Infeksi Saluran Kemih
Diunggah oleh
Niken Mareta0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
66 tayangan35 halamantanda dan gejala ISK
Hak Cipta
© Attribution Non-Commercial (BY-NC)
Format Tersedia
PPT, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen Initanda dan gejala ISK
Hak Cipta:
Attribution Non-Commercial (BY-NC)
Format Tersedia
Unduh sebagai PPT, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
66 tayangan35 halamanInfeksi Saluran Kemih
Diunggah oleh
Niken Maretatanda dan gejala ISK
Hak Cipta:
Attribution Non-Commercial (BY-NC)
Format Tersedia
Unduh sebagai PPT, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 35
wie pm
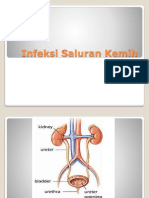
INFEKSI SALURAN KEMIH
DWI LESTARI PARTININGRUM
Nephrology and Hypertension Division
Internal Medicine Department
Medical Faculty Diponegoro University/ Kariadi Hospital
wie pm
Introduction: UTI
commonest bacterial infection for GP
substantial morbidity
wide clinical spectrum (mild severe sepsis)
Urinary tract is normally sterile
Definition of UTI:
any bacteria multiplying in the urinary tract
regardless of bacterial count
wie pm
+Definisi :
ISK akibat invasi mikro organisme pada jaringan
traktus urinarius (TU) dari orifisium uretra
korteks ginjal.
Normal TU steril.
Adanya bakteri dalam urin (bakteriuria) TU
berisiko alami infeksi.
Kultur (+) : kuman > 100.000/ml urin.
wie pm
Prevalensi ISK
wie pm
KLASIFIKASI
Lokasi Anatomis: ISK atas & ISK bawah.
ISK Complicated & ISK Uncomplicated.
Klasifikasi Klinis :
*Asymptomatic bacteriuria
*Acute uncomplicated cystitis in women
*Recurrent infections in women
*Acute uncomplicated pyelonephritis in women
*Complicated UTIs in both sexes
*Catheter-associated UTIs
wie pm
ginjal
ureter
Kandung
kemih
ISK ATAS
ISK BAWAH
Pyelonefritis
Ureteritis
Cystitis
Prostatitis
Epididimitis
Urethritis
GEJALA
Demam
Menggigil
Nyeri pinggang
Mual muntah
Penurunan BB
gejala isk bawah
Nyeri supra pubis
Disuria
Frekuensi
Urgensi
Hematuri
wie pm
Klasifikasi ISK
Dari segi PENATALAKSANAAN dibedakan atas :
1. ISK uncomplicated (simple) :
- ISK sederhana anatomik maupun fungsional TU normal.
- Terutama mengenai wanita.
- Infeksi hanya mengenai mukosa superfisial kandung kemih.
- Penyebab kuman tersering (90%) adalah E. coli.
2. ISK complicated
- Sering menimbulkan banyak masalah, krn didasari hal ttt.
- Sering kuman penyebab sulit diberantas resisten terhadap
beberapa macam antibiotik
- Sering terjadi bakteriemia, sepsis dan syok.
- Penyebab : Pseudomonas, proteus, klebsiela dll.
wie pm
ISK Complicated terdapat keadaan sbb :
1. Kelainan abnormal saluran kencing.
Contoh : batu, obstruksi, refluks vasikouretral, atoni
kandung kemih, kateter menetap, prostatitis menahun.
2. Kelainan faal ginjal. baik GGA maupun GGK.
3. Gangguan daya tahan tubuh. Penderita DM,
neutropenia, penderita dg terapi imunosupresif.
