Pharm Review
Diunggah oleh
Peter GrossmanHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Pharm Review
Diunggah oleh
Peter GrossmanHak Cipta:
Format Tersedia
HIGH YIELD
PHARMACOLOGY
ANS PHARMACOLOGY
PARASYMPATHETIC DIVISION = rest and
digest
Decreased heart rate
Bronchioles constrict
Increased motility and secretion in the digestive tract
Increased secretion from the salivary glands, pancreas
Sweating
Release of urine
AUTONOMIC NERVOUS SYSTEM
SYMPATHETIC DIVISION = fight or flight
Increased heart rate
Blood vessels to the heart and the extremities dilate
Liver produces glucose to provide energy for muscle contraction
Bronchioles dilate
Pupils dilate
Urinary retention
AUTONOMIC NERVOUS SYSTEM
NICOTI NI C RECEPTORS
Found in autonomic ganglia of the PNS and the SNS
Ligand-gated Na+/K+ channels
Activated by nicotine and ACh
MUSCARI NI C RECEPTORS
Found in neuromuscular junctions
G protein-coupled receptors that act through 2
nd
messengers
5 subtypes: M1, M2, M3, M4, M5
Activated by muscarine and ACh
CHOLINESTERASE INHIBI TORS are i ndi rect agoni sts
End in -stignine
BOTULINUM TOXIN prevents rel ease of neurotransmi tter at al l
chol i nergi c termi nal s
ACETYLCHOLINE RECEPTORS
ATROPINE (from Atropa bel l adonna)
Increased heart rate
Increased conduction velocity through the AV node
Bronchodilation
Increased body temperature (decreased sweating)
Bl ockage i s reversible i . e. can be overcome by a l arger
concentration of acetylcholine or muscari nic agoni st
MUSCARINIC RECEPTOR BLOCKERS
ALPHA RECEPTORS
ALPHA RECEPTORS
1 (heart and ki dney)
Increase intracellular cAMP
Increased heart rate and contractility
Increased renin release
Increased lipolysis
2 (respiratory and vascular smooth muscl e)
Increase intracellular cAMP
Vasodilation
Bronchodilation (hormonal epinephrine)
Increased heart rate and contractility
Increased lipolysis
Increased insulin release
ADRENERGIC RECEPTORS
ADRENERGIC AGONISTS
EFFECTS OF ADRENERGIC AGONISTS
DIRECT SYMPATHOMIMETICS
Increase the release of
stored catecholamines
Amphetamine
Block reuptake of
catecholamines
Duloxetine, cocaine
Block the enzymatic
breakdown of
norepinephrine
MAO and COMT inhibitors
INDIRECT SYMPATHOMIMETICS
CARDIAC
PHARMACOLOGY
CARDIAC FAILURE
Cardiac glycosides
Sympathomimetics
Phosphodiesterase-3
inhibitors
Vasoconstrictors
HYPERTENSION
Diuretics
Vasoconstrictors
Sympatholytics
ARRHYTHMIAS
Class I: Fast Na+
channel blockers
Class II: Beta blockers
Class III: K+ channel
blockers
Class IV: L-type Ca2+
channel blockers
Adenosine
OVERVIEW
At a given left
ventricular end-
diastolic pressure,
cardiac output is lower
than in a normal heart
Diuretics reduce LVEDP
Inotropic drugs shift the
curve upward, toward
normal
HEART FAILURE
Inhibits sodium-
potassium ATPase, which
increases intracellular
Ca2+ and force of
contraction
Increases vagal tone
Decreases heart rate
Decreases conduction
velocity at the AV node
Increases refractory period
Toxic effects = sinus
bradycardia and SA block
CARDIAC GLYCOSIDES (DIGITALIS)
ELECTRICAL EFFECTS OF DIGITALIS
Delayed afterdepolarizations
may develop resulting in
triggered tachyarrhythmias
1. DIURETICS: decrease sodi um retention and bl ood vol ume
1. VASODILATORS: rel ax vascular smooth muscl e i n resi stance
vessels
1. ACE INHIBITORS: reduce peri pheral vascular resi stance and
bl ood vol ume
2. SYMPATHOLYTICS: reduce peripheral vascular resi stance and
cardi ac output
ANTIHYPERTENSIVES
DIURETICS
ACE i nhi bitors i nhi bit the production of angi otensin II from
angi otensi n I
Counteract the ef fects of reni n- angiotensin system wi thout
refl ex sympathetic acti vation
Lower bl ood pressure pri nci pally by decreasi ng peri pheral
vascular resi stance
Tx l ong- term treatment of congestive heart fai l ure, post -
myocardial i nfarcti on, and hypertension
ACE INHIBITORS (-PRILS)
RENIN-ANGTIOTENSIN SYSTEM
Vasodilator of both
arterioles and vei ns
Can cause decreased cardiac
output
Administered i ntravenously
to treat hypertensi ve
emergencies
NO causes vasodilation
through acti vation of
guanylate cycl ase i n
vascular smooth muscl e
Of ten admi nistered wi th a
- bl ocker
NITROPRUSSIDE
GOAL = SNS
PHOSPHODIESTERASE-3 INHIBITORS
Milrinone
Mechani sms of arrhythmia
Increased automaticity of pacemaker or nonpacemaker cells
Reentrant pathways
Triggered activity
Goal of anti arrhythmia drugs:
ANTIARRHYTHMIA DRUGS
CLASS IA: moderate bl ock
phase 0 upstroke rate; prolonged AP duration
Quinidine
CLASS IB: mi l d bl ock
phase 0 upstroke rate; shortened AP duration
Lidocaine
CLASS IC: marked bl ock
phase 0 upstroke rate; no change in AP duration
Flecainide
CLASS I : BLOCK FAST NA+ CHANNELS
CLASS II: -BLOCKERS (-OLOLS)
CLASS III: BLOCK K+ CHANNELS
(TILIDES)
CLASS IV: BLOCK L-TYPE CALCIUM
CHANNELS
Verapamil
Diltiazem
ADENOSINE
Administered intravenously, adenosine is the most effective drug
for the rapid termination of reentrant SVT, such as AV nodal
reentrant tachycardia.
