GI Outline
Diunggah oleh
Liz Tollefson0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
390 tayangan11 halamanThis document provides information on diagnostic testing and procedures for gastrointestinal issues. It discusses laboratory tests including serum proteins, total lymphocyte count, nitrogen balance, and fecal analysis. Imaging tests covered include upper GI studies, barium enemas, esophagogastroduodenoscopy, colonoscopy, and proctoscopy/sigmoidoscopy. Preparation, risks, and follow-up care are outlined for each procedure. Common gastrointestinal medications and disorders of the esophagus and stomach are also reviewed.
Deskripsi Asli:
Hak Cipta
© Attribution Non-Commercial (BY-NC)
Format Tersedia
DOCX, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniThis document provides information on diagnostic testing and procedures for gastrointestinal issues. It discusses laboratory tests including serum proteins, total lymphocyte count, nitrogen balance, and fecal analysis. Imaging tests covered include upper GI studies, barium enemas, esophagogastroduodenoscopy, colonoscopy, and proctoscopy/sigmoidoscopy. Preparation, risks, and follow-up care are outlined for each procedure. Common gastrointestinal medications and disorders of the esophagus and stomach are also reviewed.
Hak Cipta:
Attribution Non-Commercial (BY-NC)
Format Tersedia
Unduh sebagai DOCX, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
390 tayangan11 halamanGI Outline
Diunggah oleh
Liz TollefsonThis document provides information on diagnostic testing and procedures for gastrointestinal issues. It discusses laboratory tests including serum proteins, total lymphocyte count, nitrogen balance, and fecal analysis. Imaging tests covered include upper GI studies, barium enemas, esophagogastroduodenoscopy, colonoscopy, and proctoscopy/sigmoidoscopy. Preparation, risks, and follow-up care are outlined for each procedure. Common gastrointestinal medications and disorders of the esophagus and stomach are also reviewed.
Hak Cipta:
Attribution Non-Commercial (BY-NC)
Format Tersedia
Unduh sebagai DOCX, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 11
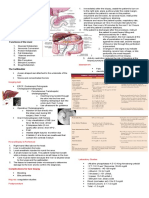
Managing Clients Experiencing Problems of the ▫ Low-residue diet 1-2 days b4 exam
Gastrointestinal ▫ Clear liquid diet day b4
I. Diagnostic Testing- Chapter 34 ▫ Laxative evening b4
A. Laboratory studies ▫ NPO after midnight
1. Serum proteins: ▫ Enemas till clear in AM
▫ Albumin, prealbumin, retinol-binding protein, & c. Nursing Care:
transferrin ▫ Always schedule barium enema BEFORE UGI
2. Total lymphocyte count (TLC) series exacuate barium first ….upi first mess up lgi
▫ Below 1800/mm3 suggests malnutrition d. Post-procedure: Encourage increased fluid &
3. Nitrogen Balance assess BM for elimination of barium
▫ Record all calories& all urine for 24 hours (4-6Gm) 9. Endoscopic Examination directly looking at
▫ Negative values indicate catabolic states or increased inner lumen
nutritional requirements a. Esophagogastroduodenoscopy (EGD) down
4. Carcinoembryonic Antigen (CEA)- “tumor marker” esphg 11 ;(
▫ Increased in colorectal cancer & inflammatory bowel b. Colonoscopy
disease c. Proctoscopy/Sigmoidoscopy
5. Fecal Analysis d. Small-bowel Enteroscopy
Cultures 10. Esophagogastroduodenoscopy (EGD)- Direct
Ova& parasites visualization of internal structures of upper GI using
Occult Blood-guiac, Hemocult gastroscope & may obtain specimens
Color a.Pre-procedure
Blood on or within NPO 8 hours prior to exam
Lipids Given a local anesthetic gargle or spray to numb
Odor throatØnumb gag reflex
Consistency IV Midazolam (Versed) provides moderate sedation
6. Gastric Analysis & relieves anxiety
a. Measures secretion of HCl & Pepsin in the Atropine may be given to decrease secretions
stomach Glucagon Ø relax smooth muscle
b.Used to diagnose duodenal ulcer, Zollinger- b. Procedure
Ellison syndrome, gastric carcinoma, & pernicious Position patient in left lateral position
anemia Ongoing assessment of patient status
c.Two Parts: c. Post-procedure gag reflex
Basal cell secretion test ▫ Assess LOC, V/S, sats, pain, signs of perforation,&
Gastric acid stimulation test~how much gastric return of gag reflex
acid after med is given that would …. 4.4 not 11. Proctoscopy-Sigmoidoscopy- Endoscopic exam of
normalendocopy the anus, rectum,& sigmoid & descending colon
d. Dx prob more in mucous layer Flexible scopes have replaced rigid scopes (that
Markedly increased indicates Zollinger-Ellison could only visualize 10 inches) & can visualize
Moderately elevated- Duodenal ulcer 16-20 inches
â levels- gastric ulcer or cancer Bowel prep: TWE or Fleet’s enema till clear
7. UGI watch how barium moves throughtrack Dietary restrictions not necessaryØno t going far
a. Upper GI Study- Fluoroscopic& X-ray Sedation usually not needed
examination of upper GI tract following Position in Left lateral w/right leg bent & placed
instillation of radiopaque liquid (often Barium) anteriorly toward chest
b. Patient Education: During procedure, monitor VS, skin color & temp.,
▫ Clear liquid diet w/NPO from midnight night before pain, & vagal response
▫ Usually withhold AM meds morning of exam Post- Monitor for bleeding & signs of perforation
c. Follow-up 12. Colonoscopy - Direct visualization of large
▫ á fluids to facilitate evacuation of stool & barium intestine (anus, sigmoid, transcending, & ascending
▫ Make sure patient has eliminated barium colon) via colonscope
8. LGI study- Visualization of lower GI tract after Can be used diagnostically or therapeutically
rectal installation of barium, “barium enema” Preparation:
b. Bowel prep: o No asprinØâ/R bleed
o Clear liquids starting at Noon b4 exam III. Meds for GI Problems
o Bowel Cleansing w. laxatives & enemas or more • See Table 37-1, p. 1206-07