4. Infeksi disebabkan organisme virulen.
Seperti proteus spp yg memproduksi urease, Infeksi
metastatik staphylococcus.
wie pm
Pathogenesis
Routes of bacterial invasion
1. Ascending
common
2. Hematogenous
staphylococcus
mycobacterium
tuberculosis
salmonella
3. Lymphatic: rare
wie pm
Host defences
1. Bladder
bladder emptying
mucosal phagocytes
2. Antibacterial substances
3. Anti-adherence mechanisms
urine, bladder & prostatic
secretions
wie pm
Pathogenesis of urinary infection
Bacterial virulence vs. host defences
1. Inoculum
2. Adherence characteristics
3. Failure of urinary defence
obstruction, calculi, VUR
incomplete bladder emptying
diabetes mellitus & elderly
wie pm
Patogenesis lanjutan
+Bacterial factor
-95% dari luar TU
-5% hematogen
+Host factor
-Wanita : uretra pendek, kolonisasi kuman pd
introitus vagina, sex intercourse, tampon,
spermatisid, diafragma, menopause (lactobaccili).
-30% ISK kandung kemih (cystitis) invasi ke ginjal
akibat dari VUR
-Infeksi pd ginjal sering di medula kons amonia
, osmol , pH , blood flow , PO2 rendah.
wie pm
Jumlah organisme pada ISK :
70% ISK jml kuman > 100.000 kuman/ml urin.
30% ISK jml kuman lebih rendah, mis; pend. pria,
wanita dg disuria akut, wanita dg ISK berulang
karena stapphylococcus.
Pemeriksaan urinalisa :
Epitel skuamos kemungkinan kontaminasi.
Piuria infeksi/ peradangan.
Silinder lekosit pielonefritis.
DIAGNOSIS
wie pm
Pemeriksaan kultur urin, yg didapat dari :
a. Urin porsi tengah (mid stream urin)
b. Urin aspirasi suprapubik
c. Urin kateter kandung kemih (hindari)
Dalam interpretasi kultur urin porsi tengah !! sbb :
95% ISK disebabkan monomikrobial
95% ISK disebabkan gram negatif/ enterococci
Staphylococcus epidermidis, diptheroids &
lactobacilli jarang menimbulkan ISK.
wie pm
Bakteri penyebab ISK
Mikroorganisme Kultur positif ( % )
E. Coli 60 - 90 %
Klebsiela / Enterobacter 10 - 20 %
Proteus 5 - 10 %
Pseudomonas aurogenosa 2 - 10 %
Staph. Epidermidis 2 - 10 %
Enterokokkus 2 - 10 %
Kandida albikan 1 - 2 %
Staph. Aureus 1 - 3 %
wie pm
Asymptomatic Bacteriuria
wUmumnya terjadi pd wanita
2% - 4% wanita muda, 10% wanita >60 th.
wBila ada DM risiko ISK 3 - 4x nya.
wLaki2 jarang sekali, kecuali umur tua dg
hipertrofi prostat.
wTidak perlu antibiotik. (kecuali didapatkan kultur +
kuman 100.000 CFU/mL pada 2x pemeriksaan, dg jenis
kuman sama)
wie pm
Asymptomatic UTI
screening & symptoms minimal (urine odour)
Prevalence (%)
Neonates 1 (-> 50% VUR)
Schoolgirls 1-2
Young women 10
Non-pregnant women 3-10
Pregnant women 5-6 (15-20% -> PN)
Elderly men & women 5-40 (age)
wie pm
Terapi ISK Uncomplicated ( Simple )
=ISK yg paling sering dijumpai dlm praktek dokter.
=Manifestasi kliniknya sindroma disuria-frekuensi.
