Danger Zone Botox
Diunggah oleh
Nur CameliaHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Danger Zone Botox
Diunggah oleh
Nur CameliaHak Cipta:
Format Tersedia
2.
0 ANCC
Aesthetic Department CE Contact Hours
Avoiding the “Danger Zones” When Injecting
Neurotoxins
Connie Brennan, RN, CPSN, CANS, CPC
INTRODUCTION seeking cosmetic improvement in greater numbers than
ever before. (Koblenzer, 2011)
Aesthetic medicine is a respected and well-accepted field
of medicine; it is characterized by minimally invasive
This field has seen a 13% increase since 2012 with a
techniques and services that utilize injectables, lasers,
total of 9.5 million nonsurgical procedures (ASAPS, 2013).
and other procedures, which require no surgery or gen-
According to the American Society of Aesthetic Plastic
eral anesthesia. The goals of aesthetic medicine are to
Surgeons (ASAPS), the top five nonsurgical cosmetic pro-
maintain a natural and healthy appearance and to assist
cedures in 2013 were the following: treatments utilizing
clients in looking their best. Advancements in aesthetic
Botulinum toxin type A (3,766,148 procedures, up 15.6%),
techniques and technology allow these procedures to be
hyaluronic acid dermal fillers (1,872,172 procedures, up
safely and effectively conducted in an office by certified,
31.5%), laser hair removal (901,571 procedures, up 2%),
experienced, and skilled aesthetic medical providers.
microdermabrasion (479,865 procedures, down 3.8%),
and photorejuvenation (456,613 procedures, up 35.3%)
Today, more than any prior generation, our current con- (ASAPS, 2013).
sensual beauty ideal of both face and body, male and Botulinum neurotoxins, the top cosmetic procedure
female is generated to a large extent by our exposure performed today (ASAPS, 2013), are proteins synthesized
to omnipresent advertising by the cosmetic, fashion, by clostridial bacteria–-isolated, purified, and formulated
and media industries, and most recently by some of our into specific products in a complex series of steps that are
colleagues. (Koblenzer, 2011) strictly regulated by the governmental agencies in most
countries where the products are approved. Neurotoxins
Many regard aesthetic medical treatments as a normal are regulated by the Food and Drug Administration (FDA)
part of their health and beauty regime. as biologics. Biologics are required to demonstrate effica-
cy, safety, and reproducibility in their manufacture before
Our culture is a culture of youth, and as the population being granted a formal indication. There are currently
ages, and as economic conditions deteriorate, men and three commercially available neurotoxins (i.e., Botulinum
women are tending to work longer and to retire at a Toxin Type A) available in the United States (Table 1).
greater age, thus increasing competition in the work- Every aesthetic injectable product has its limitations,
place. In order to remain competitive, men like women and every aging face is unique. Knowledge of how the
are struggling to look younger, healthier, more physically skin aging influences the position of vulnerable muscle
active, and more consonant with the current ideal of locations, the specific techniques used to safely admin-
masculine good looks. Thus both men and women are ister each neurotoxin, what specific “danger zones” to
avoid and what to do if complications occur, will ensure
that the aesthetic provider is well informed and prepared
Connie Brennan, RN, CPSN, CANS, CPC, is currently the Director of
Medical Aesthetic Education at the Center for Advanced Aesthetics at Life
to safely deliver optimal clinical outcomes.
Time Fitness and President/Founder of Aesthetic Enhancement Solutions,
LLC. Connie is a licensed registered nurse in 10 states and has earned
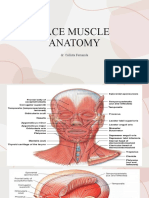
advanced certifications in aesthetic injectables, laser resurfacing, skin FACIAL AND MUSCLE ANATOMY
care, sclerotherapy, and perioperative nursing over the course of 26 years
in aesthetic medicine. Connie has worked as an expert alongside the Complete understanding of the anatomical locations of
ASPSN task force in creating the first Certified Aesthetic Nurse Specialist vulnerable muscle structures, as well as how facial aging
(CANS) examination.
