Extracapsular Cataract Extraction (ECCE) Is A Category of Eye Surgery in Which
Diunggah oleh
Ma Christina RabayaDeskripsi Asli:
Judul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Extracapsular Cataract Extraction (ECCE) Is A Category of Eye Surgery in Which
Diunggah oleh
Ma Christina RabayaHak Cipta:
Format Tersedia
Extracapsular cataract extraction (ECCE) is a category of eye surgery in which the lens of the eye is removed while the
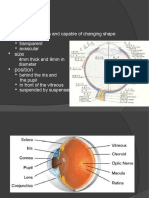
elastic capsule that covers the lens is left partially intact to allow implantation of an intraocular lens (IOL). This approach is contrasted with intracapsular cataract extraction (ICCE), an older procedure in which the surgeon removed the complete lens within its capsule and left the eye aphakic (without a lens). The patient's vision was corrected after intracapsular extraction by extremely thick eyeglasses or by contact lenses. There are two major types of ECCE: manual expression, in which the lens is removed through an incision made in the cornea or the sclera of the eye; and phacoemulsification, in which the lens is broken into fragments inside the capsule by ultrasound energy and removed by aspiration. Purpose Historical background The purpose of ECCE is to restore clear vision by removing a clouded or discolored lens and replacing it with an IOL. Cataract operations are among the oldest recorded surgical procedures; there are references to cataract surgery in the Code of Hammurabi in 1750 B . C . and in the treatises written around 600 B . C . by Susruta, a famous surgeon from India. In the ancient world, lenses damaged by cataracts were dislocated rather than removed in the strict sense; the surgeon used a lance to push the clouded lens backward into the vitreous body of the eye. This operation, known as couching, was standard practice until the mid-eighteenth century. Couching is still performed by some traditional healers in Africa and parts of Asia. The first extracapsular extraction of a cataract was performed by a French surgeon named Jacques Daviel in 1753. Daviel removed the lens through a fairly long incision in the cornea of the eye. In 1865, the German ophthalmologist Albrecht von Graefe refined the operation by removing the lens through a much smaller linear incision in the sclera of the eye. After von Graefe, however, intracapsular extraction gradually became the favored method of cataract removal even though it left the patient without a lens inside the eye. The two inventions that made extracapsular extraction preferable again were the operating microscope and the intraocular lens. The first eye surgery performed with an operating microscope was done in Portland, Oregon, in 1948; in the same year, a British ophthalmologist named Harold Ridley implanted the first IOL in the eye of a cataract patient. Between 1948 and the 1980s, manual expression was the standard form of ECCE. Although phacoemulsification was first introduced in 1967, it was not widely accepted at first because it requires special techniques that take time for the surgeon to learn as well as expensive specialized equipment. As of 2003, phacoemulsification is now performed more often in the United States and Europe than "standard" ECCE. The manual expression technique, however, is still widely used in developing countries with large numbers of patients with eye disorders and limited hospital budgets. The lens and cataract formation To understand cataract surgery, it is helpful to have a basic description of the structure of the lens in the human eye. The lens, which is sometimes called the
crystalline lens because it is transparent, is located immediately behind the iris. In humans, the lens is about 9 mm long and 4 mm wide. It consists of protein fibers and water, with the fibers arranged in a pattern that allows light to pass through the lens. There are three layers of cells in the lens: a central nucleus, which becomes denser and harder as a person ages; a cortex surrounding the nucleus, which contains cells that are metabolically active and continue to grow and divide; and a layer of cells between the cortex and the lens capsule known as the subcapsular epithelium. Although a few people are born with cataracts or develop them in childhood, most cataracts are the result of the aging process. As people grow older, the protein fibers in the lens become denser, start to clump together, and form cloudy or opaque areas in the lens. Cataracts vary considerably in their speed of progression; they may develop in a few months or over a period of many years. Some people have cataracts that stop growing at an early stage of development and do not interfere with their vision. Although most people develop cataracts in both eyes, they do not usually progress at the same rate, so that the person has much better vision in one eye than in the other. Ophthalmologists classify cataracts according to their location in the lens. It is possible for a person to have more than one type of cataract. Nuclear cataracts. Nuclear cataracts grow slowly over many years but can become very large and hard, which complicates their removal. They are sometimes called brunescent cataracts because they are characterized by deposits of brown pigment that give the lens an amber color. Nuclear cataracts are most commonly associated with age and with smoking as risk factors. Cortical cataracts. Cataracts in the cortex of the lens develop more rapidly than nuclear cataracts but remain softer and are easier to remove. They are thought to be caused by an increase in the water content of the lens. Risk factors for cortical cataracts include female sex and African or Caribbean heritage. Posterior subcapsular (PSC) cataracts. This type of cataract, which develops between the back of the lens and the lens capsule, is the softest and most rapidly growing type. PSC cataracts tend to scatter light at night and thus interfere with nighttime driving. Risk factors for PSC cataracts include diabetes and a history of treatment with steroid medications. Demographics Cataract extraction is one of the most frequently performed surgical procedures in industrialized countries. It is estimated that 300,000400,000 cases of visually disabling cataracts occur each year in the United States alone, and that between 1 and 1.5 million cataract extractions are performed annually in the United States. This frequency reflects the importance of cataracts as a In extracapsular cataract extraction, an incision is made in the eye just beneath the iris, or colored part (A). The diseased lens is pulled out (B). A prosthetic intraocular lens is placed through the incision (D), and is opened to replace the old lens (E). (Illustration by GGS Inc.)
