Cataract Morphology: Dip HE Rehabilitation Work (Visual Impairment)
Diunggah oleh
blinkbumbumDeskripsi Asli:
Judul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Cataract Morphology: Dip HE Rehabilitation Work (Visual Impairment)
Diunggah oleh
blinkbumbumHak Cipta:
Format Tersedia
UCE Birmingham Faculty of Health
Dip HE Rehabilitation Work (Visual impairment)
Cataract morphology
By Konrad Pesudovs and David B Elliott
Contents
Abstract Introduction Cataract morphology Cortical cataracts Nuclear cataracts Posterior subcapsular cataract Clinical cataract classification schema Assessment of vision in the cataract patient Deciding on the need for surgery Acknowledgments
Abstract
Cataract is the most common condition requiring assessment and referral from optometric practice. This article examines the features of the main morphological types of age-related cataract: nuclear cortical and posterior subcapsular. The steps to take in the assessment and management of cataract patients are discussed including: examination for cataract, visual assessment methods to confirm whether vision loss is present, discussion with the patient to establish if visual disability is present, and establishing criteria for referral. Keywords Cataract, disability, morphology, referral vision.
Introduction
Cataract is a frequent condition found in patients attending an optometric practice and, given the demographic changes within the population, their numbers will increase in the coming years. This article discusses the optometric assessment and management of age-related cataract. The scope includes the categorisation of cataract morphology, the assessment of vision, the assessment of visual disability, and how to determine when to refer a patient for surgery.
Copyright UCE Birmingham 64029999.doc
Visit us at www.sightlossmatters.com
Document revised 28 Sep 06
UCE Birmingham Faculty of Health
Dip HE Rehabilitation Work (Visual impairment)
Cataract morphology
Cataract increases substantially with age. Cataract causing a visual acuity (VA) of worse than 6/9 has a prevalence of approximately 5% in the 55-64 age group and over 40% in the over 75s1. There are three main types of age-related cataract: cortical, nuclear and posterior subcapsular. In the UK, cortical cataract is the most prevalent (63%), followed by nuclear (41%) and posterior subcapsular cataract (24%)2. Around 30% of eyes have mixed cataract, i.e. more than one morphological type.
Cortical cataracts
Cortical cataracts are cuneiform or wedge shaped opacities found in the anterior and/or posterior lens cortex. The base of the wedge or spoke is in the periphery of the lens, so that the cataract is often hidden behind the iris. Cortical cataracts are most often found in the inferionasal part of the lens, which may implicate ultra-violet radiation involvement in their aetiology3. Cortical opacities are often associated with water clefts, which are optically clear wedges that can be seen with slit-lamp biomicroscopy. This association gives a clue as to the pathology of cortical cataract, which is fundamentally due to water imbibition into the lens leading to disruption of the regular order of lens fibres4. The disrupted, displaced and swollen lens fibres dissolve and precipitation of components leads to an opaque suspension within the lens. These structural changes create light scattering centres with a considerable variation in refractive index. Opacification is due to the scattering of light when it meets irregular interfaces between regions of differing refractive index. The visibility of cortical cataracts at the slit-lamp results from gross backscatter (i.e. towards the observing clinician), however, forward scatter (i.e. towards the retina) also occurs and this is responsible for the degradation of vision. It is important to note that backscatter and forward scatter are not necessarily highly correlated5, thus a cortical spoke which is highly visible at the slit-lamp may not necessarily be causing a decrease in the patients vision. In addition, vision is only affected if the cortical spokes enter the pupillary area. Cortical cataracts can cause astigmatic changes and monocular diplopia (Table 1). Table 1. Cortical cataract clinical pearls Cortical cataract Prevalence (UK) Description Risk factors
Copyright UCE Birmingham 64029999.doc
~63% of all cataracts (including mixed cataract) Wedge-shaped opacity in the lens cortex with the base in the lens periphery, see Figure 1a. Age, ultra-violet light, female gender Page 2 of 9
UCE Birmingham Faculty of Health
Dip HE Rehabilitation Work (Visual impairment)
Refractive changes Idiosyncratic symptoms/signs
Possible astigmatic changes. Monocular diplopia, sometimes asymptomatic despite obvious cataract on slit-lamp examination.