or previous surgical alterations may change the structure
The author is a consultant to Allergan, Inc., Galderma Laboratories, L. P.,
and Nordson Micromedics, Inc., but has not received any funding to write
orientation, will aid the aesthetic provider in identifying
or publish this article. critical “danger zones” to avoid during the neurotoxin
Address correspondence to Connie Brennan, RN, CPSN, CANS, CPC, 5905 injection process (Seckel, 1994). As descending and thin-
Troy Lane, N, Plymouth, MN 55446 (e-mail: info@conniebrennanRN.com). ning skin may make it easier to see these important struc-
DOI: 10.1097/PSN.0000000000000064 tures, prior facial surgeries can have the opposite impact,
Plastic Surgical Nursing www.psnjournalonline.com 173
Copyright © 2014 American Society of Plastic Surgical Nurses. Unauthorized reproduction of this article is prohibited.
PSN-D-14-00042_LR 173 28/11/14 9:45 PM
Aesthetic Department
TABLE 1.Neurotoxins (i.e., Botulinum Toxin Type A) Available for Cosmetic Use in the United States
Name Nonproprietary Name Year of Glabellar Line Indication Year of Other Facial Indication(s)
a
Botox Cosmetic Onabotulinumtoxin A 2002 2013 (crow’s feet)
Dysportb Abobotulinumtoxin A 2009
Xeominc Incobotulinumtoxin A 2011
a
Allergan, Inc., Irvine, CA.
b
Galderma Laboratories, L.P., Ft., Worth, TX.
c
Merz Pharmaceuticals, LLC, Greensboro, NC.
making the location of these anatomical “danger zones” overlapping, or inserting muscles). Adverse events of
more difficult to assess. It is very important to take a com- longer duration that can be serious and are technique-
plete medical history of all prior facial surgeries during dependent are the following: blepharoptosis, brow pto-
the initial aesthetic consultation (Brennan, 2012). sis, diplopia, blurred vision or diminished visual acuity,
Intimate knowledge of the anatomy of muscles is just diminished tearing and xerophthalmia with or without
as crucial as their relative position on the face. For exam- keratitis, ectropion (potentially leads to xerophthalmia),
ple, the origin of a muscle is the bone, typically proximal, lagophthalmus (potentially leads to exposure keratitis),
which has greater mass and is more stable during a con- dysphagia, dysarthria, and dysphonia (Benedetto, 2011).
traction than a muscle’s insertion (Dorland, 2003). The in- Figures 1a and 1b identify the “danger zones” to be
sertion of a muscle is the structure it attaches to and tends aware of during neurotoxin injections. Key muscles/
to be moved by the contraction of the muscle (Dorland, anatomical locations to avoid (and associated presenta-
2003). Most of the muscles of facial expression are not at- tion) include the following: frontalis (mid brow ptosis),
tached to bone—rather they have soft tissue attachments. levator palpebrae (lid ptosis), levator labii superioris alae-
They tend not to move the body, but rather to move que nasi (lip ptosis), zygomaticus (lip ptosis), orbicularis
the skin and related structures to facilitate communica- oculi (diplopia), depressor labii inferioris, mentalis, and
tion (Spencer, 2011). The muscles of facial expression are depressor anguli oris (DAO; lip asymmetry).
connected to the overlying skin through the layer known Practical considerations for the aesthetic provider
as the superficial muscular aponeurotic system (SMAS). to remember as they prepare to inject neurotoxin into
When the underlying muscle contracts, the overlying skin these key muscles/anatomical locations include the
moves with it. The muscles of mastication, such as the following:
masseter and temporalis, have boney attachments and
Frontalis:
function to move the jaw in a way similar to the muscles
elsewhere on the body (Spencer, 2011). • Considered an elevator muscle of the upper face
Since the optimal chemodenervation effect with a neuro- • Associated with mid brow ptosis
toxin occurs when the belly of muscle is the target, know- • Caution must be used to not weaken the frontalis
ing the origin and insertion point will increase the prob- too close to the eyebrows. As a general principle,
ability of success of each neurotoxin injection. Similarly, injections should always be at least 1 cm above
knowledge of the relative thickness of the muscle is critical the eyebrow, so muscle fibers of the frontalis will
so the depth of the muscle belly can be approximated. remain functional and hold the eyebrows up.
