Afrisya Bimo Siwendro Marisha Yadian Putri Preceptor: DR - Liza Nursanty, Spb. Finacs
Diunggah oleh
irma0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
39 tayangan32 halamanappendicitis
Judul Asli
Appendicitis
Hak Cipta
© © All Rights Reserved
Format Tersedia
PPTX, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen Iniappendicitis
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PPTX, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
39 tayangan32 halamanAfrisya Bimo Siwendro Marisha Yadian Putri Preceptor: DR - Liza Nursanty, Spb. Finacs
Diunggah oleh
irmaappendicitis
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PPTX, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 32
Afrisya Bimo Siwendro
Marisha Yadian Putri
Preceptor: dr.Liza Nursanty, SpB. FINACS
The appendix first becomes visible in the 8 week
of embryologic development as a protuberance
off the terminal portion of the cecum. During
both antenatal and postnatal development, the
growth rate of the cecum exceeds that of the
appendix, displacing the appendix medially
toward the ileocecal valve. The relationship of
the base of the appendix to the cecum remains
constant, whereas the tip can be found in a
retrocecal, pelvic, subcecal, preileal, or right
pericolic position. 3 taenia coli converge at the
junction of the cecum with the appendix and can
be a useful landmark to identify the appendix
Appendix is an immunologic organ that
actively participates in the secretion of
immunoglobulin A (IgA).
Appendix is an integral component of the
gut-associated lymphoid tissue (GALT)
system.
After the age of 60 years, virtually no
lymphoid tissue remains within the appendix,
and complete obliteration of the appendiceal
lumen is common.
Inflammationof the vermiform appendix
with acute onset
Appendicitis is most frequently seen in
patients in their second through fourth
decades of life, with a mean age of 31.3
years and a median age of 22 years. There is
a slight male to female predominance (M:F
1.2 to 1.3:1).
Obstruction of the lumen is the dominant causal
factor in acute appendicitis.
Fecaliths are the usual cause of appendiceal
obstruction.
Less-common causes are hypertrophy of
lymphoid tissue, inspissated barium from
previous x-ray studies, tumors, vegetable and
fruit seeds, and intestinal parasites.
Fecaliths are found in 40% of cases of simple
acute appendicitis, 65% of cases of gangrenous
appendicitis without rupture, and nearly 90% of
cases of gangrenous appendicitis with rupture.
Symptom
- Migrating abdominal pain. (May vary, depend on
variant location of appendix)
- Anorexia, although vomiting occurs in nearly 75% of
patients, it is neither prominent nor prolonged and
most patients vomit only once or twice. Vomiting is
caused both by neural stimulation and the presence
of ileus.
- Obstipation, but it some patient, particularly
children may cause diarrhea.
Sign
- Vital signs are minimally changed. Temperature
elevation is rarely more than 1°C (1.8°F) and the
pulse rate is normal or slightly elevated.
- Patients with appendicitis usually prefer to lie
supine, with the right thigh drawn up. If asked to
move, they do so slowly and with caution.
- McBurney tenderness, Rovsing sign (+), Right sided
Hyperesthesia T 10, 11, 12
- Psoas and obturator sign (+) indicate muscle and
pelvic irritation.
Rovsing’s sign
Obturator sign
Psoas sign
When the inflamed
appendix hangs into the
pelvis, abdominal findings
may be entirely absent,
and the diagnosis may be
missed unless the rectum is
examined. As the
examining finger exerts
pressure on the peritoneum
of the cul-de-sac of
Douglas, pain is felt in the
suprapubic area, as well as
locally within the rectum.
Mild leukocytosis, ranging from 10,000 to
18,000/mm3, is usually present in patients
with acute, uncomplicated appendicitis and
is often accompanied by a moderate
polymorphonuclear predominance.
Acute Mesenteric Adenitis Acute gastroenteritis
Most often confused with Common in childhood but can
acute appendicitis in usually be easily
children. differentiated from
The pain is usually appendicitis.
diffuse, and tenderness is Viral gastroenteritis, an acute
not as sharply localized as self-limited infection of
in appendicitis. diverse causes, is
Voluntary guarding is characterized by profuse
sometimes present, but watery diarrhea, nausea, and
true rigidity is rare. vomiting.