commonly w. glycol electrolyte lavage solution • Antibx
(Go-Lytely, Colyte,& Nu-Lytely) orally over 3-4 ▫ Amoxicillin (Amoxil), Clarithromycin (Biaxin),
hours high electrolyte17 Metronidazole (Flagyl), Tetracylcine
o loose stoolsliquid stools….pulls out all fluid from • AntiD*l
body too ▫ Bismuth subsalicylate (Pepto-Bismol)
Procedure: • Histamine-2 (H2) receptor antagonists
Obtain informed consent ▫ Cimetidine (Tagamet), Famotidine (Pepcid),
Sedate w/opioid or sedative for moderate sedation Ranitidine (Zantac)
Glucagon may be given to relax colon & â spasm • Proton pump inhibitors (PPIs)
▫ Esomeprazole (Nexium), Lansoprazole (Prevacid),
Monitor V/S, color, skin temp., LOC, distention, vagal
Omeprazole (Prilosec), Pantoprazole (Protonix),
response (âP, rebound áP, sweaty pale), pain
Rabeprazole (AcidHex)
Position on left side w/knees drawn toward chest;
• Prostaglandin E1 analog- cytoprotective agents
may have to change position during test to facilitate
▫ Misoprostol (Cytotec), Sucralfate (Carafate)
advancement of the scope
• Antacids- neutralize acid in stomach
d.Post-procedure:
▫ Aluminum compounds- aluminum hydroxide,
• Maintain on BR till fully alert
carbonate or phosphate
• May experience cramps d/t increased peristalsis 2nd
▫ Magnesium compounds- magnesium hydroxide
to air insufflated into bowel
(MOM) or magnesium oxide
• Assess for S & S of bowel perforation (bleeding, pain,
▫ Calcium compounds- calcium carbonate
distention, F*{100-101}) peritonitisØperfureated
▫ Sodium compounds- sodium bicarbonate
bowelinflam starts muscles hardlocalized where
• Anticholinergics- block action of PNS
perforation is 20 contents leakout inflam
• Cholinergics- enhance PNS
• Provide patient education verbally& in writing as
• Prokinetics
sedating meds have amnesic qualities
▫ Metoclopramide (Reglan), Cisapride (Propulsid)
• Should report any bleeding to MD
▫ PNSØactive during digestionØ enhance effect of PNS
or block (diarreah)
II. A & P Review of Esophagus-Stomach
▫ REGLANØ 25
• Lower esophageal sphincter LES) prevents gastric
fluid from entering esophagus. Affected by:
IV. Disorders of Esophagus & Stomach
▫ Muscle tone, innervation, intrabd pressure, gastric
A. Disorders of the Esophagus
distention, size of bolus, rate of eating
1. Dysphagia- difficulty swallowingØneuro. Muscles,
• Stomach cells:
obstruction,
▫ Parietal- produce HCl acid (activates pepsin) produce
▫ Mechanical obstructions
intrinsic factor (needed for Vit B12 absorption)
▫ Cardiovascular abnormalitiesØfluid prob
▫ Mucous cells- produce K+ & HCO3; protects stomach
▫ Neurological
from acid
2. Regurgitation- ejection of gastric juice into mouth
• Parts of stomach:
3. Odynophagia- pain w/swallowing (too big)
▫ Fundus (top), Body (middle),& Antrum (bottom)
narrowing, restrictions
▫ Body & fundus highly distensible
Triggered by cold or carbonated beverages or solid
▫ Contents empty from antrum through pyloris into
food passign through esophagus
duodenum
4. Dyspepsia or heartburn, “indigestion”- burning
midline in lower retrosternal area that radiates toward
• Innervation
neck
▫ PNS- Vagus; stimulates
5. Achalasia- á dysphagia; “something stuck in
▫ SNS- Celiac, mesenteric, & hypogastric ganglia;
throat”
inhibit
C. Gastroesophageal Reflux (GERD) midlife, ileus
▫ Auerbach plexus- Motor
isn’t tight anymore stomach contants È to esphoageas
▫ Meissner’s plexus- Sensory
erodesprelude to esoph cancer
• Secretions
1. Inappropriate relaxation of LES w/reflux of gastric
▫ Pepsin (pepsinogen), gastrin, gastric lipase, HCl acid
or duodenal contents into esophagus
▫ Breakdown food & mix w/secretions for digestion
2 . Etiology: unknown don’t have a strong esph 2. Chronic
musc. Pressure from stomach pushes fluid us ▫ Caused by ulcers of the stomach, infect w/ H. pylori,
3. Assoc with: autoimmune diseases, excess caffeine, meds- NSAIDS,
Altered innervation, displacement of the angle of the bisphosphonate (Fosamax or Actonel), OH , smoking,
gastroesophageal junction, & incompetent LES chronic reflux of pancreatic secretions & bile into
á intragastric pressure pushes contents up stomach
4. R/FxØObesity, preg, tobacco use, high fat diet, 3. Pathophysiology
caffeine, & á estrogen & progesterone levels ▫ Mucous membrane becomes edematous &
5. Manifestations of GERD hyperemic; undergoes superficial erosion. Secretes less
May mimic ♥ attack gastric juice w/little acid & much mucus
Pyrosis (burning in the esophagus) hemorrhageupper GI bleed (throw up blood) if not
Dyspepsia blood in bm
Regurgitation ▫ IF always bleeding Fe defiency 38 ;(:::
Dysphagia 4. Manifestations of Gastritis
Odynophagia • Acute
Hypersalivation Øwatery In mouth b4 eruptation ▫ Rapid onset
▫ Abd discomfort, HA , lassitude, N*, anorexia, V*, &
Esophagitis Øinflam
hiccups
6. Management of GERD
▫ Lasts hours to days
a. Patient EducØConsume low-fat diet; avoid caffeine,
• Chronic
tobacco, OH, milk, foods containing peppermint, &
▫ Anorexia, heartburn after eating, belching, sour taste
carbonated beverages; avoid intake 2 hrs before bed;
in the mouth, N & V
maintain healthy weight; avoid tight-fitting clothes; á
▫ Some have only mild epigastric discomfort or
HOB
intolerance to spicy or fatty foods or slight pain relieved
b. Meds:
by eating
Antacids, H2 receptor antagonists(block
▫ Evidence of malabsorp of B12
hydrochloric acid), Proton pump inhibitors, or
▫ Some have no sx Øbleeding until CBC shows
Prokinetic agents(food outa stomach faster
5. Management Gastritis
into33: …to reduce,…_
Gastric mucosa repairs itself & patient recovers in
Avoid anticholinergics(want GI syst to be used),
about 1 day
Ca-channel blockers, bisphosphonates, &
Should refrain from OH & food until resolved
Theophyllin
c. Surgical management Nonirritating diet recommended
▫ Nissen fundoplicationØ fudus around stomach& Persistent sx treated w/IVF, NG(tube suck out
