Achilles Tendon Ruptures: Yanuarso, MD Indonesian Army Central Hospital
Diunggah oleh
Lim MichaelJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Achilles Tendon Ruptures: Yanuarso, MD Indonesian Army Central Hospital
Diunggah oleh
Lim MichaelHak Cipta:
Format Tersedia
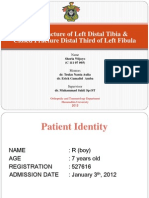
Achilles Tendon Ruptures
Yanuarso, MD Indonesian Army Central Hospital
Achilles: Hero of the Iliad
Led Greeks to conquer Troy Killed by arrow shot to heel Hippocrates this tendon if bruised or cut, causes the most acute fevers, induces choking, deranges the mind and at length brings death. Strongest tendon in the human body
Achilles Tendon
Formed by tendinous portion of gastrocnemius and soleus Plantaris lies medial and is distinct tendon Achilles progresses from round to flat as it travels distally to insert on calcaneal tuberosity Fibers of tendon rotate 90 degrees distally with medial fibers terminating posteriorly
Biochemistry
Collagen comprises 70% of tendon
95% type I Small amount of elastin
Collagen organized into fascicles surrounded by epitenon Ruptured tendon contains significant type III collagen
Blood Supply
Musculotendinous junction Surrounding connective tissue (paratenon) Bone-tendon junction Poor vascularization in midportion of tendon
Ref: Schmidt-Rolfing, Int. Orthop., 1992
Biomechanics
Peak force of 2233 newtons within achilles in vivo- Fukashiro 1995 Force builds just before heel strike, then released Force builds again and peaks at the end of push off Injury can be produced by asynchronous contraction of triceps surae
Epidemiology
Incidence 18 per 100,000 - Finland Most ruptures occur during sports (Badminton) More common in males in third and fourth decade of life Blood type O?
Etiology
Inflammatory and autoimmune conditions Collagen disorders Infectious disease Neurologic conditions Blood flow to tendon decreases with age Area prone to rupture relatively hypovascular
Etiology continued
Histologic evidence of collagen degeneration in all studies of patients with rupture Collagen degeneration occurs prior to rupture Alternating exercise with inactivity Accumulation of trauma leads to degeneration Corticosteroids injection into rabbit tendons showed necrosis and delayed healing. Several studies showed collagen damage with injected steroids Oral steroids also implicated
Fluoroquinolones and Tendon Rupture
Ciprofloxacin Direct deleterious effect on tenocytes Decreased transcription of Decorin which may modify architecture of tendon and alter mechanical properties
Bernard-Beaubois 1998
Mechanism of Rupture
Pushing off foot while extending knee- 53%
Jumping in basketball Volleyball
Sudden dorsiflexion of ankle- 17%
Fall down steps or into hole
Violent dorsiflexion of plantar flexed foot10%
Fall from height
Clinical Presentation
Sudden pain in affected limb Report being struck in back of leg Edema and bruising Palpable gap in tendon + Thompson test- 1962 Frequently missed!!
Imaging
Radiographs- usually not helpful unless avulsion of calcaneus Ultrasound used to assess gap in tendon and apposition of torn ends of tendon
Helpful with nonoperative tx
MRI useful in partial tears and tendinosis
Achilles Tendon Healing
Rabbit model Thermann et al Germany
Foot and Ankle July 2002
Nonoperative vs. operative
No difference within first week
Nonop tx showed aligned fibroblasts after 1 week At 12 weeks, nonop=op tx
High levels of type III collagen in healing tissue of ruptured tendons
Achilles Tendon Healing
Balb-C mice with ruptured achilles treated either with mobilization or immobilization More rapid restoration of load to failure in mobilized group 112 days mobilized group regained original tendon stiffness Mobilization lead to increased inflammatory cells at rupture site.