=Piuria > 10/lpb, kultur (+)
=Keluhan sering kencing sedikit2, sakit waktu kencing
serta rasa tidak enak didaerah suprapubik. Disertai
demam subfebril ().
wie pm
Antibiotika dosis
tunggal
Observasi 4-7 hari
Tanpa gejala Gejala positif
Kultur urin
Urinalisis (piura)
Kultur (bakteriuri)
negatif
positif
sembuh
Antibiotika
5-14 hari
Observasi
analgetik
Antibiotik
4 6 Minggu
Anti Chlamidia
Trachomatis
(-) (-) (+) (-)
Penatalaksanaan klinis wanita dg sindroma disuria frekuensi
(+/-) (+)
wie pm
wie pm
Anatomic or structural risk factors
Obstructive utopathy (stones, strictures, tumors, prostate associated
Instrumentation (catheter associated and nosokomial infection)
Renal cystic disease
Ureteral stents & surgical urinary diversions, ileal loop constructions
Other : vesicoreteral reflux (VUR), urachal remnant
Functional risk factors
Diabetes mellitus
Renal transplantation
Spinal cord injury & neurologic dysfunction
Neutropenia
Human immunodeficiency virus
Micellanous complicated infection
Pyonephrosis
Emphysematous pyelonephritis & cystitis
Malakoplakia and xantogranulomatous pyelonephritis
Intramural vesical abcess
Urosepsis
Tuberculosis
Infections caused by atipical or resistant organism : vancomycin resistant
enterococci, anaerobes, etc
Faktor risiko dan komplikasi ISK komplikata
wie pm
TREATMENT
1. Empiric therapy must be broad spectrum with
definitive therapy based on culture and sensitivity
2. Moderately : Levofloxacin (500 mg IV/PO q24),
ciprofloxacin (500 mg PO twice-daily/400 mg q 12h
IV)
3. Severely : cefepime 2g IV q12 hrs, ceftazidime 2 g IV
q8 hrs, Imipenem 500 mg IV q6 hrs, meropenem 1 g
IV q8 hrs, doripenem 50 mg IV q8 hrs, piperacillin-
tazobactam 3.375-4.5g IV q6 hrs
wie pm
Acute pyelonephritis
hemorrhage & swelling
PMN infiltration
H&E
wie pm
Clinical diagnosis: pyelonephritis
1. Fever T > 38
0
C, rigors, chills, sweats
2. Loin pain
3. Constitional symptoms
anorexia, nausea, vomiting, diahorrea, myalgia,
headache
4. Lower urinary symptoms
dysuria, frequency (30 - 50%)
supra-pubic discomfort
UA: pyuria, leukocytes, hematuria
wie pm
Leukocyte casts
2. Passage into urine
1. Formation of WBC cast
3. Degenerate WBC cast
in fibrillar matrix
PMN
EM
BF
Tubular lumen
Matrix
PMN
H&E
PMN
wie pm
Bacterial casts
pyelonephritis
usually with leukocytes
EM
EM
PMN
bacilli
PMN
bacilli
bacilli
wie pm
Pyelonephritis
80%
Uncomplicated
Acute
pyelonephritis
10%
Complicated
Acute
pyelonephritis
10%
Chronic
pyelonephritis
smouldering
Medical
therapy
Medical and/or
surgical therapy
Medical and/or
surgical therapy
100%
Cured
100%
Progressive
renal damage
60%
Cured
40%
Progressive
renal damage
wie pm
Pengelolaan :
1. Umum : cairan cukup, elektrolit & nutrisi.
2. Atasi komplikasi : syok, urosepsis, GGA atau DIC.
3. Pikirkan tindakan bedah, ( pus karena obstruksi
saluran kemih).
4. Antibiotika parenteral sampai 24 jam bebas
demam ganti oral.
wie pm
Sambil menunggu hasil kultur, diberikan antibiotika berspektrum
luas seperti :
- Kombinasi ampicilin dan sefalosporin gen I
- Aminoglycoside dg Betalactam.
- Ticarcillin dg clavulanic acid.
- Quinolone
Antibiotika oral selama :
O 5-14 hari = 50% relaps.
