9-Nose & Palate
Diunggah oleh
Nur Ain Faezah RoslanDeskripsi Asli:
Judul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
9-Nose & Palate
Diunggah oleh
Nur Ain Faezah RoslanHak Cipta:
Format Tersedia
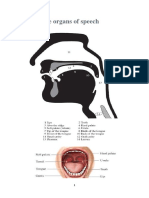
The Nose and Palate
Lecture's date: Thursday 9/4 (lec # 20) At the beginning of the lecture, the doctor has announced that he is not responsible for any studying material except the handout's and the book! So He has no idea about these summarized sheets!! We are going to speak today about: NASAL CAVITY, which is the passageway between the outside anteriorly and the nasopharynx posterior. Nasal cavity is covered by 2 covering, 1) From outside: with skin, what kind of skin is it covered with, from outside? It is stratified squamous epithelium, which is the epidermis layer of the skin 2) From inside: with Mucous Membrane, I mean the lining epithelium of that mucous membrane, which is two types: *) Olfactory Epithelium. : It usually lines the upper 1/3 of nasal cavity and it contains the sensory receptors for smell sensation. **) Respiratory Epithelium. : Which is Ciliated Pseudostratified columnar epithelium that lines the lower 2/3 of the cavity. The Nose consists of external nose and nasal cavity, both of which are divided by a septum into right and left halves. The nose two parts are: 1) The External part, we refer to it as External Nose 2) The Internal part, which is the cavity from inside, we also call it Nasal Cavity Proper, it is just above the oral cavity the only separator between the nasal and the oral cavity is the hard palate.
1) External Nose
External nose consist of bony and cartilaginous parts:
1)The Bony part, so when you touch your nose with your finger
you will notice that the upper part of your nose is bony while the lower part Is more cartilaginous, this bony part contains 3 bony parts around it, which they are; the frontal process of maxilla, the nasal bone, and the small nasal spine of frontal bone.
1
2) The Cartilaginous part however it is more dominant than
bone. *In the slides: We have 2 lateral cartilages, upper and lower one, so when you look to the nasal cartilage, you will see a large upper lateral one and lower lateral one which is also called alar cartilage. So the lower lateral one has two legs or two crura, the lateral crus of major alar cartilage and medial crus, the medial crus of major alar cartilage. *In the middle: there is also one cartilage in the middle that contributes to the midline of the nasal septum, it is called septal cartilage. We also have lesser alar cartilage; which is a small cartilage, usually three in number located behind the lateral ones. We call it like that because sometimes we refer to the lower lateral ones as greater alar.
So let's summarize: we have 4 kinds of cartilages; two upper
laterals, two Lower laterals, nasal septal in the middle and lesser alar a little bit posterior. Pay attention that the greater alar is the same as lower lateral cartilage. External Nose Contains 4 openings: *) 2 anterior openings: these are called Nostrils or Nares. **) 2 posterior openings: these are connecting the nasal cavity to the pharynx, they are called internal Nares, "Dr. told us to go and look for their names!"
Nasal septum
It is the part that separates the nasal cavity into two halves, right and left so if you look at the cross section below you will notice that posterior part is bony, and anterior part is cartilaginous, this septal cartilage is going to dissolve or decompose after death, so we actually see the bony part of the nasal cavity. When we look at the nasal septum we will see that it is formed by: 1) Perpendicular plate of Ethmoid in the posterior aspect, superiorly 2) Vomer bone, also in the posterior aspect but inferiorly 3) Septal cartilage, anteriorly and it is going to be decomposed and dissolved so we will not be able to see.
2
Perpendicular Palte of Ethmoid ( ( .Superopost Septal cartilage (.Ant )
Vomer (.Inferopost )
Moving to the 2nd component of the nose:
2) Nasal cavity
Nasal cavity is the main part of the Nose, which extends from the nostrils, the anterior openings of the nose anteriorly until the posterior aspect of the conchae where it becomes continuous with nasal part of the pharynx, this part, is known as Nasopharynx. It is divided by nasal septum into 2 cavities as I told you before.