major public health problem. The World Health Organization (WHO) estimated in 1997 that cataracts are responsible for 50% of cases of blindness around the world, or 19 million people. By 2020, that figure is expected to rise to 50 million. More recent publications estimate that 1.2% of the general population of Africa is blind, with cataracts responsible for 36% of these cases of blindness. About one person in every 50 in the general American population will eventually have to have a cataract removed. It is difficult, however, to compare the rates of cataract formation among various subgroups because present published studies use a number of different grading systems for defining and detecting cataracts. In addition, the elderly are often under-represented in general population studies even though age is the greatest single risk factor for cataract development. Three recent research projects carried out in the United States, Australia, and England, respectively, reported that 50% of people over the age of 60 have some degree of cataract formation, with the figure rising to 100% for those over 80. As of 2003, little conclusive information is available regarding the incidence of cataracts in different racial and ethnic groups in the United States. A variety of risk factors in addition to age have been associated with cataracts, but their precise significance is debated among researchers: Genetic factors. Twin studies show that the identical twin of a patient with a nuclear cataract has a 48% chance of developing one. Sex. Women are slightly more likely than men to develop cataracts. One American study found that 53.3% of women over 60 had nuclear cataracts compared to 49.7% of the men; 25.9% of the women had cortical cataracts versus 21.1% of the men. Exposure to ultraviolet radiation. Cortical cataracts are more likely to develop in people with frequent exposure to sunlight; however, nuclear cataracts are not related to sun exposure. Smoking. People who smoke more than 25 cigarettes per day are three times as likely as nonsmokers to develop nuclear or PSC cataracts. Smoking does not appear to be related to cortical cataracts. Alcohol consumption. Heavy drinking has been reported to increase the risk of developing all three types of cataracts. Diabetes. Patients with diabetes are at increased risk of developing all three types of cataracts. Use of steroid medications. PSC cataracts are known to be induced by steroids, even though they represent less than 10% of all cataracts. Socioeconomic status (SES). People with college or professional-school education have lower rates of cataract formation than people who did not finish high school, even attempting to correct for environmental and nutritional factors. There is, however, no obvious biochemical or medical explanation for this correlation, and some researchers treat it with caution.
Chronic dehydration, diarrhea, and malnutrition. Studies carried out in India indicate that severe malnutrition or repeated episodes of diarrhea in childhood carry a threeto fourfold increase in risk of developing cataracts in later life. It is not yet known, however, whether this statistic would hold true for people in other countries. Description Conventional extracapsular cataract extraction Although phacoemulsification has become the preferred method of extracapsular extraction for most cataracts in the United States since the 1990s, conventional or standard ECCE is considered less risky for patients with very hard cataracts or weak epithelial tissue in the cornea. The ultrasound vibrations that are used in phacoemulsification tend to stress the cornea. A conventional extracapsular cataract extraction takes less than an hour to perform. After the area around the eye has been cleansed with antiseptic, sterile drapes are used to cover most of the patient's face. The patient is given either a local anesthetic to numb the tissues around the eye or a topical anesthetic to numb the eye itself. An eyelid holder is used to hold the eye open during the procedure. If the patient is very nervous, the doctor may administer a sedative intravenously. After the anesthetic has taken effect, the surgeon makes an incision in the cornea at the point where the sclera and cornea meet. Although the typical length of a standard ECCE incision was 1012 mm in the 1970s, the development of foldable acrylic IOLs has allowed many surgeons to work with incisions that are only 56 mm long. This variation is sometimes referred to as small-incision ECCE. After the incision is made, the surgeon makes a circular tear in the front of the lens capsule; this technique is known as capsulorrhexis. The surgeon then carefully opens the lens capsule and removes the hard nucleus of the lens by applying pressure with special instruments. After the nucleus has been expressed, the surgeon uses suction to remove the softer cortex of the lens. A special viscoelastic material is injected into the empty lens capsule to help it keep its shape while the surgeon inserts the IOL. After the intraocular lens has been placed in the correct position, the viscoelastic substance is removed and the incision is closed with two or three stitches. Phacoemulsification In phacoemulsification, the surgeon uses an ultra-sound probe inserted through the incision to break up the nucleus of the lens into smaller pieces. The newer technique offers the advantages of a smaller incision than standard ECCE, fewer or no stitches to close the incision, and a shorter recovery time for the patient. Its disadvantages are the need for specialized equipment and a steep learning curve for the surgeon. One study found that surgeons needed to perform about 150 cataract extractions using phacoemulsification before their complication rates fell to a baseline level. Diagnosis/Preparation Diagnosis The diagnosis of cataract is usually made when the patient begins to notice changes