Generalized Hyperperistaltic abdominal
lymphadenopathy may be cramps precede the watery
noted. Laboratory stools. The abdomen is
procedures : relative relaxed between cramps, and
lymphocytosis, when there are no localizing signs.
present, suggests Laboratory values are normal.
mesenteric adenitis.
Meckel's diverticulitis causes a clinical picture
similar to that of acute appendicitis. The Meckel's
diverticulum is located within the distal 2 feet of the
ileum.
Intussusception
Differentiate intussusception from acute
appendicitis as the treatment is different.
Appendicitis is very uncommon in children younger
than age 2 years, whereas nearly all idiopathic
intussusceptions occur in children younger than
age 2 years.
Intussusception occurs typically in a well-
nourished infant who is suddenly doubled up by
apparent colicky pain. Between attacks of pain,
the infant appears well. After several hours, the
patient usually passes a bloody mucoid stool.
A sausage-shaped mass may be palpable in the
right lower quadrant. As the intussusception
progresses distally, the right lower quadrant feels
abnormally empty.
Crohn’s enteritis
The manifestations of acute regional enteritis—fever,
right lower quadrant pain and tenderness, and
leukocytosis—often simulate acute appendicitis.
Diarrhea and the infrequency of anorexia, nausea, and
vomiting favor a diagnosis of enteritis but are not
sufficient to exclude acute appendicitis.
Pelvic Inflammatory Disease
The infection is usually bilateral, but if confined to the
right tube, may mimic acute appendicitis. Nausea and
vomiting often are present in patients with
appendicitis, but only in approximately 50% of those
with pelvic inflammatory disease. The greatest value of
these symptoms for establishing a diagnosis of pelvic
inflammatory disease is their absence. Pain and
tenderness are usually lower, and motion of the cervix
is exquisitely painful. Intracellular diplococci may be
demonstrable on smear of the purulent vaginal
discharge
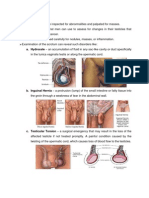
Ruptured Ectopic Ureteral Stone
Pregnancy Pain referred to the
Rupture of right tubal labia, scrotum, or
or ovarian penis; hematuria;
pregnancies can and/or absence of
mimic appendicitis. fever or leukocytosis
Patients usually give a
suggest the presence
history of abnormal of a ureteral stone.
menses; either Pyelography and CT
missing one or two scanning without oral
periods or noting only contrast usually
slight vaginal confirm the diagnosis.
bleeding.
The development of
right lower quadrant
or pelvic pain may be
the first symptom.
Diagnosis of acute appendicitis in young children is more difficult
than in the adult. The more rapid progression to rupture and the
inability of the underdeveloped greater omentum to contain a
rupture lead to significant morbidity rates in children.
Antibiotic coverage is limited to 24 to 48 hours in cases of
nonperforated appendicitis. For perforated appendicitis, 7 to 10
days of antibiotics is recommended. Intravenous antibiotics are
usually given until the white blood cell count is normal and the
patient is afebrile for 24 hours.
Laparoscopic appendectomy has been shown to be safe and
effective for the treatment of appendicitis in children.
Although the incidence of appendicitis in the
elderly is lower than in younger patients, the
morbidity and mortality are significantly
increased in this patient population.
Delays in diagnosis, a more rapid progression
to perforation, and comorbid disease are all
contributing factors.
In patients older than age 80 years,
perforation rates of 49% and mortality rates
of 21%
The incidence is approximately 1 in 2000 pregnancies. Acute
appendicitis can occur at any time during pregnancy, but is more
frequent during the first two trimesters.
As fetal gestation progresses, the diagnosis of appendicitis
becomes more difficult as the appendix is displaced laterally and
superiorly (Fig. 29-7). Nausea and vomiting after the first
trimester or new-onset nausea and vomiting should raise the
consideration of appendicitis.
