Integumentary System: By: Kelieraine U. Bon
Diunggah oleh
Irish Jane Bayle Cubillo0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
93 tayangan48 halamanburns
Judul Asli
Burns
Hak Cipta
© © All Rights Reserved
Format Tersedia
PPTX, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen Iniburns
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PPTX, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
93 tayangan48 halamanIntegumentary System: By: Kelieraine U. Bon
Diunggah oleh
Irish Jane Bayle Cubilloburns
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PPTX, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 48
INTEGUMENTARY SYSTEM
By: Kelieraine U. Bon
ANATOMY AND PHYSIOLOGY
The integument is an organ, and is an
alternative name for skin.
Includes the skin and the skin
derivatives hair, nails, and glands.
The bodys largest organ and accounts
for 15% of body weight
THREE LAYERS:
Epidermis
is the thinner and more superficial layer of
the skin
The epidermis is made up of 4 cell types:
(A) Keratinocytes
(B) Melanocytes
(C) Langerhan Cells
(D) Merkel cells
Dermis
the deeper, thicker layer composed of
connective tissue, blood vessels, nerves,
glands and hair follicles
Hypodermis
subcutaneous
Adipose tissue which provides a
cushion between the skin layers,
muscles, and bones
FUNCTION:
Thermoregulation
Cutaneous sensation
Vitamin D production
Protection
Absorption & secretion
Wound healing
DEFINITION:
Burns are injuries to tissues
caused by heat, friction, electricity,
radiation, or chemicals.
Scalds from hot liquids and steam,
building fires and flammable
liquids and gases are the most
common causes of burns.
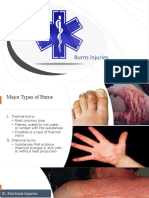
TYPES OF BURNS:
1.) Heat burns (thermal burns) are
caused by fire, steam, hot objects, or
hot liquids. Scald burns from hot
liquids are the most common burns to
children and older adults.
2.) Cold temperature burns are caused
by skin exposure to wet, windy, or cold
conditions.
3.) Electrical burns are caused by contact
with electrical sources or by lightning.
4.) Chemical burns are caused by contact
with household or industrial chemicals in
a liquid, solid, or gas form. Natural foods
such as chili peppers, which contain a
substance irritating to the skin, can cause
a burning sensation.
5.) Radiation burns are caused by the sun,
tanning booths, sunlamps, X-rays, or
radiation therapy for cancer treatment.
6.) Friction burns are caused by contact
with any hard surface such as roads
("road rash"), carpets, or gym floor
surfaces. They are usually both a
scrape (abrasion) and a heat burn.
HEAT BURN
COLD TEMPERATURE BURN
MANAGEMENT
Be sure to warm the whole body with blankets
as well as the cold injured parts.
Stay calm, find shelter, change to dry clothes,
keep moving, and drink warm fluids to prevent
further heat loss and slowly rewarm yourself.
If small areas of your body (ears, face, nose,
fingers, toes) are really cold or frozen,
try home treatment first aid to warm these
areas and prevent further injury to skin.
Warm small areas by blowing warm air on
them, tucking them inside your clothing, or
putting them in warm water.
MEDICINE:
Acetaminophen, such as Tylenol
Nonsteroidal anti-inflammatory drugs
(NSAIDs):
Ibuprofen, such as Advil or Motrin
Naproxen, such as Aleve or Naprosyn
Aspirin (also a nonsteroidal anti-
inflammatory drug), such as Bayer or
Bufferin
ELECTRICAL BURN
CHEMICAL BURN
MANAGEMENT
Prevent contaminated irrigation solution
from running onto unaffected skin.
Remove contaminated clothes.
Special situations:
-If contamination with metallic lithium,
sodium, potassium, or magnesium has
occurred, irrigation with water can result
in a chemical reaction that causes burns
to worsen. In these situations, the area
should be covered with mineral oil and the
metallic pieces should be removed with
forceps and placed in mineral oil. If forceps
are not available, soak the area with
mineral oil and cover it with gauze soaked
in mineral oil.