in his or her vision and consults an eye specialist. In contrast to certain types of glaucoma, there is no pain associated with the development of cataracts. The specific changes in the patient's vision depend on the type and location of the cataract. Nuclear cataracts typically produce symptoms known as myopic shift (in nearsighted patients) and second sight (in farsighted patients). What these terms mean is that the nearsighted person becomes more nearsighted while the farsighted person's near vision improves to the point that there is less need for reading glasses. Cortical and posterior subcapsular cataracts typically reduce visual acuity; in addition, the patient may also complain of increased glare in bright daylight or glare from the headlights of oncoming cars at night. Because visual disturbances may indicate glaucoma as well as cataracts, particularly in older adults, the examiner will first check the intraocular pressure (IOP) and the anterior chamber of the patient's eye. The examiner will also look closely at the patient's medical history and general present physical condition for indications of diabetes or other systemic disorders that affect cataract development. The next step in the diagnostic examination is a test of the patient's visual acuity for both near and far distances, commonly known as the Snellen test. If the patient has mentioned glare, the Snellen test will be conducted in a brightly lit room. The examiner will then check the patient's eyes with a slit lamp in order to evaluate the location and size of the cataract. After the patient's eyes have been dilated with eye drops, the slit lamp can also be used to check the other structures of the eye for any indications of metabolic disorders or previous eye injury. Lastly, the examiner will use an ophthalmoscope to evaluate the condition of the optic nerve and retina at the back of the eye. The ophthalmoscope can also be used to detect the presence of very small cataracts. Imaging studies of the eye (ultrasound, MRI, or CT scan) may be ordered if the doctor cannot see the back of the eye because of the size and density of the cataract. Preparation ECCE is almost always elective surgeryemergency removal of a cataract is performed only when the cataract is causing glaucoma or the eye is severely injured or infected. After the surgery has been scheduled, the patient will need to have special testing known as keratometry if an IOL is to be implanted. The testing, which is painless, is done to determine the strength of the IOL needed. The ophthalmologist measures the length of the patient's eyeball with ultrasound and the curvature of the cornea with a device called a keratometer. The measurements obtained by the keratometer are entered into a computer that calculates the correct power for the IOL. The IOL is a substitute for the lens in the patient's eye, not for corrective lenses. If the patient was wearing eyeglasses or contact lenses before the cataract developed, he or she will continue to need them after the IOL is implanted. The lens prescription should be checked after surgery, however, as it is likely to need adjustment. Aftercare
Patients can use their eyes after ECCE, although they should have a friend or relative drive them home after the procedure. The ophthalmologist will place some medicationsusually steroids and antibioticsin the operated eye before the patient leaves the office. Patients can go to work the next day, although the operated eye will take between three weeks and three months to heal completely. At the end of this period, they should have their regular eyeglasses checked to see if their lens prescription should be changed. Patients can carry out their normal activities within one to two days of surgery, with the exception of heavy lifting or extreme bending. Most ophthalmologists recommend that patients wear their eyeglasses during the day and tape an eye shield over the operated eye at night. They should wear sunglasses on bright days and avoid rubbing or bumping the operated eye. In addition, the ophthalmologist will prescribe eye drops for one to two weeks to prevent infection, manage pain, and reduce swelling. It is important for patients to use these eye drops exactly as directed. Patients recovering from cataract surgery will be scheduled for frequent checkups in the first few weeks following ECCE. In most cases, the ophthalmologist will check the patient's eye the day after surgery and about once a week for the next several weeks. About 25% of patients who have had a cataract removed by either extracapsular method will eventually develop clouding in the lens capsule that was left in place to hold the new IOL. This clouding, which is known as posterior capsular opacification or PCO, is not a new cataract but may still interfere with vision. It is thought to be caused by the growth of epithelial cells left behind after the lens was removed. PCO is treated by capsulotomy, which is a procedure in which the surgeon uses a laser to cut through the clouded part of the capsule. Risks The risks of extracapsular cataract extraction include: Edema (swelling) of the cornea. A rise in intraocular pressure (IOP). Uveitis. Uveitis refers to inflammation of the layer of eye tissue that includes the iris. Infection. Infection of the external eye may develop into endophthalmitis, or infection of the interior of the eye. Hyphema. Hyphema refers to the presence of blood inside the anterior chamber of the eye and is most common within the first two to three days after cataract surgery. Leaking or rupture of the incision. Retinal detachment or tear. Malpositioning of the IOL. This complication can be corrected by surgery. Cystoid macular edema (CME). The macula is a small yellowish depression on the
retina that may be affected after cataract surgery by fluid collecting within the tissue layers. The patient typically experiences blurring or distortion of central vision. CME rarely causes loss of sight but may take between two and 15 months to resolve completely. Normal results Extracapsular cataract extraction is one of the safest and most successful procedures in contemporary eye surgery; about 95% of patients report that their vision is substantially improved after the operation. In the words of a British ophthalmologist, "The only obstacle lying between cataract sufferers and surgical cure is resource allocation." Morbidity and mortality rates Mortality as a direct result of cataract surgery is very rare. On the other hand, several studies have indicated that patients over the age of 50 who undergo cataract extraction have higher rates of mortality in the year following surgery than other patients in the same age group who have other types of elective surgery . Some researchers have interpreted these data to imply that cataracts related to the aging