Dystocia 2010
Diunggah oleh
Meigy NitalessyHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Dystocia 2010
Diunggah oleh
Meigy NitalessyHak Cipta:
Format Tersedia
Abnormal labor and
Dystocia
Soochow university
Xu Jianying
Abnormal Labor : Dystocia
Abnormal labor ,also called dystocia.
When we last talked about childbirth ,there
are four major influencing factors. When one
or more factors abnormal or uncoordinated
as abnormal labor. that may exist singly or
in combination.
Definition
Generally, abnormal labor is very common
whenever there is disproportion between the
presenting part of the fetus and the birth canal.
Dystocia literally means difficult labor and is
characterized by abnormally slow progress of labor.
Categories of dystocia
According to the factors divided to 3 types
Abnormalities of the powers (uterine contractility and
maternal expulsive effort)
either uterine forces insufficiently strong or
inappropriately coordinated to efface and dilate the
cervix uterine dysfunction or inadequate voluntary
muscle effort during the second stage of labor.
Categories of dystocia
Abnormalities of passenger (the fetus)
excessive fetal size , malpositions ,congenital
anomalies , multiple gestation
Abnormalities of the passage (the birth
canal)
pelvic contraction , soft tissue abnormalities of the
birth canal , masses or neoplasia , aberrant placental
location
1.Abnormalities of the powers
Uterine dysfunction
hypotonic primary
uterine inertia secondary
Uterine hypertonic
Dysfunction
uterine hypercontractility
Abnormalities of the powers
-----uterine inertia
1.Etiology of uterine inertia
Cephalopelvic disproportion or Fetal malposition
Abnormal of uterine muscle
psychical-factors
Imbalance of endocrine system
Administration of analgesia
Others
Cephalopelvic disproportion or
Fetal malposition
The fetal head or presenting part could not close
presses to the cervix and lower uterine segment.
fetopelvic disproportion arises from diminished pelvic
capacity, excessive fetal size, or malpresentation
Failure to progress in either spontaneous or stimulated
labor .This term is used to include lack of progressive
cervical dilatation or lack of fetal descent.
Abnormal of uterine muscle
Uterine muscle malfunction can result from uterine
overdistention or obstructed labor, or both. Muscle fiber
excessive elongation and contractility decline .
Polyhydramnios , macrosomia, Multiple births (twins).
Muscle fiber degeneration (Past history of repeat uterus
infection , abortion , induction of labor ,or operation),
myoma , pelvic tumors, myogenic dysplasia or malformed
uterus (didelphus uterus , unicornous uterus ).
psychical-factors
Fearing labor pain , anxiety, tension
Worried about fetal safety, labor hemorrhage, injury and
dystocia
which eventually lead to Uterine dysfunction
and occur uterine inertia
Other factors
hormonal mechanism of uterine activity
(deficiency of oxytocin , estradiol, prostaglandin)
excessive sedation ,anesthesia ,unripe cervix
fatigue , early abdominal pressure,
overactive bladder filling (fetal presentation
descent) .
2.Clinical findings
hypotonic uterine dysfunction (coordinated):
Although there are still normal uterine contraction
and maintain the polarity , symmetry, and a certain
rhythm, but the contraction is weak and feeble,
with short duration , long Interval and irregular.
when the contractions in the acme, no uterus uplift
and stiffen.
When uterine contractions:
the intrauterine pressure in the lower, and often <15
mmHg,
As a finger pressing on the fundus of uterus a
depression could appear
Maternal relative quiet , prolonged process.
(painless or can endure )
fetal heart rate changes lately (no anoxia
or lately)
2.Clinical findings
hypertonic uterine inertia and Uncoordinated
contractions : often occur together ,elevated resting
tone of the uterus
the exciting site of contraction is not from the
horn of uterus, and in a particular or multiple
site, and with uncoordinated rhythm, polarity
inversion
when uterine contracts the fundus is no firm,
and the mid or lower uterine segment harder
than that.