If contamination with white phosphorus
has occurred, thoroughly irrigate the
area with water then cover the area
with water-soaked gauze. Keep the area
moist at all times. The area can also be
covered with petroleum jelly.
If eye exposures have not been
irrigated, then this should be started
immediately. Immediate removal of
caustic substances in the eye is critical.
RADIATION BURNS
FRICTION BURNS
PHASE DURATION PRIORITIES
Emergent or
Immediate
Resuscitative
- From onset of injury to
completion
of fluid resuscitation
First aid
Prevention of shock
Prevention of
respiratory distress
Detection and
treatment of concomitant
injuries
Wound assessment and
initial care
Acute
- From beginning of
diuresis to near
completion of wound
closure
Wound care and
closure
Prevention or treatment
of complications,
including infection
Nutritional support
Rehabilitation
- From major wound
closure to return
to individuals optimal
level of physical
and psychosocial
adjustment
Prevention of scars and
contractures
Physical, occupational,
and vocational
rehabilitation
Functional and
cosmetic reconstruction
Psychosocial
counseling
EMERGENT/RESUSCITATIVE PHASE:
Cool the wound
Establish airway
Supply oxygen
Insert at least 1 large bore IV line
Assess pulse
Monitor blood pressure
Extinguish the flames
Remove restrictive objects
Cover the wound
Irrigate chemical burn
ACUTE OR INTERMEDIATE PHASE
Infection prevention
Wound cleaning
Wound dressing
Wound debridement
*Grafting
Autograft
Homograft
Heterograft
MANAGEMENT:
Circulation
The nurse assesses the graft area for
signs of adequate blood supply. She
inspects the color of the graft area,
which should be the same color as the
other skin on the patients body to see if
it has enough blood supply. The nurse
also checks to make sure the graft area
is warm as this indicates sufficient
blood supply to the area.
Drainage
The nurse checks the patency of drains
placed in the graft area. She makes
sure they are not blocked, so drainage
can flow out of the graft site instead of
accumulating in it and potentially
causing an infection.
Positioning
The nurse ensures blood circulation to
the graft area by positioning the patient
off the graft. Taking pressure off the
graft and skin surrounding it reduces
the risk of decreased blood supply to
the area.
Low Pressure
The nurse may place the patient on a
low pressure bed when lying down or
low pressure cushion for sitting down.
The less pressure exerted on the graft
area, the more likely that it will be
adequately perfused. Low pressure beds
and cushions exert low pressure on the
skin.
COMPLICATIONS:
Failure of the skin graft is often due to:
Inadequate excision of the wound bed.
Inadequate vascular supply to the
wound bed.
Hematomas and seromas. These form
a barrier between the bed and skin graft
and prevent the graft from taking.
Shearing or displacement of the
graft. This prevents revascularisation of
the graft as the capillaries cannot link
up.
Infection. This can lead to disintegration of
the graft or excessive exudate that prevents
the graft from adhering to the bed (Beldon,
2003).
Late complications relate to the appearance
and function of the graft. The colour and
texture of a healed graft will contrast with the
surrounding skin and, usually, there is some
depression of the wound. Hyperpigmentation
of the graft can also be a problem (Young and
Fowler, 1998).
Contraction is the main functional problem
and can result in joint contracture and
restriction of function in the surrounding
tissue.
CLASSIFICATION OF BURNS
First-Degree
(Minor)
The burned area is painful. The
outer skin is
reddened. Slight swelling is
present.
Second-Degree
(Moderate)
The burned area is painful. The
underskin is affected.
Blisters may form. The area may
have a wet, shiny
appearance because of exposed
tissue.
Third-Degree
(Critical)
The burned area is insensitive
due to the destruction
of nerve endings. Skin is
destroyed. Muscle tissues
and bone underneath may be
damaged. The area
may be charred, white, or
grayish in color.
RULE OF NINES
A method for rapidly assessing
the extent of burns on the skin
surface, which determines the
amount of fluid required as
replacement therapy
LUND AND BROWDER METHOD
- a method for estimating the
extent of burns that allows for the
varying proportion of body
surface in persons of different
ages.
RULE OF PALM
Quick prehospital assessment used to
estimate the extent of burns.
