransplantAsim Kumar BiswasBelum ada peringkat
- Hypertensive Emergencies: Sulaiman Usaid G. MBCHB V Facilatator: DR Jack TDokumen44 halamanHypertensive Emergencies: Sulaiman Usaid G. MBCHB V Facilatator: DR Jack TUsaid SulaimanBelum ada peringkat
- Liver TransplantationDokumen17 halamanLiver Transplantationa_m_elsheemy1931Belum ada peringkat
- Hypertension: Dr. Lucia Mazur-Nicorici Md. PHDDokumen34 halamanHypertension: Dr. Lucia Mazur-Nicorici Md. PHDValerianBîcosBelum ada peringkat
- Understanding Cardiomyopathy: Causes, Symptoms and TreatmentDokumen54 halamanUnderstanding Cardiomyopathy: Causes, Symptoms and TreatmentDanny DesuBelum ada peringkat
- Cardiac TransplantDokumen135 halamanCardiac TransplantNakka SrikanthBelum ada peringkat
- Management of Cerebrovascular AccidentsDokumen42 halamanManagement of Cerebrovascular Accidentsepic sound everBelum ada peringkat
- Anesthesia for Liver TransplantationDokumen54 halamanAnesthesia for Liver TransplantationPeeyoosh RaiBelum ada peringkat
- Seminar On TransplantationDokumen53 halamanSeminar On Transplantationamox woldieBelum ada peringkat
- Heart FailureDokumen28 halamanHeart FailureStella CooKeyBelum ada peringkat
- Leukamia and Transfusion MedicineDokumen26 halamanLeukamia and Transfusion MedicineSamuel kuriaBelum ada peringkat
- Ucm 484611Dokumen92 halamanUcm 484611jackytungadiBelum ada peringkat
- Heart Transplant ContentDokumen17 halamanHeart Transplant ContentrajBelum ada peringkat
- Surgery Slide 6 - Blood TransfusionsDokumen54 halamanSurgery Slide 6 - Blood TransfusionsEman NazzalBelum ada peringkat
- Acute Heart Failure and Pulmonary EdemaDokumen48 halamanAcute Heart Failure and Pulmonary EdemaSol Gat ChupataBelum ada peringkat
- Pre Operative AssessmentDokumen33 halamanPre Operative AssessmentShimmering MoonBelum ada peringkat
- Model Answer -I & II سبتمبر 2015تحريريDokumen12 halamanModel Answer -I & II سبتمبر 2015تحريريAmr El TaherBelum ada peringkat
- 23 May 2011 Peerapat Thaisiam Yossavadee RuamcharoenDokumen109 halaman23 May 2011 Peerapat Thaisiam Yossavadee RuamcharoenRapid MedicineBelum ada peringkat
- 01 Cardiovascular IDokumen72 halaman01 Cardiovascular IcoriezaBelum ada peringkat
- Sudden Cardiac Arrest: DiscussionDokumen19 halamanSudden Cardiac Arrest: DiscussionIza Singson-CristobalBelum ada peringkat
- Pulmonary Embolism: Diagnosis, Treatment, and Prevention Philip Keith March 26, 2008Dokumen24 halamanPulmonary Embolism: Diagnosis, Treatment, and Prevention Philip Keith March 26, 2008Fahd Abdullah Al-refaiBelum ada peringkat
- Eisenmeger Syndrome Discuss The Pathology and ManagementDokumen33 halamanEisenmeger Syndrome Discuss The Pathology and ManagementNdenwaneku OkuwaBelum ada peringkat
- Presentation2 HEMATOLOGIC CCDokumen62 halamanPresentation2 HEMATOLOGIC CCnucahersheyskatBelum ada peringkat
- Congestive Heart Failure (CHF) : Dr. Shneifi AminDokumen36 halamanCongestive Heart Failure (CHF) : Dr. Shneifi Amincarmitjulya228Belum ada peringkat
- Master File 2003 - Body As A WholeDokumen32 halamanMaster File 2003 - Body As A Wholeobinna12Belum ada peringkat
- Topic Gyne ERASDokumen60 halamanTopic Gyne ERASCrown SakulprakopkitBelum ada peringkat
- Atrial FibrillationDokumen50 halamanAtrial Fibrillationkapil khanalBelum ada peringkat
- Anesthesia Lecture 3Dokumen25 halamanAnesthesia Lecture 3drhiwaomer100% (2)
- HTN and CHFDokumen29 halamanHTN and CHFkiflomBelum ada peringkat
- Stroke Prevention and Management Guideline SummaryDokumen24 halamanStroke Prevention and Management Guideline Summarynisha24100% (1)
- 02.emergency CardiologyDokumen135 halaman02.emergency Cardiologyapi-19916399Belum ada peringkat
- Aortic Stenosis: History & ExamDokumen36 halamanAortic Stenosis: History & ExamMicija CucuBelum ada peringkat