RESPIRATORY
PHARMACOLOGY
ASTHMA
Characterized by acute episodes of bronchoconstriction caused by
underlying air-way inflammation
Leukotrienes and histamine induce smooth muscle contraction,
mucus secretion, and recruitment of inflammatory cells
CHRONIC BRONCHITIS
Pulmonary obstruction caused by excessive production of mucus due
to hyperactivity of mucus-secreting goblet cells
RHINITIS
Decrease in nasal airways due to thickening of the mucosa and
increased mucus secretion
GLUCOCORTICOIDS
LEUKOTRIENE INHIBITORS
MAST CELL STABILIZERS
ANTI-INFLAMMATORY DRUGS
Anda mungkin juga menyukai
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Phctlec - Topic 3&4 - PrelimsDokumen24 halamanPhctlec - Topic 3&4 - PrelimsasdfdjfeonaBelum ada peringkat
- MJR 30 1 1Dokumen2 halamanMJR 30 1 1landoo oooBelum ada peringkat
- Peripheral Vascular DiseaseDokumen17 halamanPeripheral Vascular DiseaseJee Ho SohnBelum ada peringkat
- Autoregulation of The Cardiovascular SystemDokumen15 halamanAutoregulation of The Cardiovascular SystemErinne DefrianiBelum ada peringkat
- Optimize Your Diet With Walter Willett MD DRPH SlidesDokumen59 halamanOptimize Your Diet With Walter Willett MD DRPH SlidesPooja TBelum ada peringkat
- Journal ClubDokumen28 halamanJournal Clubapi-355090691Belum ada peringkat
- Type 2 Diabetes: Aace Comprehensive Management AlgorithmDokumen10 halamanType 2 Diabetes: Aace Comprehensive Management AlgorithmDiana YaeliBelum ada peringkat
- Hadzic - Ch22 - Neuraxial AnatomyDokumen11 halamanHadzic - Ch22 - Neuraxial AnatomyGulsahBelum ada peringkat
- Anatomy, Lecture 6, Pericardium and The Heart (Slides)Dokumen22 halamanAnatomy, Lecture 6, Pericardium and The Heart (Slides)Ali Al-Qudsi100% (1)
- MyopathyDokumen47 halamanMyopathySOUMYADEEP BHUINYABelum ada peringkat
- Lipid Lowering Drugs True-1Dokumen51 halamanLipid Lowering Drugs True-1wissam salimBelum ada peringkat
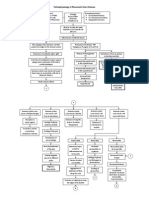
- Pathophysiology of Rheumatic Heart DiseaseDokumen3 halamanPathophysiology of Rheumatic Heart DiseaseLouie Kem Anthony Babaran50% (8)
- Daftar Isi WHO 2Dokumen52 halamanDaftar Isi WHO 2Okky HusainBelum ada peringkat
- Pathology Lecture 1 MSADokumen6 halamanPathology Lecture 1 MSAcejix87209Belum ada peringkat
- Lecture 33 - Biomarkers: Learning ObjectivesDokumen37 halamanLecture 33 - Biomarkers: Learning ObjectivesAustin KellyBelum ada peringkat
- Clinical Tips of StalwartsDokumen326 halamanClinical Tips of StalwartshayasakaBelum ada peringkat
- Summary of ECG AbnormalitiesDokumen8 halamanSummary of ECG AbnormalitiesChristine Nancy NgBelum ada peringkat
- Echo TutorialDokumen156 halamanEcho Tutorialhanibalu100% (1)
- The Different Therapeutic Choices With Arbs. Which One To Give? When? Why?Dokumen12 halamanThe Different Therapeutic Choices With Arbs. Which One To Give? When? Why?Jonathan Ian ArinsolBelum ada peringkat
- Urine Analysis FinalDokumen112 halamanUrine Analysis FinalNischita JayarajBelum ada peringkat
- Assessment Nursing Diagnosis Planning Interventions Rationale EvaluationsDokumen3 halamanAssessment Nursing Diagnosis Planning Interventions Rationale EvaluationsAjay SupanBelum ada peringkat
- Bleeding DisordersDokumen10 halamanBleeding Disorderslyli Star AngeloBelum ada peringkat
- Assessment of The Heart and Neck VesselsDokumen25 halamanAssessment of The Heart and Neck VesselsCuenca LanceBelum ada peringkat
- Epithelial TissueDokumen14 halamanEpithelial TissueDAVE CANALETABelum ada peringkat
- Pulmonary HypertensionDokumen9 halamanPulmonary HypertensionPricob ConstantinBelum ada peringkat
- Intervention MCQDokumen2 halamanIntervention MCQmoath alseadyBelum ada peringkat
- Cardiac Cycle WorksheetDokumen10 halamanCardiac Cycle WorksheetRamesh Kumar MuniandyBelum ada peringkat
- Reading Tests OET READING Part ADokumen147 halamanReading Tests OET READING Part Amanpreet kanwalBelum ada peringkat
- Electrocardiography IDokumen19 halamanElectrocardiography IsalochinBelum ada peringkat
- First Aid ManualDokumen68 halamanFirst Aid ManualAntonio Bernard100% (1)