The patients palm not including the
surface area of the digits, is
approximately 1% of the TBSA.
The patients palm without the fingers
is equivalent to 0.5% TBSA and serves
aas a general measurement for all age
groups.
FLUID REPLACEMENT:
Formula:
2-4ml x kg body weight x % TBSA
burned
Half to be given in first 8 hours
remaining half to be given over next 16
hours
LOCAL AND SYSTEMIC
RESPONSES TO BURNS
Hypovolemia
Burn edema
Pulmonary injuries
Altered renal function
Altered immunologic defenses
EFFECTS ON FLUIDS AND
ELECTROLYTES
Results to:
Hyponatremia
Hyperkalemia
Anemia
MANAGEMENT FOR MINOR
BURNS
Cool the burn
Cover the burn with a sterile
gauze bandage
Take an over-the-counter pain
reliever
CAUTION:
Don't use ice.
Don't apply egg whites, butter or
ointments to the burn.
Don't break blisters.
FOR MAJOR BURNS:
Don't remove burned clothing.
Don't immerse large severe burns
in cold water.
Check for signs of circulation
(breathing, coughing or
movement).
Elevate the burned body part or
parts.
Cover the area of the burn.
MEDICAL MANAGEMENT:
Transfer to a burn center.
Manage fluid loss and shock.
Fluid replacement therapy.
NURSING MANAGEMENT:
Assess the patients burn injury.
Aseptic management of the burn
wounds.
Monitor vital signs.
Inserting of indwelling urinary
catheter.
Administering and monitoring
intravenous therapy.
Neurologic assessment
COMPLICATIONS OF BURNS
Shock
Heart attack
Formation of scars
Anda mungkin juga menyukai
- Burns: College of NursingDokumen12 halamanBurns: College of NursingAyr Masenas100% (1)
- Burns 2Dokumen4 halamanBurns 2Charmae NaveaBelum ada peringkat
- Integumentary SystemDokumen16 halamanIntegumentary Systemshenric16100% (8)
- Burns InjuriesDokumen24 halamanBurns InjuriesRama SultanBelum ada peringkat
- Managing Burns SafelyDokumen30 halamanManaging Burns SafelyMamata BeheraBelum ada peringkat
- burnsDokumen26 halamanburnsgemergencycareBelum ada peringkat
- Burns Are Most Common Household InjuriesDokumen28 halamanBurns Are Most Common Household InjuriesSonu MishraBelum ada peringkat
- Burn InjuryDokumen80 halamanBurn InjuryQueena Neysa CalcarinaBelum ada peringkat
- Burns 2Dokumen34 halamanBurns 2Vaibhavi JainBelum ada peringkat
- Paediatric Burns FinalizedDokumen28 halamanPaediatric Burns FinalizedKarthick UnleashBelum ada peringkat
- Burn Injury Case Study: Understanding Causes, Degrees and TreatmentDokumen21 halamanBurn Injury Case Study: Understanding Causes, Degrees and TreatmentPOTENCIANA MAROMABelum ada peringkat
- AAAAAAAAAAAADokumen21 halamanAAAAAAAAAAAAM sajjad HaiderBelum ada peringkat
- BurnDokumen33 halamanBurnAbdul MajidBelum ada peringkat
- Acute Biologic Crisis - Hand OutDokumen48 halamanAcute Biologic Crisis - Hand OutLouis Carlos RoderosBelum ada peringkat
- Burn InjuriesDokumen30 halamanBurn InjuriesIndra PrasetyaBelum ada peringkat
- Management and Treatment of Burn WoundDokumen5 halamanManagement and Treatment of Burn WoundTaqi MehdiBelum ada peringkat
- Burn ManagementDokumen7 halamanBurn ManagementnrhmhealthBelum ada peringkat
- BurnsDokumen37 halamanBurnskint100% (2)
- Management of Burn PDFDokumen5 halamanManagement of Burn PDFaditiBelum ada peringkat
- BurnsDokumen9 halamanBurnsVincentus BinBelum ada peringkat
