NRS 230 Pharmacology Week 1 Students - 11!22!11
Diunggah oleh
angieswenson0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
360 tayangan110 halamanPharmacology powerpoint. Information from class
Judul Asli
NRS 230 Pharmacology Week 1 Students_11!22!11
Hak Cipta
© © All Rights Reserved
Format Tersedia
PPT, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniPharmacology powerpoint. Information from class
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PPT, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
360 tayangan110 halamanNRS 230 Pharmacology Week 1 Students - 11!22!11
Diunggah oleh
angieswensonPharmacology powerpoint. Information from class
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PPT, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 110
1
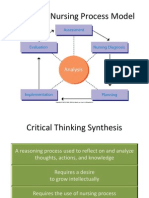
The Nursing Process
and Drug Therapy
CHAPTER 1
2
The Nursing Process
A research-based organizational
framework for professional nursing
practice
Central to all nursing care
Encompasses all steps taken by the nurse
in caring for a patient
Flexibility is important
Requires critical thinking
Ongoing and constantly evolving process
3
The Nursing Process (contd)
Assessment
Nursing diagnosis
Planning
Goals
Outcome criteria
Implementation
Evaluation
4
The Nursing Process (contd)
Assessment
Data collection
Subjective, objective
Medication history
Prescriptions
Over-the-counter medications
Herbal therapies
Responses to medications (therapeutic and adverse)
5
The Nursing Process (contd)
Nursing diagnosis
Decision about the need/problem of the
patient (actual or at risk)
Critical thinking, creativity, and accurate
data collection
NANDA-I format
6
The Nursing Process (contd)
Nursing diagnosis
Three steps
Human response to illness (actual or at risk)
related to
as evidenced by
7
The Nursing Process (contd)
Planning
Identification of goals and outcome criteria
Must be specific and measurable
Must be patient-centered
Time frame
Prioritization
8
The Nursing Process (contd)
Goals
Objective, measurable, realistic
Time frame specified
Outcome criteria
Specific standard(s) of measure
Patient oriented
9
The Nursing Process (contd)
Implementation
Initiation and completion of the nursing
care plan as defined by the nursing
diagnoses and outcome criteria
Follow the Six Rights of medication
administration
10
The Role of Nurses in Relation to
Pharmacology
Nurses share information with other health care professionals to provide the
most effective medication regimen for the patient
Nurses have to follow the Six Rights of Medication Administration
Nurses play an active role in drug administration
Nurses contribute to the planning and modification of drug therapy from their
assessment of patient factors and evaluation of progress or problems
occurring during drug therapy
In addition to: the role in patient education and compliance
1. Right drug
2. Right dose
3. Right time
4.Right Route
5. Right Patient
6. Right Documentation
11
Evaluation
Ongoing part of the nursing process
Determining the status of the goals and
outcomes of care
Monitoring the patients response to drug
therapy
Expected and unexpected responses
Clear concise documentation
12
Pharmacologic
Principles
CHAPTER 2
13
Pharmacologic Principles
Drug
Any chemical that affects the physiologic
processes of a living organism
Pharmacology
Study or science of drugs
14
Drug Names
Chemical name
Describes the drugs chemical composition and
molecular structure
Generic name (nonproprietary name)
Name given by the United States Adopted Name
Council
Trade name (proprietary name)
The drug has a registered trademark; use
of the name is restricted by the drugs patent owner
(usually the manufacturer)
15
Pharmacologic Principles
Pharmaceutics
Pharmacokinetics
Pharmacodynamics
Pharmacotherapeutics
Pharmacognosy
16
Pharmaceutics
The study of how various drug forms
influence pharmacokinetic and
pharmacodynamic activities
17
Pharmacokinetics
The study of what the body does to the
drug
Absorption
Distribution
Metabolism
Excretion
18
Pharmacodynamics
The study of what the drug does to the
body
The mechanism of drug actions in living
tissues
19
Pharmacotherapeutics
The use of drugs and the clinical
indications for drugs to prevent and treat
diseases
Empirical therapeutics
Rational therapeutics
20
Pharmacognosy
The study of natural (plant and animal)
drug sources
21
Pharmaceutics
Dosage form design affects dissolution
22
23