Abdominal pain and tenderness will be present, although rebound
and guarding are less frequent because of laxity of the abdominal
wall. Elevation of the white blood cell count above the normal
pregnancy levels of 15,000 to 20,000/L, with a predominance of
polymorphonuclear cells, is usually present.
When the diagnosis is in doubt, abdominal ultrasound may be
beneficial. Laparoscopy may be indicated in equivocal cases,
especially early in pregnancy. The performance of any operation
during pregnancy carries a risk of premature labor of 10 to 15%,
and the risk is similar for both negative laparotomy and
appendectomy for simple appendicitis.
The incidence of acute appendicitis in HIV-
infected patients is reported to be 0.5%. 67 This
is higher than the 0.1 to 0.2% incidence reported
for the general population. 68
The presentation of acute appendicitis in HIV-
infected patients is similar to that of
noninfected patients. The majority of HIV-
infected patients with appendicitis will have
fever, periumbilical pain radiating to the right
lower quadrant (91%), right lower quadrant
tenderness (91%), and rebound tenderness (74%).
HIV-infected patients will not manifest an
absolute leukocytosis.
Open appendectomy
Death is usually attributable to uncontrolled
sepsis—peritonitis, intra-abdominal
abscesses, or gram-negative septicemia.
Pulmonary embolism continues to account
for some deaths. Aspiration is a significant
cause of death in the older patient group.
Principalfactors in mortality are whether
rupture occurs before surgical treatment and
the age of the patient. The overall mortality
rate for a general anesthetic is 0.06%. The
overall mortality rate in ruptured acute
appendicitis is about 3%—a 50-fold increase.
The mortality rate of ruptured appendicitis
in the elderly is approximately 15%—a
fivefold increase from the overall rate.
Characteristically, the pain lasts longer and is less intense than that of
acute appendicitis, but is in the same location. There is a much lower
incidence of vomiting, but anorexia and occasionally nausea, pain with
motion, and malaise are characteristic. Leukocyte counts are predictably
normal and CT scans are generally nondiagnostic.
At operation, surgeons can establish the diagnosis with 94% specificity
and 78% sensitivity. There is an excellent correlation between clinical
symptomatology, intraoperative findings, and histologic abnormalities.
Laparoscopy can be effectively used in the management of this clinical
entity. Appendectomy is curative. Symptoms resolve postoperatively in 82
to 93% of patients. Many of those whose symptoms are not cured or recur
are ultimately diagnosed with Crohn's disease.
A number of intestinal parasites cause appendicitis. While
Ascaris lumbricoides is the most common, a wide spectrum
of helminths have been implicated, including Enterobius
vermicularis, Strongyloides stercoralis, and Echinococcus
granulosis. The live parasites occlude the appendiceal
lumen, causing obstruction.
The presence of parasites in the appendix at operation
makes ligation and stapling of the appendix technically
difficult. Once appendectomy has been performed and the
patient recovered, therapy with helminthicide is necessary
to clear the remainder of the gastrointestinal tract.
Amebiasis can also cause appendicitis. Invasion of the
mucosa by trophozoites of Entamoeba histolytica incites a
marked inflammatory process. Appendiceal involvement is
a component of more generalized intestinal amebiasis.
Appendectomy must be followed by appropriate antibiotic
therapy (metronidazole).