- Pathophysiology of Burns: Dr. Shiara Ortiz-Pujols Burn Fellow NC Jaycee Burn CenterDokumen75 halamanPathophysiology of Burns: Dr. Shiara Ortiz-Pujols Burn Fellow NC Jaycee Burn CenterJohnBedaLatawanMalecdanBelum ada peringkat
- Care Burn PatientsDokumen10 halamanCare Burn PatientsHILLARY JOY ACOSTABelum ada peringkat
- S M D U: KIN Anagement Ecubitis LcerDokumen77 halamanS M D U: KIN Anagement Ecubitis LcerabidBelum ada peringkat
- Primary Care of BurnsDokumen20 halamanPrimary Care of BurnsNatalie AlcântaraBelum ada peringkat
- Trauma and Emergecny Nursing: Course TittleDokumen64 halamanTrauma and Emergecny Nursing: Course TittleAbdisamed AllaaleBelum ada peringkat
- Burns & Burn Management, Asphyxiation, and Head InjuriesDokumen77 halamanBurns & Burn Management, Asphyxiation, and Head InjuriesGabz GabbyBelum ada peringkat
- Pamantasan NG Lungsod NG Maynila: (University of The City of Manila)Dokumen23 halamanPamantasan NG Lungsod NG Maynila: (University of The City of Manila)Em Hernandez AranaBelum ada peringkat
- First Aid for Burns GuideDokumen21 halamanFirst Aid for Burns Guidegashbin MahdyBelum ada peringkat
- By: Aileen C. Contreras-Limjoco M.DDokumen48 halamanBy: Aileen C. Contreras-Limjoco M.Dclara jocomilBelum ada peringkat
- Burns: Dr. Iye D. Otigba-KolawoleDokumen37 halamanBurns: Dr. Iye D. Otigba-KolawoleMaryBelum ada peringkat
- RU BurnsDokumen18 halamanRU BurnsDanah CandelarioBelum ada peringkat
- Burns DebridementDokumen27 halamanBurns DebridementNisha FatmaBelum ada peringkat
- BurnsDokumen13 halamanBurnsmsah820Belum ada peringkat
- Burn Injury M3Dokumen71 halamanBurn Injury M3CechanBelum ada peringkat
- Treatment Procedures For EachDokumen10 halamanTreatment Procedures For EachJovel WeirBelum ada peringkat
- BurnsDokumen24 halamanBurnsMutaz MandilBelum ada peringkat
- BURNS: A GUIDE TO CLASSIFICATION, PATHOPHYSIOLOGY AND MANAGEMENTDokumen35 halamanBURNS: A GUIDE TO CLASSIFICATION, PATHOPHYSIOLOGY AND MANAGEMENTMariam AntonyBelum ada peringkat
- Thermal Injuries Treatment and ManagementDokumen43 halamanThermal Injuries Treatment and ManagementSuyanto TonyBelum ada peringkat
- Interventions For ClientsDokumen68 halamanInterventions For ClientsRinkish DalliahBelum ada peringkat
- Wa0000.Dokumen48 halamanWa0000.Rajendra MaherBelum ada peringkat
- BurnDokumen7 halamanBurnpatlekhilesh8Belum ada peringkat
- Burn-Medical and Surgical ManagementDokumen6 halamanBurn-Medical and Surgical ManagementCristina L. JaysonBelum ada peringkat
- Burns Management PDFDokumen7 halamanBurns Management PDFRoh Bungaria N Garingging100% (1)
- King Saud University College of NursingDokumen49 halamanKing Saud University College of Nursinghatem alsrour100% (2)
- Wound CareDokumen7 halamanWound CareAbogadie Dione Blas ReyBelum ada peringkat
- Burns: ABC of Wound HealingDokumen4 halamanBurns: ABC of Wound HealingRicardoGamalielBelum ada peringkat
- BurnsDokumen58 halamanBurnsMarie MayBelum ada peringkat
- Skin IntegrityDokumen112 halamanSkin IntegrityHerlina NababanBelum ada peringkat
- Burn management guideDokumen36 halamanBurn management guideAshok SabalBelum ada peringkat
- Introduction To BurnsDokumen47 halamanIntroduction To BurnsanushavergheseBelum ada peringkat