Pharmacokinetics: Absorption
The rate at which a drug leaves its site
of administration, and the extent to
which absorption occurs
Bioavailability
Bioequivalency
24
Factors That Affect Absorption
Absorption characteristics vary according
to the dosage form and route
Food or fluids administered with the drug
Dosage formulation
Status of the absorptive surface
Rate of blood flow to the small intestine
Acidity of the stomach
Status of GI motility
25
Routes
A drugs route of administration affects
the rate and extent of absorption of that
drug
Enteral (GI tract)
Parenteral
Topical
26
Enteral Route
The drug is absorbed into the systemic
circulation through the oral or gastric
mucosa or the small intestine
Oral
Sublingual
Buccal
Rectal (can also be topical)
27
First-Pass Effect
The metabolism of a drug and its
passage from the liver into the
circulation
A drug given via the oral route may be
extensively metabolized by the liver before
reaching the systemic circulation (high
first-pass effect)
The same druggiven IVbypasses the
liver, preventing the first-pass effect from
taking place, and more drug reaches the
circulation
28
Parenteral Route
Intravenous (fastest delivery into the blood
circulation)
Intramuscular
Subcutaneous
Intradermal
Intraarterial
Intrathecal
Intraarticular
Transdermal also can be considered parenteral
29
Topical Route
Skin (including transdermal patches)
Eyes
Ears
Nose
Lungs (inhalation)
Rectum
Vagina
30
Distribution
The transport of a drug in the body by
the bloodstream to its site of action
Protein-binding
Water soluble vs. fat soluble
Blood-brain barrier
Areas of rapid distribution: heart, liver,
kidneys, brain
Areas of slow distribution: muscle, skin, fat
31
Metabolism/Biotransformation
The biochemical transformation of a drug
into an inactive metabolite, a more
soluble compound, or a more potent
metabolite
Liver (main organ)
Skeletal muscle
Kidneys
Lungs
Plasma
Intestinal mucosa
32
Metabolism/Biotransformation
Biologic transformation of a drug into:
An inactive metabolite
A more soluble compound
A more potent metabolite
33
Metabolism/Biotransformation
(contd)
Organs or body tissues
Liver (main)
Skeletal muscle
Kidneys
Lungs
Plasma
Intestinal mucosa
34
Metabolism/Biotransformation
(contd)
Factors that decrease metabolism
Cardiovascular dysfunction
Renal insufficiency
Starvation
Obstructive jaundice
Slow acetylator
Erythromycin or ketoconazole drug therapy
35
Metabolism/Biotransformation
(contd)
Factors that increase metabolism
Fast acetylator
Barbiturate therapy
Rifampin therapy
36
Metabolism/Biotransformation
(contd)
Delaying drug metabolism causes:
Accumulation of drugs
Prolonged action of the drugs drug toxicity
Stimulating drug metabolism causes:
Diminished pharmacologic effects
37
Excretion
The elimination of drugs from the body
Kidneys (main organ)
Liver
Bowel
Biliary excretion
Enterohepatic recirculation
38
Half-life
The time it takes for one half of the original
amount of a drug to be removed from the
body
A measure of the rate at which a drug is
removed from the body
Most drugs considered to be effectively
removed after about five half-lives
Steady state
39
The Movement of Drugs
Through the Body
Drug actions
The cellular processes involved in the
drug and cell interaction
Drug effect
The physiologic reaction of the body to
the drug
40
Onset, Peak, and Duration
Onset
The time it takes for the drug to elicit a
therapeutic response
Peak
The time it takes for a drug to reach its
maximum therapeutic response
Duration
The time a drug concentration is
sufficient to elicit a therapeutic response
41
42
Therapeutic Drug Monitoring
Peak level
Highest blood level
Trough level
Lowest blood level
43
Ways Drugs Produce
Therapeutic Effects
Once the drug is at the site of action, it can
modify the rate (increase or decrease) at
which the cells or tissues function
A drug cannot make a cell or tissue
perform a function it was not designed to
perform
44
Pharmacodynamics:
Mechanisms of Action
Receptor interactions
Enzyme interactions
Nonselective interactions
45
Pharmacotherapeutics:
Types of Therapies
Acute therapy
Maintenance therapy
Supplemental/replacement therapy
Palliative therapy
Supportive therapy
Prophylactic therapy
Empiric therapy
46
Contraindications
Any characteristic of the patient, especially
a disease state, that makes the use of a
given medication dangerous for the patient
It is important to assess for
contraindications!