O 4-6 minggu = angka keberhasilan mencapai 90%.
wie pm
Catheter associated UTI
biofilm colonisation common with long-term
urinary catheters
may cause septicemia in debilitated patient
Treat with A/B when:
fever, sepsis
symptoms attributable to UTI (e.g. agitation)
short-term catheter & UTI
Observe long-term biofilm colonisation
wie pm
Prevention of catheter-associated UTI
short duration
insert under aseptic technique by trained staff
(or trained patient for intermittent self-
catheterisation)
bag below bladder & emptied regularly
keep system closed - sample urine by sterile
aspiration
antimicrobial cream in women
A/B for cardiac valvular abnormalities
wie pm
wie pm
UTI in males
Uncircumcised boys
bacteria under foreskin -> UTI
Adult males
prostate often source
antibacterial prostatic secretion
-> fails in chronic prostatitis
Homosexual males
5% with UTI
E Coli: same serotype
wie pm
Acute bacterial prostatitis
Young men < 35 y.o. or STD risk
C. trachomatis or N. gonorrhoeae
1. Rx. as gonorrhoea then
2. doxycycline 100 mg / d x 7 days
Older men > 35 y.o.
Enterobacteriaceae
ciprofloxacin 500 mg BD x 14 days
co-trimoxazole BD x 14 days
wie pm
Anda mungkin juga menyukai
- ISK PANDUANDokumen28 halamanISK PANDUANAisyah Aftita KamrasyidBelum ada peringkat
- Kuliah ISKDokumen21 halamanKuliah ISKlisda rizky amaliaBelum ada peringkat
- Urinary Tract InfectionsDokumen10 halamanUrinary Tract InfectionssindyBelum ada peringkat
- CSS IskDokumen19 halamanCSS IskSelaBelum ada peringkat
- ISKDokumen21 halamanISKZaid Zalizan100% (1)
- Infeksi Saluran KemihDokumen20 halamanInfeksi Saluran KemihAxelJusufBelum ada peringkat
- Fionna Masitah (Isk)Dokumen16 halamanFionna Masitah (Isk)Fionna PohanBelum ada peringkat
- Referat Infeksi Saluran KemihDokumen18 halamanReferat Infeksi Saluran KemihFerdita RidhaBelum ada peringkat
- ISKDokumen34 halamanISKIvana Ester Sinta UliBelum ada peringkat
- ISK BERULANGDokumen32 halamanISK BERULANGNovita Rotua Sari SitumeangBelum ada peringkat
- ISK&Genitalpria (Dr. Hendra)Dokumen37 halamanISK&Genitalpria (Dr. Hendra)Nur HasanahBelum ada peringkat
- Interna Uro SistemDokumen157 halamanInterna Uro SistemIrma ManoyBelum ada peringkat
- Infeksi Saluran KemihDokumen168 halamanInfeksi Saluran KemihRiza MaulidaBelum ada peringkat
- INFEKSI SALURAN KEMIHDokumen46 halamanINFEKSI SALURAN KEMIHriyanBelum ada peringkat
- Askep Infeksi Saluran KemihDokumen22 halamanAskep Infeksi Saluran KemihudhinadBelum ada peringkat
- ANATOMI DAN HISTOLOGI ORGAN GENITALDokumen64 halamanANATOMI DAN HISTOLOGI ORGAN GENITALalmira valmaiBelum ada peringkat
- Referat Infeksi Saluran KemihDokumen18 halamanReferat Infeksi Saluran KemihMuhammad Reza Fahlevi100% (1)
- Infeksi Saluran Kemih BaruDokumen31 halamanInfeksi Saluran Kemih BarumarthaBelum ada peringkat
- Laporan Kasus Hidronefrosis DX Dan Uti-1Dokumen53 halamanLaporan Kasus Hidronefrosis DX Dan Uti-1Merdiana Fithroya50% (2)