support to illeus so theres less likey to have food back gastric secretion, irritants rests system,
u[ secretions that happen in GI), analgesics,
D. Barrett’s Esophagus r cell structure in llower part sedatives, antacids
of esph 6. Nursing Management- Gastritis
1. Assoc w/untreated GERD • Nursing Diagnoses
• Squamous cells of esophagus replaced by ▫ Anxiety r/t treatment
columnar epithelium resembling stomach or intestines ▫ Imbalanced nutrition, less than body requirements
• Lining is reddened rather than pink ▫ Risk for imbalanced fluid volume r/t insufficient
2. Management: intake & excessive loss 2nd to V*
▫ Monitor w/EGD ▫ Health maintenance r/t insufficient knowledge about
▫ Photodynamic therapy- laser ablation for surgical dietary management & disease process
risks ▫ Acute pain r/t irritated stomach mucosa
▫ Esophagectomy reduces risk for development of • Collaborative ProblemØRisk for complication:
adenocarcinoma Hemorrhage
E. Gastritis- Inflam of the gastric or stomach mucosa 7. Nursing Care
1. Acute meds that need to be taken w/ food bc ▫ Support client, use calm approach, explain all
irritating to stomach procedures& treatment
▫ Caused by dietary indiscretion, overuse of aspirin or ▫ NPO until acute sx subside
NSAIDS, excess OH, radiation therapy, ingestion of ▫ Monitor I & O, serum elects
strong acid or alkali, acute illness or traumatic injury
▫ When sx subside, start w/ice chipsclear ▫ Pyrosis (heartburn), V*, constipation, or D*,&
liquidsfullsolids bleeding
▫ Evaluate response to diet ▫ Sour eructation (burping) when stomach empty
▫ Teach client to avoid caffeine, OH , & cigarette ▫ V* Ø obstruction of pyloric cant get from stomach
smoking to duodemum may (not) precede N*
▫ Assess for signs of dehydration ▫ Emesis often contains undigested food
▫ Assess for signs of hemorrhagic gastritis ▫ 15% experience bleeding
Hematemesis, tachycardia, & hypotension 4. Management of PUD
F. Peptic Ulcer Disease (PUD) • Combination of antibx, proton pump inhibitors, &
1. General Information bismuth salts to suppress or eradicate H. pylori
• May be gastric, duodenal, or esophageal • Recommend therapy for 10-14 days
• An erosion & excavation in the mucosal wall; may o Triple therapy- two antibx (Flagyl or Amoxil &
through muscle leak into peritoneum Biaxin) plus a proton pump inhibitor (PPI)
• Strikes people btwn 40-60 years old; rare in women o Quadruple therapy- two antibx, PPI, & bismuth
of childbearing age but after menopause rates for salts
women equal to men, estrogen protectice o H2 receptor antagonists & PPI treat NSAID-
• Almost always d/t infect w/H. pylori not stress & induced ulcers & ulcers not assoc w/ H. pylori
anxiety as was once thought o See Table 37-3, p. 1211 for med regimens
• Excess secretion of HCl acid in the stomach also • Rest, sedatives, tranquilizers prn for comfort
contributes to formation of peptic ulcers • MaintainØH2 receptor antagonists recommended
o Milk, pop, smoking, & OH á HCl secretion for 1yrØkeep from ulcer from coming back.
o Stress & spicy foods may aggravate peptic ulcers • Patients at risk for stress ulcers treated
▫ * look up in book* Zollinger-Ellison syndrome (ZES) prophylactically w/H2 receptor antagonists &
Øsevere gastric ulsers extreme gastric (non)cancer in cytoprotective agents to decrease risk for upper GI
pancreas tract hemorrhage
2. Pathophysiology of PUD • Stress reduction & rest
▫ Erosion results from action of gastric acid (HCl) & • Smoking cessation
pepsin caused by excess activity of these substances or • Dietary modificationØAvoid extreme food
decreased resistance of the mucosa. temperatures, meat extracts, OH , coffee (even
• 53 AggravatingØh pylori, NSAIDS not enteric decaffeinated), caffeinated beverages, diets rich in
coated milk & cream; eat 3 meals a day
• Impaired defenceØ ishchemia, shock, delayed gastric 5. Nursing Diagnoses
empty, ▫ Acute pain r/t action of acid on damaged mucosa
• Stress ulcer-sepsis, ventilated Øinsult to body occurs ▫ Anxiety r/t acute illnessØthey think its something
after physiologically stressful events (burns, shock, severe
sepsis, or multiple organ trauma) ▫ Imbalanced nutrition r/t dietary changes
▫ Most common in ventilator-dependent patients after ▫ Risk for Ineffective Health Maintenance r/t deficient
trauma or surgery knowledge about prevention of sx & management of
▫ Ulcerations begin within 24-72 hrs, spread as condition
condition continues,& resolve as patient recovers 6. Collaborative Problems
• Cushing’s Ulcer- neuro in patients w/head injuries ▫ Hemorrhage
or brain trauma; occurs in esophagus, stomach, or ▫ PerforationØerodes through
duodenum ▫ PenetrationØulcer erodes to musc wall spasms
• Curling’s Ulcer- burn seen 72 hrs after extensive ▫ Pyloric obstruction (gastric outlet obstruction)Øfood
burns in antrum of stomach or the duodenum cant get outa stomach
G. Morbid Obesity
3. Manifestations of PUD come& go 1. Definitions:
Pain radiates to back, wet burps ▫ BMI > 30 z Body weight > 100 # & > 2 x deal body
▫ Sx last days, weeks, months & may disappear then weight
reappear; some are asymptomatic 2. Growing problem in US where 65% are
▫ Dull, gnawing pain or burning sensation in the overweight
midepigastric area or in the back 3. á/R for other health compØDiab, ♥ dis, stroke, htn,
gallbladder dis , arthritis, sleep apnea, & breathing prob
4. Management of Obesity After bowel sounds return & oral intake is resumed,
▫ Conservative managØDiet & exercise-Limited success 6 small feedings are provided
▫ Pharmacologic tx options Sip fluids btwn meals~ w/ meals to delay emptying
▫ Excess …â … tell when there full. 1.10 Report excessive thirst or concentrated urine
Sibutramine HCl (Meridia)- inhibits serotonin & Psychological support
NE & â appetite Long term S/EØá/R gallstones, nutritional defic, risk
May increase BP, cause dry mouth, insomnia, for weight re-gain.