47
Monitoring
The effectiveness of the drug therapy must
be evaluated
One must be familiar with the drugs:
Intended therapeutic action (beneficial)
Unintended but potential adverse effects
(predictable, adverse reactions)
48
Monitoring (contd)
Therapeutic index
Drug concentration
Patients condition
Tolerance and dependence
Interactions
Adverse drug effects
49
Monitoring (contd)
Therapeutic index
Ratio of a drugs toxic level to the level that
provides therapeutic benefits
Tolerance
Decreasing response to repeated drug doses
Dependence
Physiologic or psychological need for a drug
50
Monitoring (contd)
Interactions may occur with other drugs or
food
A drug interaction is the alteration of a drugs action by:
Other prescribed drugs
Over-the-counter medications
Herbal therapies
51
Monitoring (contd)
Drug interactions
Additive effect
Synergistic effect
Antagonistic effect
Incompatibility
52
Monitoring (contd)
Adverse drug events
Medication errors
Adverse drug reactions
53
Monitoring (contd)
Adverse drug reactions
Pharmacologic reactions, including adverse effects
Hypersensitivity (allergic) reaction
Idiosyncratic reaction
Drug interaction
54
Monitoring (contd)
Adverse effects
Predictable, well-known reactions that result in little or
no change in patient management
Predictable frequency
Occurrences are related to the size of the dose
Usually resolve when the drug is discontinued
55
Other Drug-Related Effects
Teratogenic
Mutagenic
Carcinogenic
56
Pharmacognosy
Four main sources for drugs
Plants
Animals
Minerals
Laboratory synthesis
57
Toxicology
The study of poisons and unwanted
responses to drugs and other
chemicals
58
59
Life Span Considerations
CHAPTER 3
60
Life Span Considerations
Pregnancy
Breast-feeding
Neonatal and pediatric
Elderly
61
Pregnancy
First trimester is the period of greatest
danger for drug-induced developmental
defects
Drugs cross the placenta by diffusion
During the last trimester, the greatest
percentage of maternally absorbed drug
gets to the fetus
FDA has implemented pregnancy safety
categories
62
63
Breast-feeding
Breast-fed infants are at risk for exposure
to drugs consumed by the mother
Consider risk-to-benefit ratio
64
65
Neonatal and Pediatric
Considerations:
Pharmacokinetics
Absorption
Gastric pH less acidic
Gastric emptying slowed
Intramuscular absorption faster and
irregular
66
Neonatal and Pediatric
Considerations:
Pharmacokinetics (contd)
Distribution
The younger the person, the greater the
percentage of total body water
Greater total body water means lower fat
content
Decreased level of protein binding
Immature blood-brain barriermore drugs
enter the brain
67
Neonatal and Pediatric
Considerations:
Pharmacokinetics (contd)
Metabolism
Liver immature, does not produce enough
microsomal enzymes
Older children may have increased
metabolism, requiring higher doses than
infants
Other factors
68
Neonatal and Pediatric
Considerations:
Pharmacokinetics (contd)
Excretion
Kidney immaturity affects glomerular
filtration rate and tubular secretion
Decreased perfusion rate of the kidneys
may reduce excretion of drugs
69
Factors Affecting Pediatric
Drug Dosages
Skin is thin and permeable
Stomach lacks acid to kill bacteria
Lungs have weaker mucus barriers
Body temperatures less well regulated,
and dehydration occurs easily
Liver and kidneys are immature,
impairing drug metabolism and
excretion
70
Methods of Dosage
Calculation for Pediatric
Patients
Body surface area method
Using the West nomogram
Always use weight in kilograms, not
pounds
Body weight dosage calculations
Using mg/kg (most commonly used)
71
72
The Elderly
Elderly: older than age 65
Use of over-the-counter medications
Increased incidence of chronic illnesses
Sensory and motor deficits
Polypharmacy
73
Physiologic Changes
in the Elderly Patient
Cardiovascular
Gastrointestinal
Hepatic
Renal
74
The Elderly:
Pharmacokinetics
Absorption
Gastric pH less acidic
Gastric emptying slowed
Movement through GI tract slowed
Blood flow to GI tract reduced
Use of laxatives may accelerate GI motility
75
The Elderly:
Pharmacokinetics (contd)
Distribution
Lower total body water percentages
Increased fat content
Decreased production of proteins by the
liver, resulting in decreased protein binding
of drugs (and increased circulation of free
drugs)
76
The Elderly:
Pharmacokinetics (contd)
Metabolism
Aging liver produces fewer microsomal
enzymes, affecting drug metabolism
Reduced blood flow to the liver
77
The Elderly:
Pharmacokinetics (contd)
Excretion
Decreased glomerular filtration rate
Decreased number of intact nephrons
78
The Elderly:
Problematic Medications
Analgesics, including NSAIDs and opioids
Anticoagulants
Anticholinergics
Antidepressants
Antihypertensives
Cardiac glycosides (digoxin)
Sedatives and hypnotics, CNS depressants
Thiazide diuretics
79
CHAPTER 4
Cultural, Legal, and Ethical
Considerations
80
New Drug Development
Investigational new drug (IND) application
Informed consent
U.S. FDA drug approval process
Preclinical testing
Clinical studies
Investigational drug studies
Expedited drug approval
81
U.S. FDA Drug Approval
Process
Preclinical investigational drug studies
Informed consent
Clinical phases of investigational drug
studies
Phase I
Phase II
Phase III
Phase IV
82
Ethical Nursing Practice
American Nurses Association (ANA) Code
of Ethics for Nurses
International Council of Nurses (ICN)
Code of Ethics for Nurses
83
Cultural Considerations
Assess the influence of a patients cultural
beliefs, values, and customs
Drug polymorphism
Compliance level with therapy
Environmental considerations
Genetic factors
Varying responses to specific drugs
84
Cultural Considerations (contd)
Changing national demographics
Influence of ethnicity and genetics
Rapid and slow acetylators
Examples of various ethnic groups found
in the U.S.