Tints for disability glare No, patients with these cataracts see worse with a (vision loss with glare) larger pupil
Nuclear cataracts
Nuclear cataract presents as a homogeneous increase in light scatter and absorption in the lens nucleus (Figure 1B), and can be associated with increased yellowing or brunescence of the lens. Vision loss is due to both light scatter and absorption. The pathology of the opacity is fundamentally an increase in molecular size through a cross-linking of proteins within and between cells in the lens nucleus6. This change results in an increase in optical density (and a decrease in transparency) by large molecules that absorb light and cause some light scatter. The increased yellowing and brunescence of some nuclear cataracts is indicative of wavelength-dependent light absorption by lens proteins. Nuclear cataracts can produce a marked myopic shift2, which is known as index myopia. Indeed a -0.50DS shift over two years in an elderly patient is highly indicative of developing nuclear cataract2. The average shift over 4 years is -1.50DS, giving a rate between -0.25 and -0.50DS per year. Obviously some shifts can be much larger than this. Large myopic shifts can become the basis for referral (Table 2).
Copyright UCE Birmingham 64029999.doc
Page 3 of 9
UCE Birmingham Faculty of Health
Dip HE Rehabilitation Work (Visual impairment)
Table 2. Nuclear cataract clinical pearls Prevalence (UK) Description Risk factors ~41% of all cataracts (including mixed cataract) Homogeneous increase in light scatter in lens nucleus. Blue wavelength absorption also leads to increased yellowing, see Figure 1b. Age, smoking, low levels of anti-oxidant vitamins.
Refractive changes Myopic shift Idiosyncratic symptoms/signs Tints for blue disability glare (vision loss with glare) Colour vision changes (blue-yellow confusion) These patients already have a built-in blue disability absorbing tint
Posterior subcapsular cataract
Posterior subcapsular (PSC) cataract presents centrally, at the back of the lens just in front of the posterior capsule (Figure 1C). These opacities are epithelial cells that migrate aberrantly to the posterior pole of the lens7. The migratory cells which cluster around the posterior pole interdigitate with adjacent lens fibres leading to breakdown and liquefaction of the posterior cortex with formation of globules8. The posteriorly migrating epithelium coalesce into larger "bladder cells"9. These cells and globules form large, well spaced, discrete light scattering centres. The size and spacing of the particles causes a great deal of forward scatter with comparatively little backscatter, making the opacities difficult to view at the slit-lamp yet very visually debilitating. PSC cataracts also cause a dramatic reduction in vision because they are generally centrally positioned within the pupillary area. These opacities can also present earlier than the other morphological types, at about age 55 years. PSC cataracts can be associated with other ocular and systemic diseases, such as retinitis pigmentosa and diabetes8 and are found as a side effect of systemic drugs such as oral corticosteroids10. These are the most visually disabling cataracts, and may be missed with a direct ophthalmoscope because they can be hidden behind the Purkinje images (Table 3).
Copyright UCE Birmingham 64029999.doc
Page 4 of 9
UCE Birmingham Faculty of Health
Dip HE Rehabilitation Work (Visual impairment)
Table 3. Posterior subcapsular cataract clinical pearls Prevalence (UK) Description Risk factors Refractive changes Idiosyncratic symptoms/signs ~24% of all cataracts (including mixed cataract) Circular opacities in the centre of the pupil just in front of the posterior capsule, see figure 1c. Age, smoking, diabetes, steroid use, trauma None reported Can be very visually debilitating, especially under glare, near VA worse than distance VA, can be difficult to spot with direct ophthalmoscopy, occur in younger age groups.
Tints for disability glare Yes, patients with small, central PSC see disability (vision loss with glare) better with a larger pupil.