HA , diaphoresis, & increased HR Management of Clients w/Bowel Problems: Chapter 38
Orlistat (Xenical)- â absorb of fat zâ caloric intake I. Inflammatory Problems
by binding to gastric & pancreatic lipase to prevent A. Gastroenteritis & Dysentery
digestion of fats Inflam of the stomach & intestinal tract affecting the
SE: á BM, gas w/oily discharge, â food small bowel
absorption, â bile flow, â absorption of vit S&S: D*, abd pain, cramping, N-V, F*, anorexia,
Rarely result in loss of more than 10% total distention, tenesmus, borborygmi (hyperactive
weight & low LT effectiveness bowel sounds)
6. Surgical Management of Obesity Primarily caused by contaminated food & water;
▫ Achieve weight loss Restricting intake, â absorpt, transmitted by fecal-oral route
or combo Clostridium difficile (C. diff) is a bacterial
▫ Duodem jejumum ileum Øall absorb certian things dysentery commonly seen in clients who have been
better receiving large doses of antibx for extended time, kill
Roux-en-Y gastric bypass: restrictive & normal intestinal floraovergrowth C.diff
malabsorptive *hx w/ c. diffhx of antibx
Gastric banding: restrictiveØâ /R for vit dific ▫ More & more common in hospitalized patients
Vertical-banded gastroplasty: restrictiveØmake ▫ Generally resolves in 1-5 days but can be fatal to
stomach smaller the debilitated, older or very young patient
Biliopancreatic diversion & duodenal switch: 2. Treated w/F & E replacement
restrictive & malabsorptive Irritable Bowel Syndrome disreg intestine spasms
▫ Average weight loss is 61% of previous body weight at an uncoordinated way good movmt of food
▫ Comorbid conditions such DM, htn, sleep apnea, & Common GI problem, occurring more in females
dyslipidemia È o Heredity, stress, depression-anxiety, á-fat diet,
▫ Candidates must be carefully screened & counselled food intol, OH , & smoking
▫ Less than body needs ….. It is a disorder of intestinal motility r/t
7. Common Complications neuroendocrine dysregulation, infect or irritation,
Bleeding vascular or metabdisturbance
Blood clots Peristaltic waves affected at specific segments
Bowel obstruction
Altered peristaltic intensity
Incisional or ventral hernias
No evidence of inflam or tissue changes in intestinal
Infects 2nd to leaks at anastomosis
mucosa
N d/t overfilling of pouch
1. Management of IBS
Dumping syndrome 2nd to consumption of simple
2. GoalsØRelieve pain, regulate BMs, â stress
sugars
Begins w/dietary restriction & gradual
• Sensation of fullness, weakn, faintness, dizziness,
reintroduction of foods while recording tolerance
palpitations, diaphoresis, cramping pains, & D*
High fiber diet recommended
• Vasomotor sx occur 10-90 min after
Exercise program
eatingPallor, perspiration, palpitations, HA ,
Pharmacologic agents:
feelings of warmth, dizziness, & even drowsiness
o Bulk forming productsØ +fiber bulk to BM
r bowel fx (intestine not being used) : D*, constip,
steatorrhea o AntiD*l agents
• Nutritional defic 2nd to malabsorp o Antidepressants
8. Nursing Management o Anticholinergics
Monitor for immediate post-operative complications o Tegaserod (Zelnorm)
▫ Peritonitisnleak, stomal obstruction /ulcers, Nursing Management IBS
atelectasis & pneum, thromboembolism, & Provide education
metabimbal o Understanding of disease
o Good dietary habits o If perforation occurs, an abcess may form. May need
o Eat slowly at regular times antibx & a drain to empty abcess before performing
o Chew foods thoroughly appendectomy
o Limit fluid intake at meal time Nursing Care: (See Table 38-3, p. 1242)
o Adequate daily fluid intake o Manage pain, fluids, anxiety, nutrition, & infect
o OH & smoking o May have NG tube(esp w. rupture or peritonitis) to
Malabsorp prevent paralytic ileus
Inability of digestive tract to absorb necessary vits o Patient positioned in high fowlers
&/or nutrients o Morphine usually used for pain
Conditions that lead to malabsorp: o Usually d/c in a day
▫ Mucosal (transport) disorders o If possible peritonitis, in surgery rinsed out, a drain is
▫ Infectious diseases left in place & will be kept longer for antibx &
▫ Luminal disorders monitoring
▫ Postoperative malabsorp Diverticular Disease
▫ Disorders r/t malabsorp of specific nutrients Diverticulum- saclike herniations of the lining of the
Manifestations: bowel that extends through a defect in the muscle layer
o D* or frequent, loose, bulky, foul-smelling stools & may occur anywhere in the small intestine but is most
w/increased fat content & often grayish in color common in the sigmoid colon
o Abd distention, pain, increased flatus, weakness, Diverticulosis- multiple diverticula w/o inflam or sx.
weight loss, decreased sense of well-being Very common in developed countries & increases w/age.
o Malnutrition & signs of vitamin & mineral deficiency Diverticulitis- food & bacteria retained in the
Intervention aimed at underlying cause & diverticulum produce infect & inflam perforation or
supplements abscess formation
Appendicitis o Sx complicationsØabscess, fistula (abnormal tract)
Inflam & edema of appendix formation, obstruction, perforation, peritonitis, &
Most common reason for emergency abd surgery; hemorrhage
ages 10-30 years greatest incidence Pathophysiology
Pathophysiology: o High intraluminal pressure, low volume in colon, & â
o Appendix becomes obstructed or twisted causing colon wall muscle strength mucosa & sub-mucosal
inflam -> increased intraluminal pressure causes layers of the colon to herniate inward pouch-
pain -> eventually fills w/pus. Can rupture& lead to muscular wall
generalized peritonitis. o Bowel contents accumulate in the diverticulum &
Manifestations of Appendicitis decompose, causing inflam & infect
o Vague epigastric or periumbilical pain progresses o Can perforate causing irritability & spasticity of the
to RLQ pain McBurneys colon
o Low grade F* 99-100, if high peritonitis o Abscesses can develop & perforate. This can lead to
o N*, possible V* peritonitis & erosion of arterial blood vessels &
o Anorexia subsequent bleeding
o Pain at McBurney’s pointif goes away (repture) Manifestations
infect organ dumped out peritoneum o Chronic constipation often precedes development by
o Rebound tendernessnever press over inflame many years
organ o S & S are mild & include bowel irregularity
o Positive Rosving’s sign w/intervals of D & N, anorexia, & bloating or distention
o Ruptured Appy: Diffuse abd pain, distention, elevated o Large bowel may narrow w/fibrotic strictures,
temp.,& positive obturator test leading to cramps, narrow stools, constipation, or
**If constipated, strain, avoid laxatives may cause obstruction
rupture o Weakness, fatigue, & anorexia are common
Management of Appendicitis o Strictures impede progress of BMnarrow BM