Anda mungkin juga menyukai
- Disorders of Motility2Dokumen46 halamanDisorders of Motility2valdomiroBelum ada peringkat
- PE, Tamponade, Constrictive PericarditisDokumen1 halamanPE, Tamponade, Constrictive PericarditisKaylee HvezdaBelum ada peringkat
- Major Depressive Disorder PDFDokumen22 halamanMajor Depressive Disorder PDFapi-545811586Belum ada peringkat
- Pneumothorax & Hemothorax: Farshid MokhberiDokumen32 halamanPneumothorax & Hemothorax: Farshid MokhberiYan Sheng HoBelum ada peringkat
- Cardiac Emergencies PDFDokumen57 halamanCardiac Emergencies PDFJohn Paulo CatacutanBelum ada peringkat
- Heart SoundsDokumen2 halamanHeart Soundsdanny_awwadBelum ada peringkat
- LV RV FailureDokumen118 halamanLV RV FailureMirza Thaariq HapsitoBelum ada peringkat
- Surgery Signs, Triads N SyndromesDokumen11 halamanSurgery Signs, Triads N Syndromesdrusmansaleem100% (1)
- Chest Trauma3Dokumen120 halamanChest Trauma3Rojelle LezamaBelum ada peringkat
- Aldomet Altace Atenolol Verapamil: Medication Brand Name Drug ClassDokumen11 halamanAldomet Altace Atenolol Verapamil: Medication Brand Name Drug Classshellyrn2010Belum ada peringkat
- PATHO 4-3 Diseases of The EsophagusDokumen7 halamanPATHO 4-3 Diseases of The EsophagusMiguel Cuevas DolotBelum ada peringkat
- Neuromuscular DisordersDokumen73 halamanNeuromuscular Disordersnurwahidah100% (1)
- Female Reproductive SystemDokumen3 halamanFemale Reproductive SystemJayricDepalobosBelum ada peringkat
- Acute Urinary ObstructionDokumen34 halamanAcute Urinary ObstructionHafizur RashidBelum ada peringkat
- #9 Ie 8 PDFDokumen8 halaman#9 Ie 8 PDFOmar BasimBelum ada peringkat
- Rosh NeuroDokumen11 halamanRosh NeuroSoni AliBelum ada peringkat
- Male GU ExamDokumen5 halamanMale GU ExamOmar Farid ElgebalyBelum ada peringkat
- Leg UlcerDokumen28 halamanLeg UlcerRanindya PutriBelum ada peringkat
- NEPHROTIC SYNDROME - HamidDokumen20 halamanNEPHROTIC SYNDROME - HamidAbdul Hamid OmarBelum ada peringkat
- Atresia, Akalasia, EsophaealrefluxDokumen3 halamanAtresia, Akalasia, Esophaealrefluxalmira valmaiBelum ada peringkat
- Optic NeuritisDokumen31 halamanOptic NeuritisUsman ImtiazBelum ada peringkat
- Surgical Treatment GuidelinesDokumen244 halamanSurgical Treatment GuidelinesPetru GorodetchiBelum ada peringkat
- Testicular ExamDokumen3 halamanTesticular ExamminikatitingBelum ada peringkat
- Step 2ck Important (AutoRecovered)Dokumen101 halamanStep 2ck Important (AutoRecovered)Aishwarya SridharBelum ada peringkat
- Hereditary Spherocytosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandHereditary Spherocytosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- Pulmonary Diseases - Dental ManagementDokumen45 halamanPulmonary Diseases - Dental Managementfilyouth4life100% (3)
- Congenital Heart Disease 1Dokumen14 halamanCongenital Heart Disease 1OzzeyBelum ada peringkat
- Increased ICP: A) HeadacheDokumen5 halamanIncreased ICP: A) Headachemohamed nagyBelum ada peringkat
- Bimbingan AHFDokumen61 halamanBimbingan AHFFirlando RiyandaBelum ada peringkat
- Ophthalmology - Passmedicine 2012 - 62013146Dokumen18 halamanOphthalmology - Passmedicine 2012 - 62013146abuahmed&janaBelum ada peringkat
- ENT Quick ReviewDokumen6 halamanENT Quick ReviewWade100% (1)
- Shock, Sirs & ModsDokumen37 halamanShock, Sirs & ModsambitioustamannaBelum ada peringkat