- ISK PENGERTIANDokumen27 halamanISK PENGERTIANiyamBelum ada peringkat
- ISK AnakDokumen24 halamanISK AnakRahmi MeitiaBelum ada peringkat
- Css IskDokumen37 halamanCss IskFebrian AlfaroBelum ada peringkat
- LP Infeksi Saluran KemihDokumen12 halamanLP Infeksi Saluran KemihChairunnisa Permata SariBelum ada peringkat
- Patologi UrologiDokumen46 halamanPatologi UrologinasimBelum ada peringkat
- 4 Infeksi Saluran KemihDokumen37 halaman4 Infeksi Saluran KemihmarlisaBelum ada peringkat
- Isk - Dwi - FinalDokumen35 halamanIsk - Dwi - FinalNovitha DestaryBelum ada peringkat
- Infeksi Saluran Kemih Dan Askep HastinaDokumen11 halamanInfeksi Saluran Kemih Dan Askep HastinaHastina Fcbarca SaranghaesujuBelum ada peringkat
- Infeksi Saluran KemihDokumen37 halamanInfeksi Saluran KemihRisma J Asif100% (1)
- Infeksi Saluran KemihDokumen14 halamanInfeksi Saluran KemihNurul Ilma AllauwBelum ada peringkat
- GINJALDokumen97 halamanGINJALRofi IrmanBelum ada peringkat
- Patogenesis ISKDokumen28 halamanPatogenesis ISKUmy PolpokeBelum ada peringkat
- ISK AnakDokumen14 halamanISK AnakSri rejekiBelum ada peringkat
- Infeksi Saluran KemihDokumen18 halamanInfeksi Saluran KemihRETNO MUMPUNIBelum ada peringkat
- Infeksi Non Spesifik Saluran KemihDokumen51 halamanInfeksi Non Spesifik Saluran KemihSurya ArhBelum ada peringkat
- Askep IskDokumen12 halamanAskep IskDwi Abdul RohmanBelum ada peringkat
- Laporan Pendahuluan ISK (Infeksi Saluran Kemih)Dokumen12 halamanLaporan Pendahuluan ISK (Infeksi Saluran Kemih)Elsa Ridka IdaBelum ada peringkat
- Infeksi Saluran Kemih dengan Nyeri SuprapubikDokumen18 halamanInfeksi Saluran Kemih dengan Nyeri SuprapubikBeatrix Flora E SiregarBelum ada peringkat
- Asuhan Keperawatan Klien Dengan Infeksi Saluran KemihDokumen31 halamanAsuhan Keperawatan Klien Dengan Infeksi Saluran KemihidhaBelum ada peringkat
- ISK PANDUANDokumen5 halamanISK PANDUANTri Yudha NugrahaBelum ada peringkat
- Askep Infeksi Saluran KemihDokumen6 halamanAskep Infeksi Saluran KemihLee NandoBelum ada peringkat
- LP Medis Dan Keperawatan Infeksi Saluran KemihDokumen19 halamanLP Medis Dan Keperawatan Infeksi Saluran Kemihramlabugis533Belum ada peringkat
- Gangguan Berkemih Pada GeriatriDokumen14 halamanGangguan Berkemih Pada GeriatriAbdulrahman KhaledBelum ada peringkat
- ISKDokumen42 halamanISKrizky ramadhanBelum ada peringkat
- Isk 2018 PDFDokumen23 halamanIsk 2018 PDFMira RohimahBelum ada peringkat
- Abses Tuba OvariumDokumen20 halamanAbses Tuba OvariumResna MarvinzaBelum ada peringkat
- Referat ISK DR Soni, SpUDokumen30 halamanReferat ISK DR Soni, SpURiantyBelum ada peringkat
- Isk 2018Dokumen23 halamanIsk 2018nur chasanahBelum ada peringkat
- Infeksi Saluran Kemih MeilanyDokumen36 halamanInfeksi Saluran Kemih MeilanyFaqih SultonfaqBelum ada peringkat