Asian
African American
Hispanic
Native American
85
Cultural Assessment
Health beliefs and practices
Past uses of medicine
Folk remedies
Home remedies
Over-the-counter drugs and treatment
Herbal remedies
86
Cultural Assessment (contd)
Usual response to illness
Responsiveness to medical treatment
Religious practices and beliefs
Dietary habits
87
Chapter 1
The Nursing Process
and Drug Therapy
88
1. The day shift charge nurse is making rounds. A patient tells the
nurse that the night shift nurse never gave him his medication,
which was due at 11 pm. What should the nurse do first to
determine whether the medication was given?
1. Call the night nurse at home.
2. Check the Medication Administration Record.
3. Call the pharmacy.
4. Review the nurses notes.
89
2. The nurse answers a patients call light and finds the patient
sitting up in bed and requesting pain medication. What should
the nurse do first?
1. Check the orders and give the patient the
requested pain medication.
2. Provide comfort measures to the patient.
3. Assess the patients pain and pain level.
4. Evaluate the effectiveness of previous pain
medications.
90
3. The patients Medication Administration Record lists two antiepileptic
medications that are due at 0900, but the patient is NPO for a barium
study. The nurses coworker suggests giving the medications via IV
because the patient is NPO. What should the nurse do?
1. Give the medications PO with a small sip of water.
2. Give the medications via the IV route because the
patient is NPO.
3. Hold the medications until after the test is
completed.
4. Call the physician to clarify the instructions.
91
4. The nurse goes into a patients room to give medications. The
patient is confused, and the nurse discovers that the patient is
not wearing an armband. How should the nurse identify the
patient?
1. Ask the patient to state his name.
2. Ask the visitor the patients name.
3. Ask the patient to state his birthday.
4. Check with the charge nurse to obtain an
armband.
92
Chapter 2
Pharmacologic
Principles
93
1. The nurse is giving a medication that has a high first-pass effect.
The physician has changed the route from IV to PO. The nurse
expects the oral dose to be:
1. higher because of the first-pass effect.
2. lower because of the first-pass effect.
3. the same as the IV dose.
4. unchanged.
94
2. A patient is complaining of severe pain and has orders for
morphine sulfate. The nurse knows that the route that would give
the slowest pain relief would be which route?
1. IV
2. IM
3. SC
4. PO
95
3. A patient is prescribed ibuprofen 200 mg PO every 4 hours as
needed for pain. The pharmacy sends up enteric-coated tablets,
but the patient refuses the tablets, stating that she cannot swallow
pills. What should the nurse do?
1. Crush the tablets and mix them with applesauce or pudding.
2. Call the pharmacy and ask for the liquid form of the
medication.
3. Call the pharmacy and ask for the IV form of the medication.
4. Encourage the patient to try to swallow the tablets.
96
4. When giving morning medications, the nurse is preparing to
administer a transdermal patch medication and finds that the
patient already has a medication patch on his right upper chest.
What should the nurse do?
1. Remove the old medication patch and notify the
physician.
2. Apply the new patch without removing the old one.
3. Remove the old patch and apply the new patch in the
same spot.
4. Remove the old patch and apply the new one to a
different, clean area.
97
5. Two drugs that are synergistic do not have a drug interaction
with each other.
1. True
2. False
98
Chapter 3
Life Span
Considerations
99
Most medications have been
extensively studied in a variety of
different populations and age groups.
1. True
2. False
100
2. A pregnant woman with liver disease is taking a
pregnancy category B medication for her illness.
Which statement is true in this situation?
1. The mothers liver disease will expose the fetus
to less of the medication.
2. The mothers liver disease will expose the fetus
to more of the medication.
3. Because the medication is pregnancy category
B, the medication is generally considered safe for
the fetus.
4. The liver of the fetus will protect the fetus from
the effects of the medication.
101
3. A mother calls the clinic to ask about giving
acetaminophen to her infant. She says she has used
the liquid form for her 5-year-old child, and she wants
to know how much to give to her infant, who has a
fever. The nurse should:
1. instruct the mother to give the infant the same
dose as the child.
2. instruct the mother to give the infant half the
dose that she would normally give the child.
3. assist the mother in calculating the dose for the
infant.
4. consult with a physician before instructing the
mother on giving the medication.
102
4. The elderly patient will experience
polypharmacy, but not much can be
done about it.
1. True
2. False
103
5. What percent of currently approved
drugs in the U.S. lack approval for
pediatric use?