Palmes et al J of Orthopaedic Research 2002
Nonoperative Treatment
Cast immobilization 6-8 weeks Functional brace Use ultrasound to ensure tendon apposition Higher rerupture rate vs. operative repair Fewer overall complications
Surgical Treatment
First advocated by Pare 1575 1-2% deep infection rate Rerupture rate 2-8% Pajala et al JBJS 2002 409 patients, 5.6% rerupture rate
2.2% deep infection- Finlan
Surgical Repair vs. Casting
7.7% rerupture rate with cast vs. 3% with surgery AOFAS scores similar at 3.5 years post rupture. Greater calf atrophy with cast Fewer overall complications with nonoperative tx
Beskin et al Foot/Ankle December 2001
Complications of Surgical Treatment
Wound necrosis Wound infection Sural nerve injury DVT and PE Rerupture 2-5%
Percutaneous Achilles Repair
Developed by Ma and Griffith 1977 6 small incisions to pass sutures Faster return to normal strength than cast Sural nerve entrapment Higher rerupture rate vs. open repair
Percutaneous vs. Open Repair
Percutaneous
6.4% rerupture rate
Open repair
2.7% rerupture
Percutaneous does not reestablish length Injury to sural nerve Fewer wound complications with percutaneous tx
JBJS Br 1999
Chronic Ruptures
Use V-Y advancement if gap < 4cm Central turn down for larger gaps > 4cm Augmentation with FHL tendon Allografts?
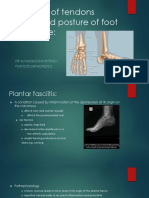
Achilles Tendonitis
Thickening and swelling of tendon May occur at insertion or midsubstance Often associated with tight gastroc Insidious onset
Achilles Tendonitis Treatment
Immobilization Physical therapy Heel lift NSAIDS PRP injection NO CORTISONE!
Operative vs. Nonoperative Treatment
Willits et al, JBJS Dec 2010 144 patients with achilles rupture Randomized to operative and nonoperative Fewer complications in nonoperative group Functional outcome no statistical difference
Summary
Functional outcome better with surgery and early motion Fewer complications with nonsurgical tx Rerupture rate
Surgery 2% Cast 8-10%
Future
Functional bracing Percutaneous repair
Postoperative Protocol
Non weight bearing x 4 weeks Cam walker brace x 6 weeks Active ROM exercises only No passive stretching for 8 weeks
Anda mungkin juga menyukai
- GDRC Distance Test 2Dokumen6 halamanGDRC Distance Test 2ravindraBelum ada peringkat
- Field Attachment Report FinalDokumen19 halamanField Attachment Report FinalAmaaca Diva100% (5)
- Ukite 08 AnswersDokumen77 halamanUkite 08 AnswersJipin Gopi100% (2)
- Columbian Exchange Graphic OrganizerDokumen2 halamanColumbian Exchange Graphic Organizerapi-327452561100% (1)
- Materials For The 21st Century PDFDokumen336 halamanMaterials For The 21st Century PDFanon_68148822100% (1)
- Achilles Tendon Ruptures Dr. YanuarsoDokumen56 halamanAchilles Tendon Ruptures Dr. Yanuarsofahmi aryandiBelum ada peringkat
- 5105 - Achilles TendonDokumen30 halaman5105 - Achilles Tendonalbertina tebayBelum ada peringkat
- Achilles TendonDokumen30 halamanAchilles TendonBetoBelum ada peringkat
- Achilles TendonDokumen30 halamanAchilles TendonMeldianaBelum ada peringkat
- Totalkneereplacementtkrppt 110208124132 Phpapp01Dokumen80 halamanTotalkneereplacementtkrppt 110208124132 Phpapp01Syeda MunazzaBelum ada peringkat