Boundaries of nasal cavity:
*The lateral wall: The conchae are always located in the lateral wall, not on the medial one, in the nasal septum; REMEMBER THIS, it is a common mistake by all the students!!! We just refer to the anterior part of the lateral wall, inside the nostrils as the vestibule; this anterior inferior aspect of the nasal cavity, is usually lined with skin, and contains some hair. Now posterior to the vestibule you will see 3 nasal conchae, superior, Middle and Inferior conchae. Superior and middle Conchae both are part of Ethmoid bone while the inferior one is a separate bone by itself. Their function is?? Forming "scroll"!! In order to cover the meatus openings beneath each one of them, meatus means a space, or passage, within the meatus, there we have the mainly openings of the paranasal sinuses, so they are covering the opening of paranasal sinuses.
*The medial wall; when we look at the medial wall of the nasal cavity, we can see the nasal septum, which is made of; perpendicular plate of Ethmoid, Vomer and septal cartilage anteriorly. *Roof/superior wall: is made of four several bones, they are: mainly 1.Cribriform plate of Ethmoid bone 2.body of sphenoid (from post to ant.) 3. Frontal bone and 4.part of nasal bone.
*Floor/inferior wall: it is made by the bony hard palate. Hard palate is separating the nasal cavity from the oral cavity beneath. And it's made up of two bony parts: 1) Palatine process of maxilla 2) Horizontal processes of palatine bone.
Nasal Conchae and Meatuses
Chonchae is a bony elevation that projects inferiorly from the lateral wall of the nasal cavity, like scrolls. As I told you before, they usually are not originated from the same bone, so: *Sup. & mid. conchae are usually from Ethmoid bone *Inf. concha: is a separate bone by itself. Beneath each Concha there is a space, we refer to this space as a meatus, so the meatus is the space where you have opening of Paranasal sinuses or other cavity in the skull. For Ex: The sup. Meatus; contains the opening of posterior Ethmoidal sinuses or air cells. The mid. Meatus: if you cut the mid. Meatus you will see two very important structures there: 1) Bulla Ethmoidalis: It looks like a bulge or a swelling within the middle meatus, it is because of the middle Ethmoidal air cells bulging there and pushing the wall outside forming this elevation. 2) Hiatus Semilunaris: semilunar passage, in the anterior end of the hiatus we have the opening of the frontal sinus along with anterior ethmoidal, and in its main posterior part you will have the opening of maxillary air sinus.
4
Lastly in the Inferior meatus you have only one small opening that is not seen, it is usually covered by mucous membrane, the only opening is Nasolacrimal duct. Nasolacrimal duct: it's not an air sinus, it is just a duct that connects the lacrimal sac in the medial angle of your eye to the nasal cavity because of this duct, When you start crying you will see the tears coming through nasal cavity.
Summary: Sup. Meatus posterior ethmoidal air cells.
Mid. meatus frontal, anterior & middle. ethmoidal & maxillary air sinuses. Inf. Meatus nasolacrimal duct. We still have a small sphenoid air sinus there, where does it open? It opens in a small recess (recess means valley/ ) just above the superior concha. Because this recess is made of 1.body of sphenoid and 2.cribriform plate of Ethmoid, we refer to it as Spheno-Ethmoidal recess. (Its angle located at the roof of nasal cavity) "If you put a wire (!!) In sphenoid body to see where does it open, you'll see it getting into the spheno-ethmoidal recess." It receives the sphenoid air sinuses from each side. So, there is no air sinus opens in the inf. Meatus!!