1. 10%
2. 25%
3. 50%
4. 75%
104
Chapter 4
Cultural, Legal, and
Ethical
Considerations
105
A 20-year-old patient is receiving chemotherapy for
leukemia. Her parents are very involved in her care. The
patient has indicated that she would like to try alternative
therapies in addition to the chemotherapy. Her parents
disapprove of this and do not want their daughter to take
any wacky treatments. The nurses responsibility is to:
1. research the safety of combining the therapies.
2. agree with the parents as they are being more
reasonable.
3. work with the patient and physician to find
appropriate alternative therapies.
4. convince the patient that the chemotherapy is most
beneficial to her health.
106
2. Two 40-year-old patients, one of Asian
origin and one of European origin, are
taking the same drug. The same drug
may result in very different responses in
these individuals.
1. True
2. False
107
3. A nurse has been asked to participate in an
elective procedure that violates the nurses
personal ethical principles. The nurse should:
1. refuse to participate.
2. ask to switch assignments with another
nurse.
3. speak to the manager or supervisor.
4. perform the procedure.
108
4. A research group is conducting an investigational drug study
on a promising new drug for osteoporosis. It has been difficult
to find research subjects that meet the criteria. Just before the
conclusion of the study, four subjects approach the
researchers and express their desire to withdraw from the
study. The researcher should first:
1. inform them that they waited too long to withdraw from
the study.
2. explore with them the reasons for withdrawing from the
study.
3. acknowledge that they can withdraw at any time from
the study.
4. request that they try to remain with the study until it is
completed.
109
5. Which racial group is predicted to be
nearly one in three U.S. residents in
2050?
1. African American
2. Asian
3. Hispanic
4. White
110
Anda mungkin juga menyukai
- Necrotizing Fasciitis, (Flesh Eating Disease) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandNecrotizing Fasciitis, (Flesh Eating Disease) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- Hypertension, Cardiovascular Disease, Analgesics, and Endocrine DisordersDari EverandHypertension, Cardiovascular Disease, Analgesics, and Endocrine DisordersJack Z. YetivBelum ada peringkat
- Notes on Nursing - What It Is, and What It Is Not: With a Chapter From 'Beneath the Banner, Being Narratives of Noble Lives and Brave Deeds' by F. J. CrossDari EverandNotes on Nursing - What It Is, and What It Is Not: With a Chapter From 'Beneath the Banner, Being Narratives of Noble Lives and Brave Deeds' by F. J. CrossBelum ada peringkat
- Approach To Pediatric AnemiaDokumen18 halamanApproach To Pediatric AnemiaMade Oka HeryanaBelum ada peringkat
- Mechanisms of Drug Toxicity: Proceedings of the Third International Pharmacological MeetingDari EverandMechanisms of Drug Toxicity: Proceedings of the Third International Pharmacological MeetingH. RaškováBelum ada peringkat
- Mechanical VentilationDokumen43 halamanMechanical VentilationsalemraghuBelum ada peringkat
- Pulmonary Arterial Hypertension in Congenital Heart Disease: Eisenmenger’s Syndrome - A Global PerspectiveDari EverandPulmonary Arterial Hypertension in Congenital Heart Disease: Eisenmenger’s Syndrome - A Global PerspectiveBelum ada peringkat
- Kimberly F. v. Mary Hitchcock, 1st Cir. (1993)Dokumen34 halamanKimberly F. v. Mary Hitchcock, 1st Cir. (1993)Scribd Government DocsBelum ada peringkat
- Interpretation of Full Blood CountDokumen25 halamanInterpretation of Full Blood CountClementBelum ada peringkat
- Group 5 - Hemodialysis - Chronic Kidney FailureDokumen31 halamanGroup 5 - Hemodialysis - Chronic Kidney FailureKimberly Abella CabreraBelum ada peringkat
- Approach To Septic ShockDokumen16 halamanApproach To Septic ShockRaja EllysyaBelum ada peringkat
- ps52 2015 Guidelines For Transport of Critically Ill Patients PDFDokumen12 halamanps52 2015 Guidelines For Transport of Critically Ill Patients PDFPalwasha MalikBelum ada peringkat