The uterus can not be completely relaxed,
uterine cavity pressure lasting with higher
state, but the cervix no dilation and fetal head
no descent progressively
Maternal lasting abdominal pain and fidgety
fetal heart rate changes early (anoxia)
2.Clinical findings
Failure to progress
Lack of progressive cervical dilatation (primiparas)
Prolonged latent phase >16hs
Prolonged active phase >8hs , cervix dilation<1.2cm/hs
Protracted active phase >2hs
Prolonged second stage >2hs
Lack of fetal descent
Prolonged descent >1cm/h
Protracted descent >1h
Prolonged labor >24hs (the total stage of
labor)
Labor-process range plan
4.Effect on maternal and fetus
maternal fatigue (Prolonged progress)
acidosis , or dehydration
infection (Prolonged progress , prom)
postpartum hemorrhage (insufficient contractility)
cesarean section rate
laceration
fetus distress , (uterine blood flow and fetal oxygenation )
birth injury ,Intracranial trauma (obstructed labor , rare)
prolapse of umbilical cord
stillbirth
5.management
Hypotonic: the rule of treatment--Strengthen
contractions and prevent PPH
the first stage of labor
General management : rest, eat more liquid
food ,sedation, correct acid , intravenous injection
Physical methods: massage uterus ,
emptying the bladder
stimulation nipple ,
artificial rupture of membrane (AROM)
enema
Drugs :
oxytocin 2.5U + 5%GS 500ml
( 5mU/ml ,8dropmin, at the begining)
diazepam 10mg iv
(Softening the cervix)
Cesarean section :
Following the above management still
ineffective or fetal distress
The second stage of labor
Forceps or vacuum extractor : second stage of
labor ,cervical fully dilated, membranes ruptured and
fetal survival, presenting part below the level of
ischial spine
Cesarean section : presenting part upward the level
of ischial spine or fetal distress
Hypertonic: the rule of treatment-- Adjusted
contractions and resume a normal polarity and
rhythm
Sedative: Dolantin or Morphine for adjusted and
resume to a normal contractions
Cesarean section Otherwise
Abnormalities of the powers
----- uterine hypercontractility
1.Clinical findings and diagnosis
Coordinated uterine hypercontractility :
uterine contraction is normal and maintain the
normal polarity , symmetry, and a certain rhythm, but
the intensity strength and frequency enhanced
the contraction with :
long duration , short Interval
precipitate delivery ( multiparas )
the total stage of labor <3hs ,
The process of labor is too fast
Birth injuries lacerations of the soft birth canal
fractures, intracranial hemorrhage of the
newborn
Postpartum hemorrhage,
uterine inversion,
Infections,
fetal distress, death
2.Effect on maternal and fetus
rupture of uterus
PPH , infection
soft birth canal trauma
fetal distress
fetal death
stillbirth
3.management
Prophylaxis reduced obstetric brutal operation.
Must be gentle , slightly and carefully
Tocolytic therapies sedatives inhibited
contractions : meperidine, magnesium sulfate.
Forceps , Vacuum extractor
Cesarean section.
1)forceps operations 2)Vacuum extractor
3)Cesarean section
Abnormalities of passage
the birth canal
pelvic contraction ,
soft tissue abnormalities of the birth canal ,
masses or neoplasia ,
aberrant placental location
Contractions of the pelvic
Bony pelvis a main composing part of birth
canal ,its size and shape have the direct relation to
the course of labor and delivery.
Any contraction of pelvic diameter that diminishes
the capacity can create dystocia.
There may be contractions of the pelvic inlet, the
midpelvis, the pelvic outlet, or a generally contracted
pelvis caused by combinations of these.