Arterial blood supply to the nose:
The nasal cavity is the richest area of blood supply! It receives blood supply from many different sources, mainly from four arteries:
1) Sphenopalatine artery:
It comes from post. Aspect, it's a terminal branch of 3rd maxillary artery that usually enters through a small foramen behind the middle conchae, we refer to it as sphenopalatine foramen, just behind the mid. Conchae you see this foramen opening into pterygopalatine fossa. If you still remember, 3rd part of maxillary artery pass within pterygopalatine fossa, 2nd part over the lateral pterygoid and 1st part before the lateral pterygoid fossa.
So terminal branches of 3rd part passes through the Sphenopalatine foramen to get into the nasal cavity to give many branches there, for both septal and lateral wall , in the lateral wall we usually call them: *1) Post.-lateral nasal artery. Post: because they come from the posterior aspect of the Nasal cavity. Lateral Nasal: because its on the lateral wall of the nasal cavity. It also gives another branch that moves medially toward the nasal septum, we call it *2) The septal branch of Sphenopalatine artery
2) Sup. Labial artery
Provides blood supply to the lips, it comes from the facial artery. Once it goes to the upper lip it gives a small branch in the medial wall to supply the ant-inf aspect of nasal septum.
3) Greater palatine artery.
It provides blood supply to the hard Palate, which is actually the floor of the nasal cavity; it is usually a branch from the descending palatine of the 3rd part of maxillary artery. Descending palatine gives two small arteries to the palate, greater and lesser one. The greater one passes all the way anteriorly until the level of incisive foramen, Where it turns back through incisive foramen and go up to the nasal cavity, so we refer to it as the incisive branch of greater palatine artery. So the descending palatine artery gives arteries that pass deep within pterygomaxillary, within pterygopalatine fossa. Appears then in the palate as greater palatine, and greater palatine back again into the incisive canal to the nasal cavity, Why does descending palatine artery supply the floor of the nasal cavity? Because the hard palate is the floor of the nasal cavity and the roof of the oral cavity, it is the separating wall between oral and nasal cavity.
So we have: *Sphenopalatine a.: to the posterior aspect *Septal branch of sup. Labial a.: to the ant. Aspect. *Greater palatine a.: to the floor. *ethmoidal arteries: to the roof.
Ethmoidal artery:
6
Ethmoidal artery has 4 branches 2 ant. And 2 post. That provide Blood supply to the roof of the nasal cavity, these branches usually come from ophthalmic artery from the orbit, one anterior ethmoidal a. and 2 posterior ethmoidal artery which pass the wall of the orbit to oral cavity. By this we have 4 arteries; all these arteries anastomose in the ant-inf aspect of the nasal septum, forming what we call (klesselbach area, an Area in the nasal septum) this is where bleeding of the nose (Epistaxis) happens. =) You have to know each artery and where does it come from.
Nasal venous plexus
Beneath The mucous membrane of the nasal cavity you have a rich network of veins, we refer to it as the nasal venous plexus, this nasal venous plexus communicates anteriorly with facial vein where posteriorly it drains into pterygoid venous plexus in the infra temporal fossa. Which (i.e. pterygoid plexus) in turn drains into maxillary vein.
Nasal bleeding-(epistaxis)
Causes; there are so many various causes, simply from just picking your nose (playing with it!!) until more systemic condition like hypertension or hemophilic disorders & so many other causes!!! Location: in the ant-inf part of the nasal septum which we refer to it as Klesselbach area, its usually from septal branches of sphenopalatine artery and the septal branch of sup. Labial artery. Treatment: is by promoting blood clotting to this area by backing it with absorbent material like a gauze ( ,) and applying direct pressure on the external nose, usually for 5-10 min, with the head at??? *when moving the head backward: the bleeding start to go back to the nasopharynx and you start to swallow the blood & youll have bleeding there!! *when moving forward: you will enhance the bleeding more by the sphenopalatine artery which Pass there!!! So the best position is neutral position!!!!