- Pre Anaesthetic Check-UpDokumen4 halamanPre Anaesthetic Check-UpUdoy PaulBelum ada peringkat
- Mechanical VentilationDokumen108 halamanMechanical Ventilationrizal aljufri100% (1)
- Guide To Case Presentation-1Dokumen36 halamanGuide To Case Presentation-1Amanda Rodriguez TejedaBelum ada peringkat
- Route of Administration 2020Dokumen37 halamanRoute of Administration 2020ForwardBelum ada peringkat
- Management of Hypoxia During AnaesthesiaDokumen5 halamanManagement of Hypoxia During AnaesthesiaNurhafizahImfista100% (1)
- Basics of ICU CareDokumen19 halamanBasics of ICU CareUmar Farooq GondalBelum ada peringkat
- Urinary Incontinence: 2 PathophysiologyDokumen8 halamanUrinary Incontinence: 2 PathophysiologyZiedTrikiBelum ada peringkat
- CH 39 Acid-Base ElectrolyteDokumen16 halamanCH 39 Acid-Base ElectrolyteJonathan EdieBelum ada peringkat
- Medication Administration Via Enteral Tube Feeding GuideDokumen31 halamanMedication Administration Via Enteral Tube Feeding GuideSara Aly YoussefBelum ada peringkat
- Mechanical Ventilation: Essentials For Registered NursesDokumen49 halamanMechanical Ventilation: Essentials For Registered NursesPraveen ThulasiBelum ada peringkat
- Overview: Project Chagas: Health and MedicineDokumen8 halamanOverview: Project Chagas: Health and MedicineRade NikolajevicBelum ada peringkat
- Transport of Critically Ill PatientsDokumen13 halamanTransport of Critically Ill Patientsansuh22100% (1)
- Maternity Antepartum Genetic TestingDokumen21 halamanMaternity Antepartum Genetic TestingBobbie N Melinda RussellBelum ada peringkat
- Final PPT Suman1-2Dokumen69 halamanFinal PPT Suman1-2sauravBelum ada peringkat
- Use of Vasopressors and InotropesDokumen14 halamanUse of Vasopressors and InotropesEdwin VargasBelum ada peringkat
- Nursing Care Plan: Assessment Diagnosis Inference Planning Intervention Rationale EvaluationDokumen3 halamanNursing Care Plan: Assessment Diagnosis Inference Planning Intervention Rationale EvaluationJessa FabicoBelum ada peringkat
- Antineoplastic DrugsDokumen16 halamanAntineoplastic DrugstheintrovBelum ada peringkat
- Pediatric Drug Calculations 03Dokumen38 halamanPediatric Drug Calculations 03Leia Avriele TankiamcoBelum ada peringkat
- SGD Case Presentation 8Dokumen34 halamanSGD Case Presentation 8Karen C. Del Rosario100% (1)
- Chapter - 037 - 1 Infective Endocarditis ClassDokumen41 halamanChapter - 037 - 1 Infective Endocarditis ClassWisdomIsMiseryBelum ada peringkat
- NR 328 Simulation 1 JPDokumen4 halamanNR 328 Simulation 1 JPJohn MixerBelum ada peringkat
- Syllabus NGR 6803 EBPDokumen12 halamanSyllabus NGR 6803 EBPmatthewBelum ada peringkat
- The Evolution of Professional NursingDokumen32 halamanThe Evolution of Professional NursingNatukunda DianahBelum ada peringkat
- Bate's Guide To Physical examination+MCQsDokumen4 halamanBate's Guide To Physical examination+MCQsRaden Adjeng PalupiBelum ada peringkat
- Sepsis Content Concepts MapDokumen2 halamanSepsis Content Concepts Mapghodghod1230% (1)
- ICU TriageDokumen27 halamanICU TriageAkmal FahrezzyBelum ada peringkat
- Factors Affecting Drug Metabolism PDFDokumen2 halamanFactors Affecting Drug Metabolism PDFPaige50% (2)
- Pacu Tylenol PresentationDokumen10 halamanPacu Tylenol PresentationStanford AnesthesiaBelum ada peringkat
- Research QuestionnaireDokumen3 halamanResearch QuestionnaireJason Roy Edward NathanBelum ada peringkat
- Therapeutic Drug MonitoringDokumen14 halamanTherapeutic Drug MonitoringChristian DavidBelum ada peringkat
- Intrahospital Transport of Critically Ill PatientsDokumen14 halamanIntrahospital Transport of Critically Ill Patientsعزالدين الزوقريBelum ada peringkat
- Huntington'S Disease: Dhakal, Gerbabuena, Jittwatanatakool, Jordan, KarnDokumen25 halamanHuntington'S Disease: Dhakal, Gerbabuena, Jittwatanatakool, Jordan, KarnIrene JordanBelum ada peringkat
- NUR 104 Nursing Process MY NOTESDokumen77 halamanNUR 104 Nursing Process MY NOTESmeanne073100% (1)
- Extubation Intubation 2016Dokumen34 halamanExtubation Intubation 2016Leandro DomingoBelum ada peringkat
- Blood TransfusionDokumen5 halamanBlood TransfusionMoustafa Hazzaa100% (1)