- Pressure Ulcers: Francisco Torres Lozada MD Ponce Health Sciences University GeriatricsDokumen67 halamanPressure Ulcers: Francisco Torres Lozada MD Ponce Health Sciences University GeriatricsStephanie RiveraBelum ada peringkat
- Care of The Burn Patient JafDokumen99 halamanCare of The Burn Patient JafPaige Fox100% (1)
- Burns: Ashkay Anita Collins KennieDokumen28 halamanBurns: Ashkay Anita Collins KennierohitBelum ada peringkat
- Añosa Caballo - First Aid For Burns HandoutDokumen21 halamanAñosa Caballo - First Aid For Burns HandoutMa. Ferimi Gleam BajadoBelum ada peringkat
- Wound CareDokumen5 halamanWound CareEdgar Garcia100% (1)
- Pressure Ulcer Prevention and TreatmentDokumen51 halamanPressure Ulcer Prevention and TreatmentIosefina DudeanuBelum ada peringkat
- BurnsDokumen55 halamanBurnsMohammad Amjad KhanBelum ada peringkat
- NELEC1 ProjectDokumen14 halamanNELEC1 ProjectRoxas CedrickBelum ada peringkat
- SpiritualityDokumen3 halamanSpiritualityIrish Jane Bayle CubilloBelum ada peringkat
- Entamoeba HistolyticaDokumen6 halamanEntamoeba HistolyticaIrish Jane Bayle CubilloBelum ada peringkat
- Strengthening SpiritualityDokumen11 halamanStrengthening SpiritualityIrish Jane Bayle CubilloBelum ada peringkat
- Nightingale's Environmental Theory and Henderson's 14 ActivitiesDokumen50 halamanNightingale's Environmental Theory and Henderson's 14 ActivitiesIrish Jane Bayle Cubillo80% (5)
- Revise Ros, Pe & PathoDokumen8 halamanRevise Ros, Pe & PathoIrish Jane Bayle CubilloBelum ada peringkat
- Chole CaseDokumen35 halamanChole CaseIrish Jane Bayle CubilloBelum ada peringkat
- Case Study on Dementia: Physical Examination FindingsDokumen47 halamanCase Study on Dementia: Physical Examination FindingsIrish Jane Bayle CubilloBelum ada peringkat
- CHNDokumen1 halamanCHNIrish Jane Bayle CubilloBelum ada peringkat
- Patient AnalysisDokumen6 halamanPatient AnalysisIrish Jane Bayle CubilloBelum ada peringkat
- Postpartum Complications ExplainedDokumen10 halamanPostpartum Complications ExplainedIrish Jane Bayle CubilloBelum ada peringkat
- Project in Microbiolog Y: Submitted To: Yolanda Ilagan Ph. D Submitted By: Irish Jane B. Cubillo BSN 2-2Dokumen28 halamanProject in Microbiolog Y: Submitted To: Yolanda Ilagan Ph. D Submitted By: Irish Jane B. Cubillo BSN 2-2Irish Jane Bayle CubilloBelum ada peringkat
- Postpartal Pueperal InfectionDokumen38 halamanPostpartal Pueperal InfectionIrish Jane Bayle CubilloBelum ada peringkat
- Healthy Horizons-Butler University Ambulatory Care Appe Rotation SyllabusDokumen13 halamanHealthy Horizons-Butler University Ambulatory Care Appe Rotation Syllabusapi-316593964Belum ada peringkat
- ID Kajian Hukum Perjanjian Perkawinan Di Kalangan Wni Islam Studi Di Kota Medan PDFDokumen17 halamanID Kajian Hukum Perjanjian Perkawinan Di Kalangan Wni Islam Studi Di Kota Medan PDFsabila azilaBelum ada peringkat
- Vastu Colors (Room by Room Home Coloring Guide)Dokumen25 halamanVastu Colors (Room by Room Home Coloring Guide)yuva razBelum ada peringkat
- B1 Mod 01 MathsDokumen152 halamanB1 Mod 01 MathsTharrmaselan VmanimaranBelum ada peringkat
- ENG01P001S02U00Dokumen14 halamanENG01P001S02U00arghasen2014100% (1)
- Nokia CaseDokumen28 halamanNokia CaseErykah Faith PerezBelum ada peringkat