- Achilles Tendon RuptureDokumen6 halamanAchilles Tendon RuptureBn Wahyu AjiBelum ada peringkat
- Achilles Tendon Disorders: Daniel Penello Foot & Ankle RoundsDokumen29 halamanAchilles Tendon Disorders: Daniel Penello Foot & Ankle RoundsAulia RahmiBelum ada peringkat
- Achilles Tendon RuptureDokumen6 halamanAchilles Tendon RupturechloramphenicolBelum ada peringkat
- Achilles Tendon Disorders: Daniel Penello Foot & Ankle RoundsDokumen29 halamanAchilles Tendon Disorders: Daniel Penello Foot & Ankle RoundsWulan NeenBelum ada peringkat
- Kauwe 2017Dokumen15 halamanKauwe 2017Nurfitrianti ArfahBelum ada peringkat
- 1952 - Murphy - Musculotendinous Injuries in Sporting DogsDokumen5 halaman1952 - Murphy - Musculotendinous Injuries in Sporting DogsYaiza Garcia CasadoBelum ada peringkat
- Achilles Tendon RuptureDokumen4 halamanAchilles Tendon RuptureabinoBelum ada peringkat
- Closed Fractures of The Tibial Diaphysis: David L. Rothberg, MD Erik N. Kubiak, MDDokumen64 halamanClosed Fractures of The Tibial Diaphysis: David L. Rothberg, MD Erik N. Kubiak, MDtilahunthmBelum ada peringkat
- Musculoskeletal Disorders of Elbow, Wrist and HandsDokumen59 halamanMusculoskeletal Disorders of Elbow, Wrist and Handssaroj yadavBelum ada peringkat
- Joshis External Stabilisation System Jess For Recurrent Ctev Due To Irregular Follow Up PDFDokumen5 halamanJoshis External Stabilisation System Jess For Recurrent Ctev Due To Irregular Follow Up PDFshankarBelum ada peringkat
- Bagus PDFDokumen4 halamanBagus PDFAditya KrisnaBelum ada peringkat
- Paid Orthobullet MCQs - SpineDokumen236 halamanPaid Orthobullet MCQs - SpineShiKid COMIX-GAMEBelum ada peringkat
- Aaos 2010Dokumen220 halamanAaos 2010Yusufa ArdyBelum ada peringkat
- Jake PPDokumen31 halamanJake PPapi-323342594Belum ada peringkat
- Capps 9.18.07 W ExtraDokumen69 halamanCapps 9.18.07 W Extrasamuel.fang3434Belum ada peringkat
- Surgery Ortho - TaskDokumen4 halamanSurgery Ortho - TasknicewanBelum ada peringkat
- Tendinopathies: The Research and Evidence: Time To Abandon The "Tendinitis" MythDokumen73 halamanTendinopathies: The Research and Evidence: Time To Abandon The "Tendinitis" MythRajesh NandaBelum ada peringkat
- Aao2016 ReconDokumen163 halamanAao2016 ReconAnonymous 43mqs5pElf100% (6)
- Case Report (Ola)Dokumen44 halamanCase Report (Ola)amel015Belum ada peringkat
- Tuberculosis of Hip JointDokumen25 halamanTuberculosis of Hip JointYousra ShaikhBelum ada peringkat
- Oite 2006Dokumen823 halamanOite 2006dastroh100% (1)
- 45 Achilles Tendon Rupt 2018 Clinical Orthopaedic Rehabilitation A Team ADokumen5 halaman45 Achilles Tendon Rupt 2018 Clinical Orthopaedic Rehabilitation A Team AJessica HongBelum ada peringkat
- Tendon Disorders of Foot and Ankle (Autosaved) 2Dokumen74 halamanTendon Disorders of Foot and Ankle (Autosaved) 2Irfan Ahmad100% (1)
- DiGiovanni 2003 PDFDokumen8 halamanDiGiovanni 2003 PDFPhooi Yee LauBelum ada peringkat
- OU Shoulder and Elbow OITE Review: September 23, 2015 Betsy M. Nolan MDDokumen159 halamanOU Shoulder and Elbow OITE Review: September 23, 2015 Betsy M. Nolan MDJayBelum ada peringkat
- Ankle Instability: Dr. Syarif Hidayatullah, SP - OT, M.KesDokumen75 halamanAnkle Instability: Dr. Syarif Hidayatullah, SP - OT, M.Kesahmad zakyBelum ada peringkat