Contracted pelvic inlet
1.simple flat pelvis
promontory of sacrum
( dotted line )
forward dislocation
2.rachitic flat pelvis
(past history of rickets)
Contracted pelvic inlet
Clinical findings:
Fetopelvic disproportion , malposition or malpresentation face and
shoulder presentations are encountered three times more frequently
uterine inertia and prolonged progress of labor prolonged latent phase ,
early active phase and protracted active phase
cord prolapse ( loophole) occurs four to six times more frequently
Midpelvicoutlet contraction
Funnel shaped pelvic
the spines are prominent, the pelvic sidewalls converge
Midpelvicoutlet contraction
Clinical findings:
Fetopelvic disproportion persistent occiput
posterior position or deep transverse arrest , molding
of head and caput succedaneum
protracted active phase or prolonged second
stage secondary uterine inertia
Uterine rupture , perineal tears obstructed labor
Generally contraction pelvic
Each pelvic plane is 2cm less than normal value
or more
Can be seen in shape more short and small ,
well-balanced women of type of figure.
Diagnosis
A history of Rickets, bone tuberculosis, polio or pelvic
fracture (warrants careful review of previous radiographs
and possibly computed tomographic pelvimetry later in
pregnancy).
Physical examination height, spine, lower limb disability
(Height <150cm , lateral curvature usually associated with contracted
pelvis)
Diagnosis
Pelvic measurement
external pelvimetry
internal pelvimetry
sterile vaginal examination
Diagnosis
Pelvimetry
diagonal conjugate 12.5~13cm
bi-ischial diameter 10cm
incisura ischiadica 5~6cm
angle of subpubic arch 90
0
Diagnosis
The fetal position and dynamic monitoring of
labor
after onset of labor ,in primipara ,fetal head
unengagement ,breech, shoulder presentation;
birth process has been slow. (Prompt the contraction of
pelvis)
management
Trial labor under the effective uterine contractions
observed the progress of labor
There is no reliable method for evaluating the adequacy of
the lower pelvic, the sterile vaginal examination should be
performed early in the course of labor.
with continuous fetal monitoring ,fetal well-being may be
ensured
management
true inlet contracted : cesarean section
Midpelvicoutlet contraction: fetal head
biparietal diameter reached the level of the spines,
and can be depressed farther ,the fetal presentation
beyond station plus 2 , vaginal delivery usually is
possible .midwifery. otherwise cesarean section.
Administration of oxytocin should avoided in true
Midpelvicoutlet contraction
management
Generally contraction pelvic term fetus
(birthweight > 3000g) needed cesarean section
The fetus is not big , fetopelvic is adaptation and
without complication can try to labor
Deformed pelvic cesarean section
Soft--tissue dystocia
Soft tissue canal :lower part of uterus,
cervix, vagina previous scar of the birth canal
laceration , cervic conization and cauterization ,
cesarean section , rape injury in a small child , or
caustic abortifacient injury to vaginal vault and cervix.
Previous scaring of the birth canal may cause tissue
rigidity and dystocia .
cesarean section is generally required
Abnormalities of passenger
Fetal dystocia
caused by malposition or malpresentation ,
excessive size of the fetus ,or fetal
malformation.
If no disproportion exists, the head readily
enters the pelvis, and vaginal delivery can be
predicted.
malposition and malpresentation
a. vertex malposition
persistent occiput posterior
persistent occiput transverse 5%
sincipital presentation 1.08%
anterior asynclitism
posterior asynclitism 0.5%~0.81%
b. brow presentation 0.03%~0.1%
c. face presentation 0.08%~0.27%
d. breech presentation 3%~4%
e. abnormal fetal lie transverse or oblique lie 0.25%
Persistent occiput posterior or
transverse position (POP, POT)
Definition : Up to later stage of delivery the occiput cant
rotate anteriorly , persistent occiput posterior (POP) or
transverse position (POT). Most often , the result of
malrotation of occiput anterior position during labor(2/3).
Etiology :
Abnormal pelvic Anthropoid and android , transverse
narrowing of the midpelvis , the fetal head often engages
in OP or OT
Etiology
Bad flexion fetal backbone near the maternal
backbone , which disadvantages fetus flexion .