Innervations to the nasal cavity
We have 2 kinds of innervations: Special sensation: olfaction, smell from the olfactory nerve, it has the olfactory 1st order neurons that are located in the olfactory epithelium its usually a simple columnar epithelium just above the sup. Concha where they ascend through the cribriform plate of Ethmoid to synapse in the olfactory pulp. General sensation: to the nasal cavity, comes from the, 1) Maxillary nerve V2 2) Ophthalmic nerve V1. The maxillary (V2) branches, which usually provide innervations for the post. Aspect of the nasal cavity, are: 1) Nasopalatine branch of maxillary nerve (enters through sphenopalatine foramen) 2) Greater palatine nerve, which provides innervation to the hard palate, which is the floor of the nasal cavity. The ophthalmic nerve (V1) now provides innervation to the anterior aspect of the nasal cavity, through anterior ethmoidal nerve, which divides into 2 branches; 1) Internal nasal (toward the vestibules) to the mucous membrane and 2) External nasal to the skin from outside until the top of your nose. in the slides there is a figure showing the nerve contributing to the general sensation in the nasal cavity, Dr. Allouh explained it repeating all the nerves above"
Paranasal sinuses
(Please read your text for complete description of these sinuses). Sinuses are air-containing spaces within cranial bones; they are lined with respiratory epithelium, which kind of respiratory epithelium? Ciliated columnar epithelium. Suggested Functions: 1) Reduce skull weight 2) Voice modification (resonators) 3) Insulation effect: prevent heat loss from nasal cavity. All these things we have previously mentioned in the skull. How many sinuses we have there? And where does each one open? We have:
8
1) The frontal sinus, that opens in the middle meatus within hiatus similunaris 1) The sphenoid sinus opens in sphenoethmoidal recess 3) The maxillary sinus. Which is the largest one; it is pyramidal in shape, and opens into middle meatus 4) Ethmoidal ear cells, they are 3 in number, Ant. one opens along with the frontal into the middle meatus, the middle one opens into middle meatus, and the post one, open into sup meatus. 5) The last one is mastoid air cells, which is present within the mastoid process of temporal bone, which opens in the middle ear.
Sinusitis and meningitis
It's a pus ( )producing infections within the air sinuses, especially, frontal and sphenoid air sinuses, since these sinuses are highly close to the cranial cavity inside. So when we have pus production, the inflammation starts to erosive the bone until getting into the bone of the cranial cavity, where it then leads to meninges inflammation which is called meningitis. So sinuses some times lead to meningitis, there is a high risky erosion of the cranial cavity in children because of the softness and thinness of bony septa.
Intracranial surgery and sphenoid sinuses
It is usually done by using an endoscope, when you go to the pituitary gland or optic nerve surgery. This is very simple, just go and read it from the slide!
The palate
What is palate, which cavities does it separate? It separates the oral and nasal cavities; it consists of hard and soft part.
1) Hard palate:
The hard palate, which contains bone, is forming the ant 2/3 or 3/4 of the whole palate it is made of 2 plates: 1) Horizontal plate of palatine bone 2) Palatine process of maxilla And it forms the floor of the nasal cavity.
2) Soft palate
9
The soft palate, is a fibromuscular fold (tendons), (Fibro: refers to fibrous tissue, usually tendons for muscle's apponurosis and, Muscular: refers to the muscle), that is covered with mucosa and attached posteriorly to the hard palate. It is forms 1/3 or 1/4 of the whole palate. It's composed of Mucous Membrane which covers its surfaces; it is covered with two types, masticatory mucosa, which is usually related to the oral cavity in the lower part, and the respiratory epithelium, which lines the upper part that pass in the nasopharynx. the main part or cornerstone ( ) that forms the soft palate is what is called: the palatine aponeurosis, aponeurosis means a flat tendnous sheet, its a fibrous sheet that represents the expanded tendon of tensor veli palatini muscle, which is a muscle that descends down from the sphenoid spine in the skull, until the level of pterygoid hamulus, which is a process that goes up from the lateral plate of pterygoid.there the tendons of this muscle turn horizontally from this side to fuse on the tendon of opposite side to form the palatine aponeurosis, it attached anteriorly to the hard palate. So soft palate base is from expanded tendon of tensor veli palatini.