o Surgery o If deverticulitis develops, there is an acute onset of
o IVF & antibx mild to severe pain in LLQ, w. N-V, áT, chills, &
leukocytosis
o If untreated, septicemia Øintest – vessles wrapped o Contents from inflamed/infected abd organs leak
around theminfection to blood stream abd cavity
Complications o Bacterial proliferation occurs
o Peritonitis- adb pain, rigid board-like abdomen, loss o Tissue edema follows w/development of
of BS, & S&S of shocksepticemia exudative fluid in a short time
o Abscess formation- Tenderness, palpable mass, F*, o Fluid in peritoneal cavity becomes turbid
leukocytosis w/proteins WBCs, cellular debris, & blood
o Bleeding- Massive rectal bleeding if erosion occurs o Fluid is lost from vascular into peritoneal cavity
into arterial branch o Causes GI hypermotility followed by paralytic ileus
Management ▫ Manifestations Øâvolemia 2.10
o Usually Tx outpatient w/diet & meds o Depends on location
Rest, analgesics, & antispasmodic meds o Early sx are d/t underlying cause
Clear liquids until inflam subsides, then high-fiber, o Starts w/diffuse pain that becomes constant,
low-fat diet recommended localized, & more intense near site of inflam
Antibx & bulk-forming laxatives prescribed o Pain is exacerbated by movement
o Acute cases managed in the hospital o Affected area extremely tender, distended,
NPO w/IVF w/muscle rigidity
NG to control V* or distention o Rebound tenderness & paralytic ileus may be
Broad spectrum antibx 7-10 days present
Opioids for pain (Demerol preferred) o Corticosteroids or analgesics may mask pain
á oral intake as sx improve o N-V & â peristalsis
Low-fiber diet until infect relievedreturn to
o áT (100-1) & P
áfiber
o SOBØ fluid pressure
Antispasmodics may be needed
Bulk products, softeners, or suppositories not –IT ▫ Management of Peritonitis
IS bc hard on inflame, edematous cant maintained o Monitor for compl:
o Surgical management- See Fig. 38-3, p. 1244 Widespread infect leading to sepsis & shock
o If complications occur -> emergency surgery o Need fluid (manage like shock), colloid, &
Procedures electrolyte replacement
o One-stage resection take out inflame sect attach Several liters of isotonic solution is
administered
good end
o Analgesics & antiemetics for pain& N-V
Inflamed area is removed & end-to-end
anastomosis is done o NG suction relieves distentionØrest bowel 2.13
o Multiple-stage o Fluid in abd cavity can restrict lung expansion so
Performed when complications occur O2 per nasal cannula improves oxygenation
Diseased area is resected but no anastomosis done o Antibx in large doses
Both ends of bowel brought out & “double-barrel” o Surgical treatment- remove infected material &
temporary colostomy formed correct underlying cause
When inflam/infect subside, may be reattached in ▫ Nursing Management of Peritonitis
separate procedure o Monitor for post-op complications
1. Nursing care- see p. 1244-45 Wound evisceration
Peritonitis - An inflam of the peritoneum Sudden appearance of serosanguineous
▫ Usually d/t bacterial infect from diseases of the GI drainage strongly suggests wound dehiscence
tract, or in women, the reproductive organs Patient may c/o pain, tenderness, &
▫ Inflam & paralytic ileus (infect, inflame in inteste ) “something gave way”
are the direct effects of infect Abscess formation
▫ Other common causes: spilling of gastric contants ▫ Often in ICU where BP monitored per arterial line &
peritoneum CVP measured via pulmonary arterial wedge
o Appendicitis, perforated ulcers, diverticulitis, & pressure
bowel perforation o Measure UOP & I & O
o Also assoc w/abd surgery & peritoneal dialysis o Evaluate fluid & electrolyte balance
▫ Pathophysiology of Peritonitis o Position w/knees flexed
o Monitor output from surgical drains
o Signs of improvement: T. & HR decrease, Scar tissue & granulomas interfere w/peristalsis
Abdomen softens, BS return, & the presence of causing crampy abd pain
flatus,& BM Abd tenderness & spasm exacerbated by eating
Inflammatory Bowel Disease Weight loss & malnutrition
▫ Two chronic disorders: inflame within the bowel Malabsorp leads to chronic D*
o Crohn’s (regional enteritis) Steatorrhea (fatty stools)
o Ulcerative colitis Other: arthritis, erythema nodosum,
o See Table for 38-4, p. 1247 for comparison conjunctivitis, & oral ulcers
▫ triggered by environmental agents (pesticides, food Ulcerative colitis
additives, tobacco, radiation)Triggeres Usually presents w/exacerbations & remissions
autoimmune responseØ kills antibodies LLQ pain
▫ Allergies & immune disorders also suggested as D* w/rectal bleeding
cause Intermittent tenesmus
▫ NSAIDs tend to exacerbate IBD Pallor, anemia, & fatigue
▫ Pathophysiology of IBS both have Anorexia, weight loss, F*, V*, & dehydration
exacerbation/remission Urgent need to defecate
o Chron’s (Regional) large/small intest, all layers Pass 10-20 liquid stools/day
of intest, areas of inflamed cellsØ separated by Hypocalcemia develops
healthy bowels, (cobble stone), tissue fibrotic, Other: Erythema nodosum, uveitis, arthritis, &
▫ Subacute & chronic inflam of bowel that extends liver disease
through all layers; usually affects distal ileum & Potential Complications of IBS á/r cancer
sometimes ascending colon. Characterized by o Regional Enteritis
periods of remission& exacerabtions.
o Intestinal obstruction or stricture
Begins w/edema & thickening of mucosa. Ulcers
o Perianal disease
appear in inflamed mucosa. These lesions are
o F & E imbalances
separated by normal tissue, taking on a “cobblestone”
appearance. o Malnutrition
Fistulas, fissures, & abscesses formØchronesall o Fistula & abscess formation
layers of colon& sm intest o á/R for colon CA
Granulomas occur in 50% of pts Ulcerative Colitis
Bowel wall thickens, becomes fibrotic, & lumen o Toxic megacolon
narrows o Perforation
Bowel loops can adhere to each other o Bleeding
a. Ulcerative Colitis large intest, submucosa layer, Management of IBS
see bleeding from stool, continueous inflame, stick o Nutrition
together?, Fluids îelec, low-residue, high-protein, high-calorie
Affects superficial mucosa of the colon & diet w. supplm vits & Fe
characterized by multiple ulcerations, diffuse inflam, & Avoid foods that exacerbate condition
shedding of eipthelium Milk, cold foods, smoking
Ulcers cause bleeding o Surgery
Mucosa edematous & inflamed; lesions are o Total colectomy w/ileostomy
contiguous (one after the other) Continent ileostomy- Kock pouchØmore liquid
Cricks Abcesses form & infiltrate is seen in bigger volume
submucosa & submucosa w/clumps of neutrophils Restorative proctocolectomy w/ileal pouch anal
found in the lumen of the cryps that line the mucosa anastomosis- procedure of choice (Fig. 38-5, p.