Remember to think three dimensionally before you (Spencer, 2011)
inject—the specific location of each facial muscle, the inser-
Levator palpebrae:
tion and origin of the muscle being targeted, as well as the
relative thickness of each muscle, so accurate triangulation • Associated with lid ptosis
of the target muscle is accomplished with each neurotoxin • Occurs when diffusion of a significant amount of
injection. Injection site accuracy and precision during the in- toxin to the levator palpebrae during glabellar in-
jection process will decrease the potential of adverse events. jections
• Instruct the patient to contract their muscle, hold,
or “gently pinch” the corrugator supercilii muscle
“DANGER ZONES” ASSOCIATED WITH with your thumb and finger and inject 1 cm above
NEUROTOXIN COMPLICATIONS the orbital rim. Place the thumb of the noninject-
Certain regions of the face are at a higher risk for ing hand on the superior orbital rim to avoid a po-
complications due to the structures that lie beneath or sur- tential diffusion of the neurotoxin into the levator
rounding the intended muscles for injection (e.g., deeper, palpebral muscle.
174 www.psnjournalonline.com Volume 34 Number 4 October–December 2014
Copyright © 2014 American Society of Plastic Surgical Nurses. Unauthorized reproduction of this article is prohibited.
PSN-D-14-00042_LR 174 28/11/14 9:45 PM
Aesthetic Department
massage lower injection point in case of diffusion
into the zygomaticus.
Depressor labii inferioris, DAO, and mentalis:
• Associated with asymmetry, dysfunctional mouth,
ptosis of the lower lip, and difficulties with eating
or drinking
• Avoid being too high, too close to the corner of
the mouth, too medial, or too close to the lower
lip with injection points
TYPICAL PRESENTATIONS OF NEUROTOXIN-
RELATED ADVERSE EVENTS
Within 1–3 days postneurotoxin treatment session, the cli-
ent may become aware of an adverse event (AE) associ-
ated with their neurotoxin injections and they will quickly
alert the aesthetic provider that “something is not right.”
The typical presentations of neurotoxin AEs, as a function
of the anatomical locations, include the following:
Mid brow ptosis:
• Feeling of heaviness
• Looking tired
• Difficulty putting eye make up on
Eyelid ptosis:
• Eyelid(s) feel(s) heavy or may not open at all
• Iris of eye partially covered
Lip drop:
• “Crooked” smile
• Upper teeth less visible
• Potential functional impairment of lip—sipping
may be difficult
• Looks like client “had a stroke”
• Difficulty with articulation
FIGURE 1. (a). The facial muscles and “danger zones” (black Xs).
(b) Model with “danger zones” (black Xs) identified. (Used with Lower lip asymmetry:
permission.)
• “Crooked” smile
• Lower lip looks uneven
Levator labii superioris alaeque nasi:
• Sipping through a straw may lead to spills/drooling
• Associated with lip ptosis, asymmetry, speaking dif- • Difficulty with speech and suction
ficulty
• Injection points on nasalis during “bunny line”
injections should be superficial and in a wheal WHAT TO DO IN THE EVENT OF AN AE
formation. Do not inject laterally down the nasal ASSOCIATED WITH A NEUROTOXIN
sidewalls.
The gradual appearance of ptosis postinjection is the
Zygomaticus: most frequent presentation of a neurotoxin injection AE.
The practical options that the aesthetic provider has in
• Associated with lip ptosis, asymmetry, smile impair-
the event of a neurotoxin AE are limited and include the
ment (due to imbalance of the lip elevators and
following:
cheek ptosis)
• Injection points should remain in the orbicularis • Let the neurotoxin wear away—typically 2–3 months
oculi for crow’s feet injections; be careful not to for a neurotoxin’s effect to diminish
Plastic Surgical Nursing www.psnjournalonline.com 175
Copyright © 2014 American Society of Plastic Surgical Nurses. Unauthorized reproduction of this article is prohibited.