- Love Against All Odds: Summary of The Wedding DanceDokumen2 halamanLove Against All Odds: Summary of The Wedding DanceLYumang, Annika Joy D.Belum ada peringkat
- Reflection Paper - InternshipDokumen7 halamanReflection Paper - Internshipapi-549362324Belum ada peringkat
- Chapter 3 - Risk and ReturnDokumen67 halamanChapter 3 - Risk and ReturnPhuonganh LeBelum ada peringkat
- Epd-Lca Meranti Plywood-Final ReportDokumen29 halamanEpd-Lca Meranti Plywood-Final ReporttangBelum ada peringkat
- Meena ResumeDokumen3 halamanMeena ResumeAnonymous oEzGNEBelum ada peringkat
- Two Sides of Effective Oral CommunicationDokumen17 halamanTwo Sides of Effective Oral CommunicationSharath KumarBelum ada peringkat
- United States v. Calvin Antonio Spencer, 68 F.3d 462, 4th Cir. (1995)Dokumen4 halamanUnited States v. Calvin Antonio Spencer, 68 F.3d 462, 4th Cir. (1995)Scribd Government DocsBelum ada peringkat
- Case - 1 Marketing and Distribution of MushroomDokumen2 halamanCase - 1 Marketing and Distribution of MushroomKetan BohraBelum ada peringkat
- Wild (E) Men and SavagesDokumen237 halamanWild (E) Men and SavagesAhmed DiaaBelum ada peringkat
- About Nysc Ict CD in Imo StateDokumen9 halamanAbout Nysc Ict CD in Imo StateIsoft PexBelum ada peringkat
- VV Siddipet Merit ListDokumen81 halamanVV Siddipet Merit ListSubashBelum ada peringkat
- Template For An Effective Statement of InterestDokumen3 halamanTemplate For An Effective Statement of InterestbabananakBelum ada peringkat
- Life Strategy 101: How To Live Live by Vision, Work With Purpose, and Achieve More SuccessDokumen31 halamanLife Strategy 101: How To Live Live by Vision, Work With Purpose, and Achieve More SuccessMichelle Casto100% (2)
- Casalla vs. PeopleDokumen2 halamanCasalla vs. PeopleJoan Eunise FernandezBelum ada peringkat
- What Is Six Sigma: Everything You Need To Know About It: by Pankaj KumarDokumen16 halamanWhat Is Six Sigma: Everything You Need To Know About It: by Pankaj KumarSuman DewanBelum ada peringkat
- Kinematic Viscosity, Units & DimensionDokumen7 halamanKinematic Viscosity, Units & DimensionPrithwish Kr SutradharBelum ada peringkat
- English 7 1st Lesson Plan For 2nd QuarterDokumen4 halamanEnglish 7 1st Lesson Plan For 2nd QuarterDiane LeonesBelum ada peringkat
- Reduction of Salivary Streptococcus Mutans Colonies in Children After Rinsing With 2.5% Green Tea SolutionDokumen6 halamanReduction of Salivary Streptococcus Mutans Colonies in Children After Rinsing With 2.5% Green Tea SolutionSistia DefariBelum ada peringkat
- Christoffel Symbols: PHYS 471: Introduction To Relativity and CosmologyDokumen9 halamanChristoffel Symbols: PHYS 471: Introduction To Relativity and Cosmologyarileo3100% (1)
- LAB 2 SimulationDokumen6 halamanLAB 2 SimulationArti Stic100% (1)
- Case Study Analysis of Six Sigma Implementation Inservice OrganisationsDokumen30 halamanCase Study Analysis of Six Sigma Implementation Inservice OrganisationsMohammed AwolBelum ada peringkat
- Corruption PDFDokumen11 halamanCorruption PDFkaleemullahBelum ada peringkat
- Khulafa-al-Rashidun, UmarDokumen9 halamanKhulafa-al-Rashidun, UmarDuha QureshiBelum ada peringkat
- SRDF S LabDokumen9 halamanSRDF S LabUma SekharBelum ada peringkat