- Status EpilepticusDokumen70 halamanStatus Epilepticusfloppyfishh100% (1)
- Patho 3Dokumen11 halamanPatho 3Dranreb Berylle MasangkayBelum ada peringkat
- Inhalers in Pediatric AsthmaDokumen53 halamanInhalers in Pediatric AsthmaKishore Chandki100% (2)
- Technique: Preventing and Controlling Infections in Home Care and HospiceDokumen7 halamanTechnique: Preventing and Controlling Infections in Home Care and HospiceOlaMostafaBelum ada peringkat
- ChemotherapyDokumen253 halamanChemotherapyalmskein100% (1)
- ABC Acute Renal FailureDokumen5 halamanABC Acute Renal FailureAngela CristinoBelum ada peringkat
- Standardised Handover Protocol 2014 PDFDokumen7 halamanStandardised Handover Protocol 2014 PDFNikkae AngobBelum ada peringkat
- Case Study 2014Dokumen56 halamanCase Study 2014amier_s100% (1)
- Top 100 Secrets About Critical CareDokumen8 halamanTop 100 Secrets About Critical CareMariaUlfaBelum ada peringkat
- Describe The Negative Feedback Mechanism Associated With Glucose That Controls Insulin and Glucagon SecretionDokumen3 halamanDescribe The Negative Feedback Mechanism Associated With Glucose That Controls Insulin and Glucagon SecretionangieswensonBelum ada peringkat
- EBP & ResearchDokumen6 halamanEBP & ResearchangieswensonBelum ada peringkat
- Unit 3 Study GuideDokumen10 halamanUnit 3 Study GuideangieswensonBelum ada peringkat
- Unit 2 Study GuideDokumen10 halamanUnit 2 Study GuideangieswensonBelum ada peringkat
- Unit 4 Study Guide PathoDokumen10 halamanUnit 4 Study Guide Pathoangieswenson100% (1)
- Unit 1 Study GuideDokumen6 halamanUnit 1 Study Guideangieswenson100% (4)
- Pharm ReviewDokumen14 halamanPharm ReviewangieswensonBelum ada peringkat
- Which of The Following Is A Protein Hormone That Is Water Soluble? A. Thyroxine (T4 B.) Aldosterone C. FollicleDokumen11 halamanWhich of The Following Is A Protein Hormone That Is Water Soluble? A. Thyroxine (T4 B.) Aldosterone C. FollicleangieswensonBelum ada peringkat
- Concept 020 IMMUNITY GiddensDokumen21 halamanConcept 020 IMMUNITY Giddensangieswenson50% (2)
- Mechanisms of Hormonal RegulationDokumen36 halamanMechanisms of Hormonal RegulationangieswensonBelum ada peringkat
- Concept 012 Glucose Regulation GiddensDokumen19 halamanConcept 012 Glucose Regulation GiddensangieswensonBelum ada peringkat
- Understanding by Design Handbook (Pp. 161-175) - Save Grading Time, Convey Effective Feedback and Promote Student LearningDokumen16 halamanUnderstanding by Design Handbook (Pp. 161-175) - Save Grading Time, Convey Effective Feedback and Promote Student LearningangieswensonBelum ada peringkat
- Chapter 018 Hormonal DiseasesDokumen32 halamanChapter 018 Hormonal DiseasesangieswensonBelum ada peringkat
- Chapter 008 StressDokumen22 halamanChapter 008 StressangieswensonBelum ada peringkat
- Violence in The Workplace Position PaperDokumen4 halamanViolence in The Workplace Position PaperangieswensonBelum ada peringkat
- Seminar Case Study Instructions FA2013Dokumen3 halamanSeminar Case Study Instructions FA2013angieswensonBelum ada peringkat
- Week 1 Drug HistoryDokumen46 halamanWeek 1 Drug HistoryangieswensonBelum ada peringkat
- Improper Conduct - Case OneDokumen4 halamanImproper Conduct - Case OneangieswensonBelum ada peringkat
- Negative Workplace BehaviorsDokumen9 halamanNegative Workplace BehaviorsangieswensonBelum ada peringkat
- Improper Conduct - Case Three PTDokumen4 halamanImproper Conduct - Case Three PTangieswensonBelum ada peringkat
- Lab ValuesDokumen8 halamanLab Valuesjdub4yaBelum ada peringkat
- All Hesi HintsDokumen27 halamanAll Hesi Hintsangieswenson100% (34)
- Negative Workplace BehaviorsDokumen9 halamanNegative Workplace BehaviorsangieswensonBelum ada peringkat
- Resumen EKGDokumen22 halamanResumen EKGWarlan Steven Soto FloresBelum ada peringkat
- Safety Plan TemplateDokumen1 halamanSafety Plan TemplateangieswensonBelum ada peringkat
- 6th Central Pay Commission Salary CalculatorDokumen15 halaman6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- APA Annotated BibliographyDokumen3 halamanAPA Annotated BibliographyangieswensonBelum ada peringkat