PSN-D-14-00042_LR 175 28/11/14 9:45 PM
Aesthetic Department
• Adjust adjacent musculature to attain symmetry Vigorous massage to the area after the injection of a
or treat the opposing musculature if possible, neurotoxin can cause it to spread and diffuse beyond the
especially in the case of ptosis targeted area and produce the same untoward adverse
results, even if the dosing is appropriate and the injection
Many experts anecdotally state that aesthetic providers
technique is flawless (Benedetto, 2011).
just learning to perform neurotoxin injections in the up-
per face have approximately a 4% incidence of inducing
ptosis, which with practice falls to 0.5% (Bauman, 2009). CONCLUSIONS
It is imperative that aesthetic providers injecting neuro-
toxins carefully consider the location of each injection,
PRACTICAL STEPS TO BE MINDFUL OF
especially in the “danger zones.” Sound knowledge of
WHEN INJECTING NEUROTOXINS IN OR
facial and muscle anatomy, especially the key areas that
NEAR “DANGER ZONES”
are prone to neurotoxin diffusion, and knowing how
Practical steps to be mindful of when injecting near aging affects the location of these anatomical structures,
“danger zones” include the following: is half of the battle in preventing eyelid ptosis, brow
ptosis, and facial asymmetry with neurotoxins. Knowl-
• In the upper face, keep injection at least 1 cm above
edge of the steps necessary to minimize eyelid ptosis and
the mid brow and orbital rim to avoid brow ptosis.
facial asymmetry will ensure that the aesthetic provider is
• In the orbicularis oculi (i.e., crow’s feet area),
adequately prepared to quickly respond if these rare but
keep the injection approximately 1 cm lateral to
noticeable adverse events occur. And finally, consistently
the orbital rim to avoid unwanted weakening of
exercising practical “neurotoxin injection tips,” whenever
the muscles of ocular motion, which are inside the
an aesthetic provider injects a neurotoxin in close prox-
orbital rim (Spencer, 2011).
imity to a “danger zone,” will ensure client safety and
• If the medial palpebral orbicularis oculi is weak-
satisfaction.
ened as the result of the unintended diffusion of the
neurotoxin, a diminution in the action of the lacri-
mal pump can occur, causing epiphora (excessive
REFERENCES
tearing). Diplopia also can result if the medial rec- ASAPS. (2013). 2013 cosmetic surgery national data bank statis-
tus is weakened by a neurotoxin (Benedetto, 2011). tics. Retrieved September 23, 2014, from https://s3.amazonaws.
• In the DAO, keep the injection point 1 cm away com/asaps/assets/stats/2013/ASAPS-2013-Stats.pdf
Bauman, L. (2009). In Bauman, L. (Ed.), Cosmetic Dermatology.
from the corner of the mouth. (2nd ed., p. 188). New York: McGraw Hill.
• Be attentive to appropriate placement. Benedetto, A. (2011). Cosmetic uses of botulinum toxin a in the
• Be aware of the dosage and dilute the neurotoxin mid face and appendix 5. In Benedetto, A. (Ed.), Botulinum
appropriately. toxins in clinical aesthetic practice (2nd ed., pp. 101–139, 276).
London: Informa Healthcare.
• Avoid massaging areas that are prone to diffusion Brennan, C. (2012). Art of the aesthetic consultation. Plastic Surgical
of the neurotoxin. Nursing, 32(1), 12–16; quiz 17–18.
• Botulinum toxin-induced lid ptosis can manifest Wesley, N. & Jones, D. (2013). Glabella. In Carruthers, A. & Carruthers,
within 48 hr or as late as a week after injections, and J. (Eds.), Botulinum Toxin. (3rd ed., p. 83). Philadelphia, PA:
Saunders Elsevier.
can last for weeks. It typically resolves within 2–6 Dorland, W. (2003). Dorland’s illustrated medical dictionary. 30th
weeks. Apraclonidine 0.5% (Iopidine, Alcon Labs, ed. Philadelphia, PA: W. B. Saunders Company.