process reflect some kind of systemic weakness rather than a disorder limited to the eye. About 23% of patients who have undergone cataract extraction have a postoperative complication. The majority of these, however, are not vision-threatening. The most common complication is swelling of the cornea (9.5%), followed by raised IOP (7.9%); uveitis (5.6%); leaking from the incision (1.2%); hyphema (1.1%); external eye infection (0.06%); endophthalmitis (0.03%); retinal detachment (0.03%); retinal tear (0.02%), and CME (0.017%). Of these complications, only endophthalmitis and retinal detachment or tear are considered potentially vision-threatening. Standard ECCE and phacoemulsification have very similar success rates and complication rates when performed by surgeons of comparable skill and length of experience. Alternatives Medical treatment As of 2003 there are no medications that can prevent or cure cataracts. Many ophthalmologists, however, recommend a well-balanced diet as beneficial to the eyes as well as the rest of the body, on the grounds that some studies suggest that poor nutritional status is a risk factor for cataract. While vitamin supplements do not prevent cataracts, there is some evidence that an adequate intake of vitamins A, C, and E helps to slow the rate of cataract progression. Elderly people who may be at risk of inadequate vitamin intake due to loss of appetite and other reasons may benefit from supplemental doses of these vitamins. Watchful waiting Not all cataracts need to be removed. A patient whose cataracts are not interfering
with his or her normal activities and are progressing slowly may choose to postpone surgery indefinitely. It is important, however, to have periodic checkups to make sure that the cataract is not growing in size or density. In the recent past, surgeons often advised patients to put off surgical treatment until the cataract had "ripened," which meant that the patient had to wait until the cataract had caused significant vision loss and was interfering with reading, driving, and most daily activities. At present, ophthalmologists prefer to remove cataracts before they get to this stage because they are harder and consequently more difficult to remove. In addition, a rapidly growing cataract that is not treated surgically may lead to swelling of the lens, secondary glaucoma, and eventual blindness. In most cases, however, it is up to the patient to decide when the cataract is troublesome enough to schedule surgery. Surgical alternatives The major surgical alternative to ECCE is intracapsular cataract extraction, or ICCE. It is rarely performed at present in Europe and North America, but is still done in countries where operating microscopes and high-technology equipment are not always available. In ICCE, the surgeon makes an incision about 150 degrees of arc, or about half the circumference of the cornea, in order to extract the lens and its capsule in one piece. The surgeon then inserts a cryoprobe, which is an instrument for applying extreme cold to eye tissue. The cryoprobe is placed on the lens capsule, where it freezes into place. It is then used to slowly pull the capsule and lens together through the long incision around the cornea. Because of the length of the incision needed to perform ICCE and the pressure placed on the vitreous body, the procedure has a relatively high rate of complications. In addition, the recovery period is much longer than for standard ECCE or phacoemulsification. PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED? Cataract surgery is performed by ophthalmologists, who are physicians who have completed four to five years of specialized training following medical school in the medical and surgical treatment of eye disorders. Ophthalmology is one of 24 specialties recognized by the American Board of Medical Specialties.If cataract surgery is being considered, it is a good idea to find out how many extracapsular extractions the surgeon performs each year. The greatest single factor in the success rate of ECCE procedures is not whether the surgeon performs a standard extraction or phacoemulsification, but the volume of operations that he or she performs. Surgeons who perform between 200 and 400 extracapsular extractions per year have higher rates of successful outcomes than those who perform fewer than 200. Extracapsular cataract extractions are done as outpatient procedures, either in the ophthalmologist's office or in an ambulatory surgery center. Read more: Extracapsular Cataract Extraction - procedure, recovery, test, blood, removal, pain, complications, adults, time, infection, operation, cells, types, risk, rate, Definition, Purpose, Demographics
NURSING CARE PLAN OF CATARACT Cataracts are the leading cause of preventable blindness among adults in the United States. Theincidence of cataracts in the United States is 1.2 to 6.0 cases per 10,000 people. A cataract isdefined as opacity of the normally transparent lens that distorts the image projected on the retina.The lens opacity reduces visual acuity. As the eye ages, the lens loses water and increases in sizeand density, causing compression of lens fibers. A cataract then forms as oxygen uptake isreduced, water content decreases, calcium content increases, and soluble protein becomesinsoluble. Over time, compression of lens fibers causes a painless, progressive loss of transparency that is often bilateral. The rate of cataract formation in each eye is seldom identical.Without surgery, a cataract can lead to blindness.Cataract a common cause of gradual vision loss is opacity of the lens or the lens capsule of theeye. The clouded lens blocks light shining through the cornea. This block, in turn, blurs theimage cast onto the retina. As a result, the brain interprets a hazy image. Cataracts commonlyaffect both eyes, but each cataract progresses independently. Exceptions are traumatic cataracts,which are usually unilateral, and congenital cataracts, which may remain stationary. Cataractsare most prevalent in people older than age 70. Surgery restores vision in about 95% of patients. CAUSES Cataracts have several causes and may be age-related, present at birth, or formed as a result of trauma or exposure to a toxic substance, Cataracts are classified by the cause: Senile cataracts develop in elderly people Congenital cataracts occur in neonates from