Muscles of the soft palate
We know that cornerstone was the palatine aponeurosis, so there are 5 several muscles that attach to this aponeurosis contributing to the soft part of the palate, these will be: The 1) Levator Veli Palatini, which when contracts, elevates the soft palate it descends down from the tube, Auditory (Eustachian tube), which connects the middle ear to the nasopharynx, and continue all the way down to fuse with the soft palate, in palatine aponeurosis. The upper two muscles are: 2) The palatoglossus m., connects the soft palate to the tongue, it is usually the boundary between the oral cavity and the pharynx. Since it's the boundary of the end of oral cavity, it usually forms a fold of mucous membrane above it; we refer to it as the palatoglossus fold (ant. to palatine tonsils). It narrows the oropahryngeal (Isthmus), its the boundary between the pharynx and the oral cavity, so when it contracts it pulls the soft palate down and elevates the tongue up 3) Palatopharyngus m.: it descends from the soft palate all the way down to the pharynx posteriorly. When it contracts it Elevate the wall of the pharynx and depresses the soft palate.
10
It forms pallatopharyngeal fold, which is a posterior fold of a mucous membrane over this muscle. (So when you open your mouth you see can see 2 folds, an anterior and a posterior one, the anterior one is the palatoglossal. The posterior one is the palatopharyngeal). Between these two upper muscles we have, the tonsilar bed where your palatine tonsils rest. 4) Tensor veli palatine, which forms the palatine aponeurosis. The last one is 5) musculus uvula: it's the muscle attached ant, to hard palate and palatine aponeurosis all the way post. To attach to the mucous membrane over the uvula. The uvula is a conical projection from the post. Border of soft palate you can just see it when you open your mouth, this uvula if we cut it's mucous membrane we can see a muscular fiber inside it, these muscle fibers are the musculus uvuli, these muscles when they contract, they elevate the uvula up The innervation for all these muscles of soft palate is: The pharyngeal plexus, a plexus of nerves consists of glosopharyngeal n., vagus n. and cranial root of accessory n., (9, 10, 11, CN); these nerves form a network of nerves providing innervation to the whole palate except one muscle, which is tensor veli palateni which is innervated by mandibular nerve V3. All muscles of the tongue are innervated by: hypoglossal nerve except palatoglossus muscle, because we consider it part of the palate, you remember last lec. So it is innervated by pharyngeal plexus The dr. repeated again this point!! (I think its very important) *all muscles of tongue are innervated by hypoglossal nerve except palatoglossus; its by pharyngeal plexus, becouse we consider it part of the soft palate. *all muscles of soft palate innervated by pharyngeal plexus except tensor palatini veli, which is innervated by mandibular nerve V3
You have to read your book for the origin, insertion, innervations and action for each of these muscles :). Refer to your textbook, Table 11-9,p.785
11
Arterial blood supply to the palate
We have 3 main arteries which supply the palate. 1) Descending palatine artery (the main one) it comes from the
3rd part of maxillary artery, which gives two arteries, the main one descends in pterygopalatine fossa, all the way in the palatine canal until it reaches the palate, where it divides into two branches, *1) Greater palatine artery: artery from greater palatine foramen to provide blood supply to hard palate *2) Lesser palatine artery: from lesser palatine foramen to provide blood supply to the soft palate. Originates from facial artery
2) Ascending palatine artery: originates from facial artery. 3) Ascending pharyngeal artery, originates from External carotid
artery, (((according to the book)).