Clinical cataract classification schema
These systems basically involve classifying the cataract morphology and grading features of the cataract seen at the slit-lamp by comparing them with standard diagrams and/or photographs. Valid systems for the classification of cataract are useful for epidemiological studies, anticataract drug trials, clinical trials where generation of cataract may be a risk, or in clinical studies where cataract severity is compared to other measures. Most importantly, cataract classification can be used in the clinical setting to provide a quantitative record of cataract severity. Numerous schemes exist for the classification of cataract11-25. Almost all are for age-related cataract and independently classify the three morphological types: nuclear, cortical and PSC. Most systems are designed for slit-lamp based assessment where grading is by comparison with standard diagrams, with the alternatives of microscopic or photographic grading. The nature and complexity of the scaling varies markedly between systems26,27. Two of the most popular schema are The Oxford Clinical Cataract Classification and Grading System and the Lens Opacities Classification System III (LOCS III). Sparrow et al developed the Oxford Clinical Cataract Classification and Grading System14. This technique, which has found wide acceptance and has been used in many clinical trials28, is a slit-lamp-based system in which cataract features are classified morphologically. This carefully designed system has the merit of equal interval steps between the grades14. The LOCS III22 evolved following experiences with 2 earlier versions15,17,22,29. LOCS III grades cataract in four dimensions: nuclear
Copyright UCE Birmingham 64029999.doc
Page 5 of 9
UCE Birmingham Faculty of Health
Dip HE Rehabilitation Work (Visual impairment)
colour (NC) nuclear opalescence (NO) cortical opacity (C) PSC (P) (Figure 2). Nuclear opalescence and colour are rated on a decimal scale from 0 to 7 in steps of 0.1 and cortical and PSC are rated on a decimal scale from 0 to 6. This is a thoroughly validated system which has been used extensively for clinical trials29-32. Alternatively, cataracts can be classified and approximately graded without these systems. The conventional 0 to 4 grading system can be used, where 0 is a clear lens, + or 1+ represents a mild cataract, ++ or 2+ a moderate cataract, +++ or 3+ a marked cataract and ++++ or 4+ a severe cataract. Alternatively, PSC and cortical cataract can be graded by the percentage of the (dilated or otherwise) pupillary area they occupy or by a brief sketch.
Assessment of vision in the cataract patient
There are many ways in which vision is affected by cataract, including increasing myopia and astigmatism, monocular diplopia, reduced light transmission and changes in colour perception33. However, visual loss in cataract is principally due to increased intraocular light scatter. Light from the object itself is scattered, reducing the contrast of its retinal image. In addition, wide-angle light scatter from peripheral glare sources can produce a veiling luminance on the retina, further reducing the contrast of the retinal image. Not surprisingly, visual decrement is greatest in glare or bright light conditions (notes on prescribing tints and coatings for cataract patients are found in Table 4). Table 4. Spectacle tints and coatings for use in the cataract patient Tints for Tints can be useful to alleviate discomfort. discomfort glare In general tints provide no benefit as the effect of the Tints for reduction in glare light is balanced by the reduction of light disability glare from the object of regard. In general, broad- brimmed hats (vision loss with are better. Some patients with small, central PSC cataract glare) may benefit from a tint due to its effect on pupil size (see Table 3) UV-blocking tints AR lens coatings These can alleviate some disability glare from fluorescence within the lens and perhaps slow cataract progression, particularly of cortical cataract. These may be useful for patients with cataract, especially those who drive at night or use a VDU.
Copyright UCE Birmingham 64029999.doc
Page 6 of 9
UCE Birmingham Faculty of Health
Dip HE Rehabilitation Work (Visual impairment)
It is well established that some patients with cataract, who retain good VA, have significant visual problems. In these cases contrast sensitivity and glare testing can be used to evaluate the level of disability.