inborn errors of metabolism or frommaternal rubella infection during the first trimester Traumatic cataracts develop after a foreign body injures the lens with sufficient force toallow aqueous or vitreous humor to enter the lens capsule Complicated cataracts occur secondary to uveitis, glaucoma, retinitis pigmentosa, or retinal detachment Toxic cataracts result from drug or chemical toxicity with prednisone, ergot alkaloids,naphthalene, and phenothiazines.Genetic Considerations; Epidemiological studies indicate that cataracts have strong geneticcomponents. Several loci have been identified for an autosomal dominant form of cataracts.Congenital cataracts occur with galactosemia and these can appear within just a few days of birth. The specific genetic contributions of the more common age-associated cataracts are stillunclear. Ethnicity and race have no known effect on the risk of cataracts. Complications Complications may include retinal disorders, pupillary block, adhesions, acute glaucoma,macular edema, and retinal detachment. Following extracapsular cataract extraction, theposterior capsule may become opacified. This condition, called a
secondary membrane or after-cataract, occurs when subcapsular lens epithelial cells regenerate lens fibers, which obstructvision. After-cataract is treated by yttriumaluminum-garnet (YAG) laser treatment to theaffected tissue. Without surgery, a cataract eventually causes complete vision loss. Assessment Nursing Care Plans For Cataract Typically, the patient complains of painless, gradual vision loss. He may also report a blindingglare from headlights when he drives at night, poor reading vision, and an annoying glare andpoor vision in bright sunlight. If he has a central opacity, the patient may report seeing better indim light than in bright light, because this cataract is nuclear and, as the pupil dilates, the patientcan see around the opacity.Physical examination. Cataract formation causes blurred vision, a loss measured by Use of thesnellen chart. Color perception of blue, green, and purple is reported as varying Shades of gray.If the cataract is advanced, shining a penlight on the pupil reveals the white area Behind thepupil. A dark area in the normally homogeneous red reflex confirms the diagnosis. Treatment Surgical lens extraction Diagnoses that may occur in Nursing Care Plans For Cataract Anxiety eficient knowledge (diagnosis and treatment) disturbed sensory perception: Visual Risk for infection Risk for injury key outcomes Nursing Care Plans For Cataract patient and his family will voice their feelings and concerns. patient will verbalize understanding of the disease and treatment. patient will regain normal visual functioning. patient will show no signs or symptoms of infection. patient will avoid injury Body image; Safety behavior: Personal; Safety behavior: Fall prevention; Safetybehavior: Home physical environment; Anxiety control; Neurological status; Rest; Sleep interventions Nursing Care Plans For Cataract
Postoperatively, monitor the patient until he recovers from the effects of the anesthetic.Keep the side rails of the bed up, monitor vital signs, and assist him with earlyambulation.
Apply an eye shield or eye patch postoperatively as ordered
Communication enhancement: Visual deficit; Activity therapy; Cognitive stimulation;Environmental management; Fall prevention; Surveillance: Safety Nursing Care Plans For Cataract Home Health: Caution him to avoid activities that increase intraocular pressure, such as straining withcoughing, bowel movements, or lifting Clients fitted with cataract eyeglasses need information about altered spatial perception.The eyeglasses should be first used when the patient is seated, until the patient adjusts tothe distortion. Instruct the client to look through the center of the corrective lenses and toturn the head, rather than only the eyes, when looking to the side. Clear vision is possibleonly through the center of the lens. Hand-eye coordination movements must be practicedwith assistance and relearned because of the altered spatial perceptions. Teach the patient or family member how to instill ophthalmic ointment or drops. driving, sports, and machine operation can be resumed when permission is granted bythe eye surgeon. If the patient has increased eye discharge, sharp eye pain , or deterioration in vision,instruct him to immediately notify the physician.
I. Definition Cataract formation is a gradual, progressive opacity of the lens or lens capsule that leads to visual loss. II. Risk Factors Aging Trauma Drug or chemical toxicity
Genetic defects Secondary effects of other disease
III. Pathophysiology Altered nutrient metabolism within the lens triggers cataracts formation. The lens becomes cloudy and has reduced accommodative power. Light rays cannot pass through the opaque lens to the retina causing vision loss. IV. Assessment/Clinical Manifestations/Signs and Symptoms Progressively worsening blurred vision Cloudy-appearing lens No pain or eye redness
Laboratory and diagnostic study findings Ophthalmoscopic Slit-lamp examination
V. Medical Management There is no medical treatment for cataracts, although use of vitamins C and E and beta-carotene is being investigated. Glasses or contacts, bifocal or magnifying lenses may improve vision. Mydriatics can be used short term, but glare is increased. Surgical Management: Two surgical techniques are available: Intracapsular cataract extraction (ICCE) and extracapsular cataract extraction (ECCE) including phacoemulsification. Indications for surgery are loss of vision that interferes with normal activities or a cataract that is causing glaucoma. Cataracts are removed under local anesthesia on an outpatient basis. Lens replacement may involve aphakic eyeglasses, contact lens, and intraocular lens (IOL) implants. When both eyes have cataracts, one eye is surgically treated at a time. VI. Nursing Diagnosis Anxiety related to possible vision loss Disturbed sensory perception related to visual impairment Ineffective health maintenance related to knowledge deficit Risk for injury related to impaired vision Self-care deficit related to impaired vision
VII. Nursing Management Provide preoperative nursing care for extraction of the cataract, which may be extracapsular or intracapsular. Explain to the client that this surgery is usually done on an outpatient basis.