Innervation to the palate
1) Greater palatine nerve. From V2, it enters through greater palatine foramen just at the posterior boundary of the hard palate and goes anteriorly to supply the hard palate and upper teeth gingiva, it's the nerve that you have to anesthetize when you want to extract any posterior tooth, (premolars and molars) You actually anesthetize the palatal gingival, which is actually the greater palatine nerve.. 2) Lesser palatine nerve, from V2, it enters through lesser palatine foramen and supplies the soft palate, the fibromuscular fold. 3) Nasopalatine nerve, from V2, it contribute to the innervation of posterior aspect of nasal cavity, it enters the nasal cavity through sphenopalatine foramen and send a septal branch all the way in nasal cavity, and then it gets into the palate through the incisive canal (within hard palate)to supply the primary palate (which is the area of the palate
12
just behind the four incisor teeth) so here it become called the incisive nerve. *Incisive nerve is a continuation of Nasopalatine nerve. When you want to extract any anterior maxillary tooth you anesthetize the region of the primary palate, incisive nerve.
Structures on the palate:
The 1st thing you can see just behind the incisors, are folds of mucous membrane, we refer to it as the Palatine Rugae 1) Palatine Rugae, they provide a rough surface on the 1st palate Suggested functions: *) In speech: when you speak you press your tongue against them that helps in producing proper pronouncing for the letters **) Also preparation of food to swallow; because once you want to swallow you also press your teeth against them, preparing to close your oral cavity. Another part,
2) Vibrating line: it is a movable part, when you look to the palate
then you can see it here by detecting the end of the hard palate and the starting of the soft palate, now when you see the soft palate, you can see that the anterior half of it is usually attached to the hard palate where it contains palatine aponeurosis, this is a non movable part, behind it there is a remaining of the soft palate, which are muscles, (5 M. we talked about it before), those parts are the movable part of the soft palate, so the vibrating line is the boundary between movable and non movable parts of the soft palate. How we discover this line? We ask the patient to open his mouth and say, aaaaaaaahhh! When he says that, you will see the soft palate vibrating. The small area, 2 mm, which doesn't move, will indicate the border between movable and non movable part, which we call the vibrating line... This line is important in prostodontics, because dentures have to be there, the posterior edge of the upper denture should be anterior to the vibrating line, in the non movable part of the soft palate... Why should it be like that? Because if a denture comes in the hard palate against the bone, it cant press the soft palate so it will keep fallings down, it will not even fit, if you have a rigid surface and you want to put another rigid surface against it, it will not fit, so it cant fit in the hard palate..
13
If you put it in the movable part of the soft palate, you will see that once the patient talks or tries to eat, his denture will fall down, this is the most common mistakes in falling down of upper denture!!, when the dentist puts the post edge of upper(denture in the movable part of soft palate..) If it is in the non movable part, which contains soft tissue that is so easy to be pressured, this will keep the denture in its position. **So it must be anterior to the vibrating line in the nonmovable hard palate, but not too much anterior until it reaches the hard palate. The vibrating line lies at short distance just behind the junction of hard and soft palate. Dr. showed on a slide a picture contains labels for uvula, hard palate etc"
Cleft palate
When we speak about cleft palate we have to know how the palate is developed! The palate start to develop by three parts, The ant part: Which we refer to it as primary palate or premaxilla, this part is developed from the median nasal process and it is present there already, it is holding the upper 4 incisors. posterior to premaxilla we have the secondary palate, which is formed by fusion of the palatal processes of maxilla , the two horizontal plates, they move up horizontally until they unite in the midline, after both processes unite, primary and sec. fuse together at the midline, so what kind of abnormally happened there? The development happened by failure of both palatine processes to fuse together, and the second to fuse with the primary palate. By this we will have a cleft in the hard palate ( ,)we refer to it as the cleft palate. This cleft in the palate will connect the oral cavity with the nasal cavity superiorly, so it will allow the air, liquids or even food to pass from mouth to nose or vice versa, so when the baby sucks his milk or food, it goes through nasal cavity or even goes into the respiratory passage, and this is a very dangerous situation before the 1st years, which leads to feeding difficulty. Later on after the child grows up and start to talk it gives the child difficulty of speaking, so when he put his tongue in the palate where there is a space, this situation will produce improper speech. The prevalence: is about 1/1000, it is most commonly in the native Indians. () Treatment: you can treat by doing a surgery to the child in his 1st years, it treated by putting an upper denture to separate between oral and nasal
14
cavity. This surgery is usually done when the child is older than 1 year old.