Process usually begins in the rectum & spreadsd 1251)
proximally to involve the entire colon Pharmacologic Management of IBS
Eventually bowel narrows, shortens, & thickens o Sedatives, antiD*l, & antiperistaltic meds rest bowel
2. Manifestations of IBS o Aminosalicylates Ø sulfasalazine (Azulfidine) Ø mild
Regional Enteritis /Chrones or moderate cases
Insidious onset w RLQ pain o Sulfa-free aminosalicylates (mesalamine [Asacol,
May present w/exacerbations & remissions or Pentasa]) prevent & tx recurrences
progressive o Antibx (metronidazole (Flagyl) Ø 2nd infects
o Corticosteroids- tx severe & fulminant disease absorption of fluids & stimulates more gastric
Stopping triggers disease, continuing leads to SE, secretion -> increases pressure within intestinal
á/r infect, can’t protect lumen-> decreases venous return, increases venous
o Immunomodulators- alter immune response, didn’t pressure, & increases capillary permeability ->
respond to meds
causes edema & congestion-> reduced arterial flow
Azathioprine (AZA), 6-mercaptopurine (6-MP),
methotrexate, cyclosporineØkills some inflame to bowel -> necrosis, & eventual rupture or
triggers perforation of intestinal wall -> peritonitis
For patients who haven’t responded to other ▫ Manifestations of Bowel Obstruction
therapies o Initial symptom: crampy pain that is wavelike &
Nursing Management of IBS colicky
o See Nursing Process & Care Plan p. 1251-1258 o May pass blood & mucus w/o fecal matter or flatus
o Education about diet& meds o V* occursØclosest to the mouth downØempty
o Refer to support groups stomach contents bile jejunumfecal type
o Monitor nutritional & fluid status If obstruction is complete, peristaltic waves are initially
o Promote balance of rest w/activity excessive & eventually reverse direction & move
o Healthy stress management contents up toward mouth
o Eliminate smoking o First vomits stomach contents
o TPN used when sx are severe o Then bile-stained contents (duodenum & jejunum)
High glucose levels can áBS o Eventually fecal-like contents of ileum
High in protein, low in fat & residue so digested o DehydrationØThirst, drowsiness, malaise, aching ,
primarily in jejunum-> doesn’t stimulate intestinal parched tongue & mucous membranes
secretions so bowel continues to rest o Abd distention (lower the obstruction, greater the
Note intolerance such as N-V, D*, or distention distention)
Intestinal Obstruction- Blocks movement of contents o Initially hyperactive BS auscultated proximal to
through GI tract
obstruction then become hypoactive or absent
Two types
o Dx made by X-ray or CT
o Mechanical
Management of Small Bowel Obstruction
Obstruction from pressure on intestinal wall
o NG tube for decompression
Intussusception, polypoid tumors & neoplasms,
o IVF to replace water, sodium, chloride, & K+
stenosis, strictures, adhesions (most common),
hernias, ,abscesses o Complete obstruction w/necrosis requires surgery to
o Fuctional (Neurogenic) cant get the message remove necrotic section
Musculature cannot propel contents forward Nursing care:
Amyloidosis, muscular dystrophy, endocrine Manage NG suction & measure output; note
disorders, & neurological disorders quality
Can be temporary & result from manipulation of Assess for fluid & electrolyte imbalances
the bowel during surgery Monitor nutritional status
o Partial or Complete Note return of bowel sounds, flatus,& BM
Monitor distention
o Vascular FactorsØblood is not supplied to a part of
Monitor& manage pain
intestine unable to perform norm peristaltic
Large Bowel Obstruction Pathophysiology: less
fxischemicabd pain áWBC, T, peritonitis fx-
dramatic than small isn’t complete bc fecal
ápermleak bacteriashock.
resorvior, distensible,
o Obstruction results in an accumulation of intestinal
Pathophysiology of Small Bowel Obstruction
contents, fluids, & gas proximal to obstruction
(SBO)
severe distention & perforation unless gas & fluid can
▫ Obstruction coming from that decendsloosing
flow back through ideal valve
fluids stim Gastric secterion â pressure blood o Even if complete may be undramatic if the blood
edema congestinartierial supply is not disturbed
bloodishemiadeathmore peritonitis 52.5 o c. If the blood supply is cut off, intestinal
▫ Intestinal contents, fluid, & gas accumulate above the strangulation & necrosis occurs-> life-threatening
obstruction Distention & fluid retention reduces
o Dehydration occurs more slowly b/c colon can o r in bowel habits
absorb its fluid contents & can distend to a size well o Passage of blood in stool 2nd most common symptom
beyond its normal size o Other: unexplained anemia, weight loss, & fatigue
o Adenocarcinoid tumors account for majority of cases ▫ Right-sided lesions: Dull abd pain & melena
Manifestations of Large Bowel Obstruct ▫ Left-sided lesions: Sx assoc w/obstruction ->Abd
o Sx develop & progress slowly pain & cramping, narrowing stools, constipation,
o Constipation only sx for months distention
o Shape of stool altered by obstructionØlrg growth in o Bright-red blood in stool
colonsquishes ▫ Rectal lesions: Tenesmus, rectal pain, feeling of
o Blood in stool from tumor or Fe defic anemia incomplete evacuation after BM, alternating *C & D*,
o weakness, weight loss, & anorexia & bloody stools
o Eventually abd distended Assessment & Dx
o Loops of bowel may become visible through abd wall ▫ Positive fecal occult blood
o Crampy lower abd pain ▫ Barium enema & endoscopic procedures reveal
o Few~Fecal V* eventually develops abnormal tissue on biopsy & cytology smear
▫ Carcinoembryonic antigen (CEA)- Not highly
o Sx of shock may occur
reliable, but elevations positive for CA
o DxØ X-ray, CT, or MRI
~With complete tumor excision, CEA returns to
Management of Lg Bowel Obstruction normal within 48 hours& later elevations suggest
o Restore intravascular volume recurrence
o Correct electrolyte abnormalities ▫ Most common complication is bowel obstruction
o NG Ø decompress bowel Management of Colorectal CA
o Colonoscopy may be performed to untwist & ▫ If obstruction present, treat that w/fluids & NG
decompress bowel ▫ Tumor treatment depends on stage:
o May insert rectal tube o Surgery to remove tumor
o Temporary or permanent colostomy may be needed o Supportive therapy
Nursing care: o Adjuvant therapy- typically delays tumor recurrence
o Monitor for worsening sx & increases survival time
o Provide emotional support & comfort Chemotherapy
Colorectal Cancer Radiation
Relatively common; 3rd most common site of new CA Immunotherpay
cases & deaths in US Multimodal therapy
A disease of Western cultures Hirschsprung’s Disease
á/RØ age, family hx, those w. IBD or polyps Most common cause of lower GI obstruction in
Cause not known neonate
▫ È screening – â deaths ▫ Occurs in 1:5000 children w/4:1 ratio male : female
▫ Early dx & prompt treatment could save almost 3 of 4 ▫ Caused by congenital absence of some or all of
persons normal bowel ganglion cells, beginning at anus,
▫ 90% 5-year survival rate is detected early; survival extending variable lengths
rates very low w/late diagnosis ▫ DxØ barium enema
▫ Unfortumately, most are asymptomatic for long ▫ S&S: Extremely dilated colon & chronic constipation,
periods & seek health care only when they notice a fecal impaction, & overflow D*Øfecal matter goes
change in bowel habits or rectal bleeding around obst.