Discuss and administer preoperative medications, which may include IV sedation, adrenergic agonists, and hyperosmotic agents. Provide postoperative nursing care. Instruct the client to remain in a semi-Fowlers position or on the nonoperative side. Explain the importance of keeping a patch or protective shield on the affected eye. Promote measures to relieve postoperative discomfort with analgesics and atropine eye drops as prescribed. Instruct the client to report severe eye pain immediately, this may indicate increasing intraocular pressure or hemorrhage. Provide postoperative discharge teaching, which usually occurs a few hours after surgery. Inform the client that the surgeon will change the patch on the second postoperative day. Discuss the need for eye protection by instructing the client to wear glasses during daytime hours (sunglasses at first) and to use an eye shield at night to prevent eye rubbing. Tell the client to avoid straining, to lie on the back or unaffected side when i n bed, to read only in moderation and to maintain a sedentary lifestyle for 2 weeks. Instruct the client to turn his head to the side to scan the entire visual field to compensate for impaired peripheral vision. Instruct the client on how to administer steroid-antibiotic eye drops. Caution the client that the medication may initially cause sensitivity to bright light. Instruct the client to notify the health care provider if eye pain occurs after administration (i.e. possible indication of underlying glaucoma).
Anda mungkin juga menyukai
- CATARACTDokumen39 halamanCATARACTpullboy1Belum ada peringkat
- Diseases of LensDokumen42 halamanDiseases of LensAmmad ShahidBelum ada peringkat
- Extracapsular Cataract Extraction (OR)Dokumen4 halamanExtracapsular Cataract Extraction (OR)Jet-Jet GuillerganBelum ada peringkat
- CataractDokumen35 halamanCataractyusufharkianBelum ada peringkat
- Glaucoma A Symposium Presented at a Meeting of the Chicago Ophthalmological Society, November 17, 1913Dari EverandGlaucoma A Symposium Presented at a Meeting of the Chicago Ophthalmological Society, November 17, 1913Belum ada peringkat
- The Skeffington Perspective of the Behavioral Model of Optometric Data Analysis and Vision CareDari EverandThe Skeffington Perspective of the Behavioral Model of Optometric Data Analysis and Vision CareBelum ada peringkat
- ENUCLEATIONDokumen14 halamanENUCLEATIONBlessy SebastianBelum ada peringkat
- Eye Disorder in Childhood & Adolescent: Lia Meuthia Zaini FK Unsyiah / RSUZADokumen54 halamanEye Disorder in Childhood & Adolescent: Lia Meuthia Zaini FK Unsyiah / RSUZACut MulianiBelum ada peringkat
- Neuro-Ophta EditedDokumen97 halamanNeuro-Ophta EditedMarshet GeteBelum ada peringkat
- The Pathophysiology and Treatment of Glaucoma PDFDokumen22 halamanThe Pathophysiology and Treatment of Glaucoma PDFNurul Dwi LestariBelum ada peringkat
- A Child Presenting With Visual Impairment 28/4/2020Dokumen40 halamanA Child Presenting With Visual Impairment 28/4/2020Sindhu BabuBelum ada peringkat
- Myopia by NamanDokumen19 halamanMyopia by NamanAkshit ChitkaraBelum ada peringkat
- TrabeculectomyDokumen28 halamanTrabeculectomyAlfu RafdiBelum ada peringkat
- Superior Oblik PalsyDokumen13 halamanSuperior Oblik PalsyYunita ManurungBelum ada peringkat
- Lowe Syndrome (Oculocerebrorenal syndrome) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandLowe Syndrome (Oculocerebrorenal syndrome) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- Retinal Vein Occlusion Concept MapDokumen2 halamanRetinal Vein Occlusion Concept MapJoe RealBelum ada peringkat
- AstigmatismDokumen1 halamanAstigmatismAmmellya PutriBelum ada peringkat
- Childhood BlindnessDokumen14 halamanChildhood BlindnessAditya Arya PutraBelum ada peringkat
- Glaucoma and CataractDokumen30 halamanGlaucoma and CataractJayselle ArvieBelum ada peringkat
- AmblyopiaDokumen33 halamanAmblyopiaSujon PaulBelum ada peringkat
- AION Anterior Ischemic Optic Neuropathy AIONDokumen22 halamanAION Anterior Ischemic Optic Neuropathy AIONNyak Rahmat100% (1)