Uterine inertia influence fetal descent , flexion ,
internal rotation .
Cephalopelvic disproportion the pelvic cavity is
narrow , which limits fetal descent , flexion , internal
rotation .
Others placenta praevia , filling of bladder ,myoma
Clinical finding
Symptoms
Fetal head engages later at the onset of labor
Concordant uterine inertia and slow dilatation of
cervix ,induces prolonged active phase or second stage
Early use abdominal pressure before the cervix full
dilate
Treatment
The first stage Strengthen contractions , trial labor
Latent phase:
sufficient rest and nourishment . ( Pethidine or diazepam )
Active phase:
AROM cervix 3-4cm , membranes intac . To induce fetal head descending ,
strengthen contraction , and internal rotation .
Oxytocin intravenous drip infusion (small dose , 2--2.5u)
Cesarean section after treatment the labor is still not progressing or fetal
distress occurs
The treatment of the second stage
Midwifery BPD arrive the ischial spine plane or
below , s> +2 , to rotate the occiput to OA , vaginal
delivery forceps
Cesarean section fetal head is much high or
CPD
The treatment of the third stage
To prevent PPH prolonged labor readily
cause bleeding of uterine inertia .
Oxytocin large dose , intravenous drip infusion (20u)
Suture lacerations
Antibiotic
Anda mungkin juga menyukai
- Hirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandHirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- Early Pregnancy Bleeding Causes and TypesDokumen51 halamanEarly Pregnancy Bleeding Causes and TypesMesk Banat100% (2)
- Managing Multiple PregnanciesDokumen33 halamanManaging Multiple PregnanciesAndi Farid ABelum ada peringkat
- Genital FistulaeDokumen15 halamanGenital Fistulaesangeetha francisBelum ada peringkat
- Mal Presentations Mal PositionsDokumen4 halamanMal Presentations Mal PositionsMelissa Aina Mohd YusofBelum ada peringkat
- Impey Obs and Gynae Revision Notes PDFDokumen9 halamanImpey Obs and Gynae Revision Notes PDFRoiseBelum ada peringkat
- ARTICLE - 3 A Conceptual Study of Upavishtaka With Special Reference To IntrauterineDokumen5 halamanARTICLE - 3 A Conceptual Study of Upavishtaka With Special Reference To IntrauterineKalpanaBelum ada peringkat
- Gynecological History Taking and ExaminationDokumen17 halamanGynecological History Taking and Examinationnmsiswaridewi100% (1)
- Molar PregnancyDokumen14 halamanMolar Pregnancyfardeal_mckk100% (1)
- د.عبد الزهره THE GYNAECOLOGICAL EXAMINATION-1 (Muhadharaty)Dokumen29 halamanد.عبد الزهره THE GYNAECOLOGICAL EXAMINATION-1 (Muhadharaty)MohammedBelum ada peringkat
- Jurnal Inggris PDFDokumen4 halamanJurnal Inggris PDFTom PrasBelum ada peringkat
- Submitted By: Diana M. Resultay A301/Group-3B Submitted To: Ms. ReyesDokumen9 halamanSubmitted By: Diana M. Resultay A301/Group-3B Submitted To: Ms. ReyesDiannetotz MoralesBelum ada peringkat
- Recurrent Pregnancy LossDokumen61 halamanRecurrent Pregnancy LossHerman FiraBelum ada peringkat
- Approach To The Patient With An Adnexal Mass - UpToDateDokumen31 halamanApproach To The Patient With An Adnexal Mass - UpToDateRamackBelum ada peringkat