Contrast Sensitivity
Contrast sensitivity at low to intermediate spatial frequencies can be reduced in patients with cataract when VA is good34,35. In these cases cataract surgery can return contrast sensitivity to age-matched normal values35. Additionally, in cataract patients, contrast sensitivity can be a better indicator of various aspects of real world vision than VA, such as driving, orientation, mobility and face expression recognition35-37. The best available test for use in cataract patients is the Pelli-Robson chart (Figure 3). At the recommended working distance of 1m, the letters are equivalent to 6/273 Snellen, and the chart gives an indication of contrast sensitivity at a spatial frequency of approximately 0.5 to 2 c/deg (just below the peak of the contrast sensitivity curve). In many cataract patients, Pelli-Robson contrast sensitivity will be normal (1.50 log contrast sensitivity or above). Any patient with a log contrast sensitivity of 1.35 or below, is likely to be complaining of poor vision, no matter how good the VA is. Poor contrast sensitivity is more likely with nuclear and PSC cataracts38-42.
Glare testing
Increased forward light scatter causes cataract patients to see poorly in bright light or glare conditions. Consider the effect of a dirty windscreen on your vision when driving. Vision is satisfactory until sunlight or light coming from car headlights hits the screen, when vision can be reduced dramatically. Similarly, with some cataract patients, VA can be adequate in the relatively low illumination conditions of the examination room, but considerably reduced when outdoors or when driving at night (Panel 1). Panel 1. Typical PSC and glare case report52. A healthy 45-year-old prison guard complained of a gradual decrease in vision over the previous year. This decrease only occurred in bright sunlight, such as when guarding prisoners working outside. Before his visit, his loss of vision had been so great as to allow two convicts to escape! His VA was measured to be 6/6 in both eyes in the examination room. However, VA measured in bright light levels was 6/120! Slit-lamp examination with a dilated pupil revealed small PSC cataracts. The case history in (see Panel 1) highlights that a patient attending for an examination in the UK in the winter with no symptoms and a VA of 6/9 or
Copyright UCE Birmingham 64029999.doc
Page 7 of 9
UCE Birmingham Faculty of Health
Dip HE Rehabilitation Work (Visual impairment)
better, could have profoundly reduced vision in a sunny environment Any suggestion of small PSC cataracts should immediately indicate glare testing and pupillary dilation with a careful slit-lamp examination. Glare tests measure the reduction in a patient's vision due to a glare source (glare loss), and indicate the effect on vision of increased light scatter and a smaller pupil. Glare test scores have been shown to correlate with VA measured outdoors and to correlate better with glare symptoms than conventionally measured VA in patients with cataract43,44. Simple methods of measuring disability glare involve measuring VA under glare conditions, such as while directing a bright penlight or ophthalmoscope light into the patient's eye45. Due to the inverse square law and light scatter varying as a function of the square of the glare angle (the angle of the glare source to the visual axis), it is very important to standardise the angle and distance of the penlight to the eye. Typical standards are 10cm and 30 degrees. A more standardised version of such tests is the Brightness Acuity Tester. Disability glare scores are usually taken as the level of VA under the glare condition. Alternatively, the impact of glare can be recorded as glare loss i.e. the number of lines on the chart lost when the glare source is introduced. Testing can be done using conventional VA, low contrast VA or contrast sensitivity charts.
Assessment of disability in the cataract patient
The decision of when to refer a patient for cataract surgery should be primarily dependent on whether the patients reduced vision interferes with their desired lifestyle. Referral should NOT be based on VA measurements alone. For example, if a patient is a taxi driver and cataract is reducing his vision so that he cannot see well enough to drive at night or on sunny days, he should be referred for surgery. Conversely, if a patient is perfectly happy with their vision and has no restrictions on their lifestyle, despite having 6/18 or even 6/24 VA, there is no need to refer for surgery, although you may discuss the possibility of future referral with them46. Therefore, it is important to determine whether the patients desired lifestyle is affected by their reduced vision. When cataract is identified, it is useful to ask some specific questions which relate to cataract-induced visual loss. For example, "Do you have any problem with glare or in bright sunlight?" and if pertinent "Do you have any problems driving at night?, or on sunny days?". In addition, ask about the effect of vision on the patient's job, sports or hobbies. There are formal instruments (questionnaires) for the measurement of visual disability caused by cataract such as the VF-14 and the VDA47,48. While these questionnaires may not be appropriate for routine use in optometric practice, they do contain questions which the optometrist may find helpful to ask.