- CH 17 Fluid and ElectrolytesDokumen125 halamanCH 17 Fluid and ElectrolytesangieswensonBelum ada peringkat
- APA Annotated BibliographyDokumen4 halamanAPA Annotated Bibliographyangieswenson83% (6)
- Solubility and PermeabilityDokumen3 halamanSolubility and PermeabilityGNCDWBelum ada peringkat
- Pharmacology Modules 1 - 2Dokumen10 halamanPharmacology Modules 1 - 2Elvira GumiBelum ada peringkat
- Exploring The Drug Development ProcessDokumen9 halamanExploring The Drug Development Processs adhikariBelum ada peringkat
- Hospitalpharmacy PDFDokumen13 halamanHospitalpharmacy PDFBhavin DesaiBelum ada peringkat
- Bonus Product Sales April-2023Dokumen3 halamanBonus Product Sales April-2023Mahbub Alam SarkerBelum ada peringkat
- Refer Books Sort ListDokumen12 halamanRefer Books Sort ListDr-Ram ChowdharyBelum ada peringkat
- Should More Patients Be Offered Treatment With Cannabinoids?Dokumen5 halamanShould More Patients Be Offered Treatment With Cannabinoids?Geral Rocha CorrealBelum ada peringkat
- Exam MarchDokumen2 halamanExam MarchkathlynmangasiBelum ada peringkat
- Chupp's Herb 3000mg Berry - BT 345 12278Dokumen1 halamanChupp's Herb 3000mg Berry - BT 345 12278CJ PetersonBelum ada peringkat
- The Pharmaceutical Industry and The Future of Drug DevelopmentDokumen42 halamanThe Pharmaceutical Industry and The Future of Drug Developmentgnk9Belum ada peringkat
- Need and Importance of Drug Information Centres in Indian Hospital System PDFDokumen8 halamanNeed and Importance of Drug Information Centres in Indian Hospital System PDFDrAmit VermaBelum ada peringkat
- Practice School On Research and Development: Key HighlightsDokumen17 halamanPractice School On Research and Development: Key Highlightssubhankar pradhanBelum ada peringkat
- Drug Master FileDokumen4 halamanDrug Master FileTHE SMURFSBelum ada peringkat
- Role of Computer-Aided Drug Design in Modern Drug DiscoveryDokumen16 halamanRole of Computer-Aided Drug Design in Modern Drug DiscoverySourav MajumdarBelum ada peringkat
- Critical Appraisal of Epidemiological StudyDokumen20 halamanCritical Appraisal of Epidemiological StudyCandela NewtonBelum ada peringkat
- Jubilant Life Sciences Receives ANDA Approval For Montelukast (Company Update)Dokumen2 halamanJubilant Life Sciences Receives ANDA Approval For Montelukast (Company Update)Shyam SunderBelum ada peringkat
- Compartment Modelling Upto IV InfusionDokumen42 halamanCompartment Modelling Upto IV Infusionuday sainiBelum ada peringkat
- BOMRA Registration Quality GuidelinesDokumen95 halamanBOMRA Registration Quality GuidelinesBK RegulatoryBelum ada peringkat
- Compounding in Community SettingDokumen19 halamanCompounding in Community Settingkhangsiean89100% (1)
- 2 Determination of Dose and Dosing IntervalDokumen36 halaman2 Determination of Dose and Dosing IntervalSreya Sanil100% (1)
- 03.affinity Efficacy PotencyDokumen33 halaman03.affinity Efficacy PotencyelitechemsBelum ada peringkat
- Dissecting The Opioid Heroin Epidemic To Discover Its Ugly RootsDokumen7 halamanDissecting The Opioid Heroin Epidemic To Discover Its Ugly RootsThavamBelum ada peringkat
- FDA Interpretation of 505 (B) (2) NDADokumen36 halamanFDA Interpretation of 505 (B) (2) NDAShilpa KotianBelum ada peringkat
- Biopharmaceutics BP604T MCQs Unit II PDFDokumen5 halamanBiopharmaceutics BP604T MCQs Unit II PDFMamta Pant88% (17)
- FDA Citizen's Charter CDRR - CPR - 22 December 2020Dokumen274 halamanFDA Citizen's Charter CDRR - CPR - 22 December 2020Jima JamBelum ada peringkat
- Edwards Sharon Axe Sue 10 Rs of Safe Multidisciplinary Drug Administration PDFDokumen9 halamanEdwards Sharon Axe Sue 10 Rs of Safe Multidisciplinary Drug Administration PDFNimrod Bautista SolosaBelum ada peringkat
- Orig 1 S 000 Other RDokumen37 halamanOrig 1 S 000 Other RCastle SkyBelum ada peringkat
- DownloadDokumen27 halamanDownloadKHAIRUNNISA FADILABelum ada peringkat
- Uttaravalli Divya: Mobile: +91 6281585287Dokumen5 halamanUttaravalli Divya: Mobile: +91 6281585287Divya UttaravalliBelum ada peringkat
- NANDA DAFFA PRASETYAWAN Fix DirDokumen2 halamanNANDA DAFFA PRASETYAWAN Fix Dirbeauty asriBelum ada peringkat