- Neurology - Saif.wesmosis.2013 104907Dokumen68 halamanNeurology - Saif.wesmosis.2013 104907Helene AlawamiBelum ada peringkat
- Vasculitis: Disorder Vessels Pathology Presentation Test TX OtherDokumen3 halamanVasculitis: Disorder Vessels Pathology Presentation Test TX OthermcwnotesBelum ada peringkat
- ABG MCQsDokumen6 halamanABG MCQssoulstakersBelum ada peringkat
- Headache: Rosen's Chapters 17 and 105 November 9, 2006 by George FiliadisDokumen45 halamanHeadache: Rosen's Chapters 17 and 105 November 9, 2006 by George Filiadishemanthshah2801Belum ada peringkat
- Approach To Unconscious PatientDokumen23 halamanApproach To Unconscious Patienttantw880% (1)
- Check Unit 557 Jan-Feb Genetics v3 PDFDokumen36 halamanCheck Unit 557 Jan-Feb Genetics v3 PDFdragon66Belum ada peringkat
- Surgery Pretest SummaryDokumen9 halamanSurgery Pretest SummaryPrince DuBelum ada peringkat
- Pyogenic MeningitisDokumen46 halamanPyogenic MeningitisShahnaaz ShahBelum ada peringkat
- Ring Enhancing LesionsDokumen50 halamanRing Enhancing LesionsVivek GuptaBelum ada peringkat
- Harrison-Principals of Internal Medicine 20th. Ed. Prt.7-11Dokumen707 halamanHarrison-Principals of Internal Medicine 20th. Ed. Prt.7-11Choi DongYiBelum ada peringkat
- Musculoskeletal: Unit 553 September 2018Dokumen34 halamanMusculoskeletal: Unit 553 September 2018dragon66Belum ada peringkat
- PnemoniaDokumen4 halamanPnemoniadhavalBelum ada peringkat
- Cardiovascular Nursing: Study Online atDokumen7 halamanCardiovascular Nursing: Study Online atLilly DayeBelum ada peringkat
- Amazing Esqs With Answers Pediatrics-ShelfDokumen31 halamanAmazing Esqs With Answers Pediatrics-ShelfDrSajid BuzdarBelum ada peringkat
- Neuroleptics & AnxiolyticsDokumen65 halamanNeuroleptics & AnxiolyticsAntonPurpurovBelum ada peringkat
- SepsisDokumen33 halamanSepsisv_vijayakanth7656Belum ada peringkat
- Approach To Cough and HemoptysisDokumen24 halamanApproach To Cough and Hemoptysisbansaleliza26Belum ada peringkat
- Pleural DiseasesDokumen4 halamanPleural DiseasesJennifer DayBelum ada peringkat
- Seizure Disorder, Spinal Injury Neural TumorDokumen52 halamanSeizure Disorder, Spinal Injury Neural TumornipoBelum ada peringkat
- Nephrotic Syndrome: Jaiganesh.M, M.D (General Medicine) Asst. Professor, S.M.C.HDokumen60 halamanNephrotic Syndrome: Jaiganesh.M, M.D (General Medicine) Asst. Professor, S.M.C.HJaiganesh MuruganandamBelum ada peringkat
- (MED II) 1.05 Emergencies in Cancer PatientsDokumen17 halaman(MED II) 1.05 Emergencies in Cancer PatientsJearwin AngelesBelum ada peringkat
- Systolic Dysfunction:: Types of Heart FailureDokumen13 halamanSystolic Dysfunction:: Types of Heart FailureElisabeth F. OjhaBelum ada peringkat
- Peads NotesDokumen18 halamanPeads Notesechofox11Belum ada peringkat
- 01 Interview FormDokumen7 halaman01 Interview FormSavage SkylenBelum ada peringkat
- Special Sense System Group 6Dokumen24 halamanSpecial Sense System Group 6RushdaBelum ada peringkat
- Appendix DuplicationDokumen3 halamanAppendix DuplicationMario TrejoBelum ada peringkat
- AppendicitisDokumen14 halamanAppendicitisNefely Joy GoBelum ada peringkat
- Appy DictationDokumen2 halamanAppy Dictationsgod34100% (1)
- Laporan Kasus AppendicitisDokumen21 halamanLaporan Kasus AppendicitisjessicaBelum ada peringkat
- AppendicitisDokumen36 halamanAppendicitisPetro MyronovBelum ada peringkat