Fort Worth, TX), naphazoline (Naphcon-A, Alcon Koblenzer, C. (2011). Prologue: The search for beauty, historical,
Labs), and phenylephrine 2.5% (Mydfrin 2.5%, Al- cultural, and psychodynamic trends. In Benedetto, A. (Ed.),
Botulinum toxins in clinical aesthetic practice (2nd ed., p. xi).
con Labs) are alpha-adrenergic agonist ophthalmic London: Informa Healthcare.
eye drops that may be used to correct eyelid ptosis Seckel, B. (1994). Facial danger zones—avoiding nerve injury in
as a result of a botulinum toxin injection. The alpha- facial plastic surgery. St. Louis: Quality Medical Publishing,
Inc.
adrenergic agonist effect stimulates Müller’s muscle
Spencer, J. (2011). Facial anatomy and the use of botulinum
to help elevate the ptotic eyelid. Typical dosage is toxin. In Benedetto, A. (Ed.), Botulinum toxins in clinical
two drops, two to three times a day, until the ptosis aesthetic practice (2nd ed., pp. 15–23). London: Informa
is resolved (Wesley & Jones, 2013). Healthcare.
For more than 26 additional continuing education articles
related to plastic surgery, go to NursingCenter.com/CE.
176 www.psnjournalonline.com Volume 34 Number 4 October–December 2014
Copyright © 2014 American Society of Plastic Surgical Nurses. Unauthorized reproduction of this article is prohibited.
PSN-D-14-00042_LR 176 28/11/14 9:45 PM
Anda mungkin juga menyukai
- Plastic and Aesthetic Nursing: Scope and Standards of PracticeDari EverandPlastic and Aesthetic Nursing: Scope and Standards of PracticeBelum ada peringkat
- 2) Incaaam PP ThreadliftDokumen47 halaman2) Incaaam PP ThreadliftFitri Fratiwi100% (4)
- Botox Best Practices Ebook PDFDokumen19 halamanBotox Best Practices Ebook PDFSuhair F Diebes0% (1)
- Facial Lifting With Aptos ThreadsDokumen9 halamanFacial Lifting With Aptos ThreadsAlejandro Saldarriaga OchoaBelum ada peringkat
- Polydioxanone Thread LiftingDokumen4 halamanPolydioxanone Thread LiftingGLORIABelum ada peringkat
- Putting BOTOX Facial Fillers Into PracticeDokumen62 halamanPutting BOTOX Facial Fillers Into PracticeVinisha Vipin Sharma100% (8)
- CanulaDokumen3 halamanCanulaCatalina Soler Lioi100% (1)
- Mid Face Rejuvenation PDFDokumen3 halamanMid Face Rejuvenation PDFAlan Long100% (1)
- Beautification and Rejuvenation With Botulinum Toxin InjectionDokumen80 halamanBeautification and Rejuvenation With Botulinum Toxin InjectionViniFortunata100% (1)
- 10-28 InjectablesDokumen31 halaman10-28 Injectablessalibagustavo60% (5)
- AMET Botox and FillerDokumen186 halamanAMET Botox and Fillerhesham100% (2)
- FillerDokumen63 halamanFillerAchmadDamiri100% (1)
- The Art of Threads A Comprehensive ReviewDokumen17 halamanThe Art of Threads A Comprehensive Reviewalejandro Gonzàlez80% (5)
- Elite Botox TrainingDokumen169 halamanElite Botox Trainingcarolina100% (4)
- Safety Injectables WorkbookDokumen110 halamanSafety Injectables Workbookgeraffe94% (17)
- Introductory Botulinum PresentationDokumen113 halamanIntroductory Botulinum Presentationprontaprintpottersbar100% (5)
- Module 2, Course B - FillersDokumen120 halamanModule 2, Course B - FillersHeather Marie Mathis100% (2)
- Skin Beauty InjectionsDokumen12 halamanSkin Beauty Injectionst3kla100% (1)
- Upper Face BotoxDokumen32 halamanUpper Face Botoxyaseer arafat67% (3)