- Posterior reversible encephalopathy syndrome (PRES) causes and treatmentDokumen33 halamanPosterior reversible encephalopathy syndrome (PRES) causes and treatmentMaroofAliBelum ada peringkat
- Cardio Part 1Dokumen41 halamanCardio Part 1Jaylord VerazonBelum ada peringkat
- Adverse Effects of Blood TransfusionDokumen3 halamanAdverse Effects of Blood Transfusionay254Belum ada peringkat
- Icu 2Dokumen57 halamanIcu 2astewale tesfieBelum ada peringkat
- Renal TransplantationDokumen49 halamanRenal TransplantationEthan Merza EctoleBelum ada peringkat
- Emergent Treatment of Aortic Rupture in Acute Type B DissectionDokumen7 halamanEmergent Treatment of Aortic Rupture in Acute Type B DissectionprofarmahBelum ada peringkat
- Discordant Atrioventricular Connections 1Dokumen1 halamanDiscordant Atrioventricular Connections 1profarmahBelum ada peringkat
- Central Aortic Cannulation For Minimally Invasive Mitral Valve Surgery Through Right MinithoracotomyDokumen2 halamanCentral Aortic Cannulation For Minimally Invasive Mitral Valve Surgery Through Right MinithoracotomyprofarmahBelum ada peringkat
- Cardiac Post Opt OrdersDokumen1 halamanCardiac Post Opt OrdersprofarmahBelum ada peringkat
- CPRDokumen10 halamanCPRprofarmahBelum ada peringkat
- Cardiac AnasthesiaDokumen3 halamanCardiac AnasthesiaprofarmahBelum ada peringkat
- Common Post Operative Complication and ManagementDokumen7 halamanCommon Post Operative Complication and ManagementprofarmahBelum ada peringkat
- Current Status of Arterial Grafts For Coronary Artery Bypass GraftingDokumen4 halamanCurrent Status of Arterial Grafts For Coronary Artery Bypass GraftingprofarmahBelum ada peringkat
- Congenital Heart Surgery ManagementDokumen9 halamanCongenital Heart Surgery ManagementprofarmahBelum ada peringkat
- Chest Wall and Sternal Resection and ReconstructionDokumen5 halamanChest Wall and Sternal Resection and ReconstructionprofarmahBelum ada peringkat
- Central Aortic Cannulation For Minimally Invasive Mitral Valve Surgery Through Right MinithoracotomyDokumen2 halamanCentral Aortic Cannulation For Minimally Invasive Mitral Valve Surgery Through Right MinithoracotomyprofarmahBelum ada peringkat
- Cabg 2Dokumen4 halamanCabg 2profarmahBelum ada peringkat
- Brom's Three-Patch Aortoplasty for Supravalvar Aortic StenosisDokumen6 halamanBrom's Three-Patch Aortoplasty for Supravalvar Aortic StenosisprofarmahBelum ada peringkat
- Aortic Valve RepiarDokumen6 halamanAortic Valve RepiarprofarmahBelum ada peringkat
- BYPASSDokumen2 halamanBYPASSprofarmahBelum ada peringkat
- Aorta Replacement and Repair Thoracic Aortic DissectionDokumen3 halamanAorta Replacement and Repair Thoracic Aortic DissectionprofarmahBelum ada peringkat
- Aortic Dissection and Aneurysm 2Dokumen13 halamanAortic Dissection and Aneurysm 2profarmahBelum ada peringkat
- Multiple Bilateral Basal Air Fluid Levels See Close Up View BelowDokumen1 halamanMultiple Bilateral Basal Air Fluid Levels See Close Up View BelowprofarmahBelum ada peringkat
- Aortic Arch Replacement With Frozen Elephant TrunkDokumen6 halamanAortic Arch Replacement With Frozen Elephant TrunkprofarmahBelum ada peringkat
- Left Lower Lobe Atelectasis CT FindingsDokumen1 halamanLeft Lower Lobe Atelectasis CT FindingsprofarmahBelum ada peringkat
- Left Hyper Lucency Left Hemithorax Larger Air in Pleural Cavity (No Vascular Markings) Atelectatic Lung (Upper Arrow) Bleb (Lower Arrow)Dokumen1 halamanLeft Hyper Lucency Left Hemithorax Larger Air in Pleural Cavity (No Vascular Markings) Atelectatic Lung (Upper Arrow) Bleb (Lower Arrow)profarmahBelum ada peringkat
- EmpyemaDokumen1 halamanEmpyemaprofarmahBelum ada peringkat
- Pleural EffusionDokumen10 halamanPleural EffusionprofarmahBelum ada peringkat