Copyright UCE Birmingham 64029999.doc
Page 8 of 9
UCE Birmingham Faculty of Health
Dip HE Rehabilitation Work (Visual impairment)
Deciding on the need for surgery
The nexus between vision, disability and cataract grading The referral of patients with cataract for surgery must be based on whether the patients reduced vision is interfering with their desired lifestyle. Referral is then justified using clinical vision tests such as distance and near visual acuity, contrast sensitivity, disability glare and for monocular pseudophakes, anisometropia and stereopsis. The presence of co-morbid eye disease (including amblyopia) needs careful assessment to determine whether or not the cataract is the major cause of the visual loss. An apportionment of the visual loss and the visual disability to each condition using potential vision tests49-51 and clinical acumen should be made. This last quality is the most difficult to teach, but in simple terms it involves an assessment of whether the level of vision, severity of cataract and degree of symptoms seem in balance. Finally, a discussion of the risk and benefits of cataract surgery as well as the costs and inconvenience is important, and this should follow the line of an informed consent discussion, similar to that which the patient will encounter when they meet the cataract surgeon. (Figure 5).
Acknowledgments
Konrad Pesudovs is supported by an Australian National Health and Medical Research Council (NHMRC) Sir Neil Hamilton Fairley Research Fellowship. Konrad Pesudovs BScOptom, PhD, MCOptom, FVCO, FAAO Bradford University and Flinders University (Australia) and David B Elliott PhD, MCOptom, FAAO Bradford University Correspondence: Dr. Konrad Pesudovs Department of Optometry University of Bradford Bradford West Yorkshire BD7 1DP, UK E-mail: K.Pesudovs@bradford.ac.uk You have reached the end of this text
Copyright UCE Birmingham 64029999.doc
Page 9 of 9
Anda mungkin juga menyukai
- Cataract Surgery: A Brief History and OverviewDokumen15 halamanCataract Surgery: A Brief History and OverviewwhiezardBelum ada peringkat
- Senile Cataract (Age-Related Cataract) - Practice Essentials, Background, PathophysiologyDokumen5 halamanSenile Cataract (Age-Related Cataract) - Practice Essentials, Background, PathophysiologyAhmad FahroziBelum ada peringkat
- Senile Cataract (Age-Related Cataract) : Practice Essentials, Background, PathophysiologyDokumen6 halamanSenile Cataract (Age-Related Cataract) : Practice Essentials, Background, PathophysiologyadliahghaisaniBelum ada peringkat
- Senile Cataract Clinical Presentation and CausesDokumen4 halamanSenile Cataract Clinical Presentation and CausesAhmad FahroziBelum ada peringkat
- Senile Cataract Clinical Presentation and CausesDokumen4 halamanSenile Cataract Clinical Presentation and CausesAhmad Fahrozi100% (1)
- Cataract For Medical StudentsDokumen7 halamanCataract For Medical StudentsJustin Michal DassBelum ada peringkat
- CataractDokumen5 halamanCataractcarls burg a. resurreccionBelum ada peringkat
- Cataract. Slit Lamp Photograph Cataract. Slit Lamp Photograph FollowingDokumen6 halamanCataract. Slit Lamp Photograph Cataract. Slit Lamp Photograph Followingekin_shashaBelum ada peringkat
- My SeminarDokumen12 halamanMy SeminarAdeleye SeunBelum ada peringkat