- PterygiumDokumen3 halamanPterygiumtri_budi_20Belum ada peringkat
- CATARACTS and GLAUCOMADokumen11 halamanCATARACTS and GLAUCOMAAmoroso, Marian Corneth D.Belum ada peringkat
- Surgical Management of Senile CataractDokumen39 halamanSurgical Management of Senile CataractKarthik ChellaBelum ada peringkat
- Cardiac Case StudyDokumen3 halamanCardiac Case Studydsaitta108Belum ada peringkat
- Primary Angle Closure GlaucomaDokumen39 halamanPrimary Angle Closure GlaucomaMaria ShafiqBelum ada peringkat
- Cataract: By: Charmagne MaranonDokumen28 halamanCataract: By: Charmagne MaranonCham'cham Araneta MarañonBelum ada peringkat
- Hyphema 2Dokumen7 halamanHyphema 2heidyBelum ada peringkat
- Short Case 1 PterygiumDokumen15 halamanShort Case 1 PterygiumAnmol KhadkaBelum ada peringkat
- Retinal Drawing A Lost Art of MedicineDokumen3 halamanRetinal Drawing A Lost Art of MedicinekavyaBelum ada peringkat
- Glaucoma ChapterDokumen32 halamanGlaucoma ChapterAhmed Omara100% (5)
- School Eye Screening and The National Program For Control of Blindness - 2Dokumen6 halamanSchool Eye Screening and The National Program For Control of Blindness - 2rendyjiwonoBelum ada peringkat
- Diseases of Lens DR D.JLDokumen113 halamanDiseases of Lens DR D.JLNithya GunasekaranBelum ada peringkat
- What Is The Difference Between Emmetrope and Presbyopia EyesDokumen8 halamanWhat Is The Difference Between Emmetrope and Presbyopia EyesNazraana AbdulBelum ada peringkat
- Childhood Cataract A Socio-Clinical Study at A Public Sector Tertiary Eye Care Centre in IndiaDokumen7 halamanChildhood Cataract A Socio-Clinical Study at A Public Sector Tertiary Eye Care Centre in IndiaInternational Journal of Innovative Science and Research TechnologyBelum ada peringkat
- Lens and CataractDokumen55 halamanLens and CataractRold Brio Sos100% (1)
- Introduction To Low VisionDokumen15 halamanIntroduction To Low VisionHira AtifBelum ada peringkat
- By: Noor Majeed RehaniDokumen23 halamanBy: Noor Majeed RehaniMihaela Toma0% (1)
- HyperopiaDokumen6 halamanHyperopiaTesfsh MekonenBelum ada peringkat
- NYCTALOPIADokumen16 halamanNYCTALOPIAAroob YaseenBelum ada peringkat
- Eyelid Lumps and BumpsDokumen43 halamanEyelid Lumps and BumpsAbdul HannanBelum ada peringkat
- Alport Syndrome A ReviewDokumen12 halamanAlport Syndrome A ReviewRodrigoBarreraBelum ada peringkat
- Asking Your Question (PICO) - NursingDokumen5 halamanAsking Your Question (PICO) - NursingBentaigaBelum ada peringkat
- CataractDokumen7 halamanCataractNader Smadi100% (2)
- 02 Preoperative Assessment of A Patient With Cataract-FinalDokumen10 halaman02 Preoperative Assessment of A Patient With Cataract-Finalmdshahidalam315Belum ada peringkat
- Eye Lid DiseasDokumen59 halamanEye Lid DiseasJohanna Tania PriatoBelum ada peringkat
- APHAKIADokumen20 halamanAPHAKIAAmitabh SatsangiBelum ada peringkat
- College of Medicine and Health Science, Department of OptometryDokumen47 halamanCollege of Medicine and Health Science, Department of Optometryhenok birukBelum ada peringkat
- Congenital Disorders of The CorneaDokumen100 halamanCongenital Disorders of The Corneaeyemd_in_trainingBelum ada peringkat
- The Dry EyeDokumen8 halamanThe Dry EyeMohit BooraBelum ada peringkat
- Glaucoma LectureDokumen166 halamanGlaucoma LectureSonali Gupta100% (1)
- HemophiliaDokumen4 halamanHemophiliaMechelle ChenBelum ada peringkat
- Angle Closure Glaucoma - Current ConceptsDokumen77 halamanAngle Closure Glaucoma - Current Conceptsapi-3742497100% (3)
- Fungal KeratitisDokumen34 halamanFungal KeratitisbhartiBelum ada peringkat
- 42fundus AngiographyDokumen28 halaman42fundus AngiographyHitesh SharmaBelum ada peringkat
- AOA ConjunctivitisDokumen33 halamanAOA ConjunctivitiseloooyiyBelum ada peringkat
- Anophthalmia and MicrophthalmiaDokumen8 halamanAnophthalmia and MicrophthalmiaLjubomirErdoglijaBelum ada peringkat
- Blindness: Prof. Dr. DudaniDokumen13 halamanBlindness: Prof. Dr. DudaniRabin BaniyaBelum ada peringkat
- Ptosis Types & Clinical Features: Made By:-Amritansh PandeyDokumen14 halamanPtosis Types & Clinical Features: Made By:-Amritansh PandeyalexBelum ada peringkat