- Pielonefritis AkutDokumen23 halamanPielonefritis AkutGabriel HezekiahBelum ada peringkat
- ASUHAN ISKDokumen11 halamanASUHAN ISKDona MaielaBelum ada peringkat
- ISK (Infeksi Saluran Kencing)Dokumen46 halamanISK (Infeksi Saluran Kencing)Samuel Amosilo KesekBelum ada peringkat
- Pielonefritis AkutDokumen35 halamanPielonefritis AkutMichelle AndreaBelum ada peringkat
- Mikrobiologi Perubatan I: Patogen dan Mikrobiologi ManusiaDari EverandMikrobiologi Perubatan I: Patogen dan Mikrobiologi ManusiaPenilaian: 2.5 dari 5 bintang2.5/5 (2)
- Mikrobiologi Medis I: Patogen dan Mikrobioma ManusiaDari EverandMikrobiologi Medis I: Patogen dan Mikrobioma ManusiaPenilaian: 4 dari 5 bintang4/5 (11)
- FROZEN SHOULDER PENANGANANDokumen5 halamanFROZEN SHOULDER PENANGANANNiken MaretaBelum ada peringkat
- Penyakit Arteri PeriferDokumen3 halamanPenyakit Arteri PeriferNiken MaretaBelum ada peringkat
- Kuliah TETANUSDokumen23 halamanKuliah TETANUSElya ViwsedBelum ada peringkat
- Hiperplasia Dan Hipertrofi GinggivaDokumen50 halamanHiperplasia Dan Hipertrofi GinggivaNiken MaretaBelum ada peringkat
- Ulkus KorneaDokumen18 halamanUlkus KorneaNiken MaretaBelum ada peringkat
- Anemia Dalam KehamilanDokumen18 halamanAnemia Dalam Kehamilanazkaaqlia21Belum ada peringkat
- F1 AnemiaDokumen6 halamanF1 AnemiaRezky Galuh SaputraBelum ada peringkat
- GoutDokumen13 halamanGoutNiken MaretaBelum ada peringkat
- Obat Golongan Opiat Pada AnestesiDokumen11 halamanObat Golongan Opiat Pada AnestesisardevBelum ada peringkat
- Batu Saluran KemihDokumen37 halamanBatu Saluran KemihNiken MaretaBelum ada peringkat
- ROP Bayi PrematurDokumen2 halamanROP Bayi PrematurNiken MaretaBelum ada peringkat
- HIPERTENSIDokumen23 halamanHIPERTENSINiken MaretaBelum ada peringkat
- BERADokumen16 halamanBERANiken MaretaBelum ada peringkat
- TINJAUAN PUSTAKA TUMOR MEDIASTINUMDokumen59 halamanTINJAUAN PUSTAKA TUMOR MEDIASTINUMNiken MaretaBelum ada peringkat
- Imejing Traktus UrinariusDokumen53 halamanImejing Traktus UrinariusNiken MaretaBelum ada peringkat
- MigrainDokumen26 halamanMigrainNiken MaretaBelum ada peringkat
- UPJO CASEDokumen46 halamanUPJO CASENiken MaretaBelum ada peringkat
- Laporan Jaga Interna, 26 OKT 2013Dokumen18 halamanLaporan Jaga Interna, 26 OKT 2013Niken MaretaBelum ada peringkat
- BERADokumen16 halamanBERANiken MaretaBelum ada peringkat
- Pemicu MigrenDokumen1 halamanPemicu MigrenNiken MaretaBelum ada peringkat
- Laporan Jaga Interna, 21 OKT 2013Dokumen16 halamanLaporan Jaga Interna, 21 OKT 2013Niken MaretaBelum ada peringkat
- KASUS RM Niken, Miftah, SupriDokumen13 halamanKASUS RM Niken, Miftah, SupriNiken MaretaBelum ada peringkat
- Leaflet DiareDokumen2 halamanLeaflet DiareNano Viand87% (15)
- Asi Eksklusif PDFDokumen60 halamanAsi Eksklusif PDFNurhasni FauzanBelum ada peringkat
- Abses Otak Otogenik Di RSMHDokumen19 halamanAbses Otak Otogenik Di RSMHSheikha Nabila MuzakkirBelum ada peringkat