- Differential Diagnosis of The Adnexal Mass 2020Dokumen38 halamanDifferential Diagnosis of The Adnexal Mass 2020Sonia MVBelum ada peringkat
- Total Abdominal HysterectomyDokumen19 halamanTotal Abdominal HysterectomyMeidina Rachma Amanda100% (1)
- CC C C: June 8, 2011 By: Santos, Edilberto DBDokumen63 halamanCC C C: June 8, 2011 By: Santos, Edilberto DBHakugeiBelum ada peringkat
- Menstrual Cycle: Prepared By: Mrs Bini P S Amuel Assistant Professor, SSRC N, VapiDokumen16 halamanMenstrual Cycle: Prepared By: Mrs Bini P S Amuel Assistant Professor, SSRC N, VapiBini Don DanielBelum ada peringkat
- Myoma UteriDokumen8 halamanMyoma UteriFaraida Arvilla100% (1)
- Non-Surgical and Surgical Management of Pelvic OrgDokumen10 halamanNon-Surgical and Surgical Management of Pelvic OrgAhmed AnwarBelum ada peringkat
- Breech Presentation and DeliveryDokumen60 halamanBreech Presentation and DeliverySilvy Amalia100% (1)
- Vaginal CandidiasisDokumen29 halamanVaginal CandidiasisMike Serge RazafiBelum ada peringkat
- Postpartum Hemorrhage GuideDokumen20 halamanPostpartum Hemorrhage Guidem_amroellahBelum ada peringkat
- Infertility IDokumen36 halamanInfertility Idr_asaleh100% (1)
- Acute Urinary Retention Pathways and CausesDokumen26 halamanAcute Urinary Retention Pathways and Causeslukmankyubi100% (1)
- Essential facts about anemia in pregnancyDokumen40 halamanEssential facts about anemia in pregnancyraph faith100% (1)
- Dr. Sharda Jain: Director: Secretary GeneralDokumen91 halamanDr. Sharda Jain: Director: Secretary GeneraljijaniBelum ada peringkat
- Malpresentation and Malposition: Supervision By: DR Ashjan Tarayra Directed By: DR Montaser AsafrahDokumen53 halamanMalpresentation and Malposition: Supervision By: DR Ashjan Tarayra Directed By: DR Montaser AsafrahMahmoud Asafrah100% (1)
- Managing Multiple Pregnancy RisksDokumen60 halamanManaging Multiple Pregnancy RiskshaisureshBelum ada peringkat
- Chronic Suppurative Otitis MediaDokumen16 halamanChronic Suppurative Otitis MediaEmil P. MuhammadBelum ada peringkat
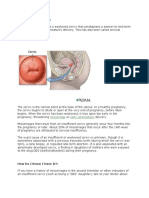
- How To Perform The Best Intrauterine Insemination A Review 2167 0250 1000140Dokumen7 halamanHow To Perform The Best Intrauterine Insemination A Review 2167 0250 1000140Anand NBelum ada peringkat
- 9fetal Well Being in PregnancyDokumen10 halaman9fetal Well Being in PregnancyuouoBelum ada peringkat
- Pap Smear - Overview, Indications, PreparationDokumen11 halamanPap Smear - Overview, Indications, PreparationBayu Surya DanaBelum ada peringkat
- Female Genital TuberculosisDokumen6 halamanFemale Genital TuberculosisallauddinbarackzaiBelum ada peringkat
- Changing Trends in Cesarean DeliveryDokumen7 halamanChanging Trends in Cesarean DeliveryEditor_IAIMBelum ada peringkat
- Pelvic Organ Prolapse GuideDokumen48 halamanPelvic Organ Prolapse GuideKerod AbebeBelum ada peringkat
- Evaluation of Right Side Foetal Myocardial Performance Index in Pregestational and Gestational Diabetes MellitusDokumen7 halamanEvaluation of Right Side Foetal Myocardial Performance Index in Pregestational and Gestational Diabetes MellitusGabyliz Gonzalez CastilloBelum ada peringkat