- Eliasson 2018Dokumen11 halamanEliasson 2018seriesediversosBelum ada peringkat
- Tuberculosis of The HipDokumen33 halamanTuberculosis of The Hipmuhammad bayu wicaksonoBelum ada peringkat
- Resurfacing For Perthes DiseaseDokumen6 halamanResurfacing For Perthes Diseaseyarimar hoyosBelum ada peringkat
- ARTHRITIS TB KNEE HIP BPTDokumen84 halamanARTHRITIS TB KNEE HIP BPTMiso100% (1)
- Orthobullets Foot and AnkleDokumen88 halamanOrthobullets Foot and AnkleStevent Richardo100% (1)
- 36 Knee Conditions: EMQ Answers 87Dokumen10 halaman36 Knee Conditions: EMQ Answers 87Eunice LimBelum ada peringkat
- Achilles Tendon InjuriesDokumen10 halamanAchilles Tendon InjurieshardboneBelum ada peringkat
- Shoulder ArthroplastyDokumen53 halamanShoulder ArthroplastyWijaya X PutriBelum ada peringkat
- Isthmic Spondylolisthesis: Anterior Vs Posterior FusionDokumen48 halamanIsthmic Spondylolisthesis: Anterior Vs Posterior FusionneareastspineBelum ada peringkat
- Aaos 2013Dokumen152 halamanAaos 2013Yusufa ArdyBelum ada peringkat
- Ankylosing Spondylitis (Marie-Strümpell Disease/ Bechterew's Disease)Dokumen39 halamanAnkylosing Spondylitis (Marie-Strümpell Disease/ Bechterew's Disease)MoineeBelum ada peringkat
- AAOS Foot Ankle 2018abDokumen54 halamanAAOS Foot Ankle 2018abFasa Roshada100% (3)
- Peroneus Longus Tendon Rupture: A Case Report: BackgroundDokumen14 halamanPeroneus Longus Tendon Rupture: A Case Report: BackgroundAlgivar DaudBelum ada peringkat
- Jor 20020Dokumen9 halamanJor 20020Adi PopoviciBelum ada peringkat
- AAOS2014 Shoulder and ElbowDokumen83 halamanAAOS2014 Shoulder and ElbowAmmar HilliBelum ada peringkat
- The Journal of Foot & Ankle SurgeryDokumen4 halamanThe Journal of Foot & Ankle SurgeryEma.diazBelum ada peringkat
- Cios 7 1Dokumen7 halamanCios 7 1Mokshit RaoBelum ada peringkat
- Achilles TendonDokumen24 halamanAchilles TendonRatu FaniaBelum ada peringkat
- SportsMedClin - 2015 - Cooper - Acute Achilles Tendon Ruptures - Does SX Offer Superior Resutls and Other Confusing IssuesDokumen12 halamanSportsMedClin - 2015 - Cooper - Acute Achilles Tendon Ruptures - Does SX Offer Superior Resutls and Other Confusing IssuesAnonymous kdBDppigEBelum ada peringkat
- Chronical Injuries ofDokumen45 halamanChronical Injuries ofapi-19916399Belum ada peringkat
- 2017 Article 9386 TendinitisDokumen9 halaman2017 Article 9386 TendinitisKirana lupitaBelum ada peringkat
- A Case of Eccrine Tumour Metastasis To Spine Managed With Posterior Spinal Stabilization With Recovering ParaparesisDokumen3 halamanA Case of Eccrine Tumour Metastasis To Spine Managed With Posterior Spinal Stabilization With Recovering ParaparesisInternational Journal of Innovative Science and Research TechnologyBelum ada peringkat
- Mobilising The Critically Ill, An Emerging ConceptDokumen27 halamanMobilising The Critically Ill, An Emerging ConceptRatsy MundluruBelum ada peringkat
- DR - O. K. A. SamuelsDokumen76 halamanDR - O. K. A. Samuelsgdudex118811Belum ada peringkat
- Distal Humeros PedDokumen55 halamanDistal Humeros PedSuad StambulieBelum ada peringkat