- Cataract LectureDokumen22 halamanCataract Lecturenashadmohammed99Belum ada peringkat
- Cet 5Dokumen4 halamanCet 5jumi26Belum ada peringkat
- Reviews in Clinical GerontologyDokumen18 halamanReviews in Clinical GerontologyRADYA PUTRA PRATAMABelum ada peringkat
- Cataract - Ophthalmology - FastbleepDokumen9 halamanCataract - Ophthalmology - FastbleepFaiq Syukri Bin SaparudinBelum ada peringkat
- Cataract For Medical StudentsDokumen6 halamanCataract For Medical Studentsopt.atiyehmhnBelum ada peringkat
- Aging-Related Cataracts: General FeaturesDokumen19 halamanAging-Related Cataracts: General FeaturespatriciamaisBelum ada peringkat
- Oxidative Damage and The Prevention ofDokumen11 halamanOxidative Damage and The Prevention ofFernando NugrohoBelum ada peringkat
- Learn About CataractsDokumen41 halamanLearn About CataractsRizkyAgustriaBelum ada peringkat
- Childhood Cataracts and Other JadiDokumen49 halamanChildhood Cataracts and Other JadiSania NadianisaBelum ada peringkat
- Cataract: Sarah Jane B. Aca-Ac BSN-3 Page 1770-1773Dokumen13 halamanCataract: Sarah Jane B. Aca-Ac BSN-3 Page 1770-1773De Sesto Rhys CarloBelum ada peringkat
- Cataracts Seminar: Causes, Treatment, and Future OutlookDokumen13 halamanCataracts Seminar: Causes, Treatment, and Future OutlookMacarena AlvarezBelum ada peringkat
- Biology Invesigatory Project: Group MembersDokumen13 halamanBiology Invesigatory Project: Group MembersNavaneeth KrishnanBelum ada peringkat
- Mature CataractDokumen24 halamanMature CataractmethadamayBelum ada peringkat
- Cataract, Senile: Author: Vicente Victor D Ocampo JR, MD, Head, Uveitis and Ocular ImmunologyDokumen7 halamanCataract, Senile: Author: Vicente Victor D Ocampo JR, MD, Head, Uveitis and Ocular ImmunologyDicki Pratama HolmesBelum ada peringkat
- CataractDokumen10 halamanCataractPrakash DeubaBelum ada peringkat
- Clinical and Experimental Advances in Congenital and Paediatric CataractsDokumen16 halamanClinical and Experimental Advances in Congenital and Paediatric CataractsFitri Amelia RizkiBelum ada peringkat
- Extracapsular Cataract Extraction (ECCE) Is A Category of Eye Surgery in WhichDokumen13 halamanExtracapsular Cataract Extraction (ECCE) Is A Category of Eye Surgery in WhichMa Christina RabayaBelum ada peringkat
- Catarata Relacionado Con LaedadDokumen11 halamanCatarata Relacionado Con LaedadMarcos Fernando Piñas CanchanyaBelum ada peringkat
- Cataract NotesDokumen4 halamanCataract NotesJeremy LauBelum ada peringkat
- Keratoconus: Picture 1Dokumen6 halamanKeratoconus: Picture 1BuiyiWongBelum ada peringkat
- Keratoconus: Picture 1Dokumen6 halamanKeratoconus: Picture 1BuiyiWongBelum ada peringkat
- CataractsDokumen72 halamanCataractsKusum RoyBelum ada peringkat
- CATARACTDokumen25 halamanCATARACTDea NabilaBelum ada peringkat
- Traumatic Cataracts: Causes and Presentations of Blunt and Penetrating Ocular InjuriesDokumen3 halamanTraumatic Cataracts: Causes and Presentations of Blunt and Penetrating Ocular InjuriesGrandy TalanilaBelum ada peringkat
- Lens DiseaseDokumen80 halamanLens Disease39 Akshit SetiaBelum ada peringkat
- Eye InjuryDokumen69 halamanEye InjurymalathiBelum ada peringkat
- Low Vision Manuscript Group 7Dokumen13 halamanLow Vision Manuscript Group 7Jay JimenBelum ada peringkat