- The Dermal Filler Approach FinalDokumen32 halamanThe Dermal Filler Approach FinalhenkyBelum ada peringkat
- 34 37 AM JUN15 Facial Ageing 3Dokumen4 halaman34 37 AM JUN15 Facial Ageing 3EvieYoung67% (3)
- Lifting Vs Volumizing-The Difference in Facial Minimally Invasive Procedures When Respecting The Line of LigamentsDokumen7 halamanLifting Vs Volumizing-The Difference in Facial Minimally Invasive Procedures When Respecting The Line of LigamentsArcelino Farias100% (1)
- Perioral RejuvenationDokumen11 halamanPerioral RejuvenationjuliemonneypennyBelum ada peringkat
- Lower Face Clinical AnatomyDokumen23 halamanLower Face Clinical AnatomyΔρ Βάιος Αγγελόπουλος100% (2)
- Illustrated Guide To Aesthetic BTX Injections - CH 4 - Estetik - Kort VariantDokumen16 halamanIllustrated Guide To Aesthetic BTX Injections - CH 4 - Estetik - Kort Variantbobocmihail0% (1)
- Botulinum Toxin in Facial Rejuvenation (Kate Coleman) (Z-Library)Dokumen124 halamanBotulinum Toxin in Facial Rejuvenation (Kate Coleman) (Z-Library)Danny MolinaBelum ada peringkat
- 12 Filler PointsDokumen15 halaman12 Filler PointsSripada Lk Kingjorn100% (1)
- Vascular Complication of Injectable FillerDokumen17 halamanVascular Complication of Injectable Fillerahmed100% (1)
- Botulinum Toxins in Clinical Aesthetic Practice 3rd Edition Volume Two - Functional Anatomy and Injection Techniques 2018Dokumen237 halamanBotulinum Toxins in Clinical Aesthetic Practice 3rd Edition Volume Two - Functional Anatomy and Injection Techniques 2018Dogukan Demir75% (4)
- MD CodesDokumen41 halamanMD CodesTatiana Araujo67% (3)
- Copper For BusbarDokumen60 halamanCopper For BusbarSunil Gadekar100% (3)
- Inject Able S SafetyDokumen110 halamanInject Able S SafetyYuko YamaguchiBelum ada peringkat
- Mesotherapy RejuvenationDokumen40 halamanMesotherapy RejuvenationerlanggawidyaputriBelum ada peringkat
- C779-C779M - 12 Standard Test Method For Abrasion of Horizontal Concrete SurfacesDokumen7 halamanC779-C779M - 12 Standard Test Method For Abrasion of Horizontal Concrete SurfacesFahad RedaBelum ada peringkat
- Z Hãng Algeness dermal filler training manual 2019 - Giới thiệu sản phẩm PDFDokumen156 halamanZ Hãng Algeness dermal filler training manual 2019 - Giới thiệu sản phẩm PDFLe Dung100% (1)
- Botox HH TrainingDokumen15 halamanBotox HH Trainingfajarrudy qimindra100% (1)
- Module 1, Course B - A Practical Guide To Botulinum Toxin Type A - The Scientific Art of Softening Lines and Wrinkles 2Dokumen97 halamanModule 1, Course B - A Practical Guide To Botulinum Toxin Type A - The Scientific Art of Softening Lines and Wrinkles 2Heather Marie Mathis100% (1)
- BOTOX LectureDokumen74 halamanBOTOX LectureAnonymous 8hVpaQdCtr100% (6)
- 2018 Hassan Galadari (Auth.) - Soft Tissue Augmentation - Principles and PracticeDokumen92 halaman2018 Hassan Galadari (Auth.) - Soft Tissue Augmentation - Principles and PracticeMohan100% (3)
- Nefertiti Lift BotoxDokumen9 halamanNefertiti Lift BotoxAnamaria Zaccolo100% (2)
- A 10-Point Plan For Avoiding Hyaluronic Acid Dermal Filler-Related Complications During Facial Aesthetic Procedures and Algorithms For ManagementDokumen9 halamanA 10-Point Plan For Avoiding Hyaluronic Acid Dermal Filler-Related Complications During Facial Aesthetic Procedures and Algorithms For Managementleenatalia93100% (1)