- Neethus Part A 40 TestDokumen244 halamanNeethus Part A 40 TestNadeeka GamageBelum ada peringkat
- Joint Clinico-Pathologic Conference: October 3, 2008Dokumen50 halamanJoint Clinico-Pathologic Conference: October 3, 2008ianjohn724Belum ada peringkat
- Management of Acute Appendicitis in Adults - UpToDateDokumen28 halamanManagement of Acute Appendicitis in Adults - UpToDateaulia rachman100% (1)
- The Coach in The Operating Room - The New Yorker PDFDokumen25 halamanThe Coach in The Operating Room - The New Yorker PDFAhmad RajabiBelum ada peringkat
- Case Study of AppendicitisDokumen14 halamanCase Study of AppendicitisArvin Ian Penaflor89% (27)
- Appendicitis, Acute Sandy Craig, MD, Adjunct Associate Professor, Department of Emergency Medicine, UniversityDokumen21 halamanAppendicitis, Acute Sandy Craig, MD, Adjunct Associate Professor, Department of Emergency Medicine, UniversityIndiIndhysaBelum ada peringkat
- AADokumen20 halamanAAAiyaz AliBelum ada peringkat
- Acute AppendicitisDokumen29 halamanAcute AppendicitisSilhouette Dream100% (1)
- ReflectionDokumen42 halamanReflectionRaidis PangilinanBelum ada peringkat
- 11 AppendixDokumen15 halaman11 AppendixOmar MohammedBelum ada peringkat
- Appendicitis by Tilden, John Henry, 1851-1940Dokumen62 halamanAppendicitis by Tilden, John Henry, 1851-1940Gutenberg.orgBelum ada peringkat
- What Is The Appendix? A Vestigial Organ, or One With A Purpose?Dokumen9 halamanWhat Is The Appendix? A Vestigial Organ, or One With A Purpose?Azizah RahawarinBelum ada peringkat
- EML2322L Design Report TemplateDokumen36 halamanEML2322L Design Report TemplateAlexandra GrtBelum ada peringkat
- TNM Classification of Malignant Tumours Website 15 MAy2011Dokumen50 halamanTNM Classification of Malignant Tumours Website 15 MAy2011Daniel RusieBelum ada peringkat
- Dissertation Appendix SampleDokumen7 halamanDissertation Appendix SamplePayToDoMyPaperUK100% (1)
- Comunicat Presa RevalorizareDokumen271 halamanComunicat Presa RevalorizareAnonymous PYgnwOWK100% (1)
- Acute Appendicitis & NPI - Edmalyn GozarDokumen78 halamanAcute Appendicitis & NPI - Edmalyn GozarKM100% (1)
- SURGERYFinals - 1. The AppendixDokumen10 halamanSURGERYFinals - 1. The AppendixRenatoCosmeGalvanJuniorBelum ada peringkat
- Pathophysiology Precipitsting Factors: Predisposing FactorsDokumen2 halamanPathophysiology Precipitsting Factors: Predisposing FactorsGeofrey MaglalangBelum ada peringkat
- Instructions For Company Project ProposalDokumen7 halamanInstructions For Company Project ProposalIHangMyBelum ada peringkat
- Anna University Project Report Format UG PDFDokumen7 halamanAnna University Project Report Format UG PDFGokulraju RangasamyBelum ada peringkat
- Conf. 9.24: (Rev. Cop17) Criteria For Amendment of Appendices I and IiDokumen18 halamanConf. 9.24: (Rev. Cop17) Criteria For Amendment of Appendices I and Iileonita soebagioBelum ada peringkat
- Acute Appendicitis in Adults: Clinical Manifestations and Differential DiagnosisDokumen32 halamanAcute Appendicitis in Adults: Clinical Manifestations and Differential DiagnosisGrethel CalderónBelum ada peringkat
- Appendicitis (Case Study)Dokumen40 halamanAppendicitis (Case Study)Cherr Noll SanchezBelum ada peringkat
- Acute Appendicitis and PeritonitisDokumen8 halamanAcute Appendicitis and PeritonitisYosuaBelum ada peringkat