- Disorders of the Patellofemoral Joint: Diagnosis and ManagementDari EverandDisorders of the Patellofemoral Joint: Diagnosis and ManagementBelum ada peringkat
- Aged Garlic Extract and Coenzyme Q10 Have Favorable Effect On Inflammatory Markers and Coronary Atherosclerosis ProgressionDokumen9 halamanAged Garlic Extract and Coenzyme Q10 Have Favorable Effect On Inflammatory Markers and Coronary Atherosclerosis ProgressionLim MichaelBelum ada peringkat
- Bab 327 Iatrogenesis PDFDokumen2 halamanBab 327 Iatrogenesis PDFLim MichaelBelum ada peringkat
- Ticker Date/Time Percent Close Ticker Date/Time MA50Dokumen4 halamanTicker Date/Time Percent Close Ticker Date/Time MA50Lim MichaelBelum ada peringkat
- Bab 452 Metabolisme KalsiumDokumen2 halamanBab 452 Metabolisme KalsiumLim MichaelBelum ada peringkat
- Bab 444 Nodul TiroidDokumen6 halamanBab 444 Nodul TiroidLim MichaelBelum ada peringkat
- Bab 331 Elder MistreatmentDokumen3 halamanBab 331 Elder MistreatmentLim MichaelBelum ada peringkat
- Bab 444 Nodul TiroidDokumen6 halamanBab 444 Nodul TiroidLim MichaelBelum ada peringkat
- Bab 429 Asidosis LaktatDokumen3 halamanBab 429 Asidosis LaktatLim MichaelBelum ada peringkat
- Bab 379 Tumor JantungDokumen2 halamanBab 379 Tumor JantungLim MichaelBelum ada peringkat
- Bab 347 Gangguan Irama Jantung Yang Spesifik PDFDokumen5 halamanBab 347 Gangguan Irama Jantung Yang Spesifik PDFLim MichaelBelum ada peringkat
- Bab 370 Tatalaksana Infark Miokard Akut Tanpa Elevasi STDokumen6 halamanBab 370 Tatalaksana Infark Miokard Akut Tanpa Elevasi STLim MichaelBelum ada peringkat
- Bab 321 Penatalaksanaan Infeksi Pada Usia Lanjut PDFDokumen5 halamanBab 321 Penatalaksanaan Infeksi Pada Usia Lanjut PDFLim MichaelBelum ada peringkat
- Bab 313 Dizziness Dan SinkopDokumen2 halamanBab 313 Dizziness Dan SinkopLim MichaelBelum ada peringkat
- Bab 348 Fibrilasi AtrialDokumen5 halamanBab 348 Fibrilasi AtrialLim MichaelBelum ada peringkat
- Bab 314 Demensia PDFDokumen5 halamanBab 314 Demensia PDFLim MichaelBelum ada peringkat
- Bab 324 Kegawatdaruratan Pasien GeriatriDokumen2 halamanBab 324 Kegawatdaruratan Pasien GeriatriLim MichaelBelum ada peringkat
- Bab 321 Penatalaksanaan Infeksi Pada Usia Lanjut PDFDokumen5 halamanBab 321 Penatalaksanaan Infeksi Pada Usia Lanjut PDFLim MichaelBelum ada peringkat
- Bab 327 Iatrogenesis PDFDokumen2 halamanBab 327 Iatrogenesis PDFLim MichaelBelum ada peringkat
- Bab 328 Asuhan Pada Kondisi Terminal PDFDokumen2 halamanBab 328 Asuhan Pada Kondisi Terminal PDFLim MichaelBelum ada peringkat
- Bab 316 Penyakit ParkinsonDokumen5 halamanBab 316 Penyakit ParkinsonLim MichaelBelum ada peringkat
- Bab 391 Rabies PDFDokumen4 halamanBab 391 Rabies PDFakyafauzanBelum ada peringkat
- Bab 323 Pengkajian Paripurna Pada Pasien GeriatriDokumen5 halamanBab 323 Pengkajian Paripurna Pada Pasien GeriatriLim MichaelBelum ada peringkat
- Bab 387 Pemakaian Antimikroba Secara Rasional Di KlinikDokumen3 halamanBab 387 Pemakaian Antimikroba Secara Rasional Di KlinikFebe Rangga TambingBelum ada peringkat
- Bab 397 Infeksi NosokomialDokumen3 halamanBab 397 Infeksi NosokomialSyafril LubisBelum ada peringkat
- Kaki DiabetesDokumen4 halamanKaki Diabetesmu_crBelum ada peringkat