- Avoiding Dermal Filler Complications PDFDokumen10 halamanAvoiding Dermal Filler Complications PDFAndreas DilipidiBelum ada peringkat
- PDO Thread Lift Treatment Los AngelesDokumen8 halamanPDO Thread Lift Treatment Los AngelesSimmi Goyal0% (1)
- Holy Spirit Mass SongsDokumen57 halamanHoly Spirit Mass SongsRo AnnBelum ada peringkat
- Botox For The Eyes and BrowDokumen5 halamanBotox For The Eyes and Browlfan0% (1)
- Complications of Thread Lift and How To Manage - Thread Protrusion, Infection, Dimpling and BruisingDokumen4 halamanComplications of Thread Lift and How To Manage - Thread Protrusion, Infection, Dimpling and BruisingAnonymous LnWIBo1G0% (1)
- BotoxDokumen28 halamanBotoxrnvisBelum ada peringkat
- Cosmetic Uses of Botulinum ToxinDokumen28 halamanCosmetic Uses of Botulinum Toxineby_3tamaBelum ada peringkat
- Botox EbookDokumen15 halamanBotox Ebookdoraemon100% (2)
- Botulinum Toxins: Cosmetic and Clinical ApplicationsDari EverandBotulinum Toxins: Cosmetic and Clinical ApplicationsJoel L. CohenBelum ada peringkat
- Calculations: M 0 M 1 c1 c1 0 c2 c2 1 2Dokumen6 halamanCalculations: M 0 M 1 c1 c1 0 c2 c2 1 2shadab521100% (1)
- Anti-Aging Therapeutics Volume XIVDari EverandAnti-Aging Therapeutics Volume XIVPenilaian: 3 dari 5 bintang3/5 (1)
- Nonsurgical Lip and Eye Rejuvenation Techniques: Gabriella Fabbrocini Maria Pia de Padova Antonella TostiDokumen125 halamanNonsurgical Lip and Eye Rejuvenation Techniques: Gabriella Fabbrocini Maria Pia de Padova Antonella Tostikleidi8588% (8)
- Facial MesotherapyDokumen3 halamanFacial Mesotherapydanielagonzalezt5Belum ada peringkat
- Botox FillerDokumen42 halamanBotox Fillermeiranty NingrumBelum ada peringkat
- Dermal Filler 4Dokumen59 halamanDermal Filler 4Ahmed Sad100% (1)
- Mesoglow y MesoliftDokumen2 halamanMesoglow y MesoliftPablo BaudinoBelum ada peringkat
- PDO Thread LiftsDokumen2 halamanPDO Thread LiftsDrekka Hanibal Putra33% (3)
- A Guide To Cheek Augmentation Single-Point Deep inDokumen8 halamanA Guide To Cheek Augmentation Single-Point Deep inAnantya SophanBelum ada peringkat
- The Evolution of Aesthetic Medicine: The Evolution of a New Field of Medicine by a Pioneer Voted the Top Aesthetic Doctor in the WorldDari EverandThe Evolution of Aesthetic Medicine: The Evolution of a New Field of Medicine by a Pioneer Voted the Top Aesthetic Doctor in the WorldBelum ada peringkat
- Rubber Stamp BusinessDokumen4 halamanRubber Stamp BusinessvasantsunerkarBelum ada peringkat
- Computer Forensics ReportDokumen7 halamanComputer Forensics ReportMatias IacobuzioBelum ada peringkat
- Aesthetic Procedures: Nurse Practitioner's Guide to Cosmetic DermatologyDari EverandAesthetic Procedures: Nurse Practitioner's Guide to Cosmetic DermatologyBelum ada peringkat
- MesobotoxDokumen12 halamanMesobotoxNiculae Bogdan Dimitrie100% (1)
- Blotchy Skin in Seniors (Bateman Purpura or Dermatoporosis) Treated by Topical Vitamin C, Etc. - RCT Aug 2017Dokumen1 halamanBlotchy Skin in Seniors (Bateman Purpura or Dermatoporosis) Treated by Topical Vitamin C, Etc. - RCT Aug 2017Nur CameliaBelum ada peringkat
- Monika Sukoco, Asih Budiastuti, Paulus YogyartonoDokumen7 halamanMonika Sukoco, Asih Budiastuti, Paulus YogyartonoNur CameliaBelum ada peringkat