- Obstetrics Case PresentationDokumen27 halamanObstetrics Case PresentationMahaprasad sahoo 77Belum ada peringkat
- Hepatitis B in PregnancyDokumen17 halamanHepatitis B in PregnancysnazzyBelum ada peringkat
- Obstetric Anal Sphincter Injury (OASIS) - UpToDateDokumen39 halamanObstetric Anal Sphincter Injury (OASIS) - UpToDateErickBelum ada peringkat
- Trial of LabourDokumen2 halamanTrial of Labourgeorgeloto12Belum ada peringkat
- Benign Lesions of Vulva and VaginaDokumen34 halamanBenign Lesions of Vulva and VaginaCabdiBelum ada peringkat
- HepatitisDokumen3 halamanHepatitisElieth ConcepciónBelum ada peringkat
- Gynecological LaparosDokumen32 halamanGynecological LaparosYosef Dwi Cahyadi Salan100% (1)
- Biomarkers in Abnormal Uterine Bleeding: Precision Medicine in Assisted Reproductive Technologies Special IssueDokumen12 halamanBiomarkers in Abnormal Uterine Bleeding: Precision Medicine in Assisted Reproductive Technologies Special IssueWahyuning PutriBelum ada peringkat
- Female Reproductive SystemDokumen6 halamanFemale Reproductive SystemAlyanna L. ArquillanoBelum ada peringkat
- Abnormal Uterine BleedingDokumen5 halamanAbnormal Uterine Bleedingwuryan dewiBelum ada peringkat
- Disease JaundiceDokumen19 halamanDisease JaundiceMeena KoushalBelum ada peringkat
- AFE, RUPTURE OF UTERUS, (Autosaved)Dokumen31 halamanAFE, RUPTURE OF UTERUS, (Autosaved)maezu100% (1)
- Placenta PreviaDokumen2 halamanPlacenta PreviaAnonymous 0C4OZmRBelum ada peringkat
- Diagnosis and Management of Pelvic Organ ProlapseDokumen47 halamanDiagnosis and Management of Pelvic Organ ProlapseWindy Puspa Kusumah100% (1)
- Cervical Insufficiency:: Miscarriage Early (Premature)Dokumen2 halamanCervical Insufficiency:: Miscarriage Early (Premature)Ardelean EmanuelBelum ada peringkat
- Identification and Management of Ambiguous GenitaliaDokumen31 halamanIdentification and Management of Ambiguous Genitaliateslimolakunleraji100% (1)
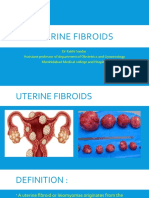
- Uterine FibroidsDokumen21 halamanUterine FibroidsPrasun BiswasBelum ada peringkat
- Normal Conduct of LaborDokumen62 halamanNormal Conduct of LaborFaye Cabotaje LinganBelum ada peringkat
- Green Top Guidelines 13Dokumen29 halamanGreen Top Guidelines 13garfield1Belum ada peringkat
- Endometriosis, ovarian cancer stages, infertility factors, missed abortion, accidental hemorrhage, pre-requests for forcepsDokumen20 halamanEndometriosis, ovarian cancer stages, infertility factors, missed abortion, accidental hemorrhage, pre-requests for forcepsDr-Amr Yakout MohamedBelum ada peringkat
- Ovarian Cysts and Cancer in PregnancyDokumen15 halamanOvarian Cysts and Cancer in Pregnancykarina100% (1)
- Abdominal WallDokumen75 halamanAbdominal WallJojo RyelciusBelum ada peringkat
- 10 Kasus Terbanyak Pasien Ginekologi & ObstretiDokumen2 halaman10 Kasus Terbanyak Pasien Ginekologi & ObstretiAbdillah AdilBelum ada peringkat
- Sample MCQ QuestionsDokumen11 halamanSample MCQ QuestionsPreeti ChouhanBelum ada peringkat