- Nurses Role in The Early Detection of CataractsDokumen8 halamanNurses Role in The Early Detection of Cataractsintan juitaBelum ada peringkat
- ASKEP KATARAK m.2Dokumen24 halamanASKEP KATARAK m.2Given MalelakBelum ada peringkat
- Age-Related Cataract & GlaucomaDokumen26 halamanAge-Related Cataract & Glaucomasweetyeyal2002Belum ada peringkat
- Vitreous Floater1Dokumen7 halamanVitreous Floater1mithaa octoviagnesBelum ada peringkat
- Pemicu 1 Pengindraan c2Dokumen113 halamanPemicu 1 Pengindraan c2CcBelum ada peringkat
- 14th Lecture CataractDokumen3 halaman14th Lecture CataractMuhammad KhalilBelum ada peringkat
- Pemicu 1 PENGINDRAAN C2Dokumen113 halamanPemicu 1 PENGINDRAAN C2CcBelum ada peringkat
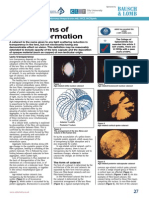
- Mechanisms of Cataract Formation: Nicholas Phelps Brown MD, FRCS, FrcophthDokumen7 halamanMechanisms of Cataract Formation: Nicholas Phelps Brown MD, FRCS, FrcophthQomariah RiaBelum ada peringkat
- Vitreous Floaters: Publication DetailsDokumen6 halamanVitreous Floaters: Publication Detailsmithaa octoviagnesBelum ada peringkat
- Article Wjpps 1533027420Dokumen25 halamanArticle Wjpps 1533027420rahayuBelum ada peringkat
- Classification of CataractsDokumen8 halamanClassification of CataractsAbdelrahman M. AlnweiriBelum ada peringkat
- Juvenile CataractDokumen12 halamanJuvenile CataractSofea Mustaffa100% (1)
- Yanoff DukerDokumen8 halamanYanoff DukerFerdinando BaehaBelum ada peringkat
- CataractDokumen63 halamanCataractMutti KakarBelum ada peringkat
- Сataract 09Dokumen32 halamanСataract 09somebody_maBelum ada peringkat
- CataractDokumen35 halamanCataractyusufharkianBelum ada peringkat
- Diseases of LensDokumen42 halamanDiseases of LensAmmad ShahidBelum ada peringkat
- ABSTRAC1Dokumen38 halamanABSTRAC1Rahid KhanBelum ada peringkat
- Final TouchDokumen49 halamanFinal TouchmalathiBelum ada peringkat
- Myopic Degeneration - Myopic CrescentsDokumen3 halamanMyopic Degeneration - Myopic CrescentsFerdinando BaehaBelum ada peringkat
- Complications in UveitisDari EverandComplications in UveitisFrancesco PichiBelum ada peringkat
- Atracurium Besylate Injection DescriptionDokumen13 halamanAtracurium Besylate Injection DescriptionblinkbumbumBelum ada peringkat
- Telp Dosen-DosenDokumen6 halamanTelp Dosen-DosenIndah Sarie100% (6)
- James-Projection of Diabetes Burden ThroughDokumen5 halamanJames-Projection of Diabetes Burden ThroughblinkbumbumBelum ada peringkat
- Muscle RelaxantDokumen9 halamanMuscle RelaxantblinkbumbumBelum ada peringkat
- Atracurium Besylate Injection DescriptionDokumen13 halamanAtracurium Besylate Injection DescriptionblinkbumbumBelum ada peringkat
- Skenario A Blok 16Dokumen24 halamanSkenario A Blok 16blinkbumbumBelum ada peringkat
- James-Projection of Diabetes Burden ThroughDokumen5 halamanJames-Projection of Diabetes Burden ThroughblinkbumbumBelum ada peringkat
- Soal Blok 14Dokumen8 halamanSoal Blok 14blinkbumbumBelum ada peringkat
- Ips 7.0" Hdmi LCD TFT Datasheet: RVT70HSHNWC00-BDokumen17 halamanIps 7.0" Hdmi LCD TFT Datasheet: RVT70HSHNWC00-BC OBelum ada peringkat
- GCE Biology Unit 6 TSM Final (Unit 6 Guide and Examples From Edexcel)Dokumen76 halamanGCE Biology Unit 6 TSM Final (Unit 6 Guide and Examples From Edexcel)razoraz90% (10)