- BronchgramDokumen1 halamanBronchgramprofarmah100% (1)
- Calcified Nodes Calcified Nodules in Lungs: HistoplasmosisDokumen1 halamanCalcified Nodes Calcified Nodules in Lungs: HistoplasmosisprofarmahBelum ada peringkat
- PneumoniaDokumen7 halamanPneumoniaprofarmahBelum ada peringkat
- Treatment of TB in Adults: by Dr. Irfhan Ali Hyder AliDokumen45 halamanTreatment of TB in Adults: by Dr. Irfhan Ali Hyder AliInspireGutsBelum ada peringkat
- College of Nursing: Pharmacology Drug StudyDokumen2 halamanCollege of Nursing: Pharmacology Drug StudyChristine Pialan SalimbagatBelum ada peringkat
- Suz 183Dokumen29 halamanSuz 183Benny Chris TantoBelum ada peringkat
- MBBS - General Medicine Reg Id: KMC - 142105 RX ID: 406824261Dokumen1 halamanMBBS - General Medicine Reg Id: KMC - 142105 RX ID: 406824261Dipam HalderBelum ada peringkat
- EMT Training at Mansion Mandiri HotelDokumen4 halamanEMT Training at Mansion Mandiri Hotelyuna triazBelum ada peringkat
- Distraksi Menonton Efektif Menurunkan Nyeri Ringan Pasien: Congestive Heart Failure (CHF)Dokumen7 halamanDistraksi Menonton Efektif Menurunkan Nyeri Ringan Pasien: Congestive Heart Failure (CHF)Devy YahyaBelum ada peringkat
- Multiple Births Carrying Multiples:-Triplets, Quadruplets, Quintuplets, SextupletsDokumen5 halamanMultiple Births Carrying Multiples:-Triplets, Quadruplets, Quintuplets, SextupletsSheryll Almira HilarioBelum ada peringkat
- Nursing Care of a Patient with Hypovolemic ShockDokumen46 halamanNursing Care of a Patient with Hypovolemic ShockBianca MaeBelum ada peringkat
- Maternity Clinical Network Contact DetailsDokumen18 halamanMaternity Clinical Network Contact DetailsAlina-Gabriela MarinBelum ada peringkat
- Brain 101 Info (Merged) PDFDokumen186 halamanBrain 101 Info (Merged) PDFrosyuaBelum ada peringkat
- Pharmacology Lab (1) : Routes of Drug AdministrationDokumen14 halamanPharmacology Lab (1) : Routes of Drug AdministrationBotan AbdullahBelum ada peringkat
- GERD Nursing CareDokumen9 halamanGERD Nursing CareTrisha ArizalaBelum ada peringkat
- Sodium Chromate Anhydrous PDFDokumen6 halamanSodium Chromate Anhydrous PDFErika WidiariniBelum ada peringkat
- Predictions Using Data Mining and Case Based Reasoning A Case Study For RetinopathyDokumen4 halamanPredictions Using Data Mining and Case Based Reasoning A Case Study For RetinopathyBiraj kumar BholBelum ada peringkat
- Introduction To Epidemiology of Infection Diseases PDFDokumen17 halamanIntroduction To Epidemiology of Infection Diseases PDFRovaidKhanBelum ada peringkat
- Unconventional Fixed Partial Denture: A Simple Solution For Aesthetic RehabilitationDokumen4 halamanUnconventional Fixed Partial Denture: A Simple Solution For Aesthetic RehabilitationAdvanced Research PublicationsBelum ada peringkat
- Heritage Health - Pre Auth FormDokumen6 halamanHeritage Health - Pre Auth FormBOOKREADER_NOWBelum ada peringkat
- SDL 3 MCN 1Dokumen3 halamanSDL 3 MCN 1Milagros Florita100% (1)
- Nurs FPX 4050 Assessment 4 Final Care Coordination PlanDokumen6 halamanNurs FPX 4050 Assessment 4 Final Care Coordination PlanEmma WatsonBelum ada peringkat
- Unit 4: Medical EmergenciesDokumen44 halamanUnit 4: Medical EmergenciesMR々๛ AKMツBelum ada peringkat
- Progress in Retinal and Eye Research: Contents Lists Available atDokumen40 halamanProgress in Retinal and Eye Research: Contents Lists Available atSalsa BillaBelum ada peringkat
- Nursing Skills Checklist - RTDokumen6 halamanNursing Skills Checklist - RTapi-309674272Belum ada peringkat
- Fixed Prosthodontic Ii: Department of Fixed ProsthodonticsDokumen70 halamanFixed Prosthodontic Ii: Department of Fixed Prosthodonticsعبد الرحمن خالد الزميليBelum ada peringkat
- Jadwal Emsb FebDokumen2 halamanJadwal Emsb FebArdianto SucintaBelum ada peringkat