- Dystocia: Bagian / UP Obgin FK - UNHAS /RS - Dr.Wahidin Sudirohusodo MakassarDokumen69 halamanDystocia: Bagian / UP Obgin FK - UNHAS /RS - Dr.Wahidin Sudirohusodo MakassarYhaya 'Dzulhijjahyanti'Belum ada peringkat
- Nclex A2 Group08Dokumen4 halamanNclex A2 Group08Infan BrianBelum ada peringkat
- Pre-Eclampsia and EclampsiaDokumen19 halamanPre-Eclampsia and EclampsiaBiscuits and milkBelum ada peringkat
- Updated NCM 107 Lecture Week 7Dokumen27 halamanUpdated NCM 107 Lecture Week 7Quencee CalaycayBelum ada peringkat
- Alternatives To ChildbirthDokumen4 halamanAlternatives To ChildbirthMaria Donabella OngueBelum ada peringkat
- Placenta Previa Case StudyDokumen7 halamanPlacenta Previa Case StudyphearlieBelum ada peringkat
- Birth Story 1Dokumen7 halamanBirth Story 1api-251902149Belum ada peringkat
- Prolonged Labour: Mr. KamauDokumen17 halamanProlonged Labour: Mr. KamauFred Fredrick0% (1)
- WWW Scribd Com Document 437023289 Polyhydramnios CASE STUDYDokumen14 halamanWWW Scribd Com Document 437023289 Polyhydramnios CASE STUDYJv LalparaBelum ada peringkat
- Evidence-Based Routine Antenatal CareDokumen35 halamanEvidence-Based Routine Antenatal Caresalah subbahBelum ada peringkat
- Obstructed LabourDokumen15 halamanObstructed LaboursunilBelum ada peringkat
- 10 Management of Gynaecologic and Obstetrical EmergenciesDokumen34 halaman10 Management of Gynaecologic and Obstetrical EmergenciesRisal MujahidinBelum ada peringkat
- JOGCan 2018 Fetal Surveillance A AntepartumDokumen21 halamanJOGCan 2018 Fetal Surveillance A AntepartumMiguel Guillermo Salazar ClavijoBelum ada peringkat
- Case Scenario IDokumen2 halamanCase Scenario IGynesis Lim RoqueroBelum ada peringkat
- Amniotic FluidDokumen34 halamanAmniotic Fluidannu panchalBelum ada peringkat
- DR ScrapbookDokumen8 halamanDR Scrapbookcrenz23_shaniyha15Belum ada peringkat
- Obstetric Analgesia and Anesthesia: John J. BonicaDokumen8 halamanObstetric Analgesia and Anesthesia: John J. BonicaJoebestBelum ada peringkat
- TESTS - Obstetrics and GynecologyDokumen38 halamanTESTS - Obstetrics and GynecologyTemitope AdeosunBelum ada peringkat
- Diagnostic TestsDokumen6 halamanDiagnostic TestsKelsey MacaraigBelum ada peringkat
- Due Date CalculatorDokumen6 halamanDue Date CalculatorSanjay Kumar SanjuBelum ada peringkat
- OB HX and PEDokumen37 halamanOB HX and PEdenekeBelum ada peringkat
- DR Mercola - How Are The COVID Shots Affecting Mothers-To-BeDokumen10 halamanDR Mercola - How Are The COVID Shots Affecting Mothers-To-Beguy777Belum ada peringkat
- PartogramDokumen31 halamanPartogramRemelou Garchitorena AlfelorBelum ada peringkat
- Medical Jurisprudence ProjectDokumen11 halamanMedical Jurisprudence ProjectUtkarshini VermaBelum ada peringkat
- PartographDokumen4 halamanPartographElonah Gien DimalaluanBelum ada peringkat
- GMEC SCN Fetal Monitoring in Labour CTG Guideline FINAL V2.1 September 2020Dokumen33 halamanGMEC SCN Fetal Monitoring in Labour CTG Guideline FINAL V2.1 September 2020Anel BecirspahicBelum ada peringkat
- A. FirstTrim ISUOG GuidelinesDokumen37 halamanA. FirstTrim ISUOG GuidelinesSurya Andri AntaraBelum ada peringkat