We have 4 degrees of cleft palate or even 5 sometimes. 1)1st degree: We refer to it as, Cleft uvula, when Just the uvula, the little V-shaped fleshy mass hanging from the back of the soft palate. 2) The 2nd degree: failure of the 2 palatine processes (in 2o palate) to fuse along with the 1st degree, cleft uvula 3)The 3rd degree: cleft between the 2nd palate, the uvula and one side between secondary and primary palate, so its unilateral cleft, total unilateral cleft lip and palate. 4) The 4th degree: Total Bilateral cleft lip and palate, or cleft palate only, but most of the time it associated with a cleft in the lip failure of fusion between the uvula, the palatine processes of maxilla, primary palate and sec palate in both sides. It's called "total bilateral cleft lip & palate or palate only) The 5th degree: A very rare form may occur in which a bilateral cleft lip and failure of the primary palate to fuse with the palatal processes of the maxilla on each side are present What you have to know for this course, is just the degrees of the cleft Palate, you will study treatment and stuff later in the 4th year. Finally done! Forgive me for any mistakes :) Anhar 3loush. Special thanks to my fianc, Ibrahem - you are the source of my courage and strength, Thank you for what you have given me.obelnja7 bel emte7anat, shed 7alak, brtakan 3leek... T7yee lkol 9a7bate O l a7la shrekat bkol eldnya Samar Mawasi, o Heba Khalelye, omabrrok el ta5aroj, 3okbalna ya rab
15
Marwa Rayyan, Huda Abo mo5, 3rd yr, 6b asnan, 3njaad shokran 3la kolshi, wallah ma Fe mnkom Edited & revised by: AYA E. Sawalmeh Edited by # 4.
16
Anda mungkin juga menyukai
- 11 PharynxDokumen8 halaman11 PharynxNur Ain Faezah RoslanBelum ada peringkat
- 7 Infratemporal RegionDokumen8 halaman7 Infratemporal RegionNur Ain Faezah RoslanBelum ada peringkat
- 2 - The Brain#1Dokumen10 halaman2 - The Brain#1Nur Ain Faezah RoslanBelum ada peringkat
- 2 - The Brain#1Dokumen10 halaman2 - The Brain#1Nur Ain Faezah RoslanBelum ada peringkat
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Maxillary Impression ProceduresDokumen40 halamanMaxillary Impression ProceduresSeena SamBelum ada peringkat
- SpokenEnglish Sec1 Lesson1Dokumen8 halamanSpokenEnglish Sec1 Lesson1AugustoCésarBelum ada peringkat
- Voiceless Voiced: Bilabial BilabialDokumen4 halamanVoiceless Voiced: Bilabial BilabialAhmed El-SaadanyBelum ada peringkat
- Use of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFDokumen9 halamanUse of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFJose Luis Granados SolerBelum ada peringkat
- Essay Phonetics Question Number 2Dokumen2 halamanEssay Phonetics Question Number 2Victor TanBelum ada peringkat
- Clinical Anatomy of ORAL CAVITY-2016 PDFDokumen29 halamanClinical Anatomy of ORAL CAVITY-2016 PDFshagufta lailaBelum ada peringkat
- Maxillofacial Defects and Their Classification: A Review.: ArticleDokumen7 halamanMaxillofacial Defects and Their Classification: A Review.: ArticleVivek ShankarBelum ada peringkat