- Bilateral Nevus of Ota Treated With Combination of CO Fractional Laser and 1064 NM Nd:YAG LaserDokumen10 halamanBilateral Nevus of Ota Treated With Combination of CO Fractional Laser and 1064 NM Nd:YAG LaserNur CameliaBelum ada peringkat
- Erythema Multiforme Major in Hiv Patient: Nur CameliaDokumen5 halamanErythema Multiforme Major in Hiv Patient: Nur CameliaNur CameliaBelum ada peringkat
- HIV N Leprosy 2011Dokumen4 halamanHIV N Leprosy 2011Nur CameliaBelum ada peringkat
- Operating Instructions: Vacuum Drying Oven Pump ModuleDokumen56 halamanOperating Instructions: Vacuum Drying Oven Pump ModuleSarah NeoSkyrerBelum ada peringkat
- TCC Number 153-4-4Dokumen1 halamanTCC Number 153-4-4jeremie gamonBelum ada peringkat
- Fundamentals of Logistics XI - 2023Dokumen45 halamanFundamentals of Logistics XI - 2023saiyaBelum ada peringkat
- Os Unit-1Dokumen33 halamanOs Unit-1yoichiisagi09Belum ada peringkat
- Light Design by Anil ValiaDokumen10 halamanLight Design by Anil ValiaMili Jain0% (1)
- Solution Manual For Understanding Business 12th Edition William Nickels James Mchugh Susan MchughDokumen36 halamanSolution Manual For Understanding Business 12th Edition William Nickels James Mchugh Susan Mchughquoterfurnace.1ots6r100% (51)
- Syllabus EM1Dokumen2 halamanSyllabus EM1Tyler AnthonyBelum ada peringkat
- Rawtani 2019Dokumen9 halamanRawtani 2019CutPutriAuliaBelum ada peringkat
- Letter For LACDokumen7 halamanLetter For LACDahlia G. MaglasangBelum ada peringkat
- Lean Six SigmaDokumen5 halamanLean Six SigmavinBelum ada peringkat
- Support of Roof and Side in Belowground Coal MinesDokumen5 halamanSupport of Roof and Side in Belowground Coal MinesNavdeep MandalBelum ada peringkat
- Culture Performance and Economic Return of Brown ShrimpDokumen8 halamanCulture Performance and Economic Return of Brown ShrimpLuã OliveiraBelum ada peringkat
- Variables in The EquationDokumen3 halamanVariables in The EquationfiharjatinBelum ada peringkat
- Bob Jones: This CV Template Will Suit Jobseekers With Senior Management ExperienceDokumen3 halamanBob Jones: This CV Template Will Suit Jobseekers With Senior Management ExperienceDickson AllelaBelum ada peringkat
- Paper 19 AugustDokumen552 halamanPaper 19 AugustUma Sankar Pradhan100% (1)
- HRIRDokumen23 halamanHRIRPhuong HoBelum ada peringkat
- Transfer CaseDokumen46 halamanTransfer Casebantuan.dtBelum ada peringkat
- Continuous Improvement SYMPOSIUM SCRIPTDokumen3 halamanContinuous Improvement SYMPOSIUM SCRIPTChanda Marie AsedillaBelum ada peringkat
- Reading Comprehension Lesson Plan FinalDokumen9 halamanReading Comprehension Lesson Plan Finalapi-254917183Belum ada peringkat
- EDUHUBDokumen6 halamanEDUHUBishant sharmaBelum ada peringkat
- Ancient India: Book Recommendation: Indian Feudalism Urban Decay in India - RS SharmaDokumen5 halamanAncient India: Book Recommendation: Indian Feudalism Urban Decay in India - RS SharmaShraddha 7Belum ada peringkat
- Water Quality MonitoringDokumen3 halamanWater Quality MonitoringJoa YupBelum ada peringkat
- EtchDokumen2 halamanEtchlex bactolBelum ada peringkat
- 1st Quarter 2016 Lesson 5 Powerpoint With Tagalog NotesDokumen25 halaman1st Quarter 2016 Lesson 5 Powerpoint With Tagalog NotesRitchie FamarinBelum ada peringkat