- What Causes Cataract?Dokumen3 halamanWhat Causes Cataract?Eye spacialistBelum ada peringkat
- What? I Can't Believe My Eyes! Caren McCarter/Lynne Smith-MillsDokumen47 halamanWhat? I Can't Believe My Eyes! Caren McCarter/Lynne Smith-MillsCaren McCarterBelum ada peringkat
- Trataka Intelligence MemoryDokumen3 halamanTrataka Intelligence MemorySreeraj Guruvayoor S100% (1)
- Macular Function Test: Dr. PushpanjaliDokumen53 halamanMacular Function Test: Dr. Pushpanjalipushpanjali ramteke83% (6)
- Lens Types Advantages DisadvantagesDokumen2 halamanLens Types Advantages DisadvantagesnasikaceliaBelum ada peringkat
- EcceDokumen2 halamanEcceGeneva Amandy RoxasBelum ada peringkat
- BCQ Seq Paper A Ophthalmology 2015Dokumen7 halamanBCQ Seq Paper A Ophthalmology 2015Hira Panhwer0% (1)
- KeratoconusDokumen10 halamanKeratoconusbijujcBelum ada peringkat
- Example10 enDokumen20 halamanExample10 enapi-279889431Belum ada peringkat
- Opening The Third EyeDokumen4 halamanOpening The Third Eyetower1Belum ada peringkat
- 29 Days Study Plan and Important Stuff by Hafiz Bilal For 4TH Year MBBS PDFDokumen3 halaman29 Days Study Plan and Important Stuff by Hafiz Bilal For 4TH Year MBBS PDFDaneyal Arshad100% (2)
- Job ResumeDokumen2 halamanJob ResumeSyahru RamadhanBelum ada peringkat
- Ilyas S, Yulianti SR. Ilmu Penyakit Mata Edisi Ke Empat. Jakarta: FKUI Press 2012Dokumen3 halamanIlyas S, Yulianti SR. Ilmu Penyakit Mata Edisi Ke Empat. Jakarta: FKUI Press 2012Tompasobaru DuaBelum ada peringkat
- Lens Luxation in DogsDokumen4 halamanLens Luxation in DogsBernadhete Gaudia SabiroseBelum ada peringkat
- Lid Wiper EpitheliopathyDokumen35 halamanLid Wiper EpitheliopathyDavid VásquezBelum ada peringkat
- A Randomised, Prospective Study To Investigate The Efficacy of Riboflavinultraviolet A 370 NM Coroneal Collagen Cross Linkage To Halt The Progression of KeratoconusDokumen7 halamanA Randomised, Prospective Study To Investigate The Efficacy of Riboflavinultraviolet A 370 NM Coroneal Collagen Cross Linkage To Halt The Progression of Keratoconusurs lovinglyBelum ada peringkat
- CHAPTER 3 - SensationDokumen59 halamanCHAPTER 3 - Sensationflammy07100% (1)
- Lasik FlowChartDokumen2 halamanLasik FlowChartKae Parilla100% (1)
- Ophthalmic Exam UpennDokumen9 halamanOphthalmic Exam UpennlechamariaBelum ada peringkat
- ProP - Differentiating Nuclear Sclerosis From CataractsDokumen6 halamanProP - Differentiating Nuclear Sclerosis From CataractsDita TaepangBelum ada peringkat
- Fundamentals of Clinical Ophtalmology - Cataract Surgery (PDFDrive)Dokumen233 halamanFundamentals of Clinical Ophtalmology - Cataract Surgery (PDFDrive)Eka WahyuBelum ada peringkat
- Wrodzone Wady Gałki Ocznej U Dzieci - Obserwacje Własne Cases of Congenital Eye Malformations in ChildrenDokumen9 halamanWrodzone Wady Gałki Ocznej U Dzieci - Obserwacje Własne Cases of Congenital Eye Malformations in ChildrenAntek MulaBelum ada peringkat
- Lens-Induced Glaucoma: Diagnosis and Management ofDokumen4 halamanLens-Induced Glaucoma: Diagnosis and Management ofasfwegereBelum ada peringkat
- Clínica Oftalmológica Del Caribe (COFCA) ColombiaDokumen11 halamanClínica Oftalmológica Del Caribe (COFCA) ColombiaJulio Martinez-ClarkBelum ada peringkat
- Human Eye Lesson 1Dokumen5 halamanHuman Eye Lesson 1Nicketa AndersonBelum ada peringkat
- Biology Notes For O LevelDokumen36 halamanBiology Notes For O LevelemmaBelum ada peringkat
- Gold Exp B2 U6 Lang Test A PDFDokumen2 halamanGold Exp B2 U6 Lang Test A PDFPmp Practice Makes Perfect75% (4)
- Glaucoma: DefinitionDokumen5 halamanGlaucoma: DefinitionDani PhilipBelum ada peringkat
- Exercises To Help Keep The Eyes HealthyDokumen8 halamanExercises To Help Keep The Eyes Healthymuthu189100% (9)
- Ophtha - Eor and LensDokumen86 halamanOphtha - Eor and Lensapi-3856051Belum ada peringkat
- Lecture Three Convergence and Accommodation (AC/A) : Mr. Natnael L. (Lecturer) April/2017Dokumen33 halamanLecture Three Convergence and Accommodation (AC/A) : Mr. Natnael L. (Lecturer) April/2017henok birukBelum ada peringkat