- Bab 394 KoleraDokumen4 halamanBab 394 KoleraSyafril LubisBelum ada peringkat
- Bab 429 Asidosis LaktatDokumen3 halamanBab 429 Asidosis LaktatLim MichaelBelum ada peringkat
- Bab 431 Retinopati DiabetikaDokumen4 halamanBab 431 Retinopati DiabetikaLim MichaelBelum ada peringkat
- Bab 438 Diabetes Melitus Pada Usia LanjutDokumen4 halamanBab 438 Diabetes Melitus Pada Usia LanjutLim MichaelBelum ada peringkat
- Bab 423 Farmakoterapi Pada Pengendalian Glikemia DMT2Dokumen4 halamanBab 423 Farmakoterapi Pada Pengendalian Glikemia DMT2Lim MichaelBelum ada peringkat
- MCQ ChoDokumen31 halamanMCQ Choامجد حسين جواد كاظمBelum ada peringkat
- AMORC Index Degrees 5 and 6Dokumen48 halamanAMORC Index Degrees 5 and 6Alois HaasBelum ada peringkat
- ABUUU (AutoRecovered)Dokumen14 halamanABUUU (AutoRecovered)Tariku TadesaBelum ada peringkat
- Kisi2 Inggris 11Dokumen3 halamanKisi2 Inggris 11siti RohimahBelum ada peringkat
- Asperger SyndromeDokumen4 halamanAsperger SyndromeJonald AlvaranBelum ada peringkat
- OMFC Application RequirementsDokumen1 halamanOMFC Application RequirementshakimBelum ada peringkat
- Case Presentation OF: Iron Deficiency AnemiaDokumen33 halamanCase Presentation OF: Iron Deficiency Anemiaitshurt_teardrops100% (1)
- 2016 PAD ACC+AHA SlidesDokumen74 halaman2016 PAD ACC+AHA SlidesPonpimol Odee BongkeawBelum ada peringkat
- Premio 20 DTDokumen35 halamanPremio 20 DThyakueBelum ada peringkat
- Essay ModelDokumen4 halamanEssay ModelEmma MalekBelum ada peringkat
- Cotton Varieties HybridsDokumen15 halamanCotton Varieties HybridsAjay KumarBelum ada peringkat
- CDC Org ChartDokumen1 halamanCDC Org Chartwelcome martinBelum ada peringkat
- Animal Protection Reiki PDFDokumen6 halamanAnimal Protection Reiki PDForlatan100% (1)
- Medication ErrorsDokumen15 halamanMedication ErrorsShubhangi Sanjay KadamBelum ada peringkat
- ChitnisDokumen1 halamanChitnisAkash Dhiman100% (1)
- Background: Abruptio PlacentaeDokumen6 halamanBackground: Abruptio PlacentaeEj ZGBelum ada peringkat
- 1.-Write The Verb in Brackets in Past Simple or Present PerfectDokumen1 halaman1.-Write The Verb in Brackets in Past Simple or Present PerfectLaura LBelum ada peringkat
- EsophagogastroduodenosDokumen34 halamanEsophagogastroduodenosAngela Beatriz Dela Vega100% (1)
- WHO International Standards For Drinking Water PDFDokumen204 halamanWHO International Standards For Drinking Water PDFAnonymous G6ceYCzwt100% (1)
- Bionic EyeDokumen6 halamanBionic EyeAsfia_Samreen_29630% (1)
- Armstrong 2017 Diabetic Foot Ulcers and Their RecurrenceDokumen11 halamanArmstrong 2017 Diabetic Foot Ulcers and Their Recurrencefebyan yohanesBelum ada peringkat
- DCA and Avemar A Theoretical Protocol FoDokumen33 halamanDCA and Avemar A Theoretical Protocol FosiesmannBelum ada peringkat
- Tet PGTRB Zoology Model Question Paper 2Dokumen14 halamanTet PGTRB Zoology Model Question Paper 2Subbarayudu mamillaBelum ada peringkat
- Nguyen 2019Dokumen6 halamanNguyen 2019ClintonBelum ada peringkat
- Choledo A4Dokumen53 halamanCholedo A4Czarina ManinangBelum ada peringkat
- Lesson 7 - Nervous, Endocrine, Reproductive, Urinary SystemDokumen37 halamanLesson 7 - Nervous, Endocrine, Reproductive, Urinary SystemAlejandro GuerreroBelum ada peringkat