Pathophysiology of Colorectal CA ▫ TxØ Surgically resect affected segment & reattach
o 95% - adenocarcinoma lrg bowel obstruct, polyps healthy bowel
become malignant, clip to â Malignant (arising from ▫ Nursing: Encourage bonding, prepare 4
epithelial lining of intestine) interventions, explain that colostomy will be
o May start as a benign polyp that becomes malignant- temporary
> invades & destroys normal tissues-> extends into Pyloric Stenosis Narrowing of pyloric orifice, food
surrounding structures stomachsmall intest.
o Cells may migrate to other areas (often the liver) In children, excessive thickening of the pyloric
▫ Manifestations of Colorectal CA sphincter or átrophy & plasia of mucosa &
o Sx determined by location, stage, & fx of segment submucosa of pylorus is responsible
TxØ w/revision of the muscles of the pylorus
▫ Celiac Disease Malabsorp or gluten-induced
enteropathy
o A sensitivity or immunologic response to protein,
especially protein found in grains
o When child ingests gluten, intestinal mucosa or villi
changes & prevents absorption of food into blood
o Children develop inability to absorb fat
S & S:
o Cramp, abd pain, unable to absorb food, nutrients
cant blood stream
o Steatorrhea (elim fat bc cant use) & defic in fat-
soluble vits (A, D, E, & K)
o Malnutrition, distended abdomen & possible rickets
o Hypoprothombinemia loss of Vit K
o hypochormic anemia (Fe deficiency)
o â albuminemia Ø poor protein absorption
▫ Relatively rare condition, but needs early recognition
to prevent complications
▫ Affects children of northern European inherited
illness
▫ different degrees of involvement
▫ á incidence in Down’s synd
Treatment:
o Educated about following a gluten-free diet for life
o Prone to GI CA later in life if diet not followed
o Celiac crisis:
o When child develops any type of infect, a crisis of
extreme sx may occur
Acute V & D
Rapid F & E imbal Ø immediate, intensive therapy
Anda mungkin juga menyukai
- Gastrointestinal SystemDokumen7 halamanGastrointestinal SystemSofia P. PanlilioBelum ada peringkat
- p1w1 Nur149 Session 1Dokumen75 halamanp1w1 Nur149 Session 1Alliah Marie CababarosBelum ada peringkat
- Accessory OrgansDokumen6 halamanAccessory OrgansNadia AbdurasidBelum ada peringkat
- Stomach: Clinical Clerk: Jarney Dyenn Bito-OnonDokumen44 halamanStomach: Clinical Clerk: Jarney Dyenn Bito-OnonLajel S. LachicaBelum ada peringkat
- Gastro-Intestinal System Diagnostic TestsDokumen11 halamanGastro-Intestinal System Diagnostic TestsFev BanataoBelum ada peringkat
- GI Liver PerceptionDokumen9 halamanGI Liver PerceptionJUDE ARIZALABelum ada peringkat
- Nursing of Clients With Gastrointestinal DisordersDokumen228 halamanNursing of Clients With Gastrointestinal DisordersLane Mae Magpatoc Noerrot100% (1)
- Gastrointestinal Disorders PnleDokumen23 halamanGastrointestinal Disorders Pnledelieup02100% (2)
- Finals Pedia EncodedDokumen62 halamanFinals Pedia EncodedCezanne Danabelle HutallaBelum ada peringkat
- Metabolic DisturbancesDokumen34 halamanMetabolic DisturbancesKyle DapulagBelum ada peringkat
- Rad Contrast MidtermDokumen29 halamanRad Contrast Midtermmaxineanne.alberto.mnlBelum ada peringkat
- GerdDokumen34 halamanGerdPriyankaBelum ada peringkat
- Medsurg Gi AnaphysioDokumen13 halamanMedsurg Gi AnaphysioNermeen Mudsol100% (1)
- ConciseDokumen10 halamanConciseLeiBelum ada peringkat
- Hepatobiliary and Pancreatic DisordersDokumen12 halamanHepatobiliary and Pancreatic DisordersMiden AlbanoBelum ada peringkat
- Medical-Surgical NCLEX Practice QUIZ Flashcards - QuizletDokumen9 halamanMedical-Surgical NCLEX Practice QUIZ Flashcards - QuizletErika Bacarro100% (1)
- Gastro HandoutDokumen16 halamanGastro HandoutAud SyneBelum ada peringkat
- Med Surg 2 - 2 Diagnostic Examinations For Gastrointestinal SystemDokumen18 halamanMed Surg 2 - 2 Diagnostic Examinations For Gastrointestinal SystemMaxinne RoseñoBelum ada peringkat
- NCM 116 Gep MidtermDokumen20 halamanNCM 116 Gep MidtermKM PanganibanBelum ada peringkat
- Gastrointestinal System: Anatomy Physiology &disordersDokumen52 halamanGastrointestinal System: Anatomy Physiology &disordersprabha5050100% (1)
- OmdDokumen19 halamanOmdNadiya SafitriBelum ada peringkat
- Digestive System: Diagnostic Tests For Diseases of The Digestive SystemDokumen14 halamanDigestive System: Diagnostic Tests For Diseases of The Digestive Systemmai-maiBelum ada peringkat
- Gastrointestinal Tract: Monometric StudiesDokumen9 halamanGastrointestinal Tract: Monometric StudiesJosh LimBelum ada peringkat
- GIT Assessment & PEDokumen56 halamanGIT Assessment & PEMargaret Xaira Rubio MercadoBelum ada peringkat
- The GI System Is Composed of Two General Parts Gi TractDokumen14 halamanThe GI System Is Composed of Two General Parts Gi TractRexson Alcantara DalanginBelum ada peringkat
- Surgery2 07 Stomach and Small IntestineDokumen85 halamanSurgery2 07 Stomach and Small Intestinezein0217zienBelum ada peringkat
- Gastrointestinal SystemDokumen17 halamanGastrointestinal SystempreetBelum ada peringkat
- 2018.surgery Intestinal Obstruction in Infants and ChildrenDokumen11 halaman2018.surgery Intestinal Obstruction in Infants and ChildrenFranz SalazarBelum ada peringkat
- Gastrointestinal SystemDokumen9 halamanGastrointestinal SystemMikaella CondeBelum ada peringkat
- Peptic Ulcer Concept MapDokumen17 halamanPeptic Ulcer Concept MappotchistroberriBelum ada peringkat
- Gastric Fluid AnalysisDokumen3 halamanGastric Fluid AnalysisanonacadsBelum ada peringkat
- Gastroschisis Final PresentationDokumen43 halamanGastroschisis Final PresentationlhedavenBelum ada peringkat
- GI - Secretions - NASPGHAN - Picture RemovedDokumen56 halamanGI - Secretions - NASPGHAN - Picture Removedmalikbaseerat32Belum ada peringkat