- Malayalam InternationalDokumen469 halamanMalayalam InternationalReshmiBelum ada peringkat
- Full Download Test Bank For Cleft Palate Craniofacial Anomalies Effects On Speech and Resonance 3rd Edition PDF Full ChapterDokumen36 halamanFull Download Test Bank For Cleft Palate Craniofacial Anomalies Effects On Speech and Resonance 3rd Edition PDF Full Chaptermoviequilter3ouid100% (17)
- Speech OrgansDokumen4 halamanSpeech OrgansJoshua Basa100% (1)
- The Organs of SpeechDokumen6 halamanThe Organs of SpeechAnonymous ToHeyBoEbX100% (1)
- Cleft Palate: Wan Khadijah Wan Yusoff Noor Afika Binti AzriDokumen91 halamanCleft Palate: Wan Khadijah Wan Yusoff Noor Afika Binti AzriWOne WannBelum ada peringkat
- Phonetics I - Producción Pedagógica (New) PDFDokumen85 halamanPhonetics I - Producción Pedagógica (New) PDFDariusVelzBelum ada peringkat
- Hard & Soft Palate + InnervationDokumen7 halamanHard & Soft Palate + InnervationSahrish IqbalBelum ada peringkat
- Posterior Palatal SealDokumen74 halamanPosterior Palatal SealAmit Bhargav50% (2)
- How The Speech Organs Work in English?Dokumen18 halamanHow The Speech Organs Work in English?haithamBelum ada peringkat
- Posterior Palatal SealDokumen55 halamanPosterior Palatal SealEazhil RajBelum ada peringkat
- Malayalam International TransliterationDokumen89 halamanMalayalam International TransliterationSASHMIRA MENONBelum ada peringkat
- Sommerlad-2003-Plastic and Reconstructive SurgeryDokumen7 halamanSommerlad-2003-Plastic and Reconstructive SurgeryAbdul HameedBelum ada peringkat
- Speech Assessment and Nasopharyngoscopy HO 11 07 11Dokumen164 halamanSpeech Assessment and Nasopharyngoscopy HO 11 07 11catatutuBelum ada peringkat
- Cleft Lip and PalateDokumen23 halamanCleft Lip and PalateStella100% (1)
- Speechmechanism 130116053514 Phpapp02Dokumen36 halamanSpeechmechanism 130116053514 Phpapp02Robert MestiolaBelum ada peringkat
- BAAPSDokumen147 halamanBAAPSGaurav Patodia100% (1)
- Test Bank For Cleft Palate Craniofacial Anomalies Effects On Speech and Resonance 3rd EditionDokumen11 halamanTest Bank For Cleft Palate Craniofacial Anomalies Effects On Speech and Resonance 3rd EditionTina Vetter100% (31)
- Cleft Palate and Craniofacial Anomalies Effects On Speech and Resonance 3rd Edition Kummer Test BankDokumen11 halamanCleft Palate and Craniofacial Anomalies Effects On Speech and Resonance 3rd Edition Kummer Test BankAnnetteOliverrbwcx100% (14)
- History of Maxillofacial ProsthesisDokumen34 halamanHistory of Maxillofacial ProsthesisMoataz Mohamed Barakat100% (1)
- OralMechanismExamKit 1Dokumen11 halamanOralMechanismExamKit 1ABELIZ DURANT MUNIZBelum ada peringkat
- 10-16-01 Cleft Lip and Palate Part 1Dokumen52 halaman10-16-01 Cleft Lip and Palate Part 1Zoilo NuñezBelum ada peringkat
- Test Bank For Cleft Palate Craniofacial Anomalies Effects On Speech and Resonance 3rd EditionDokumen11 halamanTest Bank For Cleft Palate Craniofacial Anomalies Effects On Speech and Resonance 3rd EditionswungnauticaldenBelum ada peringkat
- Phonetics and PhonoDokumen24 halamanPhonetics and PhonoMOHAMMAD AGUS SALIM EL BAHRIBelum ada peringkat