- Ol80 - Bea 220265 en 04Dokumen32 halamanOl80 - Bea 220265 en 04Ds KuzmenkoBelum ada peringkat
- Seminar Report of VRDDokumen34 halamanSeminar Report of VRDSrivatsa RaoBelum ada peringkat
- Commercial Displays BrochureDokumen44 halamanCommercial Displays Brochuredwika katonBelum ada peringkat
- LK315T3LA77 PantallaDokumen23 halamanLK315T3LA77 PantallaIvan ZuñigaBelum ada peringkat
- 7' VisionDokumen17 halaman7' VisionZidane ZizouBelum ada peringkat
- Penetrant Testing History and Visual AcuityDokumen61 halamanPenetrant Testing History and Visual AcuityAhmed Adel100% (1)
- Lighting Handbook Provides Road Lighting Design GuidelinesDokumen244 halamanLighting Handbook Provides Road Lighting Design GuidelinesYamral WubetuBelum ada peringkat
- How to use Dialux for professional lighting design and planningDokumen25 halamanHow to use Dialux for professional lighting design and planningDestiany PrawidyasariBelum ada peringkat
- HDRContrastCTydtgat Et AlDokumen14 halamanHDRContrastCTydtgat Et AldunmunroBelum ada peringkat
- Low Vision - AidsDokumen209 halamanLow Vision - AidsDudi50% (2)
- MOSH-Chapter 9 (Light and Vision)Dokumen46 halamanMOSH-Chapter 9 (Light and Vision)siti zubaidahBelum ada peringkat
- Principles of Art in TeachingDokumen13 halamanPrinciples of Art in TeachingM-Jay GalveroBelum ada peringkat
- CIBSE Lighting Guide LG3-Visual Environment For Display Screen UseDokumen84 halamanCIBSE Lighting Guide LG3-Visual Environment For Display Screen UseANJIBelum ada peringkat
- Halcon 6.1 Shape Matching PDFDokumen46 halamanHalcon 6.1 Shape Matching PDFJonathan PalaciosBelum ada peringkat
- Acer Al2002w (ET) PDFDokumen60 halamanAcer Al2002w (ET) PDFAmanda MillerBelum ada peringkat
- SST102 Introduction to Human Factors and Systems DesignDokumen90 halamanSST102 Introduction to Human Factors and Systems DesignLouis TeoBelum ada peringkat
- The Effect of Omega 3 Supplementation on Contrast Sensitivity in Tuberculosis Patients Treated with EthambutolDokumen11 halamanThe Effect of Omega 3 Supplementation on Contrast Sensitivity in Tuberculosis Patients Treated with EthambutolTeuku Muhammad IrwansahBelum ada peringkat
- TOA1 - 02a Articulation of FormDokumen3 halamanTOA1 - 02a Articulation of Formarkiosk83% (12)
- Accessibility WCAG 2.1 Checklist and Guide - UX TricksDokumen38 halamanAccessibility WCAG 2.1 Checklist and Guide - UX TricksMatías Clemente ArrayaBelum ada peringkat
- HCIA-Intelligent Vision V1.0 Lab GuideDokumen290 halamanHCIA-Intelligent Vision V1.0 Lab GuiderafikiinfoBelum ada peringkat
- Lighting Schemes GuideDokumen6 halamanLighting Schemes Guidepsahoo67% (3)
- Mandatory Appendix V - Asme VDokumen2 halamanMandatory Appendix V - Asme VAngelTinocoBelum ada peringkat
- Dip Unit 1Dokumen75 halamanDip Unit 1sheikdavoodBelum ada peringkat
- TOR CDR ManualDokumen7 halamanTOR CDR ManualAnonymous 2gLSPeBelum ada peringkat
- Human SensesDokumen106 halamanHuman Sensesoracel dataBelum ada peringkat
- Introduction To Penetrant TestingDokumen61 halamanIntroduction To Penetrant TestingjerryceppyBelum ada peringkat
- VA320E Service ManualDokumen24 halamanVA320E Service Manualmosavla100% (1)
- Schematic Eye Model ExplainedDokumen42 halamanSchematic Eye Model ExplainedViora RiandaBelum ada peringkat