- 116 - Alterations in GI EliminationDokumen12 halaman116 - Alterations in GI EliminationGino-o, KyleBelum ada peringkat
- Obstetrics - GastrointestinalDokumen6 halamanObstetrics - GastrointestinalJonathanBelum ada peringkat
- CONCEPT MAP HirschsprungsDokumen3 halamanCONCEPT MAP Hirschsprungskaycee gwapaBelum ada peringkat
- A&p - All Files in OneDokumen104 halamanA&p - All Files in OneElvira MirandaBelum ada peringkat
- Short Written Mock 2021 Mn1 - AnsweredDokumen20 halamanShort Written Mock 2021 Mn1 - AnsweredMatthew NgBelum ada peringkat
- GIT Fully DoneDokumen14 halamanGIT Fully DoneTirtha Taposh100% (1)
- E-Learning Midterm BSN-IV 1Dokumen18 halamanE-Learning Midterm BSN-IV 1Ahmad BaolayyanBelum ada peringkat
- Placino GASTROINTESTINALDokumen37 halamanPlacino GASTROINTESTINALSienaBelum ada peringkat
- 1 Gastrointestinal System DisordersDokumen14 halaman1 Gastrointestinal System DisordersAnna Sofia Reyes100% (1)
- Gastrointestinal System DisordersDokumen112 halamanGastrointestinal System DisordersTaate MohammedBelum ada peringkat
- Ms Prelim NewDokumen12 halamanMs Prelim NewJane LaquihonBelum ada peringkat
- 4.special Methods and Clinical Identification in Digestive SystemDokumen37 halaman4.special Methods and Clinical Identification in Digestive SystemToafan MegaBelum ada peringkat
- UntitledDokumen44 halamanUntitledKaye A. JardinicoBelum ada peringkat
- Intestinal DisordersDokumen11 halamanIntestinal DisorderspulmonologistBelum ada peringkat
- MS PrelimsDokumen50 halamanMS PrelimsDhawell AnnBelum ada peringkat
- GI SimDokumen5 halamanGI SimIyath SaeedBelum ada peringkat
- SX Unit NotesDokumen4 halamanSX Unit NotesAilyn Capitin BacunawaBelum ada peringkat
- MEDSURG 1 NotesDokumen43 halamanMEDSURG 1 NotesNEIL NETTE S. REYNALDOBelum ada peringkat
- Gastrointestinal and HepatobiliaryDokumen54 halamanGastrointestinal and Hepatobiliaryjeshema100% (2)
- Internal Medicine Qs For GP Saudi PrometricDokumen140 halamanInternal Medicine Qs For GP Saudi PrometricM A100% (4)
- 2 CARE OF CLIENTS GERD HIATAL HERNIA ACHALASIA PUD GI BLEEDING FinalDokumen114 halaman2 CARE OF CLIENTS GERD HIATAL HERNIA ACHALASIA PUD GI BLEEDING Finalevren yilmazBelum ada peringkat
- Orca Share Media1529402803039Dokumen44 halamanOrca Share Media1529402803039LHARA KHAYOGBelum ada peringkat
- Penyakit DigestiDokumen131 halamanPenyakit DigestiGigih Prila Aditama100% (1)
- Necrotizing Enterocolitis ProtocolDokumen3 halamanNecrotizing Enterocolitis Protocoleddy riachyBelum ada peringkat
- Tumor Boards Final 2 EditedDokumen64 halamanTumor Boards Final 2 Editedsjmc.surgeryresidentsBelum ada peringkat
- Group 4 Diet For Peptic Ulcer Pre and Post OpDokumen7 halamanGroup 4 Diet For Peptic Ulcer Pre and Post OpJanela TaboraBelum ada peringkat
- Gastritis Definition: Gastritis Can Be An Acute orDokumen46 halamanGastritis Definition: Gastritis Can Be An Acute orOdey BeekBelum ada peringkat
- MS 2 P1 Part 1 PDFDokumen17 halamanMS 2 P1 Part 1 PDFAngel YN Patricio FlorentinoBelum ada peringkat
- Gi - PathophysiologyDokumen96 halamanGi - Pathophysiologyjmosser100% (4)
- IbandronatedrugscomDokumen25 halamanIbandronatedrugscomroyBelum ada peringkat
- PU Perforation (Text)Dokumen9 halamanPU Perforation (Text)Hart ElettBelum ada peringkat
- Gastro Intestinal SystemDokumen9 halamanGastro Intestinal SystemJe Lyn100% (1)
- Peptic UlcerDokumen4 halamanPeptic UlcerNathalie DeebBelum ada peringkat
- Citicoline Mode of ActionDokumen5 halamanCiticoline Mode of ActionBeverlyBelum ada peringkat
- GRDDS., NDDSDokumen19 halamanGRDDS., NDDSGauri RautBelum ada peringkat
- Welcome To TampcolDokumen5 halamanWelcome To TampcolmurugangdBelum ada peringkat
- Medical-Surgical Nursing Exam 20: NLE Style (100 Items) : Answers & RationaleDokumen15 halamanMedical-Surgical Nursing Exam 20: NLE Style (100 Items) : Answers & RationaleHasan A AsFourBelum ada peringkat
- Chemistry Project To Determine Which Antacid Neutralizers Stomach Acid MostDokumen4 halamanChemistry Project To Determine Which Antacid Neutralizers Stomach Acid MostAnsia MeenazBelum ada peringkat
- Oana EnglezaDokumen83 halamanOana EnglezaOana SovarBelum ada peringkat
- Internal MedicineDokumen195 halamanInternal Medicineصقر حورانBelum ada peringkat
- Gram RodsDokumen223 halamanGram RodsGeric Sam LopezBelum ada peringkat
- Consultation TrackerDokumen103 halamanConsultation TrackerEdson AbdonBelum ada peringkat
- 8th March 2020 Plab 1 MockDokumen33 halaman8th March 2020 Plab 1 MockZoha Qureshi100% (1)
- IMEDICS AKT Errors FINALDokumen24 halamanIMEDICS AKT Errors FINALUmer AnwarBelum ada peringkat
- Perforated Peptic Ulcer DiseaseDokumen9 halamanPerforated Peptic Ulcer DiseaseMade Oka HeryanaBelum ada peringkat
- Ws Viii Dyspepsia - Dr. Ignatia Sinta Murti, SP - Pd-KgehDokumen79 halamanWs Viii Dyspepsia - Dr. Ignatia Sinta Murti, SP - Pd-KgehSriHandaryatiBelum ada peringkat
- Angina PectorisDokumen7 halamanAngina PectorisMOGHEEZ AHMEDBelum ada peringkat
- Hep & GIT Final MCQ 21 BDokumen23 halamanHep & GIT Final MCQ 21 BBaraa Elmasedy100% (3)
- Answers Surgery ExamDokumen17 halamanAnswers Surgery ExamKing Bal94Belum ada peringkat
- OMEPRAZOLEDokumen2 halamanOMEPRAZOLEkaye barrionBelum ada peringkat
- Holistic Health Solutions PDFDokumen667 halamanHolistic Health Solutions PDFBhargavaBelum ada peringkat
- Medical-Surgical Nursing Assessment and Management of Clinical Problems 9e Chapter 42Dokumen16 halamanMedical-Surgical Nursing Assessment and Management of Clinical Problems 9e Chapter 42sarasjunkBelum ada peringkat
- Gastric Antral Perf in 15 Yr BoyDokumen29 halamanGastric Antral Perf in 15 Yr BoyRajesh MenonBelum ada peringkat
- H. PyloriDokumen5 halamanH. PyloriWaleed El SaidBelum ada peringkat
- Reiki Rays: The Solar Plexus ChakraDokumen8 halamanReiki Rays: The Solar Plexus ChakraJohn Best100% (1)